
A more recent article on streptococcal pharyngitis is available.
This is a corrected version of the article that appeared in print.
Am Fam Physician. 2016;94(1):24-31
Patient information: See related handout on strep throat, written by the authors of this article.
Author disclosure: No relevant financial affiliations.
Group A beta-hemolytic streptococcal (GABHS) infection causes 15% to 30% of sore throats in children and 5% to 15% in adults, and is more common in the late winter and early spring. The strongest independent predictors of GABHS pharyngitis are patient age of five to 15 years, absence of cough, tender anterior cervical adenopathy, tonsillar exudates, and fever. To diagnose GABHS pharyngitis, a rapid antigen detection test should be ordered in patients with a modified Centor or FeverPAIN score of 2 or 3. First-line treatment for GABHS pharyngitis includes a 10-day course of penicillin or amoxicillin. Patients allergic to penicillin can be treated with first-generation cephalosporins, clindamycin, or macrolide antibiotics. Nonsteroidal anti-inflammatory drugs are more effective than acetaminophen and placebo for treatment of fever and pain associated with GABHS pharyngitis; medicated throat lozenges used every two hours are also effective. Corticosteroids provide only a small reduction in the duration of symptoms and should not be used routinely.
Pharyngitis is diagnosed in 11 million persons in the outpatient setting each year in the United States.1 Although most episodes are caused by viruses, group A beta-hemolytic streptococcal (GABHS) infection accounts for approximately 15% to 30% of sore throats in children and 5% to 15% in adults.1 Approximately 80% of these episodes are diagnosed in the primary care setting.2 This article reviews common questions about GABHS pharyngitis and provides evidence-based answers.
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Physicians should diagnose GABHS pharyngitis using an approach that combines a validated clinical decision rule (e.g., modified Centor score, FeverPAIN score) with selective use of rapid antigen detection testing. | A | 1, 21, 22 |
| Penicillin is the first-line antibiotic for treating GABHS pharyngitis. | A | 22, 24, 28, 32 |
| Symptomatic treatment of GABHS pharyngitis can include medicated throat lozenges, nonsteroidal anti-inflammatory drugs, and topical anesthetics. | B | 3, 35, 36, 38, 39 |
Who Is at Increased Risk of GABHS Pharyngitis?
EVIDENCE SUMMARY
Several risk factors should increase the index of suspicion for GABHS pharyngitis. Children five to 15 years of age who have been exposed in the past 72 hours to someone with GABHS infection are at highest risk.1,3,4 The incubation period for GABHS infection is 24 to 72 hours.1 A 2010 meta-analysis found that symptomatic children five to 15 years of age are more likely to have throat cultures positive for GABHS infection compared with younger children (37% vs. 24%).6 Additionally, 2012 guidelines from the Infectious Diseases Society of America (IDSA) indicate that GABHS infection is uncommon in children younger than three years.3 The prevalence of acute pharyngitis secondary to GABHS infection in adults ranges from 5% to 15%.1,3 GABHS pharyngitis is more common in late winter and early spring.1,5 Although contact with GABHS carriers has been implicated in pharyngeal infections, the actual carrier transmission rate is 3% to 11%.1,3,7,8 Adults with frequent exposure to school-aged children are at increased risk of GABHS infection.6,9
How Is GABHS Infection Differentiated from Other Causes of Pharyngitis?
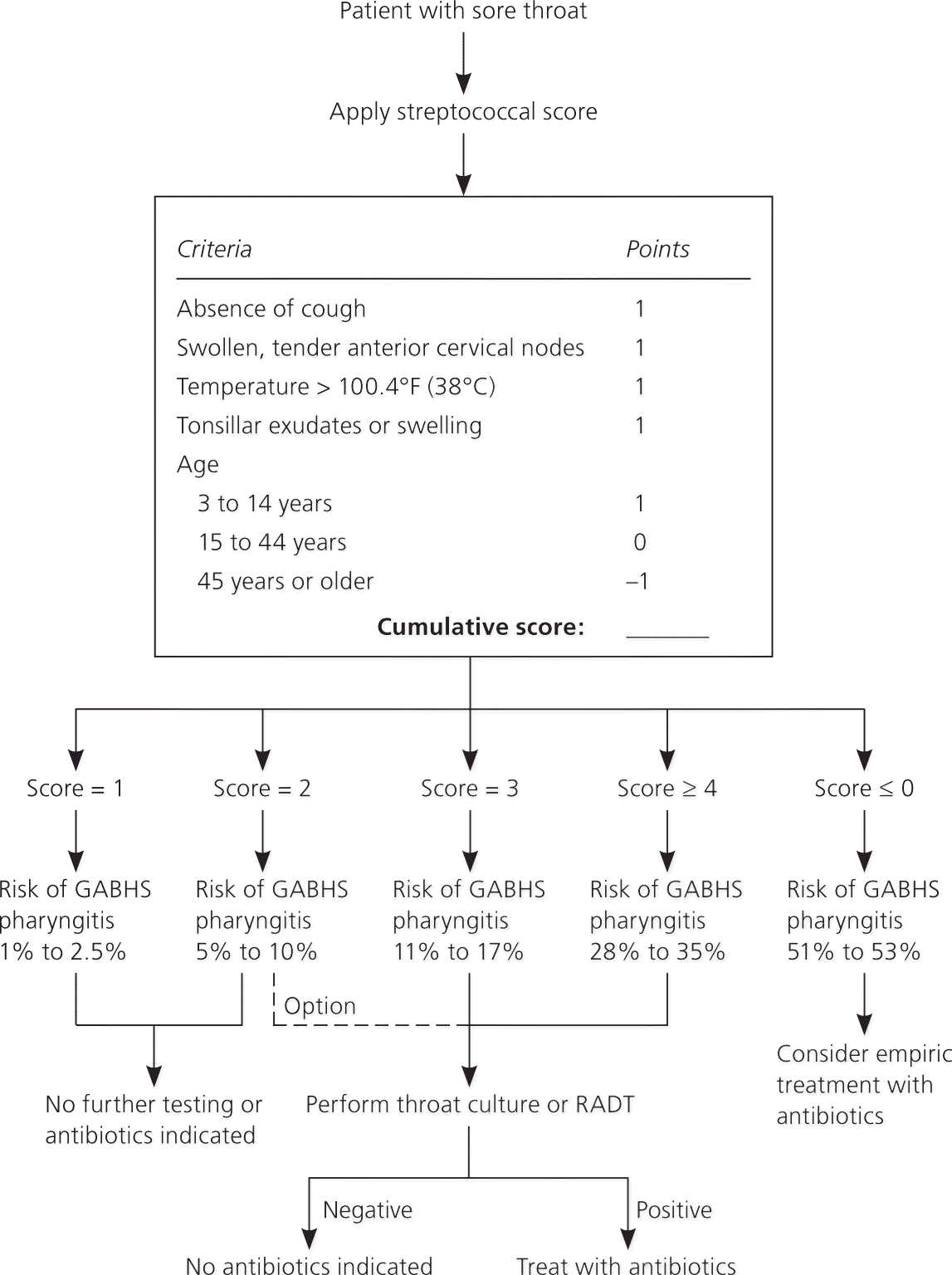
GABHS pharyngitis should be suspected in patients with fever, tonsillar exudates, absence of cough, intensely inflamed tonsils, acute onset, and tender anterior adenopathy.10,11 Infectious mononucleosis should be considered in patients with posterior cervical adenopathy, fatigue, and atypical lymphocytosis.12–14 Hand-foot-and-mouth disease should be considered in patients with oral lesions, sometimes accompanied by an exanthem on the hands and feet.15–17 Clinical rules such as the modified Centor score (Figure 11,18) and FeverPAIN score (Table 111) can be used to identify patients at low, moderate, and high risk of GABHS infection.10,11

| Signs and symptoms | Points | ||
| Fever in past 24 hours | 1 | ||
| Intensely inflamed tonsils | 1 | ||
| No cough or coryza | 1 | ||
| Presentation within three days of symptom onset | 1 | ||
| Purulent tonsils | 1 | ||
| Total: | ______ | ||
| Points | Risk of group A or C streptococcal pharyngitis (%) | Recommendation | |
| 0 or 1 | 1 to 10 | No testing or treatment needed; consider backup throat culture in children three to 15 years of age | |
| 2 | 11 to 17 | Rapid antigen detection testing | |
| 3 | 28 to 35 | Rapid antigen detection testing | |
| 4 or 5 | 51 to 53 | Empiric antibiotics | |
EVIDENCE SUMMARY
A systematic review of the clinical diagnosis of GABHS pharyngitis found that clinical characteristics, seasonality, and age can help differentiate GABHS infection from other etiologies of sore throat.6 Herpangina can be distinguished from GABHS pharyngitis by the presence of vesicular oral lesions in the posterior oral cavity.15,19 Hand-foot-and-mouth disease can present with painful oral lesions similar to herpangina, but can also be accompanied by an exanthem on the hands and feet. Additionally, herpangina and hand-foot-and-mouth disease occur more often in the summer and are more common in children younger than five years.15–17,20
Epstein-Barr virus causes 90% of infectious mononucleosis cases and may also be confused with GABHS infection (Figure 2). However, infectious mononucleosis is more common in persons 10 to 30 years of age and is associated with fatigue, posterior cervical adenopathy, and atypical lymphocytosis.12–14 A prospective study evaluating the most common symptoms of infectious mononucleosis found that the pharyngitis was typically associated with fatigue (77% of cases), posterior cervical adenopathy (59%), and atypical lymphocytosis.14 These signs and symptoms are usually less severe or lacking in GABHS pharyngitis.
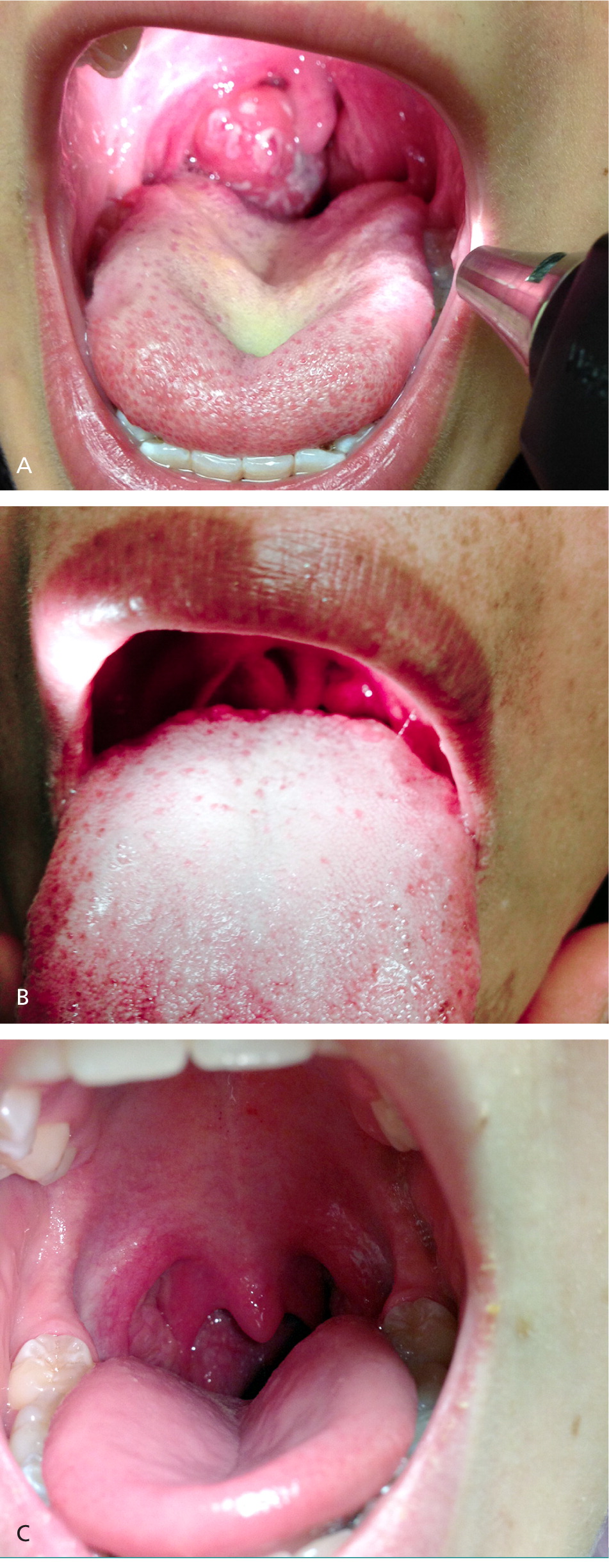
The best data for the diagnosis of GABHS pharyngitis come from studies that combine age, signs, and symptoms to determine the likelihood of disease. These clinical decision rules will be discussed in more detail.
When Should RADT Be Ordered?
Results from rapid antigen detection testing (RADT) should be used in conjunction with a validated clinical decision rule such as the modified Centor score or the FeverPAIN score. Patients at low risk of GABHS pharyngitis can be treated symptomatically, RADT should be ordered for those at intermediate risk, and empiric antibiotics are an option for those at high risk.
EVIDENCE SUMMARY
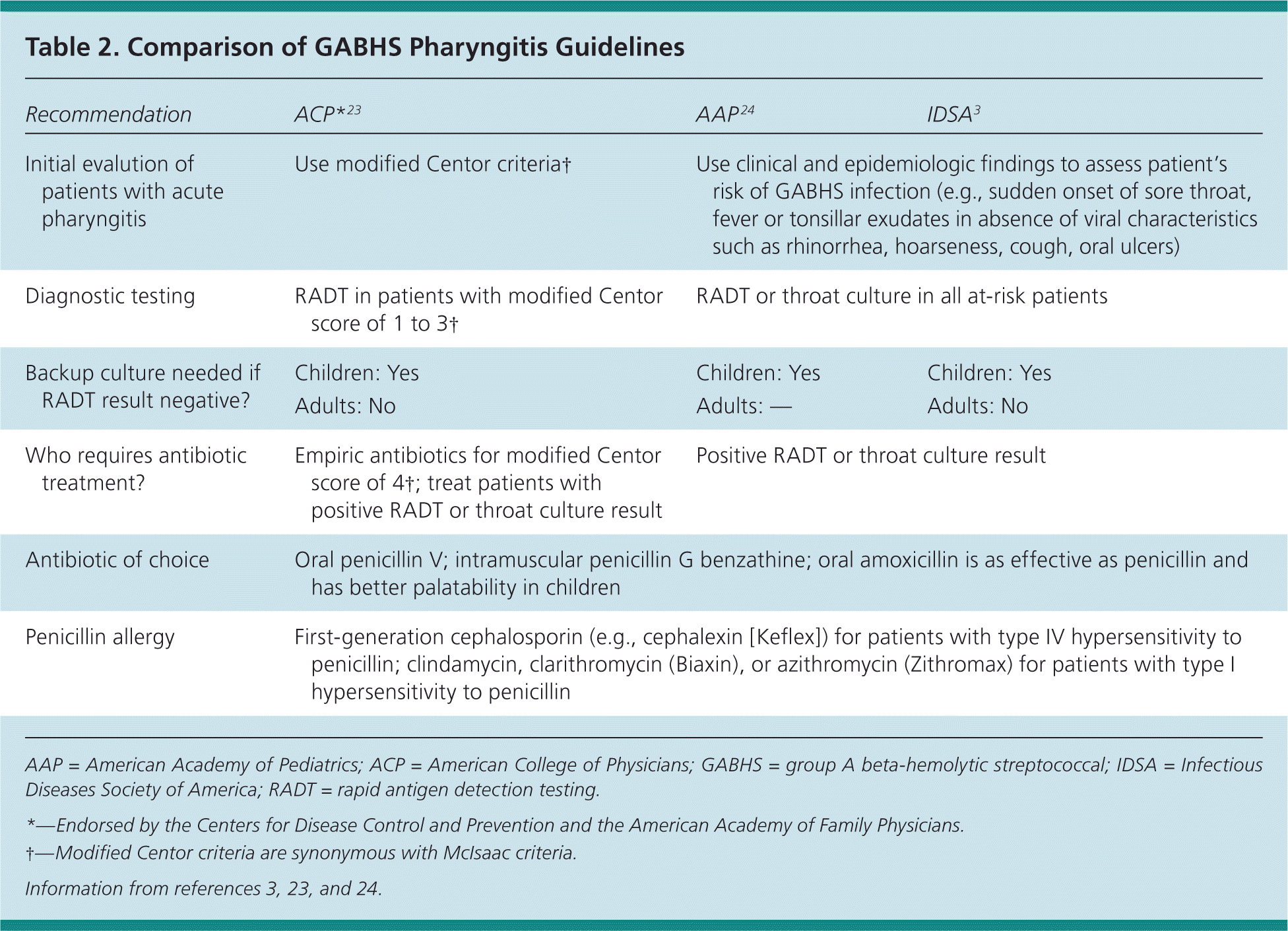
Two commonly used rules, the Centor and modified Centor (also known as McIsaac) rules, are recommended by the Centers for Disease Control and Prevention to determine which patients require RADT for diagnosis.1,21,22 The Centor rule gives one point for each of the following: fever; absence of cough; presence of tonsillar exudates; and swollen, tender anterior adenopathy (Figure 11,18 ). The modified Centor score adds an additional point for patient age of three to 14 years and subtracts one point for patients older than 45 years.1,21,22 A combined approach using clinical decision rules and RADT results is the best method to reduce the cost of unnecessary testing and unwarranted antibiotics. Table 2 describes testing and treatment guidelines from different groups.3,23,24
| Recommendation | ACP*23 | AAP24 | IDSA3 |
|---|---|---|---|
| Initial evalution of patients with acute pharyngitis | Use modified Centor criteria† | Use clinical and epidemiologic findings to assess patient's risk of GABHS infection (e.g., sudden onset of sore throat, fever or tonsillar exudates in absence of viral characteristics such as rhinorrhea, hoarseness, cough, oral ulcers) | |
| Diagnostic testing | RADT in patients with modified Centor score of 1 to 3† | RADT or throat culture in all at-risk patients | |
| Backup culture needed if RADT result negative? | Children: Yes | Children: Yes | Children: Yes |
| Adults: No | Adults: — | Adults: No | |
| Who requires antibiotic treatment? | Empiric antibiotics for modified Centor score of 4†; treat patients with positive RADT or throat culture result | Positive RADT or throat culture result | |
| Antibiotic of choice | Oral penicillin V; intramuscular penicillin G benzathine; oral amoxicillin is as effective as penicillin and has better palatability in children | ||
| Penicillin allergy | First-generation cephalosporin (e.g., cephalexin [Keflex]) for patients with type IV hypersensitivity to penicillin; clindamycin, clarithromycin (Biaxin), or azithromycin (Zithromax) for patients with type I hypersensitivity to penicillin | ||
If RADT results are negative, patients should be treated symptomatically and asked to return if symptoms persist after five days or worsen. If symptoms persist beyond five days, patients should be evaluated for signs and symptoms of infectious mononucleosis, peritonsillar abscess, and human immunodeficiency virus infection.22 If any of these conditions are suspected, further testing should be performed. If a throat culture was not performed during the initial visit, it should be ordered at this time.
A retrospective study analyzed data from 2006 to 2008 in 206,870 patients with sore throat who presented to a pharmacy-based clinic.25 The clinicians followed, with more than 99% adherence, an acute pharyngitis protocol that required recording patients' signs and symptoms before ordering RADT. Among patients 15 years and older, 7% of those with a modified Centor score of 0 and 12% with a score of 1 tested positive for GABHS pharyngitis. Among patients three years and older, 8% of those with a modified Centor score of 0 and 14% with a score of 1 tested positive for GABHS pharyngitis.
Is a Backup Throat Culture Necessary After RADT?
Backup throat cultures are not needed for adults with negative RADT results. Because children are at higher risk of complications such as peritonsillar abscess, rheumatic fever, and poststreptococcal glomerulonephritis, backup throat cultures are recommended for children with negative RADT results. When using one of the newer highly sensitive optical immunoassay or molecular tests, a backup culture is of little value, even in children, and may be omitted. Physicians should be aware of the type of RADT used in their clinical setting.
EVIDENCE SUMMARY
The 2012 guidelines from the IDSA recommend backup throat cultures in children with negative RADT results to avoid the development of complications such as peritonsillar abscess, rheumatic fever, and poststreptococcal glomerulonephritis.3 Although these complications are rare in the United States, they can be prevented if antibiotics are started within the first nine days of infection.26
A throat culture has 90% to 95% sensitivity in diagnosing GABHS infection, whereas lateral flow RADT has a wide variability in sensitivity (59% to 96%).3,27 Optical immunoassays are 86% sensitive for diagnosis, and molecular RADT models are even more sensitive (89% to 96%).27 Molecular tests (e.g., polymerase chain reaction testing, DNA probes, fluorescence in situ hybridization testing) are currently too expensive for most practices to use and have a turnaround time of one to three hours. Therefore, the need to use backup throat culture in patients with negative RADT results depends on the type of RADT used. Given a pretest probability of GABHS infection of 25% in children, 33 to 50 backup throat cultures would need to be ordered to detect one case of GABHS pharyngitis missed by optical immunoassay or molecular RADT.27 On the other hand, 14% of GABHS infections are missed if a backup culture is not ordered for a patient with negative RADT results.27 Based on these findings, backup cultures are recommended when lateral flow RADT is used, but not when optical immunoassays or molecular tests are available. If backup culture is not performed, patients should be advised to return for further evaluation if symptoms persist for more than five days. At that time, further testing, including a throat culture, should be performed.
Which Antibiotics Are Most Effective for Treatment of GABHS Pharyngitis?
Based on its narrow spectrum of activity, cost, few adverse effects, and effectiveness, penicillin is recommended by the American Academy of Family Physicians,23 the American Academy of Pediatrics,24 the American Heart Association,28 the IDSA,29 and the World Health Organization30 for the treatment of GABHS pharyngitis. For patients with type IV hypersensitivity reactions to penicillin (e.g., rash), a first-generation cephalosporin is an alternative. Patients with type I hypersensitivity reactions (i.e., anaphylaxis) should be prescribed clindamycin, clarithromycin (Biaxin), or azithromycin (Zithromax).3
Recurrent GABHS pharyngitis is defined as a repeat infection within 30 days of the initial illness. These infections are usually a result of noncompliance with treatment. Amoxicillin/clavulanate (Augmentin), clindamycin, or intramuscular penicillin G benzathine is effective in patients with recurrent GABHS pharyngitis. If a first-generation cephalosporin (e.g., cephalexin [Keflex]) is used for the initial infection, a third-generation cephalosporin (e.g., cefdinir [Omnicef]) should be used to provide broader coverage for repeat illness.29 Patients diagnosed with GABHS pharyngitis may return to work or school 24 hours after starting antibiotics and when afebrile.31
EVIDENCE SUMMARY
A 2013 Cochrane review studied 17 trials with 5,352 participants and compared penicillin and a cephalosporin as first-line treatments for GABHS pharyngitis.32 The review did not find significant differences in effectiveness, adverse effects, or relapse rates between groups. Based on the low cost and resistance rate of penicillins to GABHS infection, the review supports penicillins as first-line therapy for GABHS pharyngitis. Cephalosporins should be used for patients with delayed allergic reactions to penicillin.
A 2012 Cochrane review comparing a three- to six-day course of antibiotics with a 10-day course found similar effectiveness between groups.33 Therefore, a shorter course of antibiotics is an option when the prevalence of rheumatic fever is low and the primary goal of treatment is symptom relief. However, in areas with a higher prevalence of rheumatic fever, a 10-day course of penicillin should be prescribed. A 10-day course is recommended by the American Academy of Pediatrics,24 the American College of Physicians,23 and the IDSA.3
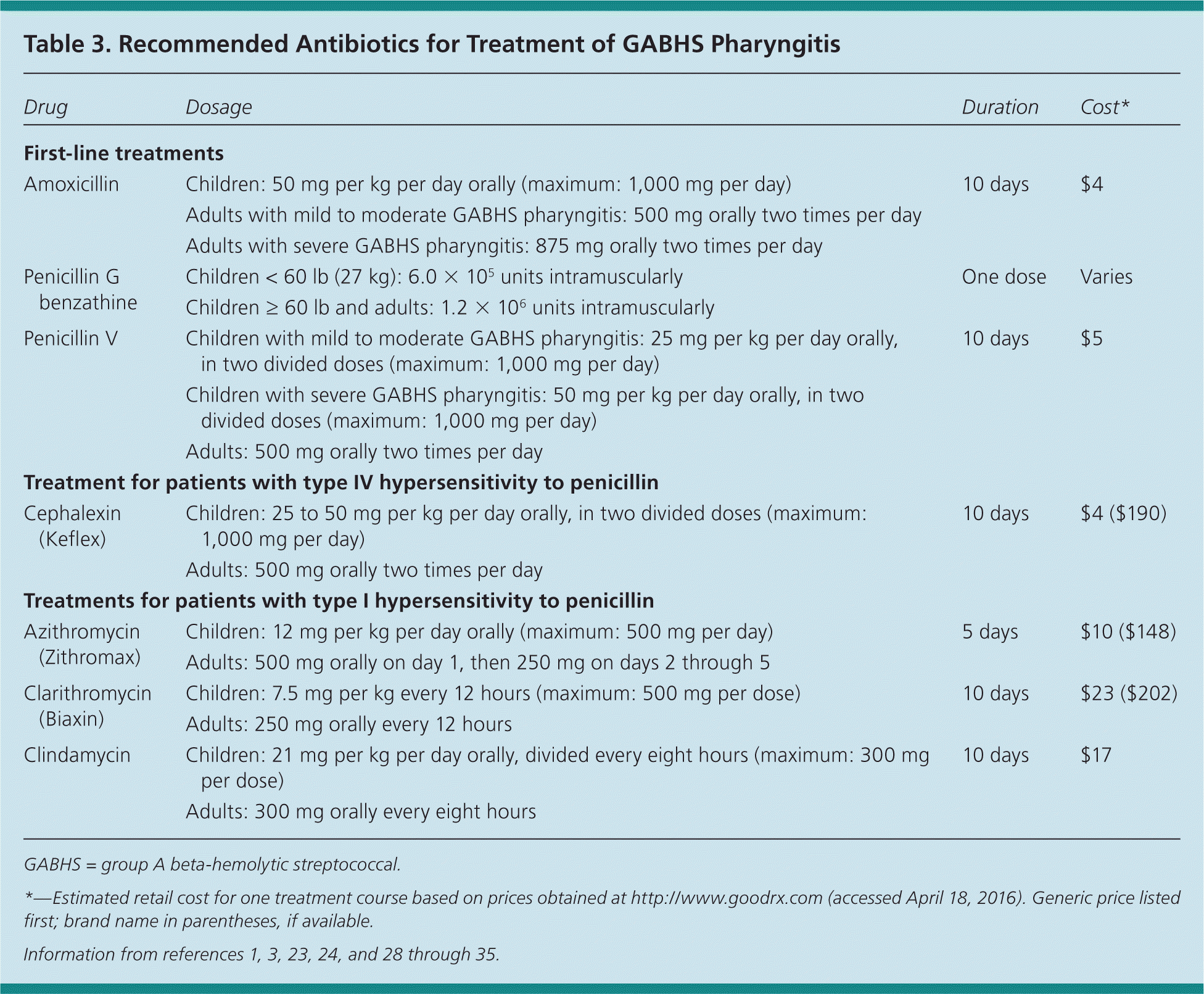
Clindamycin is a reasonable option for treating patients with type I immunoglobulin E–mediated reactions to penicillin (Table 3).1,3,23,24,28–35 Clindamycin resistance is approximately 1%.34 An oral macrolide (e.g., erythromycin, clarithromycin, or azithromycin at a dosage of 12 mg per kg per day, up to 500 mg) is also reasonable for patients with penicillin allergy. Erythromycin is associated with substantially higher rates of gastrointestinal adverse effects than other antibiotics. Antibiotic-resistant strains of GABHS infection are widespread in some areas of the world and have resulted in treatment failures. In a recent study, macrolide resistance rates among pharyngeal isolates were 5% to 8% in most areas of the United States.34 In a 2001 longitudinal study, 48% of GABHS pharyngitis isolates were resistant to erythromycin. None were resistant to clindamycin.35
| Drug | Dosage | Duration | Cost* |
|---|---|---|---|
| First-line treatments | |||
| Amoxicillin | Children: 50 mg per kg per day orally (maximum: 1,000 mg per day) | 10 days | $4 |
| Adults with mild to moderate GABHS pharyngitis: 500 mg orally two times per day | |||
| Adults with severe GABHS pharyngitis: 875 mg orally two times per day | |||
| Penicillin G benzathine | Children < 60 lb (27 kg): 6.0 × 105 units intramuscularly | One dose | Varies |
| Children ≥ 60 lb and adults: 1.2 × 106 units intramuscularly | |||
| Penicillin V | Children with mild to moderate GABHS pharyngitis: 25 mg per kg per day orally, in two divided doses (maximum: 1,000 mg per day) | 10 days | $5 |
| Children with severe GABHS pharyngitis: 50 mg per kg per day orally, in two divided doses (maximum: 1,000 mg per day) | |||
| Adults: 500 mg orally two times per day | |||
| Treatment for patients with type IV hypersensitivity to penicillin | |||
| Cephalexin (Keflex) | Children: 25 to 50 mg per kg per day orally, in two divided doses (maximum: 1,000 mg per day) | 10 days | $4 ($190) |
| Adults: 500 mg orally two times per day | |||
| Treatments for patients with type I hypersensitivity to penicillin | |||
| Azithromycin (Zithromax) | Children: 12 mg per kg per day orally (maximum: 500 mg per day) | 5 days | $10 ($148) |
| Adults: 500 mg orally on day 1, then 250 mg on days 2 through 5 | |||
| Clarithromycin (Biaxin) | Children: 7.5 mg per kg every 12 hours (maximum: 500 mg per dose) | 10 days | $23 ($202) |
| Adults: 250 mg orally every 12 hours | |||
| Clindamycin | Children: 21 mg per kg per day orally, divided every eight hours (maximum: 300 mg per dose) | 10 days | $17 |
| Adults: 300 mg orally every eight hours | |||
Which Symptomatic Treatments Are Effective for GABHS Pharyngitis?
Nonsteroidal anti-inflammatory drugs (NSAIDs) have shown the most benefit in relieving fever and pain in patients with GABHS pharyngitis.3,36 Corticosteroids shorten the duration of symptoms somewhat, but should not be used routinely to treat symptoms of GABHS pharyngitis.37 Medicated throat lozenges and topical anesthetics may alleviate throat pain but must be used frequently for patients to receive any benefit.35,38,39 Chinese herbal therapies are not effective in the symptomatic treatment of GABHS pharyngitis.40
EVIDENCE SUMMARY
The 2012 IDSA guidelines support using NSAIDs for symptomatic care in patients with GABHS pharyngitis.3 A multicenter randomized controlled trial conducted in 21 primary care centers showed that moderate doses of NSAIDs were more effective than acetaminophen and placebo in reducing fever, pain, and odynophagia (P ≤ .01).41 A 2010 systematic review involving 10 studies with 1,096 patients compared corticosteroids with placebo in patients with acute pharyngitis.37 It found that patients who received corticosteroids had a 4.5-hour reduction in pain (95% confidence interval, −7.19 to −1.89), which was not of sufficient clinical significance to support routine corticosteroid use in GABHS pharyngitis. Medicated throat lozenges are effective when used every two hours.38 Topical anesthetics containing benzocaine can be used in adults, but should be avoided in children because they can lead to methemoglobinemia.39 A 2010 Cochrane review of seven poor-quality trials with 1,253 participants concluded that Chinese herbal preparations are not effective for sore throat.40
If a Patient Has Recurrent Streptococcal Pharyngitis, Is Tonsillectomy Recommended?
Tonsillectomy is recommended for a small subgroup of patients with recurrent streptococcal pharyngitis. It should be considered in patients with a high frequency of throat infections, allergic reactions to multiple antibiotic treatments, or a history of peritonsillar abscess. Because most episodes of pharyngitis spontaneously decrease after the age of 10 years, patients should be judiciously referred for this invasive procedure.41,42
EVIDENCE SUMMARY
The American Academy of Otolaryngology–Head and Neck Surgery released a clinical practice guideline in 2011 that listed the indications for tonsillectomy.42 Tonsillectomy is recommended for patients who have had seven or more throat infections (viral or bacterial) in one year, five or more infections per year for the past two years, or three or more infections per year for the past three years. Tonsillectomy is also recommended in patients who are difficult to treat medically, including those who are allergic to multiple antibiotics. Tonsillectomy may result in multiple morbidities, including hemorrhage, delayed feeding, and fever. Up to 3.9% of patients who undergo tonsillectomy are readmitted for complications.41,42
The short-term effectiveness of tonsillectomy is minimal. A 2014 Cochrane review of seven trials and 987 participants found that patients who did not undergo tonsillectomy had 3.6 episodes of sore throat at one year after randomization compared with 3.0 episodes in patients who had surgery.43 Long-term effectiveness was harder to gauge because many patients were lost to follow-up.
Data Sources: A PubMed search was completed in Clinical Queries using the key terms streptococcal pharyngitis, Centor criteria, McIsaac score, RADT, throat culture, and treatment for streptococcal pharyngitis. The search included meta-analyses, randomized controlled trials, and reviews. Also searched were the Cochrane Database of Systematic Reviews, the Centers for Disease Control and Prevention website, Essential Evidence Plus, the online Texas A&M Library, and the U.S. Food and Drug Administration website. References from within those sources, as well as from UpToDate, were also searched. Search dates: September 15, 2014, to April 18, 2016.
This article updates previous articles on this topic by Choby1 ; Vincent, et al.44 ; and Hayes and Williamson.45
