Am Fam Physician. 2016;94(6):479-481
As published by the U.S. Preventive Services Task Force.
Summary of Recommendation and Evidence
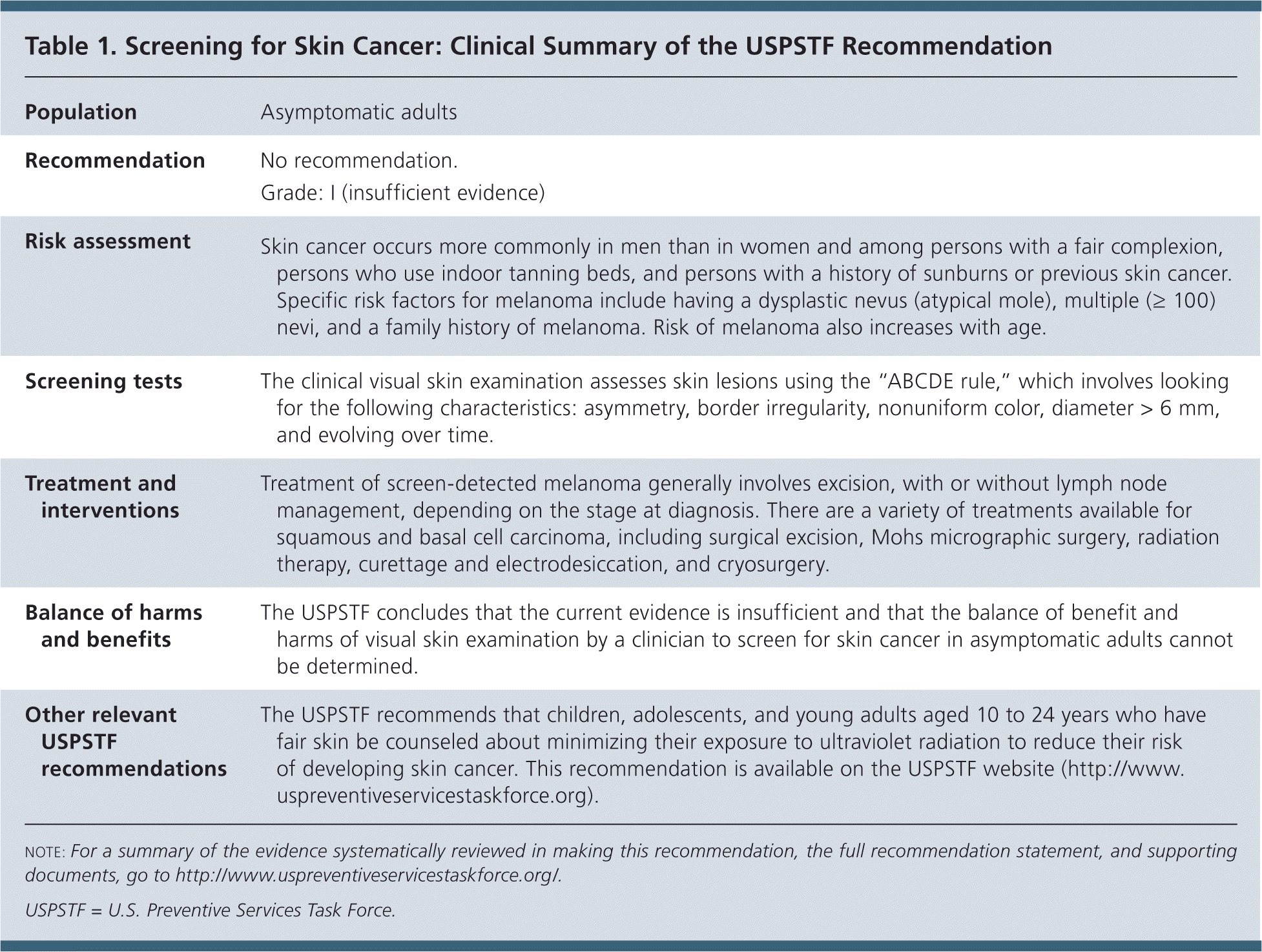
The USPSTF concludes that the current evidence is insufficient to assess the balance of benefits and harms of visual skin examination by a clinician to screen for skin cancer in adults (Table 1). I statement.
| Population | Asymptomatic adults |
| Recommendation | No recommendation. |
| Grade: I (insufficient evidence) | |
| Risk assessment | Skin cancer occurs more commonly in men than in women and among persons with a fair complexion, persons who use indoor tanning beds, and persons with a history of sunburns or previous skin cancer. Specific risk factors for melanoma include having a dysplastic nevus (atypical mole), multiple (≥ 100) nevi, and a family history of melanoma. Risk of melanoma also increases with age. |
| Screening tests | The clinical visual skin examination assesses skin lesions using the “ABCDE rule,” which involves looking for the following characteristics: asymmetry, border irregularity, nonuniform color, diameter > 6 mm, and evolving over time. |
| Treatment and interventions | Treatment of screen-detected melanoma generally involves excision, with or without lymph node management, depending on the stage at diagnosis. There are a variety of treatments available for squamous and basal cell carcinoma, including surgical excision, Mohs micrographic surgery, radiation therapy, curettage and electrodesiccation, and cryosurgery. |
| Balance of harms and benefits | The USPSTF concludes that the current evidence is insufficient and that the balance of benefit and harms of visual skin examination by a clinician to screen for skin cancer in asymptomatic adults cannot be determined. |
| Other relevant USPSTF recommendations | The USPSTF recommends that children, adolescents, and young adults aged 10 to 24 years who have fair skin be counseled about minimizing their exposure to ultraviolet radiation to reduce their risk of developing skin cancer. This recommendation is available on the USPSTF website (http://www.uspreventiveservicestaskforce.org). |
Rationale
IMPORTANCE
Skin cancer includes melanoma and basal and squamous cell carcinoma. Basal and squamous cell carcinoma, known together as nonmelanoma skin cancer, are the most common types of cancer in the United States and represent the vast majority of all cases of skin cancer (> 98%).1 However, nonmelanoma skin cancer rarely results in death or substantial morbidity (< 0.1% of patient deaths are caused by this type of cancer), whereas melanoma skin cancer has notably higher mortality rates.1 For this reason, although a visual skin examination by a clinician will detect all 3 of these cancer types, in understanding the potential benefit of screening, the USPSTF prioritized outcomes related to melanoma in developing this recommendation statement. In 2016, an estimated 76,400 U.S. men and women will develop melanoma and 10,100 will die from the disease.1
DETECTION
Evidence is adequate that visual skin examination by a clinician has modest sensitivity and specificity for detecting melanoma. Evidence is more limited and inconsistent regarding the accuracy of the clinical visual skin examination for detecting nonmelanoma skin cancer.2
BENEFITS OF EARLY DETECTION AND TREATMENT
Evidence is inadequate to reliably conclude that early detection of skin cancer through visual skin examination by a clinician reduces morbidity or mortality.
HARMS OF EARLY DETECTION AND TREATMENT
Evidence is adequate that visual skin examination by a clinician to screen for skin cancer leads to harms that are at least small, but current data are insufficient to precisely bound the upper magnitude of these harms. Potential harms of skin cancer screening include misdiagnosis, overdiagnosis, and the resulting cosmetic and—more rarely—functional adverse effects resulting from biopsy and overtreatment.
USPSTF ASSESSMENT
The USPSTF concludes that the current evidence is insufficient and that the balance of benefit and harms of visual skin examination by a clinician to screen for skin cancer in asymptomatic adults cannot be determined.
Clinical Considerations
PATIENT POPULATION UNDER CONSIDERATION
This recommendation applies to asymptomatic adults who do not have a history of premalignant or malignant skin lesions. Patients who present with a suspicious skin lesion or who are already under surveillance because of a high risk of skin cancer, such as those with a familial syndrome (e.g., familial atypical mole and melanoma syndrome), are outside the scope of this recommendation statement.
ASSESSMENT OF RISK
Skin cancer of any type occurs more commonly in men than in women and among persons with a fair complexion, persons who use indoor tanning beds, and persons with a history of sunburns or previous skin cancer. Specific risk factors for melanoma include having a dysplastic nevus (atypical mole), having multiple (i.e., ≥ 100) nevi, and having a family history of melanoma.3,4 Like most types of cancer, the risk of melanoma increases with age; the median age at diagnosis is 63 years, and the median age at death is 69 years.1
SUGGESTIONS FOR PRACTICE REGARDING THE I STATEMENT
Potential Benefit of Early Detection and Treatment. Direct evidence to assess the effect of screening with a clinical visual skin examination on the risk of death from skin cancer is limited.3 A single ecologic study (Skin Cancer Research to Provide Evidence for Effectiveness of Screening in Northern Germany [SCREEN]) with important methodological limitations suggests that a 1-time, general population-based screening program (with limited participation of 19%) combined with a disease awareness campaign may result in, at most, 1 fewer death due to melanoma per 100,000 persons over a decade.5 An independent analysis of the SCREEN population found that the observed melanoma mortality rate returned to preintervention levels after 5 years of follow-up (see Figure at http://www.uspreventiveservicestaskforce.org/Page/Document/RecommendationStatementFinal/skin-cancer-screening2#fig).6
Potential Harms of Early Detection and Treatment. Information on the harms of screening is also sparse.3 The majority of suspicious skin lesions excised during screening are not cancerous; for example, the SCREEN study found that between 20 and 55 excisions were performed to detect 1 case of melanoma, depending on patient age.7 The SCREEN study did not report the number of excisions required to prevent 1 death from melanoma, but it can be estimated at more than 4,000. Overdiagnosis and overtreatment—the diagnosis and treatment of cancer that would never have harmed the patient in the absence of screening—are other important potential harms. Ecologic evidence suggests that screening with a visual skin examination results in the overdiagnosis of skin cancer8,9; however, current evidence is insufficient to be reliably certain of the magnitude of this effect.
Current Practicex. Contemporary data on clinician practice patterns related to skin cancer screening are limited. A 2005 survey of U.S. physicians found that 81% of dermatologists, 60% of primary care physicians, and 56% of internists reported performing a full-body visual skin cancer screening examination on their adult patients.10
SCREENING TESTS
The clinical visual skin examination assesses skin lesions using the “ABCDE rule,” which involves looking for the following characteristics: asymmetry, border irregularity, nonuniform color, diameter greater than 6 mm, and evolving over time.
SCREENING INTERVAL
The optimal interval for visual skin examination by a clinician to screen for skin cancer, if it exists, is unknown.
TREATMENT
Treatment of screen-detected melanoma generally involves excision, with or without lymph node management, depending on the stage at diagnosis. There are a variety of treatments available for squamous and basal cell carcinoma (which have excellent cure rates), including surgical excision, Mohs micrographic surgery, radiation therapy, curettage and electrodesiccation, and cryosurgery, among other options.
OTHER APPROACHES TO PREVENTION
The USPSTF recommends that children, adolescents, and young adults aged 10 to 24 years who have fair skin be counseled about minimizing their exposure to ultraviolet radiation to reduce their risk of developing skin cancer.11
USEFUL RESOURCES
The Community Preventive Services Task Force has made a number of recommendations related to preventing skin cancer through the use of interventions that target child care centers; outdoor occupational, recreational, and tourism settings; primary and middle schools; and communities (available at http://www.thecommunityguide.org/cancer/index.html).
This recommendation statement was first published in JAMA. 2016;316(4):429–435.
The “Other Considerations,” “Discussion,” “Update of Previous USPSTF Recommendation,” and “Recommendations of Others” sections of this recommendation statement are available at http://www.uspreventiveservicestaskforce.org/Page/Document/UpdateSummaryFinal/skin-cancer-screening2.
The USPSTF recommendations are independent of the U.S. government. They do not represent the views of the Agency for Healthcare Research and Quality, the U.S. Department of Health and Human Services, or the U.S. Public Health Service.