Am Fam Physician. 2017;95(2):online
Related editorial: The Cholesterol Dilemma: Treating the Risk or Treating to LDL-C Goal?
Summary of Recommendations and Evidence
The USPSTF recommends that adults without a history of cardiovascular disease (CVD) (i.e., symptomatic coronary artery disease or ischemic stroke) use a low- to moderate-dose statin for the prevention of CVD events and mortality when all of the following criteria are met: (1) they are aged 40 to 75 years; (2) they have 1 or more CVD risk factors (i.e., dyslipidemia, diabetes, hypertension, or smoking); and (3) they have a calculated 10-year risk of a cardiovascular event of 10% or greater (Table 1). B recommendation.
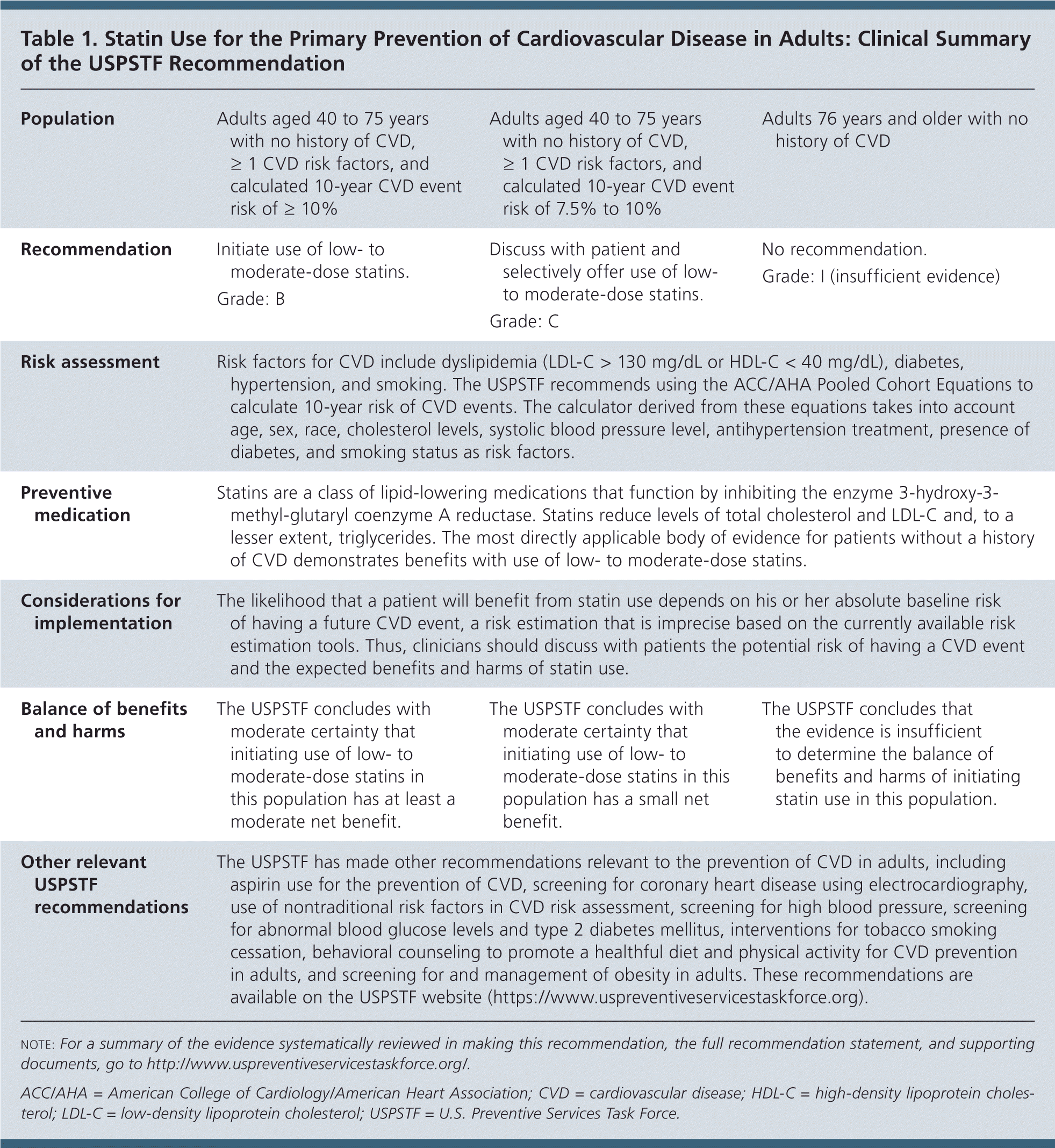
| Population | Adults aged 40 to 75 years with no history of CVD, ≥ 1 CVD risk factors, and calculated 10-year CVD event risk of ≥ 10% | Adults aged 40 to 75 years with no history of CVD, ≥ 1 CVD risk factors, and calculated 10-year CVD event risk of 7.5% to 10% | Adults 76 years and older with no history of CVD |
| Recommendation | Initiate use of low- to moderate-dose statins. | Discuss with patient and selectively offer use of low- to moderate-dose statins. | No recommendation. |
| Grade: B | Grade: C | Grade: I (insufficient evidence) | |
| Risk assessment | Risk factors for CVD include dyslipidemia (LDL-C > 130 mg/dL or HDL-C < 40 mg/dL), diabetes, hypertension, and smoking. The USPSTF recommends using the ACC/AHA Pooled Cohort Equations to calculate 10-year risk of CVD events. The calculator derived from these equations takes into account age, sex, race, cholesterol levels, systolic blood pressure level, antihypertension treatment, presence of diabetes, and smoking status as risk factors. | ||
| Preventive medication | Statins are a class of lipid-lowering medications that function by inhibiting the enzyme 3-hydroxy-3- methyl-glutaryl coenzyme A reductase. Statins reduce levels of total cholesterol and LDL-C and, to a lesser extent, triglycerides. The most directly applicable body of evidence for patients without a history of CVD demonstrates benefits with use of low- to moderate-dose statins. | ||
| Considerations for implementation | The likelihood that a patient will benefit from statin use depends on his or her absolute baseline risk of having a future CVD event, a risk estimation that is imprecise based on the currently available risk estimation tools. Thus, clinicians should discuss with patients the potential risk of having a CVD event and the expected benefits and harms of statin use. | ||
| Balance of benefits and harms | The USPSTF concludes with moderate certainty that initiating use of low- to moderate-dose statins in this population has at least a moderate net benefit. | The USPSTF concludes with moderate certainty that initiating use of low- to moderate-dose statins in this population has a small net benefit. | The USPSTF concludes that the evidence is insufficient to determine the balance of benefits and harms of initiating statin use in this population. |
| Other relevant USPSTF recommendations | The USPSTF has made other recommendations relevant to the prevention of CVD in adults, including aspirin use for the prevention of CVD, screening for coronary heart disease using electrocardiography, use of nontraditional risk factors in CVD risk assessment, screening for high blood pressure, screening for abnormal blood glucose levels and type 2 diabetes mellitus, interventions for tobacco smoking cessation, behavioral counseling to promote a healthful diet and physical activity for CVD prevention in adults, and screening for and management of obesity in adults. These recommendations are available on the USPSTF website (https://www.uspreventiveservicestaskforce.org). | ||
Identification of dyslipidemia and calculation of 10-year CVD event risk requires universal lipids screening in adults aged 40 to 75 years. See the “Clinical Considerations” section for more information on lipids screening and the assessment of cardiovascular risk.
Although statin use may be beneficial for the primary prevention of CVD events in some adults with a 10-year CVD event risk of less than 10%, the likelihood of benefit is smaller, because of a lower probability of disease and uncertainty in individual risk prediction. Clinicians may choose to offer a low- to moderate-dose statin to certain adults without a history of CVD when all of the following criteria are met: 1) they are aged 40 to 75 years; 2) they have 1 or more CVD risk factors (i.e., dyslipidemia, diabetes, hypertension, or smoking); and 3) they have a calculated 10-year risk of a cardiovascular event of 7.5% to 10%. C recommendation.
The USPSTF concludes that the current evidence is insufficient to assess the balance of benefits and harms of initiating statin use for the primary prevention of CVD events and mortality in adults 76 years and older without a history of heart attack or stroke. I statement.
CONSIDERATIONS FOR IMPLEMENTATION
To determine whether a patient is a candidate for statin therapy, clinicians must first determine the patient's risk of having a future CVD event. However, clinicians' ability to accurately identify a patient's true risk is imperfect, because the best currently available risk estimation tool, which uses the Pooled Cohort Equations from the 2013 American College of Cardiology/American Heart Association (ACC/AHA) guidelines on the assessment of cardiovascular risk,1 has been shown to overestimate actual risk in multiple external validation cohorts.2–4 The reasons for this possible overestimation are still unclear. The Pooled Cohort Equations were derived from prospective cohorts of volunteers from studies conducted in the 1990s and may not be generalizable to a more contemporary and diverse patient population seen in current clinical practice. Furthermore, no statin clinical trials enrolled patients based on a specific risk threshold calculated using a CVD risk prediction tool; rather, patients had 1 or more CVD risk factors other than age and sex as a requirement for trial enrollment.
Because the Pooled Cohort Equations lack precision, the risk estimation tool should be used as a starting point to discuss with patients their desire for lifelong statin therapy. The likelihood that a patient will benefit from statin use depends on his or her absolute baseline risk of having a future CVD event, a risk estimation that is imprecise based on the currently available risk estimation tool. Thus, clinicians should discuss with patients the potential risk of having a CVD event and the expected benefits and harms of statin use. Patients who place a higher value on the potential benefits than on the potential harms and inconvenience of taking a daily medication may choose to initiate statin use for reduction of CVD risk. The USPSTF has made several other recommendations relevant to the prevention of CVD in adults (see the “Other Approaches to Prevention” section).
PATIENT POPULATION UNDER CONSIDERATION
These recommendations apply to adults 40 years and older without a history of CVD who do not have current signs and symptoms of CVD (i.e., symptomatic coronary artery disease or ischemic stroke). Some individuals in this group may have undetected, asymptomatic atherosclerotic changes; for the purposes of this recommendation statement, the USPSTF considers these persons to be candidates for primary prevention interventions. These recommendations do not apply to adults with a low-density lipoprotein cholesterol (LDL-C) level greater than 190 mg/dL (to convert LDL-C values to mmol/L, multiply by 0.0259) or known familial hypercholesterolemia; these persons are considered to have very high cholesterol levels and may require statin use.
Rationale
IMPORTANCE
CVD is a broad term that encompasses a number of atherosclerotic conditions that affect the heart and blood vessels, including coronary heart disease, as ultimately manifested by myocardial infarction (MI), and cerebrovascular disease, as ultimately manifested by stroke. CVD is the leading cause of morbidity and mortality in the United States, accounting for 1 of every 3 deaths among adults.5
Statins are a class of lipid-lowering medications that function by inhibiting the enzyme 3-hydroxy-3-methyl-glutaryl coenzyme A reductase, which is involved in the rate-limiting step in the production of cholesterol. Statins reduce levels of total cholesterol and LDL-C and, to a lesser extent, triglycerides, and probably have anti-inflammatory and plaque stabilization effects as well.6
POTENTIAL BENEFITS OF STATIN USE
The USPSTF found adequate evidence that use of low- to moderate-dose statins reduces the probability of CVD events (MI or ischemic stroke) and mortality by at least a moderate amount in adults aged 40 to 75 years who have 1 or more CVD risk factors (dyslipidemia, diabetes, hypertension, or smoking) and a calculated 10-year CVD event risk of 10% or greater.
The USPSTF found adequate evidence that use of low- to moderate-dose statins reduces the probability of CVD events and mortality by at least a small amount in adults aged 40 to 75 years who have 1 or more CVD risk factors (dyslipidemia, diabetes, hypertension, or smoking) and a calculated 10-year CVD event risk of 7.5% to 10%.
The USPSTF found inadequate evidence to conclude whether initiating statin use in adults 76 years and older who are not already taking a statin is beneficial in reducing the incidence of CVD events and mortality.
POTENTIAL HARMS OF STATIN USE
The USPSTF found adequate evidence that the harms of low- to moderate-dose statin use in adults aged 40 to 75 years are small. Randomized, clinical trials (RCTs) of statin use for the primary prevention of CVD events have largely used low and moderate doses; under these conditions, statin use was not associated with serious adverse events such as cancer, severely elevated liver enzyme levels, or severe muscle-related harms. However, evidence concerning the association between statin use and diabetes mellitus is mixed, with 1 prevention trial suggesting that there may be a small increased risk of developing diabetes with use of high-dose statins. Myalgia is a commonly reported adverse effect of statins, but placebo-controlled trial data do not support the conclusion that statin use has a major causative role in its occurrence. Evidence for cognitive harms is relatively sparse; further research would be needed to more definitively establish the relationship between statin use and cognitive function. The USPSTF found no clear evidence of decreased cognitive function associated with statin use. These findings are consistent with those from a recent systematic review of RCTs and observational studies assessing the effect of statins on cognition that found no effect on incidence of Alzheimer disease or dementia.7 The recently published HOPE-3 (Heart Outcomes Prevention Evaluation 3) trial found that statin use increased risk of cataract surgery, which was unanticipated and not a predetermined outcome of the trial.8 None of the other primary prevention trials reported this outcome.9
The USPSTF found inadequate evidence on the harms of statin use for the prevention of CVD events in adults 76 years and older without a history of heart attack or stroke.
USPSTF ASSESSMENT
The USPSTF concludes with moderate certainty that initiating use of low- to moderate-dose statins for the prevention of CVD events and mortality in adults aged 40 to 75 years without a history of CVD who have 1 or more CVD risk factors (dyslipidemia, diabetes, hypertension, or smoking) and a calculated 10-year CVD event risk of 10% or greater has at least a moderate net benefit.
The USPSTF concludes with moderate certainty that initiating use of low- to moderate-dose statins for the prevention of CVD events and mortality in adults aged 40 to 75 years without a history of CVD who have 1 or more CVD risk factors (dyslipidemia, diabetes, hypertension, or smoking) and a calculated 10-year CVD event risk of 7.5% to 10% has a small net benefit. The decision to initiate therapy in this population should reflect an assessment of patients' specific circumstances and their preference for a potential small benefit relative to the potential harms and inconvenience of taking a lifelong daily medication.
The USPSTF concludes that the evidence is insufficient to determine the balance of benefits and harms of initiating statin use for the primary prevention of CVD events and mortality in adults 76 years and older without a history of CVD.
Clinical Considerations
RISK FACTORS FOR CVD
For the purposes of this recommendation, dyslipidemia is defined as an LDL-C level greater than 130 mg/dL or a high-density lipoprotein cholesterol (HDL-C) level less than 40 mg/dL (to convert HDL-C values to mmol/L, multiply by 0.0259). Most participants enrolled in trials of statin use for the prevention of CVD had an LDL-C level of 130 to 190 mg/dL or a diabetes diagnosis; hypertension and smoking were also common among trial participants.6 Persons with an LDL-C level greater than 190 mg/dL were usually excluded from trial participation, as it was not considered appropriate to randomly assign them to placebo. Thus, these recommendations do not pertain to persons with very high cholesterol levels (i.e., LDL-C > 190 mg/dL) or familial hypercholesterolemia, as they were excluded from most prevention trials.
One trial, JUPITER (Justification for the Use of Statins in Prevention: An Intervention Trial Evaluating Rosuvastatin), which excluded persons with dyslipidemia or diabetes, evaluated the effect of high-dose rosuvastatin vs. placebo in participants with elevated C-reactive protein (CRP) levels.10 The USPSTF previously reviewed the evidence on the utility of CRP as a risk predictor of coronary heart disease and found that although there is an association between elevated CRP levels and coronary heart disease events, there is insufficient evidence that a reduction in CRP levels results in fewer CVD events.11 Additionally, CRP is not currently included in any of the major risk prediction calculators, and the effects of using CRP in addition to traditional CVD risk factors to guide the prescription of statins for reducing CVD risk are uncertain. As such, the USPSTF does not recommend for or against the use of CRP alone as a risk factor in screening to prevent CVD events in asymptomatic adults without a history of CVD.12 In JUPITER, most of the trial participants either also had hypertension (57%) or were smokers (15%)10—risk factors the USPSTF prioritized for determining potential suitability for statin therapy. In the recent HOPE-3 trial, there was no difference in the effects of statins among participants with or without elevated CRP levels.8
10-YEAR RISK OF CVD EVENTS
The USPSTF recommends using the ACC/AHA Pooled Cohort Equations to calculate 10-year risk of CVD events.13 In 2013, the ACC/AHA released the Pooled Cohort Equations with the publication of new statin therapy guidelines.1 The calculator derived from these equations takes into account age, sex, race, cholesterol levels, systolic blood pressure level, antihypertension treatment, presence of diabetes, and smoking status as risk factors in the prediction model and focuses on hard clinical outcomes (heart attack and death from coronary heart disease; ischemic stroke and stroke-related death) as the outcomes of interest.
This risk calculator has been the source of some controversy, as several investigators not involved with its development have found that it overestimates risk when applied to more contemporary U.S. cohorts, especially those at the lower end of the risk spectrum.14 Although other risk prediction tools are available, they address varying populations, risk factors, and outcomes and have their own limitations. The ACC/AHA risk calculator is, to date, the only U.S.-based CVD risk prediction tool that has published external validation studies in other U.S.-based populations. Other advantages are that it can generate sex- and race-specific risk predictions and that it includes ischemic stroke as an outcome.
Nonmodifiable risk factors for CVD include older age, male sex, and race/ethnicity; however, statin trials have not included persons with only these risk factors. Other risk factors, such as family history of premature coronary artery disease, have not been demonstrated to improve risk prediction in a clinically meaningful way.15
It is important to note that the calculated 10-year CVD event risk derived from the ACC/AHA risk calculator is heavily influenced by age. For example, 41% of men and 27% of women aged 60 to 69 years without a history of CVD will be found to have a calculated 10-year CVD event risk of 10% or greater.16 Many older adults, particularly those aged 65 to 75 years, may meet the recommended risk threshold for treatment with statins in spite of the absence of dyslipidemia, diabetes, hypertension, or smoking. No trial data evaluated statin use among persons in this age group without CVD risk factors; thus, the evidence is insufficient to know whether statin use provides them the same or less benefit than in similarly aged adults with CVD risk factors. Decisions about initiating statin use in this age group should be based on shared decision making between clinicians and patients about the potential benefits and harms. Specific recommendations from other organizations for such individuals are discussed in the “Recommendations of Others” section.
Periodic assessment of cardiovascular risk factors from ages 40 to 75 years, including measurement of total cholesterol, LDL-C, and HDL-C levels, is required to implement this recommendation. The optimal intervals for cardiovascular risk assessment are uncertain. Based on other guidelines and expert opinion, reasonable options include annual assessment of blood pressure17 and smoking status18 and measurement of lipid levels every 5 years.1 Shorter intervals may be useful for persons whose risk levels are close to those warranting therapy, and longer intervals are appropriate for persons who are not at increased risk and have repeatedly normal levels.
SCREENING AND STATIN USE IN ADULTS AGED 21 TO 39 YEARS
The USPSTF systematically searched for evidence on the effect of screening for dyslipidemia in adults aged 21 to 39 years. It found insufficient evidence that screening for dyslipidemia before age 40 years has an effect on either short- or longer-term cardiovascular outcomes.19,20 The USPSTF found no studies that evaluated the effects of screening vs. no screening, treatment vs. no treatment, or delayed vs. earlier treatment in adults in this age group. Thus, the USPSTF recommends neither for nor against screening for dyslipidemia in this age group. A separate recommendation statement also found insufficient evidence to assess the balance of benefits and harms of screening for dyslipidemia in children and adolescents.21
The USPSTF recognizes the rationale for screening for dyslipidemia in adults aged 21 to 39 years to identify those at risk for the development of early atherosclerosis, including those with familial hypercholesterolemia. Unfortunately, the evidence is lacking in this age group. The USPSTF found 4 trials of statin use for primary prevention that enrolled patients younger than 40 years. However, results were not reported separately for this age group, and it comprised a small part of the overall population.19,20 One cohort study compared the effects of statins vs. no statins for the treatment of familial hypercholesterolemia.22 However, the mean age of patients in this study was 44 years. Given the lack of data on the efficacy of screening for or treatment of dyslipidemia in adults aged 21 to 39 years, the USPSTF encourages clinicians to use their clinical judgment for patients in this age group.
STATIN USE IN ADULTS AGED 40 TO 75 YEARS
Nineteen RCTs evaluated the effects of statins vs. placebo or no statins in adults aged 40 to 75 years without known CVD. Most of the trials, including the recently published HOPE-3 trial,8 enrolled participants based on an elevated LDL-C level, a diabetes diagnosis, or at least 1 CVD risk factor. Use of low- or moderate-dose statins was associated with a reduced risk of all-cause mortality (pooled risk ratio [RR], 0.86 [95% CI, 0.80 to 0.93]), cardiovascular mortality (RR, 0.69 [95% CI, 0.54 to 0.88]), ischemic stroke (RR, 0.71 [95% CI, 0.62 to 0.82]), heart attack (RR, 0.64 [95% CI, 0.57 to 0.71]), and a composite cardiovascular outcome (RR, 0.70 [95% CI, 0.63 to 0.78]).6
Among the study populations, the proportion of CVD events prevented (i.e., the relative risk reduction) was similar across age, sex, race/ethnicity, lipid level, and other risk factor categories.6 Among trials that stratified participants according to a baseline global cardiovascular risk score, similar relative risk estimates were observed among those classified at a higher vs. lower CVD event risk.10,23
Given similar relative risk reductions, the absolute magnitude of benefit that an intervention with demonstrated efficacy can have in a specific population directly depends on the incidence of disease over time in that population. In other words, the more likely it is that persons in a certain population will have a heart attack or ischemic stroke, the greater the potential reduction in the number of CVD events with statin use will be in that population. This is one of the fundamental reasons for the distinction between a grade B and C recommendation for the population that presents with dyslipidemia, diabetes, hypertension, or smoking and a 10% or greater vs. 7.5% to 10% 10-year CVD event risk.
In the absence of other risk factors, adults with an LDL-C level greater than 190 mg/dL may still fall below the risk threshold for statin use for CVD prevention. As noted previously, these persons were generally excluded from the prevention trials evaluating the effects of statin use on health outcomes, because expert opinion strongly favors intervention for these individuals. It is possible that the relative risk reduction in this group is higher than in adults with a lower LDL-C level and that the absolute benefit is greater than would be predicted from a risk calculator.24
DOSAGE
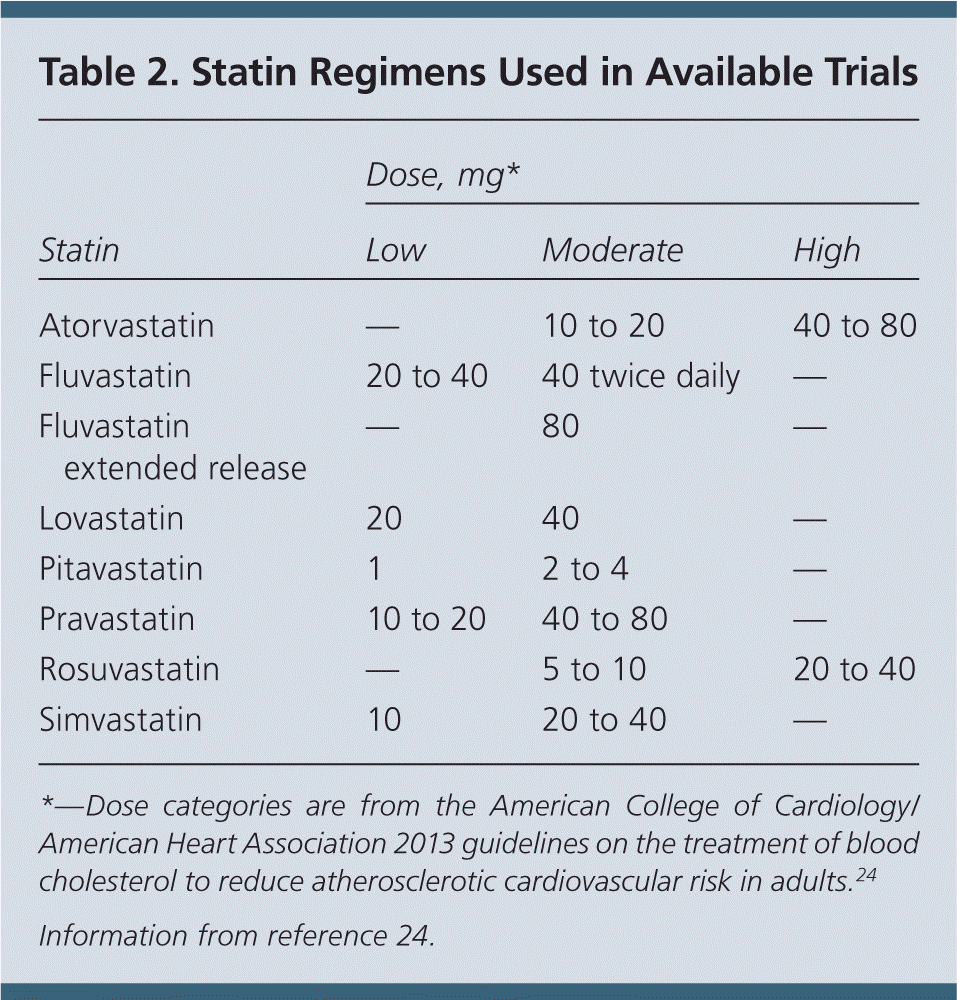
As previously noted, available RCTs evaluating statins for the prevention of CVD events largely used low and moderate doses. There were no clear differences in estimates of effect when the trials were stratified according to statin dose (see Table 224 for the drug regimens used in the available trials). The Cholesterol Treatment Trialists meta-analysis showed that greater degree of LDL-C reductions achieved were associated with proportional reductions in major cardiovascular events.25 However, these analyses were based not on randomized comparisons but the degree of LDL-C reduction achieved. The degree of cholesterol reduction may be attributable, in part, to interindividual variability in response to statins, not just statin dosage.
| Dose, mg* | |||
|---|---|---|---|
| Statin | Low | Moderate | High |
| Atorvastatin | — | 10 to 20 | 40 to 80 |
| Fluvastatin | 20 to 40 | 40 twice daily | — |
| Fluvastatin extended release | — | 80 | — |
| Lovastatin | 20 | 40 | — |
| Pitavastatin | 1 | 2 to 4 | — |
| Pravastatin | 10 to 20 | 40 to 80 | — |
| Rosuvastatin | — | 5 to 10 | 20 to 40 |
| Simvastatin | 10 | 20 to 40 | — |
Limited information is available about use of high-dose statins in a primary prevention population. As such, the harms of statin use for the prevention of CVD events in adults aged 40 to 75 years can only be bounded as small for low- or moderate-dose statins. There may be individual clinical circumstances that warrant consideration of high-dose statin use; decisions about dose should be based on shared decision making between patients and clinicians. However, the most directly applicable body of evidence for patients without a history of CVD demonstrates benefits with use of low- to moderate-dose statins.
Available information about use of high-dose statins in a prevention population comes from the JUPITER trial. The trial found an increased risk of physician-reported incident diabetes with statin use compared with placebo after 2 years of follow-up (3.2% vs. 2.4%; RR, 1.25 [95% CI, 1.05 to 1.49]), which was not reported in trials evaluating use of moderate- or low-dose statins.10 Post hoc analysis subsequently suggested that many of the diabetes cases in JUPITER may have occurred in participants who had other risk factors for diabetes at baseline (e.g., impaired fasting blood glucose or obesity).26
SUMMARY
The incidence of CVD events in a population increases linearly with CVD risk level; there is no threshold at which event rates abruptly escalate. As such, any cut point for assessing where the net benefit of statin use shifts from small to moderate for a population requires judgment. Evidence indicates that currently available risk calculators tend to overestimate CVD risk, suggesting that actual benefits may be lower than estimated. Issues to consider include the uncertainty of current risk prediction methods, the overall probability of CVD events occurring in the population, the known and unknown associated harms of statin use, and patient preferences.
The USPSTF concludes that adults who smoke or have dyslipidemia, diabetes, or hypertension and a 10% or greater 10-year CVD event risk should be offered a low- to moderate-dose statin. Adults with diabetes or dyslipidemia and a 20% or greater 10-year CVD event risk are most likely to benefit from statin use.
Clinicians may selectively offer adults who smoke or have dyslipidemia, diabetes, or hypertension and a 7.5% to 10% 10-year CVD event risk a low- to moderate-dose statin. Fewer persons in this population will benefit from the intervention, so the decision to initiate use of low- to moderate-dose statins should reflect shared decision making that weighs the potential benefits and harms, the uncertainty about risk prediction, and individual patient preferences, including the acceptability of long-term use of daily medication.
SUGGESTIONS FOR PRACTICE REGARDING THE I STATEMENT FOR INITIATING STATIN THERAPY FOR PRIMARY PREVENTION IN ADULTS 76 YEARS AND OLDER
Potential Preventable Burden. Adults 76 years and older were not included in any of the randomized trials of statin use for the primary prevention of CVD.6 Thus, understanding of the potential benefits of initiating statin use for primary prevention in this age group is limited.
Potential Harms. Evidence on the potential harms of statin use for the primary prevention of CVD events in adults 76 years and older is very limited. Observational evidence suggests there may be an association between very low cholesterol levels and an increased risk of mortality with advanced age, after adjusting for other risk factors.27,28
Current Practice. The most current data from the National Health and Nutrition Examination Survey indicate that nearly half (47.6%) of adults 75 years and older in the United States use prescription cholesterol-lowering medications. The majority (> 80%) use a statin alone.29 The survey did not distinguish between the use of cholesterol-lowering medications for the purposes of primary vs. secondary prevention, so it is not possible to determine how many of these persons have had a previous heart attack or ischemic stroke. Another study using data from the Medical Expenditure Panel Survey, which did allow for the differentiation of individuals with and without vascular disease (defined as coronary heart disease, stroke, or peripheral vascular disease), found that the rate of statin use among adults 80 years and older for the purposes of primary prevention increased from about 9% in 1999–2000 to 34% in 2011–2012.30
The Society for Post-Acute and Long-Term Care Medicine, as part of the Choosing Wisely campaign, highlighted the use of cholesterol-lowering medications in adults with limited life expectancy (i.e., 70 years and, most particularly, 85 years and older) among its “10 Things Physicians and Patients Should Question” because of the increased likelihood of an overall unfavorable risk-to-benefit ratio.31
OTHER APPROACHES TO PREVENTION
The USPSTF has made other recommendations relevant to the prevention of CVD in adults, including aspirin use for the prevention of CVD,32 screening for coronary heart disease using electrocardiography,33 use of nontraditional risk factors in CVD risk assessment,12 screening for high blood pressure,17 screening for abnormal blood glucose levels and type 2 diabetes mellitus,34 interventions for tobacco smoking cessation,18 behavioral counseling to promote a healthful diet and physical activity for CVD prevention in adults,35 and screening for and management of obesity in adults.36
This recommendation statement was first published in JAMA. 2016; 316(19):1997–2007.
The “Other Considerations,” “Discussion,” “Update of Previous USPSTF Recommendation,” and “Recommendations of Others” sections of this recommendation statement are available at https://www.uspreventiveservicestaskforce.org/Page/Document/UpdateSummaryFinal/statin-use-in-adults-preventive-medication1.
The USPSTF recommendations are independent of the U.S. government. They do not represent the views of the Agency for Healthcare Research and Quality, the U.S. Department of Health and Human Services, or the U.S. Public Health Service.