
The jury's still out on how hospitalists affect patient care, but many family physicians are choosing to give up hospital service before the verdict comes in.
Fam Pract Manag. 1998;5(10):54-62

At the 1997 AAFP Congress of Delegates, the hospitalist movement was a hot topic. Many family physicians saw it as a threat to their scope of practice, the identity of the profession and the care of their patients. The Academy responded to its delegates' concerns by appointing a task force of family physicians to study the issue.
One year later, thanks in large part to surveys and other research conducted by this task force, the movement's real impact on family physicians is better understood. We now know that family physicians are still managing the inpatient care of a majority of their hospitalized patients, that they expect to continue and that only a small percentage of them have been excluded from providing inpatient care. But a lot of unanswered questions remain, and with them, plenty of challenges for family physicians and the specialty.
Is there a larger issue?
The more pressing issue for the specialty might well be the number of family physicians who have chosen not to provide inpatient care. Some 27 percent of family physicians responding to an Academy survey reported that the percentage of hospitalized patients they care for personally had changed in the last year. Of these respondents, more than three-fourths indicated that the change was voluntary or partly voluntary (see “Selected data from the AAFP inpatient care survey”).
Responses to a February 1998 letter to AAFP members from then-president Neil Brooks, MD, which solicited opinions about the hospitalist concept, provided another indication that family physicians' attitudes about inpatient care are changing. The largest group of the 273 respondents, 40 percent, indicated that they were “supportive ... with some concerns.” Thirty-three percent opposed the concept, and the remainder were neutral.
Why do family physicians like this concept, and why are so many choosing not to manage the care of their own hospitalized patients?
“I think the motive is convenience,” says family physician James Cotter, MD, physician in charge of the Napa medical offices for Kaiser Permanente of Northern California. “By and large, these doctors have chosen to focus their work in the clinic and have more predictable hours. We've seen this in a number of surveys. The hospitalist movement is not being driven by economics, it's being driven by doctors' lifestyle preferences.” Two-thirds of the family physicians in Cotter's system opted out of inpatient care when a hospitalist system was instituted there.
But is this phenomenon really new? “We've been using rotating inpatient services for call sharing as a matter of convenience for 20 years, and now we've given these systems a name. I've sometimes wondered what the big deal is,” says Bruce Bagley, MD, of Latham, N.Y., who chaired the Academy's Task Force on Hospitalists and recently became AAFP president-elect.
Some important differences between the hospitalist movement and the historic use of rotating inpatient services by family physicians help to explain why the concept is now a hot issue. For one, managed care organizations (MCOs) are designing and instituting the systems now, not just physician groups; and they're doing it primarily to control costs, not to safeguard the private time of the physicians they contract with. At the same time, the economics of managed care practice is making it harder for family physicians to provide inpatient care — and the design of some inpatient care models makes it impossible.
Selected data from the AAFP inpatient care survey
The AAFP Task Force on Hospitalists surveyed 4,800 Academy members this summer about inpatient care management models that might be affecting them, their patients and their practices. The sample survey drew a response rate of 45.6 percent. Note that in the graphs below, “patients” refers to adult general-medicine patients.
In the last 12 months, have you been excluded from managing inpatient care for your hospitalized patients by a managed care organization or by any organization with which you are professionally affiliated?
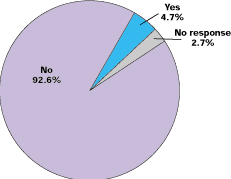
How did the percentage of your hospitalized patients managed by you change over the past 12 months?
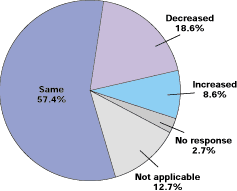
Note: When asked how they anticipate this percentage might change in the next 12 months, 62.5 percent of respondents said they thought it would stay the same, 11.9 percent thought it would decrease, and 11.0 percent thought it would increase.
Source: AAFP survey “Family Physicians and Inpatient Care”; 1998.
Ready, willing and unable
“Our surveys did suggest that some physicians are not being given the option of taking care of their patients in the hospital, and that's certainly disturbing,” says Bagley. But he emphasizes that requiring physicians to hand off the care of their patients to hospitalists remains uncommon.
Eleven of 15 physician leaders in major national MCOs and integrated delivery systems who responded to a recent AAFP survey indicated that their organizations had begun using hospitalists. The dominant model is one in which family physicians can choose to use hospitalists' services, although some of the respondents reported that they require hand-offs to hospitalists.
“If our members are qualified and trained and willing to take care of patients in the hospital but are being excluded, we should fight that with the same energy we've devoted to other hospital privileging issues,” says Bagley. The AAFP has adopted a policy advocating that the decision about whether to provide inpatient care should be left to individual physicians.
Family physicians who opt out of inpatient care also stand to lose hospital privileges. Moreover, AAFP survey findings suggest that some family physicians have had trouble with MCO credentialing because of their lack of privileges — a consequence that could make it difficult for family physicians in some markets to maintain a viable outpatient practice.
It's too soon to tell whether recredentialing will also pose a problem for family physicians who have lost hospital privileges. “Hospitalist systems have been around just long enough that we're starting to see physicians who need to be recredentialed who haven't actually been to the hospital in a couple of years,” Cotter says. “Some systems are trying to work around that by creating categories of privileges that keep you on staff, but you aren't actually admitting to the hospital. I think that will eventually be worked out. There are too many doctors affected for it not to be.”
Bagley agrees and predicts that, like obstetrics, inpatient care will continue to be part of the scope of family practice for most of the family physicians who desire it. The Academy's semiannual practice profile survey shows that in 1998, 86 percent of family physicians have hospital privileges. Bagley says the AAFP will continue to monitor that statistic closely.
Encouraging choice
Some family physicians are more concerned. “I think health plans will continue experimenting with the hospitalist model, based on anticipated reductions in service utilization and length of stay,” says Marc L. Rivo, MD, MPH, a member of the Task Force on Hospitalists and medical editor of Family Practice Management. AvMed, the Miami-area health plan for which Rivo is medical director, is in the process of instituting a hospitalist model of its own.
Rivo says it's not enough to ensure that family physicians can choose whether to participate in inpatient care services; family physician leaders must also work to ensure that the choice is an attractive one. “In many systems, there is an economic incentive to spend more time in the outpatient setting and an economic disincentive to follow your own patients, and that's helping to drive this movement,” Rivo explains. “We have to advocate for compensation systems that don't discourage family physicians from providing inpatient care.”
Rivo also stresses that family physicians should try to be involved in designing inpatient care systems to preserve their own interests and those of their patients. Where hospitalist systems do exist, the family physician can play an important role in ensuring that the principles of family medicine — such as communication, attentiveness to psychosocial issues and, to the extent possible, continuity of care — are perpetuated. To that end, the task force developed "Guidelines for Interaction in Hospitalist Models" for use by family physicians.
“Guidelines for Interaction in Hospitalist Models”
The following guidelines were developed by the AAFP Task Force on Hospitalists and approved by the Academy's Board of Directors. The guidelines, the AAFP policy statement on “Hospitalist Systems of Inpatient Care Management” and other information from the task force are available to members on request by calling the AAFP Order Department at 800–944–0000 and asking for reprint 708.
The overarching objective for all should be the best possible care for the patient.
At the request of the family physician (or other primary care physician), the inpatient care physician (who may also be a family physician) should admit and coordinate the care of all patients admitted to the hospital regardless of the admitting diagnosis or type of insurance coverage.
If patients present to the emergency department (ED) and the ED physician assesses them, the ED physician should then contact the patient's family physician to determine if admission is necessary or if close follow-up or outpatient workup is more appropriate.
If admission is necessary, the family physician should communicate information on pre-hospital treatment, workup, co-morbidities and ongoing specialty consultations, along with family and social concerns, advanced directives, etc., to the inpatient care physician who is assuming management of the patient's care.
The inpatient care physician will assess the patient at admission and determine the best course of treatment. This may include treat and release, admit for general medical management, or admit for medical or surgical subspecialty care while providing general medical oversight.
During the period of hospitalization, decisions regarding care, consultation, admission, transfer and discharge should be the sole responsibility of the inpatient care physician in consultation with the patient and, as appropriate, the patient's family physician and/or family members.
The inpatient care physician should be readily available to discuss the patient's medical problems and hospital course with the family and should provide timely updates to the family physician designated by the patient. Communication with the family physician is extremely important at the time of any changes in the patient's status, complications or new diagnoses (e.g., cancer).
The inpatient care physician should communicate the treatment plan and follow-up recommendations to the patient's family physician or the covering physician on the day of discharge. This may be best accomplished by having the discharge summary dictated and faxed to the family physician.
When family physicians refer their hospitalized patients to the care of an inpatient physician, the AAFP strongly encourages them to maintain ongoing communication with the patients and their families throughout the hospitalization. Family physicians should also provide written communication to the inpatient care physician after the first post-hospital visit at the office where there may be an educational benefit.
Health care systems that utilize inpatient care management models should seek to constantly monitor and improve their processes through the use of ongoing surveys for patient and physician satisfaction with the system. Data on health care outcomes is essential to the ultimate evaluation of these models.
Training for hospital practice
Another point of concern is whether family physicians feel adequately prepared to treat hospitalized patients in an environment dominated by increasingly sick patients.
The task force surveyed almost 500 family practice residency directors to determine whether they believe their recent graduates could function comfortably in various inpatient care roles. Ninety- eight percent agreed that their graduates would be comfortable “managing virtually all their own inpatient care,” and the same percentage of respondents agreed that graduates would be comfortable caring for their own and those of other physicians in their groups on a rotating basis. More than three-fourths said their graduates would be comfortable functioning as full-time hospitalists.
The task force determined that no different or added training would be necessary for the residency-trained family physician to be able to function as an inpatient attending physician.
Gerald Hejduk, associate director of the AAFP's Residency Assistance Program and staff executive for the task force, says a number of family practice residency programs are providing inpatient care management services for physicians in their communities who no longer admit or take care of their own hospitalized patients.
Ronald Goldschmidt, MD, who directs a family practice inpatient service affiliated with the University of California- San Francisco (UCSF) and based in a county hospital, says this model has worked well there for 19 years. “We can provide our residents with excellent training in inpatient care, be especially attentive to the needs of family physicians in outlying areas at the same time, and ensure that patients get the kind of care they're accustomed to from their regular family physician,” he says.
The task force also reviewed the AAFP's CME programming with inpatient care in mind. The group concluded that because hospitalization is just one stage in the continuum of caring for a patient, designing or designating inpatient-care-specific CME would “artificially fragment” the educational content, says Hejduk. The group reached no conclusions about what kind of CME a family physician who was functioning solely as a hospitalist would need, according to Hejduk.
Lingering concerns about outcomes
Other questions about the hospitalist model remain unanswered, most having to do with its effects on the quality of care. This is a point of frustration for many family physicians, Bagley says. The best way to ensure that inpatient care will always be part of family practice would be to prove that it's in patients' best interests to have family physicians there, he says. Continuity of care, the cornerstone of family medicine, is perhaps the most logical argument against hospitalist systems, but its value has yet to be proven.
John M. Eisenberg, MD, MBA, an internist and administrator of the Agency for Health Care Policy and Research (AHCPR), emphasized the need for more research in his keynote address at the National Association of Inpatient Physicians' (NAIP) first conference last April. Eisenberg acknowledged that the concept has potential, but he urged health care systems not to adopt widespread organizational change with less evidence than would be required for a new drug or technology. AHCPR hopes to help fill the gap, he says, although the agency has not yet funded any studies to examine the clinical outcomes of hospitalist systems.
Several large health care organizations, including Kaiser Permanente of Northern California and Park Nicollet Clinic of HealthSystem Minnesota in Minneapolis, have conducted their own internal hospitalist research. Overall, studies tend to report changes that lead to cost savings.
Cotter says that one of the best indications Kaiser has of the effect of a hospitalist system on clinical quality is that its system has increased the use of clinical guidelines and made their use more consistent. “Our care is more alike than it has ever been,” Cotter says.
Longitudinal studies that examine clinical outcomes across the continuum of care are expensive and fraught with difficulties. The large MCOs that have the capital and infrastructure to carry out this kind of research have thus far examined the results of hospitalist systems in a more limited way. “The quality data are lacking, and the cost data are really very weak,” Goldschmidt says. “But large health systems will eventually do the work.”
In the meantime, peer reviewed studies of hospitalist systems are scarce, and because no two systems are alike, it's difficult to make generalizations based on existing research. (See “Suggested reading.”)
What it means to patients
Goldschmidt says patient satisfaction implications deserve more attention than they've been given. Cotter reports that Kaiser has examined patient satisfaction with hospitalist models and found no significant difference between satisfaction among patients treated in facilities with hospitalist programs and those treated in facilities without them. And Park Nicollet has reported that there were no statistically significant changes in the results of patient satisfaction surveys conducted before and after its inpatient service was established.
But neither organization specifically asked patients whether they'd have preferred to have their personal physicians manage their hospital care. In findings published in the proceedings of a national conference on hospitalists sponsored by the UCSF last December, Richard Freese, MD, senior vice president of Park Nicollet Clinic, wrote, “It is our experience that if 200 patients are asked whether they prefer their personal physician attend them in the hospital, 200 patients reply in the affirmative. If, however, one asks numerous other questions about the quality of their care and satisfaction, there is no difference.”
The Park Nicollet research also reported on outpatient satisfaction before and after the inpatient service was implemented. Statistically significant differences included “improved perception of ease in making appointments,” decreased waiting time in the exam room and in the internal medicine department, improved “advice for preventive care” and improved overall quality of care. Freese wrote that the increases in satisfaction were attributable to “the more reliable availability of the outpatient physicians to expand their hours and be on time with their first appointments.”
Goldschmidt says studies show that patients in his program are satisfied with hospitalists, too, and he says that family physicians have to come to terms with such results. “To fight it seems fruitless,” he says. “But just because patients are satisfied with hospitalists doesn't mean that can be the only system of care. The studies have addressed the general question of whether patients can be satisfied with a hospitalist, but they haven't shown that to be a preference.”
What it means to internists
As potentially divisive as the hospitalist issue is for family physicians, it may pose an even greater dilemma for internists. Prominent internists — including Steven Schroeder, MD, president of the Robert Wood Johnson Foundation, and Harold C. Sox, MD, of Dartmouth Medical School and president of the American College of Physicians-American Society of Internal Medicine (ACP-ASIM) — have said more research is needed and have worried aloud that the movement will lead to an additional blurring of the identity of internal medicine in the eyes of patients, would-be internists in medical school and health plans.
In the proceedings of the UCSF conference last winter, Sox wrote that “internal medicine has invested a great deal to assert its identity as a specialty that cares for the sickest patients in the community in whatever setting they need care,” referring to the ACP's recent public-awareness campaign and three-year project to define the curriculum of internal medicine residencies and identify the competencies of the general internist. Sox fears that the “involuntary” hospitalist model would divide internal medicine and that the larger of the two groups, outpatient internists, would “have less to distinguish themselves from nurse practitioners, family physicians and independent-practice nurses.”
Also at the UCSF conference, Mark Kelley, MD, chair of the American Board of Internal Medicine, said he doesn't believe that hospitalist practice constitutes another subspecialty within internal medicine. He said that hospitalists do not appear to claim unique knowledge or medical skill, the role doesn't require additional training and it's a “mistake to judge the legitimacy of a discipline by its popularity.”
Suggested reading
The articles listed below are among those used by the AAFP Task Force on Hospitalists to research the use of hospitalists and family physicians' inpatient care roles. To date, only a few articles in the clinical literature address the hospitalist model specifically.
From the clinical literature
From Family Practice Management
The supply of hospitalists
Despite what seems to be a growing skepticism about the hospitalist movement, the NAIP has progressed over the past year from a fledgling operation to an association with offices, an annual conference, a board of directors, a web site (http://www.hospitalmedicine.org/) and plans for a pediatric section. But the NAIP might not be quite as powerful as it sounds. The association is in the midst of a membership drive to convert the people on its mailing list of 2,000 into dues-paying members. And the NAIP is receiving administrative and financial support from ACP-ASIM in exchange for granting ACP-ASIM approval rights for NAIP's bylaws, budget, policy statements and some of its activities. But under the three-year agreement, NAIP remains a distinct organization; not all its members are internists.
What's next?
Although the future of the hospitalist movement is uncertain, it is forcing some family physicians to make very important and difficult choices. In its policy statement on hospitalists, the AAFP cautions family physicians to “strongly consider the mid- and long-range implications for their practices before they relinquish hospital privileges.”
Complicating family physicians' decisions about their inpatient care roles is the changing role of the hospital itself. In his speech at the UCSF conference, Schroeder commented that “the hospital is a shrinking corpus” and cited a litany of information to suggest that the number and importance of hospitals as we know them will continue to diminish.
In that scenario, the family physician who is a skilled diagnostician and healer with the expertise to coordinate the provision of a wide range of subspecialty services in a complex maze of focused-care facilities will be a valuable commodity.
But the choice is not just about economics or personal satisfaction. “Family physicians also should consider what's best for their patients. And without any solid information about outcomes, they'll have to base that decision on what they personally believe,” says Rivo.
More observations on the hospitalist movement
“It bears close monitoring, not least of all because it marks the first time that creation of a new specialty has been driven not by a new disease (like AIDS), or new knowledge or technology, but by organizational and financial priorities.”
Steven A. Schroeder, MD, internist and president of the Robert Wood Johnson Foundation, in the proceedings of “The Emerging Role of Hospitalists in American Health Care: A National Conference,” December 1997.
“Cradle to grave? Sure. As long as it happens from 9 a.m. to 5 p.m., and the patient can come to the office.”
Robert G. Brown, MD, of the McLennan County Family Practice Residency Program in Waco, Texas, writing in American Family Physician (1998;58(2):339–340).
“Angioplasty is sexy. Swan-Ganz catheters are sexy. Putting a needle in someone's pericardium to relieve cardiac tamponade is sexy. Increasing the Naprosyn dose? Not sexy. ... My cynical outlook is that general internists, who for a generation now have tried to figure out a way to make themselves sexy, have finally found a way. ... Anytime you can say the word ‘stat’ in a sentence, you're sexy.”
Mark Smith, MD, MBA, internist and president of the California Health Care Foundation, speaking at “The Emerging Role of Hospitalists in American Health Care: A National Conference,” December 1997.
“Residency time spent in the hospital is a ridiculous use of our educational resources. We need to ask why family medicine residents spend so much of their training time focused on hospital care when that is such a small part of what they will do in practice.”
Vance Brown, MD, director of the family medicine residency program at the University of Massachusetts Medical Center in Worcester, from a debate at the annual meeting of the Society of Teachers of Family Medicine and published in Family Practice News (July 1, 1998:9).
“Particularly with increasing life-prolonging technology, and the ethical difficulties posed by the controversies concerning resuscitation, prolongation of dying and assisted suicide, it becomes more important than ever that someone who knows that patient over a period of time be instrumental in decisions ... about the end of life. Unfortunately, patients have become strangers. ... This may be more a criticism of modern medicine as a whole, but the argument certainly may achieve its most dramatic expression within the context of the hospitalist movement.”
Faith T. Fitzgerald, MD, program director of internal medicine at the University of California at Davis, writing in Medical Tribune (Aug. 13, 1998:7).
“Continuity of care has already been so disrupted in many settings that the further disruption of a shift to a hospitalist system may not be noticeable.”
Barry G. Saver, MD, MPH, and Mark P. Doescher, MD, MSPH, of the Department of Family Medicine, University of Washington, Seattle, writing in The Journal of Family Practice (1998;46(6):465–468).