
Fam Pract Manag. 2001;8(5):22-23
Family practice match numbers drop again
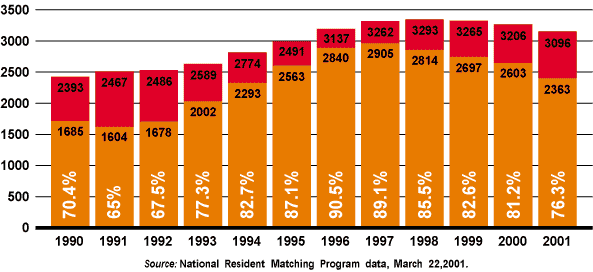
The number of positions filled in family practice residency programs dropped in 2001 for the fourth consecutive year, according to preliminary data from the National Resident Matching Program (NRMP). Of the 3,096 positions offered this year, 76.3 percent were filled; 49 percent were filled by U.S. seniors.
Family practice isn't the only specialty facing declining fill rates; all primary care specialties experienced a drop this year. Meanwhile, obstetrics/gynecology, anesthesiology, diagnostic radiology and emergency medicine all saw increases.
According to the NRMP, today's medical students may be more attracted to the lifestyles of some subspecialties that have fewer external pressures and higher financial rewards than primary care, a trend AAFP President Richard Roberts, MD, JD, calls disturbing. “America's population continues to grow, but with fewer students choosing family practice, the number of family physicians won't keep up. The result will be more subspecialists trained to care for individual health problems – but not enough doctors trained to care for the whole person, or the whole family,” said Roberts.
The four-year decrease in family practice fill rates comes after a six-year, record-setting increase that ended in 1998.
HIPAA privacy rules take effect
After a two-month delay, the privacy rules of the Health Insurance and Portability Act (HIPAA) took effect April 14. Health care providers and insurers will have two years to comply with the rules, which seek to protect the privacy of patients' medical records. The Bush administration had considered delaying the privacy rules to consider health care industry objections that the standards would impose costly administrative burdens. Instead, the administration plans to modify or revise some parts of the rules as guidelines for implementation are developed. “There has to be some fix-up of the rules to inject a greater degree of common sense,” said Health and Human Services Secretary Tommy G. Thompson in the April 13 New York Times. For more information about the HIPAA privacy rules, see “What You Need to Know About HIPAA Now,” FPM, March 2001, p. 43, available online at www.aafp.org/fpm/20010300/43what.html.
PRACTICE PEARLS from here and there
Ask “why” five times
When faced with a problem in your organization, don't try solving it until you've identified the root cause by asking “why” five times. If you fail to dig deeply enough, you could waste your time treating mere symptoms.
For example, a practice faced with an angry patient might ask the following:
Why is the patient angry? Because he was prescribed a new drug that interfered with his other medications.
Why was he prescribed a new drug that interfered with his other medications? Because the medical team did not have a complete list of his current medications.
Why didn't the medical team have a complete list of his current medications? Because the patient had not been asked about his current medications.
Why wasn't the patient asked about his current medications? Because the nurse and the physician each assumed the other had asked.
Why did the nurse and physician assume the other person had asked? Because they had not explicitly agreed on which elements of the patient's history the nurse would collect.
– Improvement tip: ask “why” five times to get to the root cause. Continuous Improvement newsletter. Boston: Institute for Healthcare Improvement; April 2001.
PRACTICE PEARLS from here and there
Improving the history and exam
An accurate diagnosis depends on an effective physical exam and history. To brush up your skills try the following tips:
Control the environment: The room should have the lights turned up and the door or curtain closed for quiet and privacy.
Build rapport: Know the patient's name when you enter the room, ask the patient's permission to begin the exam and then ask questions and listen.
Think global: Ask about factors in the patient's life that could influence his or her health, such as travel, sports, hobbies, family history, pets and diet.
– Kelly C. Good diagnostic skills should begin at the bedside. ACP-ASIM Observer. February 2001:7.
PRACTICE PEARLS from here and there
Warning! Poor employee performance
Documenting an employee's poor performance is important because it gives the employee a chance to improve and helps build your defense should the employee be fired and ever take you to court. Here's the correct way to write a warning:
State the problem in detail.
Explain how the employee's action has had a negative impact on your practice.
State your practice's policy on the situation.
If you've discussed the employee's poor performance before, include reference to previous written or verbal warnings.
Include a summary about what you and the employee have agreed to do to correct the problem.
State the consequences for failing to correct the problem.
– Performance reviews: cut liability, add punch to annual chore. You & the Law newsletter. McLean, Va: National Institute of Business Management; 2001;31(3):7.
Back to the basics
While some physicians are turning to computers to correct the problem of prescription errors, others are opting for a more low-tech solution: handwriting classes. “People may at first think of penmanship as a frivolous concern, but it has turned out to be a major public health issue,” said Ray Muller, assistant director of pharmacy at Memorial Sloan-Kettering Cancer Center, who conducts seminars on poor penmanship and medication errors, reports the March 19 Newsday.
Great expectations
Patients who choose doctors of the opposite sex may be more satisfied with their care than patients who choose doctors of the same sex, reports a study in the November 2000 Journal of General Internal Medicine. Of all groups studied, female patients who chose female physicians were the least satisfied. Researchers speculate that such patients may be expecting a more sensitive, empathetic style of care that is nearly impossible to provide in today's competitive health care environment.
Nature and well-being
Numerous studies have shown that contact with nature can promote healing, improve mental health, reduce stress and decrease the frequency of minor health problems, reports the April 2001 American Journal of Preventive Medicine. Researchers suggest that physicians consider “prescribing” nature, when appropriate, perhaps by encouraging patients to spend more time outdoors, adopt a pet or plant a garden.
Health care racketeering
A federal lawsuit brought by the Texas, California and Georgia state medical associations as well as individual doctors from seven states is accusing health insurers including Aetna Inc. and Cigna Corp. of having “undertaken a common scheme to systematically deny, delay and diminish payments to health care providers,” reports the March 27 New York Times. The suit contends the insurers' actions violate the federal Racketeer Influenced and Corrupt Organizations Act and that their decisions on whether to pay or deny claims are based on “purported actuarial criteria, unrelated to medical necessity.”
How would you fix Medicare?
The House Committee on Energy and Commerce is asking for input on how the Medicare program can be more efficient and less burdensome. Various specialty societies are calling for changes to the program, including the AMA's request for reduced paperwork hassles and better appeal rights for physicians, reports the March 5 Part B News. Individual physicians can voice their opinions as well by taking the online survey at www.house.gov/commerce/hcfasurvey.htm.
Continuity works
A recent study by the University of Washington is helping to prove the value of continuity of care by showing that children who regularly see the same physician are healthier overall. According to the study, children with low continuity of care were 60 percent more likely to visit an emergency room and 54 percent more likely to be hospitalized.
Ask your rabbi
Suggesting that the health care industry is behind in its use of information technology, the Feb. 15 Wall Street Journal posed the question, “Why is it easier to e-mail a rabbi than a doctor?” According to results of the AAFP's e-Health Survey 2000, 70 percent of physicians do not use e-mail to communicate with their patients. The most commonly cited impediments were cost, security and confidentiality concerns.
Medicaid's mysteries revealed

Thanks to a typographical error, Virginia Medicaid beneficiaries phoning for educational information were recently directed to “Miss Cleo,” a telephone psychic who addresses callers' problems for $4.99 a minute, reports the March 30 Newport News Daily Press. This proves what physicians have suspected for years – that it takes a mind reader to explain Medicaid.