
It’s easier than you might think to get what’s coming to you.
Fam Pract Manag. 2003;10(9):31-36


Few non-clinical issues have created as much controversy as the CPT codes for evaluation and management (E/M) services and the accompanying documentation guidelines. They have spurred a cottage industry of templates, cheat sheets, score cards, tool kits and the like, all designed to help you verify that your medical records contain the documentation necessary to support the codes you choose. Tools in hand, physicians, midlevel providers and support staff members hurry to E/M coding seminars in hopes of finally getting it right.
Despite these efforts, evidence suggests that family physicians may in fact be under-coding a good deal of the time. A recent study designed to evaluate the coding accuracy of family physicians found that in 33 percent of the visits involving established patients, physicians’ code selections were lower than those of expert coders (and higher than the experts only 16 percent of the time).1
Perhaps this comes as no surprise. With all the press about fraud and abuse and increased scrutiny of coding and documentation practices, many physicians have decided the safest approach is to deliberately undercode. Add to this the confusion surrounding the E/M documentation guidelines (see the box on page 33), and you have a recipe for lost revenue.
KEY POINTS
Family physicians lose significant revenue as a result of undercoding.
Because only two of the three key components are required for coding established patient office visits, you don’t have to count body systems or exam elements to code a 99214.
If you spend at least 25 minutes with a patient and more than half the time involves counseling or coordination of care, you can code 99214 based on time.
Impact on family physicians
Let’s take a conservative look at the financial impact of undercoding. Suppose you see 30 established patients per day and, like the physicians in the study, you undercode approximately 30 percent of those encounters. Assuming the difference between the Medicare allowable amount for the level of service you code and the level of service you actually provide is $27 on average, you’re losing approximately $240 per day. This is a significant loss, but not nearly as impressive as the corresponding annual loss of $57,600 per physician (that’s $230,400 for a practice of four). Just think: You can increase your revenue substantially without having to change anything about the care you provide. You simply need to select the code that accurately describes the encounter. Here’s how:
Coding 99214
CPT defines a 99214 or level-IV established patient visit as one involving a detailed history, detailed examination and medical decision making of moderate complexity. But wait! CPT also states that only two of the three key components are required for the selection of the level of service. This means that the coding can be based on the extent of the history and medical decision making only. In this instance, you don’t have to worry about counting body systems or exam elements to justify the reported level of care, and coding 99214 visits suddenly becomes easier than you may have thought. Of course, in cases where the history isn’t detailed or the medical decision making isn’t moderate but you provided and documented a high-level exam, it would be well worth your trouble to count your findings. So let’s review all three components of E/M coding for a 99214.
History. The requirements for a detailed history are actually easy to remember. According to the documentation guidelines, a detailed history requires that you note at least four elements in the history of present illness (HPI) (or the status of at least three chronic or inactive conditions, as explained in the right-hand column), a review of two to nine organ systems (ROS), and either the patient’s past history, family history or social history (PFSH). It might read something like this: “CC: stomach pain. Patient complains of intermittent, dull, epigastric pain that began two months ago. No N, V, D. No chest pain or dyspnea. Non-smoker.” You might actually take a more extensive history, but this is all that’s required for reporting the detailed history associated with a level-IV established patient visit.
Not all presenting problems lend themselves to documenting a history of present illness in the fashion just described. For example, you’ll also meet the HPI requirement when you see a patient with three or more chronic or inactive conditions (e.g., hypertension, diabetes and coronary artery disease) and document the status of each.2 Likewise, you will meet the ROS requirements since you will question the patient about signs and symptoms since his or her last visit and note accordingly. And finally, because CPT considers the review of a patient’s medications and responses to treatment to be a component of the patient’s past history, you will also have met the requirement for assessing one aspect of the PFSH. You can see that many of your patient encounters routinely meet at least the PFSH component for documenting the detailed history that a level-IV visit requires.
When you consider the thresholds for the components of the history, it is not really necessary to count anything to ensure that a detailed history has been performed. Documentation is the key! To meet the minimum requirements for a detailed history, you need only remember to do the following:
Document in some detail the circumstances or conditions that brought the patient to your office,
Document responses to a review of the affected organ system and at least one other system,
Document your medication review or mention some other aspect of the PFSH, such as smoking status.
Exam. The requirements for the detailed exam are a little more difficult to remember. In part, this is because a detailed exam can be defined in more than one way. It can be either an examination of at least five organ systems/body areas (according to the 1995 version of the documentation guidelines) or the performance and documentation of at least 12 specific exam findings (according to the 1997 version).2 In most circumstances, it is easier to use the first definition since it requires documentation of less detailed information. You frequently perform this level of exam when managing patients with multiple chronic conditions.
Here’s an example of a detailed exam involving a common complaint: a patient presenting with a fever, cough and chest discomfort. It might be documented as follows:
Vitals: temperature 101.5, BP 140/80;
ENT: negative;
Neck: supple;
Chest: rales in both bases, pain on deep inspiration;
CV: negative;
Abd: benign.
Remember, in cases where your history and medical decision making are going to support the level of service, you don’t need to spend time quantifying the extent of the examination you provided. Of course it is necessary to document any abnormal or unexpected exam findings, but details about normal findings related to organ systems outside the area of focus are not required for coding and documentation purposes.
A BRIEF HISTORY OF THE E/M DOCUMENTATION GUIDELINES
Understanding the history behind Medicare’s reimbursement methodology may help you to gain the confidence you need to code your patient encounters accurately. In 1992, when the Medicare physician fee schedule was introduced, the E/M codes used to describe patient visits were completely restructured. The goal was to standardize the selection of codes across specialties and to better delineate differences in physician work. In the new scheme, reimbursement was designed to be influenced by the resources necessary to evaluate and treat patients rather than by physician specialty. As a result, all physicians are now paid the same rate for the E/M services they provide.
Not long after the E/M codes were introduced, it became apparent that guidance was needed to more clearly define the differences among levels of service and encourage consistent coding. This guidance took the form of Medicare’s “Documentation Guidelines for Evaluation and Management Services,” which were first published in 1995 and revised in 1997. Until recently the Centers for Medicare & Medicaid Services (formerly the Health Care Financing Administration) was working on another revision meant to address complaints from physicians and others that the guidelines were too onerous. That revision was suspended by Health and Human Services Secretary Tommy Thompson earlier this fall. The fate of the revision and of the guidelines themselves is unclear. For now, you should continue to use either the 1995 or 1997 version of the documentation guidelines.
Medical decision making. Medical decision making of moderate complexity is based on two of three factors:
The number of diagnoses or management options being considered,
The amount and complexity of data involved,
The risk to the patient of either the presenting problem or the planned interventions.
Although it is generally easy to identify straightforward or high-complexity encounters, low and moderate levels of decision making often feel more ambiguous. It may be useful to think of medical decision making as a type of comparative analysis. Throughout the day, you subconsciously judge patient encounters to be simple, difficult, complex or a myriad of other adjectives. These terms seldom refer to the performance of the history or physical exam but, rather, to your cognitive work. There is a difference in the way you think about the uncomplicated patient with well-controlled hypertension and the patient who requires frequent medication changes for a chronic condition and has additional medical problems. Likewise, formulating a treatment plan for a patient presenting with abdominal pain, nausea and vomiting when there is a viral gastroenteritis in the community requires fewer considerations than evaluating a patient with similar but unexplained symptoms.
When determining the level of medical decision making, take into account the extent of your differential diagnosis or the seriousness of the problem. If you are dealing with multiple medical problems, have several data elements to review or your level of uncertainty is increased, then you should begin to think about your medical decision making as moderate. This might be a patient with three stable illnesses who is being managed on prescription drugs. It could also be a patient presenting with an acute problem with systemic symptoms.
Although nothing in CPT or the documentation guidelines requires that medical decision making be one of the two required components for a 99214, it seems logical that it serve as the foundation. It may be more difficult than documenting the history and exam, but documenting your medical decision making and letting it guide your selection will probably lead you to the appropriate code.
Family physicians see many patients with multiple medical problems and are often the first providers to evaluate new conditions or complications. The referral specialist is likely dealing with an established diagnosis affecting a limited number of organ systems. This doesn’t mean that the work of the specialist is not valuable but, rather, that you may not be giving yourself credit for the complexity of your own medical decision making.
Documentation requirements for established patient visits
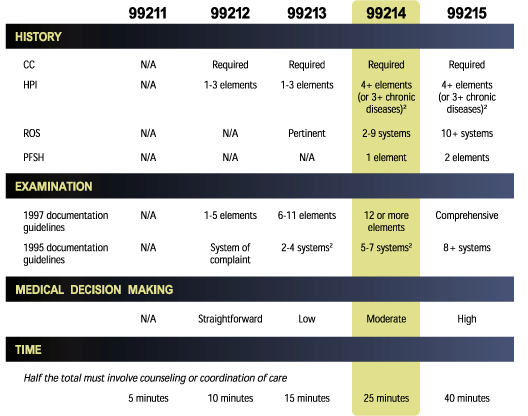
Another way to define 99214
Because you spend a lot of time educating patients about their conditions, discussing compliance issues and treatment options and reviewing findings from diagnostic studies, you may occasionally have a patient encounter that doesn’t meet the level-IV history and exam requirements but that can still be appropriately coded at that level. For example, say a patient returned to your practice to review the findings of diagnostic tests and to discuss the resulting management options. You obtained only an interval history and didn’t perform a physical exam. You don’t have to “downcode” the visit just because the history and exam are limited. If you spent at least 25 minutes with the patient and more than half of that time involved counseling or coordination of care, you can bill 99214 based on time.
When billing based on time, you code according to the total time spent with the patient. Times are noted in the CPT descriptors for many, but not all, E/M services. These times are most often used for reference; they represent average or “typical” times associated with a range of services that vary according to the clinical circumstance. When your coding is based on meeting two of the three key components, you needn’t worry about whether your service took less time than CPT says is typical. But when your coding is based on time, you must meet or exceed the times associated with the reported E/M code. In the office setting, time is measured based on the face-to-face encounter between the physician and the patient. It’s measured as floor or unit time in a hospital or nursing care facility. In each case, face-to-face time includes the time in which the physician obtains a history, performs a physical exam and counsels the patient. Remember: You can use time as the determining factor for the level of care only if counseling or coordination of care activities account for more than 50 percent of the visit. Be sure to document the total time spent with the patient and include a description of the counseling or coordination of care activities.
HOW OFTEN DO YOU CODE 99214?
Medicare data show family physicians billed 60 percent of established patient office visits at level-III and 16 percent at level IV during 1999. If family physicians undercode by 30 percent, as one recent study suggests, approximately 21 percent of the established patient office visits you provide may really be 99214s.1

Source: Centers for Medicare & Medicaid Services.
Putting it together
According to data from the Centers for Medicare & Medicaid Services, the majority of encounters for established patients are reported using levels III and IV. The table demonstrates the differences between the documentation requirements for each of the codes.
Because level-V established patient visits describe comprehensive evaluations with high-complexity medical decision making, these visits are relatively uncommon and relatively easy to recognize when they occur. While level-IV visits may not seem as apparent, you can successfully code and document them by simply remembering the minimum requirements.
Don’t shortchange yourself
This article is not about changing how you treat patients. It is about getting paid for the work you already do. The key is to document everything you do and code for what you document. As a family physician, you play a major role in caring for complex health problems. You deserve to be paid appropriately.