
These six tips make coding for observation services easier and more productive.
Fam Pract Manag. 2004;11(2):23-24

Billing for observation services can be confusing, particularly when an observation stay lasts more than one day or when a patient’s status changes from observation to inpatient. Observation services include initiating observation status, supervising the care plan and reassessing the patient periodically. The tips below should help you bill more accurately for observation services.
1. E/M services provided on the same date as the observation admission are separately billable only if they aren’t related to the admission.
For example, a follow-up visit for diabetes in the morning could be reported in addition to admitting a patient with chest pain to observation status in the evening.
2. Initial observation services are per calendar date, not per 24-hour period.
The codes for initial observation services (99218-99220) correspond to the services most physicians think of as the “history and physical” (H&P). They should be used to report the first face-to-face encounter with the patient in observation status, which may or may not occur on the same date the patient was admitted to observation status. The date/day distinction is particularly useful when6 trying to determine whether you can bill for an E/M service related to the admission. If it occurred on the date prior to your first face-to-face encounter with the patient in observation status, you can.
Initial observation codes have the same key components and documentation requirements as the codes for initial hospital visits in terms of history, exam and medical decision making. And they essentially have the same relative value units (RVUs) as the initial hospital visit codes, so reimbursement for the two types of service should be similar. If you use a form for observation services, make sure it has sufficient space for the review of systems and the past, family and social history. When it comes to documentation, these two elements are often forgotten, and their omission can prevent you from being able to code and be reimbursed at the level you’re entitled to.
When your patient is admitted and discharged from observation status on the same date, use observation or inpatient care services codes 99234-99236. These codes include the work for both admission and discharge. Documentation requirements for the admission portion of the service are the same as for the other initial care codes (both observation and inpatient). The RVUs are higher for these visits because payment for the discharge is included. (To determine what you can earn for this service and others related to observation care, see “RVUs for observation-related services.”)
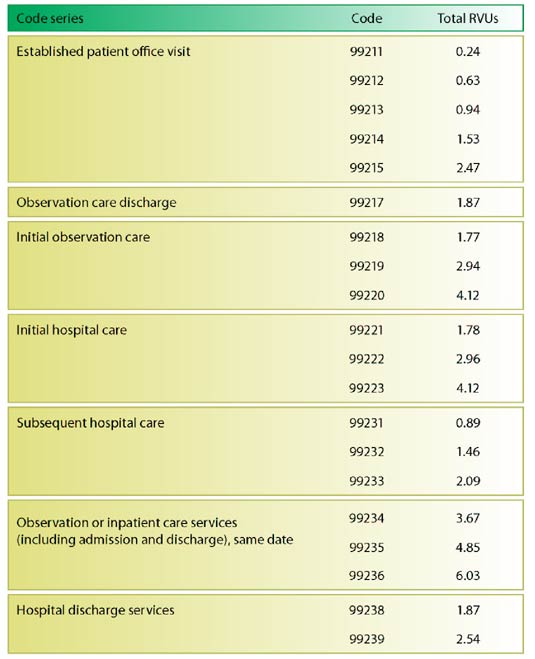
RVUs FOR OBSERVATION-RELATED SERVICES
If you’re unsure when coding for observation services, you could be shortchanging yourself. The table below shows the relative value units (RVUs) you can earn for a range of services.
3. The second day of observation status should be coded differently from the first day.
If your patient remains in observation status a second day and is not admitted to the hospital or discharged that day, you should bill the second day of observation care using office or other outpatient visit codes 99211-99215. Since the observation services codes are by date, the second day begins at 12 a.m., even if your initial observation services were provided just an hour earlier. New patient visit codes 99201-99205 should not be used if you or another family physician in your practice initiated the observation status the previous day; these patients do not meet the criteria for new patients. Also, do not use subsequent hospital visit codes for these services, since the patient has not been admitted to the hospital.
4. An inpatient admission code (99221-99223) can sometimes be billed in addition to an observation services code.
If you perform a complete inpatient admission service on a date subsequent to admitting the patient to observation status, you might be able to code the admission using initial inpatient codes 99221-99223. Make sure you meet the criteria for at least the lowest level of admission and that the level of service you provide is medically necessary. Services provided when transferring a patient from observation to inpatient status are often more accurately coded using the subsequent hospital care codes (99231-99233).
5. Select your discharge code based on the patient’s status.
If the patient is still in observation status at the time of discharge, use 99217. If the patient is an inpatient, use codes 99238 or 99239. Remember to use observation discharge when the patient’s status is observation and use inpatient discharge when the patient’s status is inpatient.
6. Other physicians who provide services to your patients should use office visit or outpatient consult codes.
If you ask another physician to see your patient during his or her observation stay, that physician should use office or outpatient visit codes 99201-99215 or outpatient consult codes 99241-99245. Inpatient consult codes and subsequent hospital visit codes should not be used because the patient has not been admitted to inpatient status.
A few practical examples
Now that I’ve shared my billing tips, let me illustrate them:
You perform level-II initial observation care on a patient in the morning and discharge the patient later that same day. The correct code for this service is 99235.
You perform level-II initial observation care on a Thursday eve-ning. The patient remains in observation status on Friday. At that time, you document a detailed history, detailed exam and moderate-complexity medical decision making. The patient is discharged on Saturday. The correct codes for these services are 99219 (Thursday), 99214 (Friday) and 99217 (Saturday).
You perform a level-II initial observation late Monday afternoon and admit the patient to the hospital on Tuesday. You see the patient in the hospital from Wednesday through Friday. The patient is discharged on Saturday. The correct codes for these services are: 99219 (Monday); 99221-99223 (Tuesday) if another H&P is performed and documented or 99231-99233 if not; 99231-99233 (Wednesday through Friday); and finally, 99238 or 99239 (Saturday), depending on the amount of time spent.
It’s worth the effort
Admittedly, coding for observation services isn’t as straightforward as any of us would like, but that doesn’t mean we need to suffer in solitude. Some things in life (and coding) are meant to be shared. And let’s face it: How to bill for observation services is one of them.