These strategies will help you turn problematic encounters into productive ones.

As many as 15 percent of patient-physician encounters are rated as “difficult” by the physicians involved.1 Patient characteristics that suggest the likelihood of difficult encounters include the presence of depressive or anxiety disorders, more somatic symptoms and greater symptom severity, according to the study. Not all difficult encounters can be blamed on the patient side of the interaction. Physician attitudes about care, fatigue, stress and burnout can create circumstances in which physicians are responsible for the difficulties. Language barriers, cross-cultural issues and the need to relay bad news can also make for challenging encounters.
Using a framework adapted from Adams and Murray,2 we present some common scenarios you may encounter in your practice, along with strategies for dealing with them. In this model, patient characteristics, physician characteristics and situational characteristics all contribute to difficult clinical encounters.
Patient factors
It can be hard to have productive encounters when patients exhibit the following characteristics. Here's how to identify them and respond appropriately.
Angry, defensive, frightened or resistant patients. Clenched fists, furrowed brows, wringing of the hands, restricted breathing patterns and warnings from office staff that something is wrong can help to identify these patients. When you see these signs, try to uncover the source of difficulty for the patient and pay attention to the way his or her emotions relate to the medical issues at hand. Don't get drawn into a conflict. Instead, define your boundaries and recognize when your “triggers” are invoked, as this will help you to modulate your response to the situation and allow you to empathize with the patient. Use reflective statements such as, “I can understand why you might feel that way,” and follow with a discussion about what it might take to resolve the situation2,3
For example, a patient who is in pain and has been waiting for an hour because you have been tending to a hospital emergency might be quite angry when you finally get to the room. He may say, “My time is as valuable as yours. I don't understand why I had to wait.” Your own sense of being harried and running late may trigger an angry reaction from you, but simply taking a deep breath and offering a sincere apology would be a more constructive response than having your own meltdown. A statement such as, “I can understand why you are upset, and I appreciate your waiting for me,” would go a long way toward easing the patient's frustration. If you can say with confidence that you'll handle the situation differently next time, for instance, by instructing your office staff to tell your patients that you are running late and to offer alternatives to waiting, such as rescheduling, then tell the patient what you intend to do.
If you sense that a patient is fearful about a diagnosis or treatment, encourage the patient to talk about it, and assess whether the fear is appropriate in proportion to the situation. This may help to establish a context for the fear, allowing the patient to deal with it more constructively.
Of course, if at any point during an encounter with an angry patient you sense a potential for harm to you or your staff, ask for assistance from law enforcement and remove those you can from harm's way.
Manipulative patients. These patients often play on the guilt of others, threatening rage, legal action or suicide. They tend to exhibit impulsive behavior directed at obtaining what they want, and it is often difficult to distinguish between borderline personality disorder and manipulative behavior. The keys to managing encounters with manipulative patients are to be aware of your own emotions, attempt to understand the patient's expectations (which may actually be reasonable, even if his or her actions are not) and realize that sometimes you have to say “no.”
Somatizing patients. These patients present with a chronic course of multiple vague or exaggerated symptoms and often suffer from comorbid anxiety, depression and personality disorders. They often have “doctor-shopped” and likely have a history of multiple diagnostic tests. Keys to productive encounters with somatizing patients include describing the patient's diagnosis with compassion and emphasizing that regularly scheduled visits with a primary physician will help to mitigate any concerns. Be sure to effectively manage any comorbid psychological conditions as well. It is important to refrain from suggesting that “it's all in your head,” and avoid the cycle of vigorous diagnostic testing and referrals.
A strategy for communicating with a new somatizing patient who has “doctor-shopped” might be to address the issue directly at the beginning of the encounter. For example, “I noticed that you have seen several physicians and have had extensive medical tests to try to uncover the cause of your symptoms. I recognize that the symptoms are a real difficulty for you, but I believe that these tests have ruled out any serious medical problems. I have another strategy to suggest that has worked well for patients of mine in similar situations. I would like to make a contract with you to see you every two to four weeks – often enough to see if there is anything truly new going on. If something significant develops that has not already been worked up, we will do more tests. We will meet frequently enough to provide you some assurance that we are not missing anything, and we will avoid uncomfortable and costly tests and procedures unless they are clearly necessary.”
Grieving patients. Recognizing the effect of grief on some patients' health requires familiarity with the normal stages of grief and the cultural context in which it occurs. Look for vegetative signs of depression and maladaptive behaviors that prevent progression through the normal grieving process, and treat them. Help grieving patients by validating their emotional experience and making sure they understand that grief is a process that takes varying degrees of time for different people. Encourage open communication, avoid inappropriate medication to suppress emotions, and caution against major lifestyle changes too early in the process.
“Frequent fliers.” These patients may stand out due to the sheer bulk of their medical charts. They may be lonely, dependent or too afraid or embarrassed to ask the questions they really want answered. They may also be patients with a large number of perfectly rational questions, the “worried well” or simply patients who have been given misinformation that needs clarification.
The first step to a productive interaction is to identify the underlying reasons for the frequent visits. Begin by acknowledging that you notice the pattern of frequent visits, and explain that you have seen other patients schedule frequent visits for different reasons, including concern about undiagnosed symptoms, a need for reassurance, a need for relief from chronic pain or a need to talk. Ask whether any of these reasons apply or whether the patient has other ideas as to the reasons for the frequent visits. Showing understanding of the patient's reasons often will foster an open discussion of the “reasons behind the reasons.” Contract with the patient for regularly scheduled return visits, and use patient education and support personnel as needed. Well-honed pain-management skills may also come in handy for patients who schedule frequent appointments due to chronic pain.
COMPONENTS OF A DIFFICULT CLINICAL ENCOUNTER
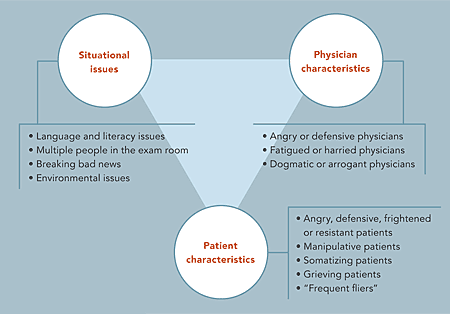
Source: Adams J, Murray R. The general approach to the difficult patient. Emerg Med Clin North Am. 1998;16:689–700. Adapted with permission from Elsevier Inc.
Physician factors
Physicians' own attitudes and behaviors, including the following, may also contribute to difficult encounters with patients.
Angry or defensive physicians. Physicians who are burned out, stressed and generally frustrated over near-term crises or long-term concerns are more likely to react negatively to patients, not just those with characteristics that may contribute to a difficult encounter. Recognizing our own trigger issues and knowing what personal baggage we bring into the exam room can be valuable.
Fatigued or harried physicians. Most of us have been overworked, sleep deprived or generally busier than we needed to be at one time or another. “Over commitment” is a closely related phenomenon that is all too common among high-achieving professionals. It is important that we be sensitive to the impact of physician fatigue on medical errors and patient safety and set reasonable limits for ourselves.3 Consider these strategies: Diplomatically bow out of commitments, delegate to others as appropriate and seek work environments that value setting appropriate limits.
Dogmatic or arrogant physicians. Each of us has things we feel strongly about. Personal beliefs and values, as well as our beliefs and values about medical care, can lead us to overemphasize our own beliefs and emotions in ways that disempower patients or prevent them from providing us with adequate information about their care. Our own baggage may also prevent us from assessing that information without bias. Identify your trigger issues and avoid situations in which your beliefs may inappropriately close off adequate exchange of information and the shared decision making that is critical to a healthy patient-physician relationship.
Situational factors
Sometimes difficult encounters have more to do with the circumstances surrounding the encounter than with the people involved. You should be ready to address the following challenges when they arise.
Language and literacy issues. As the United States develops a more diverse population, family physicians increasingly find themselves needing to communicate with individuals whose primary language is different than their own. Try to allow extra time for these encounters. Whenever possible, work with a trained interpreter rather than trying to communicate through a patient's family or friends. Ensure that the interpreter translates everything that is said rather than “editing” the conversation. Direct your eyes and speech toward the patient rather than the interpreter. Working across cultures requires sensitivity to different beliefs about health and illness, religious issues and gender issues. You may not be able to be “culturally competent” for all people, but your goal should be to remain “culturally sensitive” in all situations.
Multiple people in the exam room. As many as 16 percent of adult patients have a companion present during ambulatory medical appointments.4 This phenomenon requires thoughtful assessment of the situation and mindfulness of the patient's needs. Consider these issues: Does the patient want the other individual in the room — for the history and the physical exam? Is there a need to talk with the patient alone? Will the third person be involved in health care decisions, or are there cultural reasons for him or her to be present? Is there any evidence that the third person is forcing the patient to acquiesce to his or her presence?
For example, if a female patient comes in for a well-woman visit and her male companion insists on being in the room during the exam, it could be for a variety of positive or negative reasons. The patient may be concerned about some portion of the exam or potential findings, or there could be a cultural or religious prohibition against anyone seeing the patient in a state of undress without her husband present. Or the companion may be controlling or abusive or have an inappropriate desire to witness the examination for sexual or other reasons. Whatever the circumstances, it is important to discuss the issue of the companion's presence with the patient alone and, if she wants him to be present, to consider the request in light of the situation at hand. You might broker a compromise in which the companion is not in the room during the exam but is present for the discussion afterward, or you may decide to allow him to be present along with your staff chaperone. The key point is to have the conversation with your patient in private and honor what is in the patient's best interests, given the situation.
When patients have companions in the exam room, be sure to speak directly to the patient, avoid taking sides in any conflict, and evaluate all parties' understanding of the information and the management plan.
Breaking bad news. When it is necessary to give patients information that will be difficult for them to hear, preparation is critical. Know who will be present for the discussion, allow adequate time and privacy, and review the clinical situation. In the early stages of the encounter, assess what the patient already understands or believes about the situation and how much more information he or she wants. Disclose the news directly, allowing adequate response time for the patient and others in the room to experience their emotions and process the information. After giving the news, discuss the implications, offer additional resources, agree on next steps, summarize the discussion and be certain to arrange for follow-up.
Environmental issues. Physicians often overlook the fact that their surroundings may increase the likelihood of a difficult patient encounter. If the environment is noisy, chaotic or doesn't afford appropriate privacy, patients, providers and staff are all more likely to be unhappy or unpleasant. These factors can often be alleviated with a bit of forethought.
SUGGESTED READING
- “Sticking the Landing: How to Create a Clean End to a Medical Visit.” Lutton ME. FPM. July/August 2004:51–53.
- “Getting the Most From Language Interpreters.” Herndon E, Joyce L. FPM. June 2004:37–40.
- “The Fine Art of Refusal.” Spickerman F. FPM. February 2004:80.
- “When Your Patients Are in Mourning.” Kreger J. FPM. November/December 2003:49–50.
- “Focusing on Today's Visit.” Redka JW. FPM. June 2003:59–60.
- “Caring for Frequent-Visit Patients.” Gillette RD. FPM. May 2003:57–62.
- “'Oh, by the Way…”: Agenda Setting in Office Visits.” Olson KP. FPM. November/December 2002:63–64.
- “Achieving a More Minority-Friendly Practice.” Glenn-Vega A. FPM. June 2002:39–43.
- “Interviewing When Family Members Are Present.” Lang F, Marvel K, Sanders D, et al. American Family Physician. 2002;65:1351–1354.
- “Cultural Competence.” Sutton M. FPM. October 2000:58–60.
- “'Problem Patients': A Fresh Look at an Old Vexation.” Gillette RD. FPM. July/August 2000:57–62.
- “Mindful Practice.” Epstein RM. JAMA. 1999;282:833–839.
Communicate with care
Being aware of factors that contribute to difficult clinical encounters and being prepared to address them will go a long way toward preventing them. But don't underestimate the positive difference that good interpersonal communication skills can make in these situations and other, more typical encounters as well. For example, remain seated during the encounter, practice active listening, respond to “Oh, by the way” questions instead of dismissing them, and close the interview with a specific question, such as “Do you have any questions about what we discussed today?”
In addition, attending to your own physical and mental processes as you see patients and remaining aware of your own emotional baggage in the exam room (the art of “mindful practice”) may decrease the number and intensity of difficult encounters you experience. (The “Suggested reading” list includes articles that describe these and other skills.) No physician can avoid the difficult clinical encounter, but having the tools to deal with these situations when they arise can make for a better experience for both you and your patient.

