
The most effective leaders realize that everyone's input is valuable.
Fam Pract Manag. 2012;19(1):8-11
Dr. Parchman is professor in the Department of Family & Community Medicine, University of Texas Health Science Center at San Antonio, and Interim Center Principal Investigator, VERDICT Research Center, South Texas Veterans Health Care System, San Antonio. Author disclosure: no relevant financial affiliations disclosed. Funding support: This study is supported by the National Institute of Diabetes and Digestive and Kidney Diseases (R 18 DK 075692) and the U.S. Department of Veterans Affairs, follows the CONSORT guidelines, and is registered per ICMJE guidelines: Clinical Trial Registration number: NCT00482768. The views expressed are those of the investigators and do not necessarily represent the views of the U.S. Department of Veterans Affairs.
We are in the third year of a study to improve diabetes care in 40 small primary care clinics. Practice facilitators are working closely with the physicians and staff in these clinics to implement the chronic care model (CCM),1 a forerunner of the patient-centered medical home.
One dominant theme that has emerged from physician and staff surveys and from observations by practice facilitators is this: When leadership is inclusive of all team members, changes are easier to implement. The purpose of this article is to share observations and findings from the first 20 clinics that are related to the concept of leader inclusiveness and its importance in small primary care clinics working to improve patient care.
What is leader inclusiveness?
The inclusive leader is one whose words and deeds invite contributions from others and who demonstrates appreciation of those contributions. The inclusive leader encourages all members of the group to speak up, especially those who would not usually have their voices heard.2
Inclusive leadership creates a culture of psychological safety. The current health care model is a hierarchical system made up of members with different perceived status levels. Some members, such as physicians, have high status while others, such as receptionists, have lower status. This difference in status can influence beliefs about speaking up to offer ideas, discuss concerns, or ask questions.
Research has shown the importance of psychological safety in creating an environment in which team members, especially lower-status team members, will feel comfortable speaking up. In psychologically safe environments, people believe that if they make a mistake others will not penalize them or think less of them or their ability to do their job. Team members who feel safe also feel open about asking for help.2
How is leader inclusiveness related to chronic illness care?
We divided the clinics in our study into two groups based on physician and staff responses to questions on the Assessing Chronic Illness Care survey: one group whose scores reflect full implementation of the CCM (scores of 9 or higher) and another group whose scores reflect that the CCM is not fully implemented (scores less than 9).3 Clinics where the physicians and staff feel that an inclusive leadership style has created an environment where everyone's point of view is valued, where communication is open, and where time and space are allowed for discussion are more likely to have fully implemented the CCM (see “The importance of inclusive leadership”).
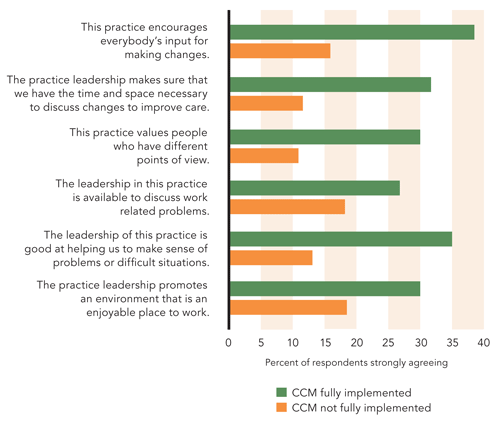
THE IMPORTANCE OF INCLUSIVE LEADERSHIP
As the chart shows, practices in the study that displayed characteristics of inclusive leadership were more likely to have achieved full implementation of the chronic care model (CCM).
How can you incorporate these ideas into your practice?
Over the past three years, we have worked with these clinics to promote leader inclusiveness and an environment where everyone feels safe to speak up. Here are some strategies that our research indicates are effective:
Huddles. Huddles are a quick, inexpensive, and easy way to improve communication and invite new ideas within the clinic. All members of the team participate, and all are invited to share ideas. Huddles can also improve efficiency through improved communication and teamwork. Time spent in the huddle prepares the entire team to provide the best possible care for that day's patients by initiating activities such as preparing resources, reviewing medications, checking lab results, or following up on prior consults. (To learn more, see “Huddles: Improve Office Efficiency in Mere Minutes,” FPM, June 2007.)
Here are two stories from the clinics in the study:
Dr. B found that huddles facilitate brainstorming and creative problem solving when challenges emerge. During the H1N1 outbreak, for instance, she asked the staff for ideas about how to handle the increase of patients needing acute visits and the need to keep these patients secluded in a small office. Her staff came up with the idea of a drive-through “carhop” approach. The patients would call to let the staff know they were coming to be evaluated for H1N1. The staff would go out to the car, interview the patient, do a quick examination, and give treatment without the patient ever leaving the car.
Dr. M reports that after trying huddles for a few weeks she felt that she no longer had time in the morning to continue them. When she told her staff she no longer wanted to do huddles, they revolted and told her that they must continue. The staff had quickly noticed that huddles allowed them to improve their communication and ability to quickly solve problems as a team.
Regular meetings with clear rules. Most of the clinics in our study were not holding staff meetings when we began the study. To share information with the staff, doctors or administrators would go to each team member individually to pass on the message. This process was time consuming and didn't always leave staff members with a clear understanding of the information or a chance to ask for clarification. Reserving time for regular clinic meetings is crucial. These scheduled meetings need to have a set of rules that support the sense that this is a time to share ideas and ask questions free of criticism. During these meetings, everyone's ideas should be considered and discussed.
In the study, practice facilitators used several methods to model effective meeting strategies. During the first meeting with the entire group, the facilitator would help the group develop ground rules for each meeting. The ground rules were unique for each clinic and reflected the specific needs of the group. Examples of meeting ground rules might be that meetings will always start on time, that everyone in the group is encouraged to participate, that all participants are considered equal in this discussion, that all participants must keep an open mind and listen to each other, and that all ideas are held up for consideration, reflection, and inquiry.
The practice facilitators often modeled appropriate behavior during facilitation meetings by demonstrating how to express appreciation, valuing the comments of all members of the group, and reminding participants not to criticize the ideas of other team members. Another method was to have two facilitators work together during a meeting to clearly demonstrate effective behaviors. The facilitators would meet for a short huddle before the meeting to discuss the topics that needed to be covered. During the staff meeting, they would show the clinic how to plan ahead, use time wisely, and communicate ideas or clinic changes effectively, with all members' input valued and respected. (For more on effective meetings, see “The Makings of a Good Meeting,” FPM, November/December 2007, and “How to Make Your Meetings More Productive,” FPM, July/August 2003.)
Reserving time and space for reflection and conversation. As shown in the chart above, setting aside a separate meeting specifically for reflection is crucial. In clinics where the CCM was fully implemented, staff were almost three times as likely to agree strongly that leadership provided “time and space necessary to discuss changes to improve care.” During this time the medical team takes an in-depth look at their current clinical structure, identifies areas they would like to improve, and works together to create solutions. Given all the demands of the clinic day, this activity will not occur unless the team leader makes a conscious effort to reserve time for this activity and expects the team members to be present and to participate fully in the discussion and improvement projects.
During the study, the facilitation sessions forced clinics to take time for reflection and conversation. For some clinics this was the first time that all members of the team had sat down together as a group. This time creates opportunities for new ideas to come from all members and leads to creative brainstorming of improvements to patient care. The clinics in our study have found this time to be crucial for the clinic to continue moving forward.
Here is another story from one of the clinics in the study:
Dr. M's staff noticed that patients frequently had questions about the clinical staff, what to expect during the visit, and how best to prepare for their visit. After several sessions of reflection and discussion, they decided to develop a brochure that covered this basic information and helped prepare patients to come to their visit with their medications and questions for the physician. Together they have created an informative brochure that is given to all patients and mailed to new patients before their first appointment.
Cross-training staff for a broader understanding of all roles. Many clinics struggle with staff turnover and providing coverage for absent staff members. One solution is to train staff in multiple or all areas and have them rotate roles for a time to learn the details of each position. This technique allows team members to develop a deeper understanding of each person's role in the clinic, which may increase respect and mutual support among team members. This technique also allows other staff members to look at the position with a fresh perspective and perhaps develop new ways to complete a task.
The inclusiveness imperative
In our current health care system, clinics are constantly reacting to change. The small primary care clinic must find ways to identify areas of improvement, work as a team to create solutions, and implement changes to the practice. We believe that an essential ingredient in this process is leader inclusiveness, especially with the current need to redesign primary care.
