With a little practice, these seven vital skills can become a natural part of your patient consultations.

Despite enormous advances in the science of medicine, the interpersonal encounter between patient and physician remains a keystone of medical care. Considerable research has explored various aspects of this relationship, including physician-patient communication, difficult patient interactions, and what physicians find meaningful in their work. These interpersonal aspects of the healing enterprise can be considered the art of medicine.
Most research into the art of medicine has tended to focus on theory instead of specifying how doctors should act. So, in teaching family medicine residents over the years, I have reviewed the literature and delineated seven behaviors that foster more consistent practice of the art of medicine. I call these behaviors “The Magnificent Seven.”
THE MAGNIFICENT SEVEN
- Take a moment to focus before entering the consultation room.
- Establish a connection with the patient by developing rapport and agreeing on an agenda.
- Assess the patient's response to illness and suffering.
- Communicate to foster healing.
- Use the power of touch.
- Laugh a little.
- Show some empathy.
1. Focus on the patient. Before entering the consultation room, take a moment to personally prepare for the encounter. This will set the stage for all that is to follow. Become aware of what is going on in your body, whether you are feeling rushed or tense or are still thinking about the previous patient. If so, take a deep breath and let go of that tension or preoccupation so that you do not carry it into the next encounter.
Then, think about the patient you are about to see. What do you know about him or her? Where are you in terms of developing your relationship? What would you like to learn about this person that you don't already know? What is the topic of the encounter, if known, and how might that drive what needs to be accomplished during the consultation? Becoming mindful of these details outside the consultation room is a precursor to being mindful inside the consultation room.
2. Establish a connection with the patient. Use the first few minutes of the consultation to connect with the patient – before opening the electronic health record. Connection occurs on at least two levels: interpersonal and intellectual. Interpersonal contact is aimed at developing rapport and generally begins by incorporating a short, non-medical social interaction to open the interview. This is a good time to get to know a bit more about the patient. A good tactic is to refer to something mentioned in earlier consultations as a way to reinforce the continuity of your relationship, such as “How is your son doing?” or “How is your garden coming along?” When the patient answers, simply observe and listen, and you'll often find clues about his or her emotional state. Other aspects of interpersonal connection involve the effective use of attending behaviors that show you are listening, such as furthering responses (“uhhuh”), eye contact, and open body language. Spending a small amount of time socializing with and listening to the patient is worth the investment, as it has been shown to yield higher patient satisfaction than spending more time with the patient.1
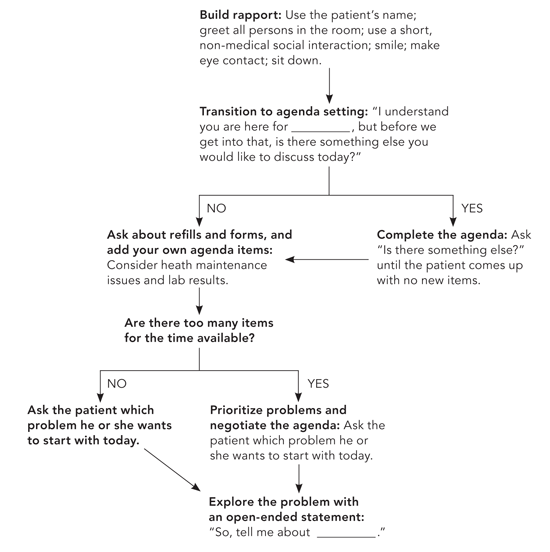
The intellectual aspect of connection involves taking time to assure the patient that you are interested in addressing what is important to the two of you. This also signals that you are transitioning from the social/rapport-building aspects of the interview to the medical aspects. Ideally, in a team-driven environment, your staff and patient would negotiate an agenda before you even walk in the room. If that hasn't taken place, you can quickly negotiate an agenda by sharing your understanding of the reason for the visit and then inquiring whether there are other issues the patient wishes to discuss today. If the patient responds affirmatively, continue to ask until the patient identifies no further issues for discussion, and then inquire as to whether the patient needs any refills or forms completed. Having surfaced the patients' concerns, prioritize them and negotiate a workable agenda for the time available. If necessary, ask the patient to schedule another appointment to address the remaining issues (see “Agenda-setting algorithm”). Setting an agenda adds negligible time to the consultation, promotes greater patient satisfaction, and makes patients less likely to raise concerns when you are trying to close the visit.2–4
In setting the agenda, it may help to understand that patients visit their doctor for five basic reasons:5 1) They may have trouble tolerating some aspect of their disease; 2) They may be anxious that their symptoms foretell dire consequences; 3) They may have problems in life that present as symptoms, such as tension headaches; 4) They may appoint for administrative reasons, such as a work release; or 5) They may need preventive services. Patients can present with more than one of these concerns (e.g., they may have pain they consider intolerable and are anxious about what it means). Understanding the reason or reasons for the visit ensures that you address the heart of why the patient is seeing you.
3. Assess the patient's response to illness and suffering. The diagnosis and treatment of a patient's illness is a core clinical function, but it is also important to assess the patient's response to their illness and suffering. Patients commonly share clues about their illness experience, which you can explore with a modest time investment. Listen for what the patient tells you he or she can no longer take for granted – e.g., “It's hard getting up the stairs, Doc” or “I just can't make it through the workday anymore without a nap” – and express curiosity about that. This can uncover significant clinical information and is associated with a better resolution of patient concerns.6,7
Patient suffering is more than just physical pain. It is “the state of severe distress associated with events that threaten the intactness of the person.”8 In other words, it affects their personhood. To assess a patient's suffering, ask questions such as, “How is your illness affecting you personally?” “How do you find comfort when you are suffering?” and “Despite your suffering, do you feel hopeful about your future?” Some patients are able to find meaning in their suffering or express a sense of hope, even if their condition is incurable, while others may feel despair and withdraw into their suffering.9 These latter patients will require more care, attention, and relationship building, and your management plan will be more effective if it addresses ways for them to find comfort in the face of illness and suffering.
4. Communicate to foster healing. Renowned psychologist Carl Rogers suggested that those who counsel patients need to display three things in their communication:10
- Congruence (being authentic and letting the patient experience who you really are, instead of putting on a facade),
- Acceptance (showing that you value the person even if you don't agree with his or her actions),
- Understanding (relating and being sensitive to what the patient is experiencing).
Rogers' research indicated that individuals exposed to a relationship with high degrees of these qualities grew in their potential.
Patients who have problems of living (such as domestic problems, socioeconomic challenges, or emotional issues) that present as medical problems can be particularly difficult to communicate with and are often labeled “problem patients.” Managing them will require you to use two skills that can be uncomfortable. The first is relational immediacy, that is, the ability to communicate about a dynamic or behavior that is happening in the present moment of the encounter (e.g., “I feel like we're misunderstanding one another” or “I'm feeling frustrated, and I'm sensing that you are too. Can we start over?”).
The other skill you'll need involves confrontation. This is one of the most powerful actions you can take to support another's growth because it focuses on areas that the individual may need to change. However, confrontation can trigger volatile, defensive reactions. Useful tactics are to introduce your concern with a positive observation to help the patient absorb some of the shock of your confrontation and then use curiosity or wonderment to express your concern. For example, “I can tell that you love your family very much and you want them to have a happy home life. But I wonder if hiding your depression from them might have the opposite effect of creating distance in your relationship and keeping you from getting the support you really need?”
5. Use the power of touch. A general rule is to always touch the part that hurts, but never touch the part that hurts first. A warm handshake or a pat on the shoulder can often help calm distraught patients, and touch may have health-enhancing benefits as well. For example, massage can strengthen immune function11 and gentle touch has been shown to reduce pain responses to heel stick in premature infants.12
Of course, reactions to touch may be unpredictable with patients who have been physically abused and associate touch with exploitation or pain, patients who are psychiatrically or developmentally challenged, and patients who are seductive. You can still use touch with these patients, but proceed with some caution. Also, be culturally sensitive. If you sense that a patient is uncomfortable with touch because of his or her culture or beliefs, be sure to explain what the physical examination will entail before you begin and, in some cases, ask permission to proceed.
6. Laugh a little. Medicine is a serious business, and doctors are seriously busy people. But if you're too serious or too busy to recognize humor in your workday, then you and your patients are missing out on something powerful. Humor can be helpful in establishing rapport, relieving anxiety, communicating messages and caring, enhancing healing, and providing an acceptable outlet for anger and frustration.13 It has generally favorable physiological effects but, like any other tool, should be used appropriately. Humor carries less risk if it is gently self-deprecating, is externally focused (not directed at the patient), is not used as the sole means of communication, is grounded in empathy, and is reciprocal.
When using humor, remember that there are three types of people: those without a sense of humor, those who enjoy humor, and those who generate humor. If you sense the patient lacks a sense of humor, forego this recommendation; humor will only make the patient angry. If you lack a sense of humor, forego this recommendation; you won't be funny. For everyone else, be discerning but please give yourself license to laugh a little.
7. Show some empathy. As discussed earlier, psychologist Carl Rogers included understanding, or empathy, as an important ingredient in communication. I've put empathy in its own category, however, because I believe it is so vital but so seldom practiced. Rogers described it as sensing the patient's world “as if it were your own, without ever losing the ‘as if’ quality.”10 This attempt to understand the patient's experience not only helps to establish a caring relationship but also can affect physiology. For example, patients with highly empathetic physicians have been shown to have better glycemic control and LDL levels and cold symptoms that last two fewer days than those of patients whose physicians are less empathetic.14,15
Being empathetic usually involves making an explicit comment concerning the patient's feelings or experience. Saying “I'm sorry,” while sympathetic and often appropriate, is not empathetic because it references your feelings, not the patient's. Examples of empathetic remarks are, “That must be very frustrating” (feeling) or “The stairs are really becoming a struggle for you” (experience). Empathy can be coupled with expressions of sympathy: “I'm sorry for your loss. I can't imagine how devastating this must be.”
Making a mental note to be explicitly empathetic is important because medical training and medical culture can sometimes erode empathy. For example, you may have learned over the years to consider subjective information as suspect or to disconnect from a patient's experience to ensure technical proficiency during an unpleasant or painful procedure. Being explicitly empathetic is important because “empathy withers with silence.”16 Patients cannot know whether you have grasped their experience and understand them as individuals unless you state what you understand. By being explicit in your understanding, you communicate your receptiveness to the patients' concern, which may encourage the sharing of more personal, clinically important information.
The benefits
Although no empirical tests have verified the thesis that using these seven strategies will enhance your practice of the art of medicine, the behaviors recommended are based on empirical data. They incorporate a patient-centered approach to communicating with patients, which has been shown to improve health outcomes, increase patient satisfaction, and decrease malpractice liability.17
But using these activities may have an added benefit: In an environment in which physicians are becoming increasingly disillusioned and burnt out, utilizing “The Magnificent Seven” may help you deepen your relationships with patients. In so doing, you may uncover those changes in perspective, connections with patients, and experiences of making a difference in another's life that bring meaning to your work.18
The science of medicine has wrought miracles in the prevention, diagnosis, and treatment of disease. But the art of medicine remains the medium through which illness and suffering are relieved and becomes paramount when biomedicine runs its course and has little to offer the patient. By practicing the art of the consultation, you just might rediscover and nourish the altruistic motivations that called you to be a healer.