
Am Fam Physician. 1998;57(11):2628-2630
to the editor: I would like to share a tried, inexpensive and effective method of treating leg ulcers. I have used this procedure in many patients over the course of 20 years, and it has been favorably adopted by my fellow physicians. Although it is not a controlled or scientifically proven treatment, it has worked for me.
While in Australia, with the help of physical therapists, my colleagues and I developed this simple technique of healing leg ulcers. These indolent infected craters are often associated with local leg ischemia and are the result of arteriosclerosis, diabetes, minor trauma and pressure.
In contrast to the wet dressings, pressure bandages and grafting methods used in current treatments, our approach relies on the restoration of an active blood supply to the open ulcer base. If an “ulcer” is surveyed closely, a red granulomatous center is found, often with superficial purulent matter, and an encircling firm, bandlike rim of edematous tissues is present that blends into the surrounding normal skin.
Our approach restores a healthy pink center to the ulcer by removing the compressing rim. The procedure is simple: the physician gently massages the center of the ulcer with the thumb in a circular manner using a mix of 2 percent lidocaine (Xylocaine Viscous) and polymyxinbacitracin ointment as a lubricant (see figure). This circular massage, performed daily, is later carried more firmly to the rim around the edge of the ulcer. This therapy alleviates ulcer pain in the early days of treatment, helps to remove the surface infection and begins the slow destruction of the rim, which is the key to the process.
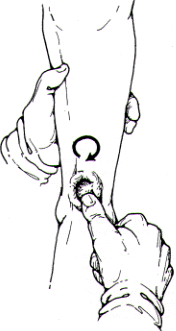
After a few days, the ulcer is usually painless and lidocaine is no longer needed. Shortly thereafter, the superficial infection will clear and use of the antibiotic ointment can be discontinued. Continue daily massaging using vegetable oil (maize, peanut, soya or safflower) as a lubricant. This firm massaging will remove the constricting rim in a few days and allows blood to reach the base of the ulcer. In a remarkably short time (one to two weeks), even a fairly large ulcer (3 cm) can be persuaded to heal. During the periods between massaging, a simple nonadherent dressing can be used to protect the ulcer if circumstances dictate, but the better approach is to leave the ulcer exposed to the air with a thin covering of lubricant.
Once the physician demonstrates the proper technique, the daily massage can be continued at a clinic or by a visiting nurse. As soon as progress is evident, the family or even the patient can take over. When the ulcer appears to be healed, a visit to the physician for a final check and instructions for prophylactic care (regular light oiling of the legs, early treatment of minor trauma and smoking cessation) should prevent a recurrence. This technique is simple, effective and offers a rapid healing of the leg ulcer.