
Am Fam Physician. 1998;58(5):1185-1186
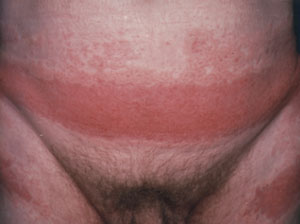
A 34-year-old man presented to his physician with an intensely pruritic eruption at his waist and groin that had continued to worsen over the past five years (see the accompanying photograph). He had previously experienced some erythema on his neck and axilla but seldom the redness, scaling and blistering present on his waist and groin. The eruption waxed and waned but was always present and seemed to worsen in hot weather. The use of topical corticosteroids—the stronger the better—helped; the rash, however, would flare up when the steroid was discontinued.
Question
Discussion
The answer is C: allergic contact dermatitis. “Waistband dermatitis,” also known as “bleached rubber syndrome,” is a common form of allergic contact dermatitis, with a distinct history and etiology. While many patients are allergic to various components of rubber and elastic on clothing such as underwear, patients with this condition are usually not allergic to the elastic of the underwear itself, but rather to elastic that has been subjected to repeated washing with liquid bleach. After repeated bleaching, the elastic becomes much more allergenic, possibly as a result of the greater availability of carbamates in the bleached clothing.1 Potent topical or systemic corticosteroids will provide very rapid relief of the dermatitis, but the affected person must discard all bleached underwear and purchase new underclothing that must never be bleached.1
If the rash persists, the patient should undergo patch testing to determine the presence of an allergic contact dermatitis to some other ubiquitous elastic component. Ad hoc patch testing may be easily performed on a patient suspected of having an allergic contact dermatitis by cutting a 1-cm square of bleached elastic (e.g., from the underwear waistband) and taping it, dry and occluded, to the upper arm or back for 48 hours.An eczematous eruption arising within 96 hours of applying the patch confirms the diagnosis. More formal patch testing may be performed with an easy-to-use patch test battery such as Tru-test.2
While tinea corporis can occur at any site on the body, it would not remain as focal and symmetric over time as the eruption pictured here. An examination using potassium hydroxide should be done on every red, scaly eruption to rule out a fungal etiology before a corticosteroid is prescribed. Irritant contact dermatitis is a possibility, as 80 percent of all contact dermatitides are irritant rather than allergic in nature. A careful history of topical medication use and laundering practices should help exclude a purely irritant cause. Atopic dermatitis (atopic eczema) may also cause large areas of red, scaly, itchy skin. Because moisture and occlusion tend to ameliorate this form of eczema, the groin would be the area least affected, rather than the only area involved. It would be extremely unlikely for Bowen's disease (squamous cell carcinoma in situ) to involve such a large area and create such a symmetric pattern.
Any persistent red, scaly patch that either defies diagnosis or fails to respond to repeated therapy should be biopsied to exclude Bowen's disease, superficial basal cell carcinoma or mycosis fungoides.