
Am Fam Physician. 2001;63(11):2231-2237
Fishing is a common recreational sport. While serious injuries are uncommon, penetrating tissue trauma involving fishhooks frequently occurs. Most of these injuries are minor and can be treated in the office without difficulty. All fishhook injuries require careful evaluation of surrounding tissue before attempting removal. Ocular involvement should prompt immediate referral to an ophthalmologist. The four most common techniques of fishhook removal and injury management are described in this article. The choice of the method for fishhook removal depends on the type of fishhook embedded, the location of the injury and the depth of tissue penetration. Occasionally, more than one removal technique may be required for removal of the fishhook. The retrograde technique is the simplest but least successful removal method, while the traditional advance and cut method is most effective for removing fishhooks that are embedded close to the skin surface. The advance and cut technique is almost always successful, even for removal of large fishhooks. The string-yank method can be used in the field and can often be performed without anesthesia. Wound care following successful removal involves extraction of foreign bodies from the wound and the application of a simple dressing. Prophylactic antibiotics are generally not indicated. Tetanus status should be assessed and toxoid administered if needed.
Angling is a popular sport worldwide, and fishhook injuries are common in recreational and commercial fishing settings. Persons with fishhook injuries may not present to the office or emergency department because removal of embedded fishhooks can usually be accomplished in the field. However, some embedded fishhooks cannot be removed in this manner and require evaluation of the injury and exploration of the wound for the presence of a foreign body. Four techniques for removing embedded fishhooks are described in this article
Patient Evaluation
Most fishhook injuries are penetrating soft tissue injuries to the hand, face, head or upper extremity but can involve any body part. These injuries usually do not involve deeper tissue structures because of the linear forces applied along the fishing line to the fishhook that drive the point parallel to the skin and keep it from deep penetration.
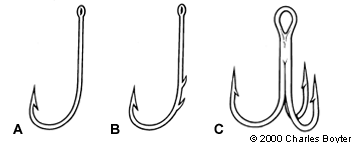
Many different types and sizes of fishhooks are available (Figure 1). When examining the hook, it is important to note if the fishhook is single, multiple or treble, whether the hook is barbed, and the number and location of the barbs—these details will help determine the best removal technique. Often, persons will know the type of hook they were using and may be able to provide a sample for inspection.
Occasionally, more serious tissue trauma occurs from fishhook injury. While not routinely performed, radiographs may aid in determining the type of fishhook and the depth of penetration in difficult cases.1 Neurologic and vascular status, proximal and distal to the wound, should be assessed. Any fishhook injury that may involve deeper structures such as bone, tendons, vessels or nerves requires careful evaluation before attempting removal.
Cases of penetrating eye trauma secondary to fishhook injury have been reported in the literature.2–5 One such injury even included intracranial trauma.3 Fishhooks that penetrate the orbital area or are embedded in a location in which removal may injure the eye should be covered with a metal patch or cup and the patient should be sent immediately for ophthalmologic consultation.6 Permanent vision damage may occur with removal of the fishhook although minimal vision deficit was evident on initial presentation.
Principles of Removal
Four primary techniques have been described for the removal of fishhooks: retrograde, string-yank, needle cover, and advance and cut. Each method and some modifications to these techniques are described in detail in this article. The method selected to remove anembedded fishhook is usually based on the judgment of the physician, the anatomic location of the injury and the type of fishhook.
Most embedded fishhooks can be removed with minimal surgical intervention. Generally, the retrograde and string-yank methods should be the first techniques attempted because they result in the least amount of tissue trauma. The more invasive procedures, such as the needle cover and advance and cut techniques, are reserved for more difficult fishhook removal.7 Sometimes multiple techniques must be attempted before the fishhook is successfully removed.
Most removal methods require the administration of a local anesthetic or a nerve block. Superficially embedded hooks may not require anesthesia if they can be backed out or removed easily by the string-yank method.
Local care typically involves cleaning the site with povidone-iodine or hexachloro-phene solution before attempting removal of the fishhook. Saline irrigation may be required. Fishhooks with more than one point (i.e., treble fishhooks) should have the uninvolved points taped or cut to avoid imbedding these during the removal procedure. A local anesthesia should be administered before attempting removal of any barbed fishhook. All items attached to the hook (i.e., fish line, bait and the body of the lure itself) should be removed. The physician and bystanders should take care not to be struck by the hook on removal. Eye protection should be worn, especially when performing the string-yank method.
Retrograde Technique
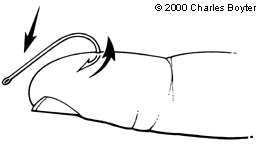
Retrograde technique is the simplest of the removal techniques but has the lowest success rate. It works well for barbless and superficially embedded hooks. Downward pressure is applied to the shank of the hook. This maneuver helps rotate the hook deeper and disengage the barb, if present, from the tissue. The hook can then be backed out of the skin along the path of entry (Figure 2). Any resistance or catching of the barb during the procedure should alert the physician to stop and consider other removal methods.
String-Yank Technique
The string-yank technique is a highly effective modification of the retrograde technique and is also referred to as the “stream” technique. It is commonly performed in the field and is believed to be the least traumatic because it creates no new wounds and rarely requires anesthesia.8 It may be used to remove any size fishhook but generally works best when removing fishhooks of small and medium size. This technique also works well for deeply embedded fishhooks, but cannot be performed on parts of the body that are not fixed (e.g., earlobe).9 Physicians should be familiar with the concepts of this method because improper technique could cause further tissue damage.
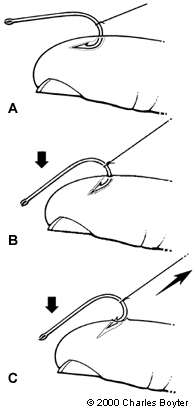
A string, such as fishing line, umbilical tape or silk suture, should be wrapped around the midpoint of the bend in the fishhook with the free ends of the string held tightly (Figure 3). A better grip on the string can be achieved by wrapping the ends around a tongue depressor.1 The involved skin area should be well stabilized against a flat surface as the shank of the fishhook is depressed against the skin. Continue to depress the eye and/or distal portion of the shank of the hook, taking care to keep the shank parallel to the underlying skin. A firm, quick jerk is then applied parallel to the shank while continuing to exert pressure on the eye of the fishhook. The fishhook may come out with significant velocity so the physician and bystanders should remain out of the line of flight. A commercial fishhook removal device, based on this technique, is available. (Minto Research and Development In Redding, Calif.)10
Needle Cover Technique
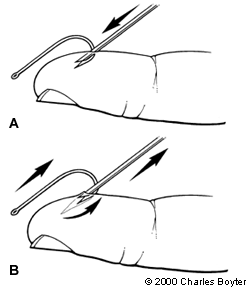
The needle cover technique requires dexterity on the part of the physician. It works well for the removal of large hooks with single barbs but is most effective when the point of the fishhook is superficially embedded and can be easily covered by the needle. After skin preparation and administration of local anesthesia, an 18-gauge or larger needle is advanced along the entrance wound of the fishhook (Figure 4). The direction of insertion should be parallel to the shank. The bevel should point toward the inside of the curve of the fishhook, enabling the needle opening to engage the barb. It is important to have the bevel pointed in the correct direction so that the longer edge of the needle matches the angle of the fishhook point. The physician should advance the fishhook to disengage the barb, then pull and twist it so that the point enters the lumen of the needle. The physician can then back out the fishhook (the same way as in the retrograde technique), taking care to move the needle along the track with the fishhook.
A modification of this technique involves sliding a no. 11 scalpel blade along the wound to the point of the fishhook. The fishhook may then be backed out because the incision allows room for the point. This modification may also be used in combination with the needle cover technique for more difficult fishhook injuries
Advance and Cut Technique
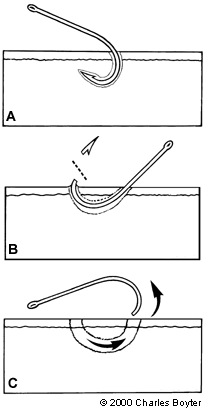
One advantage of this traditional method of fishhook removal is that it is almost always successful, even when removing larger fishhooks; however, additional trauma to the surrounding tissue is a disadvantage. The advance and cut technique is most effective when the point of the fishhook is located near the surface of the skin.9 It involves two methods of removal: one for single-point fishhooks (Figure 5) and one for multiple-barbed fishhooks (Figure 6). Infiltration with a local anesthetic is performed over the area where the fishhook has penetrated the skin. Using pliers or needle drivers, the point of the fishhook (including the entire barb) is advanced through the skin. The point is then cut free with the pliers or another cutting tool, allowing the rest of the fishhook to be backed out with little resistance.
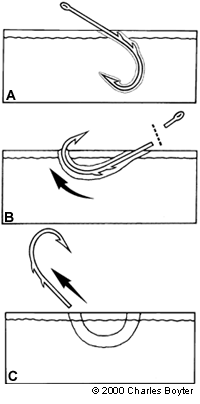
For multiple-barbed fishhooks, the area should be anesthetized and the fishhook advanced. Instead of removing the point, the eye of the fishhook is removed. The physician can then continue to pull the fishhook in the same direction as the point was advanced.
Post-Removal Wound Care
After removal of the fishhook, the wound should be explored for possible foreign bodies (e.g., bait). It is usually sufficient to leave the wound open, then apply an antibiotic ointment and a simple dressing. Tetanus toxoid should be administered to persons for whom more than five years has elapsed since their last tetanus booster. Well-conducted, controlled studies do not exist that support the need for systemic antibiotics in these cases; they are generally not indicated.7 Prophylactic antibiotic therapy may be considered for persons who are immunosuppressed or have poor wound healing (e.g., patients with diabetes mellitus or peripheral vascular disease). Prophylactic antibiotic therapy may also be considered for deeper wounds that involve the tendons, cartilage or bone. Follow-up care should be performed to ensure adequate healing and the absence of infection.