
Am Fam Physician. 2001;64(1):141-142
A 31-year-old woman with a 10-year history of chronic renal insufficiency secondary to bilateral obstructive hydronephrosis presented for evaluation of pain in the right hip. She had undergone bilateral ureterostomies, but her creatinine level remained chronically elevated. She had a type I renal tubular acidosis that required high doses of daily potassium.
A magnetic resonance imaging scan revealed a fracture of the right femoral neck necessitating internal fixation. The patient incidentally reported that the tips of her fingers had increased in size over the past six months. On examination, she had clubbing of her fingers with no skin lesions, joint swelling or tenderness. She had no history of lung disease, cardiac disease, neoplasm or liver disease to explain the clubbing. Her creatinine level on admission was 4.4 mg per dL (390 mmol per L).
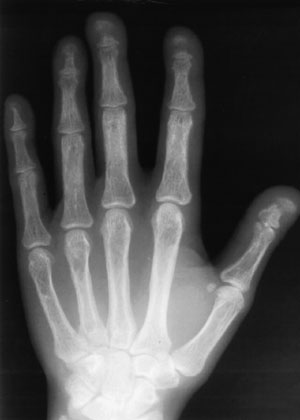
A radiograph of the patient's right hand was obtained (see the accompanying figure).
Question
Discussion
The correct answer is B: hyperparathyroidism. In this patient, hyperparathyroidism is secondary to renal osteodystrophy. The hip fracture and clubbing are consistent with hyperparathyroidism. The radiograph demonstrates subperiosteal resorption, which causes a fine lace-like irregularity along the outer margins of the cortical surface of the distal phalanges.
Rheumatoid arthritis is a synovitis of the peripheral joints that most commonly occurs in persons who are between 20 and 60 years of age. Morning stiffness, symmetric joint swelling and pain with motion are classic symptoms. Radiographic findings include soft tissue swelling and erosions, usually at the proximal interphalangeal joints, ulnar deviation in the phalanges and joint space narrowing.
Pseudohypoparathyroidism is a congenital disorder in which hypocalcemia is caused by target organ insensitivity to parathyroid hormone (PTH).1 Most patients are of short stature, obese and may have mental retardation. Radiographs of the hands may demonstrate a characteristic shortness of the fourth and fifth metacarpals.
Osteopetrosis (marble bone disease) is a genetic disease with a defect in bone resorption. Reconstruction of bone is impaired because of a defect in osteoclast function. Radiographs demonstrate a uniformly dense sclerotic bone, often with no distinction between the cortical and cancellous areas. There are various forms of osteopetrosis that differ in their clinical presentation and severity. The disorder may be discovered incidentally on radiographs. Other patients may present with fractures, bone pain, cranial nerve palsies and osteomyelitis.2
Heberden's nodes are osteophytes of the distal interphalangeal joint, typically seen in osteoarthritis. The most distal tuft of the phalanx is not involved.
Although subperiosteal resorption is often not detectable in mild or slowly progressive disease, it is a pathognomonic radiographic finding in hyperparathyroidism. Osteopenia is also noted in the radiograph. This osteopenia likely contributed to the patient's hip fracture.
Primary hyperparathyroidism is the result of a parathyroid tumor, usually a single parathyroid adenoma (80 to 90 percent of cases). Multiple adenomas, carcinoma of the gland or ectopic production of PTH associated with malignancy are other causes. The identification of primary hyperparathyroidism has increased (up to 0.1 percent of adult patients), largely because of routine measurement of serum calcium levels.
Secondary hyperparathyroidism is encountered most commonly in patients with chronic renal failure but may occur in association with vitamin D deficiency, renal tubular acidosis or intestinal malabsorption. Hyperphosphatemia and decreased renal production of 1,25 dihydroxyvitamin D3 cause a decrease in serum calcium levels. Chronic hypocalcemia leads to a compensatory parathyroid hyperplasia. The enlarged parathyroid glands may become autonomous in some cases.
Most patients with hyperparathyroidism are asymptomatic or have vague, nonspecific complaints. Hypocalcemia and increased levels of parathyroid hormone are seen early in the course of renal failure and are usually worse in those patients with more severe metabolic acidosis. Occasionally, hypercalcemia can develop in patients with advanced renal failure and who have been receiving long-term dialysis.
The constellation of bone changes seen in secondary hyperparathyroidism is known as renal osteodystrophy. Subperiosteal resorption of cortical bone is the hallmark. Other radiographic findings include osteosclerosis, which manifests as broad bands of increased radiodensity seen most often in the vertebral bodies, and generalized osteopenia.
The patient in this case underwent parathyroidectomy, which is recommended for patients with symptomatic hyperparathyroidism, kidney stones or bone disease. After surgery, the patient developed tetany and generalized paresthesias requiring large amounts of intravenous calcium and oral vitamin D. The symptoms are typically transient, reflecting a rapid decrease in serum calcium levels.