
Am Fam Physician. 2003;68(7):1321-1322
What is gastroesophageal reflux disease?
Gastroesophageal reflux disease, or GERD, is a common digestive problem (say: gas-troess-off-ah-gee-al ree-flux). In GERD, acid from the stomach flows backward into the esophagus.
The lining of the stomach is designed to handle the strong acids that break down food. However, the lining of the esophagus gets irritated when strong acid touches it.
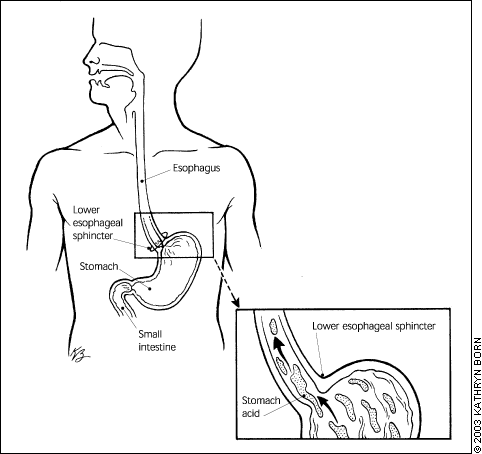
A muscle usually keeps stomach acid from flowing back into the esophagus. If you have GERD, this muscle does not close the right way, and acid from your stomach gets into your esophagus and irritates its lining (see the pictures below).
What are the symptoms of GERD?
The most common symptoms of GERD are heartburn and regurgitation (say: ree-gerj-ihtay-shun). Heartburn is a burning feeling in your chest. This burning feeling may move up toward your throat. If you have regurgitation, stomach contents mixed with acid back up into your esophagus and cause a bad (sour) taste in your mouth.
Less common symptoms of GERD include too much saliva in your mouth and the feeling that you always have a lump in the back of your throat. Some people with GERD have an ongoing cough, a sore throat, or a hoarse voice.
How is GERD diagnosed?
Most likely, your doctor will be able to tell that you have GERD based on your answers to some questions and the results of your physical exam. You may need to have some tests if medicine does not make you feel better or if you have other symptoms (such as chest pain or choking).
How is GERD treated?
Lifestyle changes may help some symptoms of GERD. Here are some things you can do:
Avoid foods that may make your symptoms worse, such as acidic foods (citrus-and tomato-based products), alcohol, chocolate, caffeinated drinks, fatty foods, garlic, onions, and peppermint.
Avoid large meals and do not eat anything for 3 to 4 hours before you go to bed.
Lose weight, if you need to.
Raise the head of your bed by 4 to 8 inches.
If you smoke, stop.
Over-the-counter antacids are sometimes helpful in treating GERD. In addition, your doctor may prescribe a medicine that will help lower the amount of acid in your stomach. Surgery helps some people who do not get better with medicine and lifestyle changes.
How long does GERD last?
The right treatment usually relieves the symptoms of GERD within a few days. However, many people have GERD for a long time. It is common for people to get GERD again.
When should I call my doctor?
You should call your doctor if you have heartburn or regurgitation plus any of the following “alarm” symptoms:
Blood in your stools
Chest pain
Choking
Early fullness after a meal
Pain or difficulty when swallowing
Unexplained weight loss
Vomiting