
Am Fam Physician. 2003;68(11):2239-2241
A 19-year-old woman presented one day after a week-long vacation in Ecuador with a cutaneous eruption localized to her face. In Ecuador, she swam in the Amazon River, ate fresh limes, was bitten by mosquitoes, and painted her face with a yellow pigment from the root of an unidentified plant. At the time of initial evaluation, the patient had multiple, well-demarcated oval lesions in a symmetrical distribution on her face (see accompanying figure). The patient described a prodrome of intense “burning,” followed by the development of erythematous lesions, which filled in from the periphery, resulting in brown macules. Some of the lesions had an exudative discharge, resulting in honey-colored crusts. Lesion development began on the sixth day of the trip, and continued for two weeks after she returned to the United States.
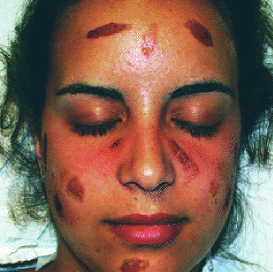
Question
Discussion
The answer is C: phytophotodermatitis. Treatment involved discontinuing contact with and ingestion of limes. Topical triamcinolone was used to decrease the dermatitis, and oral cephalexin was given for secondary impetigo.
Phytophotodermatitis is a phototoxic eruption following skin contact with an irritant plant substance (the yellow root pigment in this case) while in the presence of a systemic photosensitizing compound and ultraviolet radiation. Psoralen, a substance responsible for inducing photosensitization, is found in lemons, limes, bergamot, figs, dill, mustard, parsnip, and garden and wild carrot.1 Lesions develop hours to days after exposure. Areas of erythema, vesicles, or hyperpigmented plaques develop, often in the form of finger marks or streaks corresponding to sites of plant contact with the skin.2 Hyperpigmentation resolves over a period of weeks to months.3
The differential diagnosis for this rash distribution includes allergic contact dermatitis, irritant contact dermatitis, pseudophytophotodermatitis, and chemical burn.
Allergic contact dermatitis is the result of sensitization to an allergen. On re-exposure, patients develop an acute, pruritic, eczematous dermatitis, often with blisters in a linear configuration at the site of contact. Expansion of the cutaneous eruption and accompanying pruritus beyond the original site of exposure distinguishes allergic contact dermatitis from phytophotodermatitis and other irritant rash etiologies.4
Irritant contact dermatitis can occur with plant exposure, usually caused by contact with irritant plant hairs or surface chemicals that are strong primary irritants. Although all people who have contact with an irritant substance will develop a cutaneous eruption, the severity of the reaction correlates with the thickness of the horny skin layer at the site of contact and climatic factors (such as skin temperature and sweating) that affect penetration of the irritant substance.5 Patients with irritant contact dermatitis give a history of itching, burning, and stinging within seconds to minutes after exposure, followed by the development of well-demarcated plaques of erythema, edema, vesicles, erosions, and crusts.6 Irritant contact dermatitis can be exacerbated by phototoxic reactions, as occurred in this patient with phytophotodermatitis. The most commonly reported systemic phototoxic agents include lomefloxacin, nalidixic acid, doxycycline, chlorpromazine, amiodarone, furosemide, and hydrochlorothiazide.6 There also are topical phototoxic agents, such as berloque (used in fragrances), coal tar derivatives, and dyes (for example, yellow cadmium in tattoos).
Patients with pseudophytophotodermatitis often recall an encounter with a specific plant, unaware that arthropods infecting the plants are the actual cause of the cutaneous eruption. Petechiae, wheals, vesicles, and pustules develop in distributions correlating to the locations of exposure.4
Chemical burns may initially present as erythematous plaques, vesicles, or hyperpigmentation in odd shapes, especially when associated with abuse.7
Because many different causes of skin injury, irritation, or sensitization lead to similar, nonspecific rash presentations, careful history-taking is essential in distinguishing which of the many possible etiologies are responsible for a given case of rash.