
Am Fam Physician. 2004;69(9):2185-2186
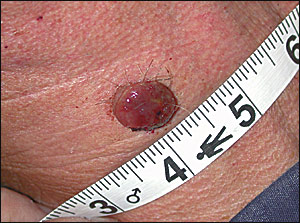
A 67-year-old white man presented with an enlarging lesion on his neck. He first noticed the lesion while shaving six weeks before his visit to the office. He thought it looked like a small blood blister. The lesion had grown significantly during the past six weeks. The patient had no history of similar lesions and no previous injury to the area. Physical examination revealed a soft erythematous exophytic nodule with a small area of ulceration on his right neck that measured 1.5 cm (0.6 in) by 1.5 cm (see accompanying figure). The lesion was excised and sent for pathology.
Question
Discussion
The answer is C: nodular melanoma. It is the second most common form of melanoma, accounting for about 15 percent of all melanomas.1 Nodular melanomas tend to grow vertically, in contrast to superficial spreading melanomas, and thus the prognosis is worse if they are not identified early.
Basal cell carcinoma is the most common type of skin cancer and is associated with sun exposure. It tends to appear as a papule or nodule with an epithelialized, pearly appearance, but may ulcerate in some cases. Basal cell carcinomas rarely metastasize.2
Pyogenic granuloma is a rapidly growing vascular tumor that usually is found in patients younger than 30 years.2 It typically presents as an isolated red nodule that often is ulcerated or friable. One third of the lesions occur at sites of previous skin trauma. Their appearance can be difficult to differentiate from nodular malignant melanoma, emphasizing the need for biopsy of such lesions in older patients, not just destructive therapy.1
Bacillary angiomatosis is a cutaneous vascular tumor associated with a systemic infection by Bartonella species. It occurs almost exclusively in patients infected with human immunodeficiency virus. Treatment is with antibiotics such as erythromycin and tetracycline.3
Squamous cell carcinoma is a malignant tumor of squamous cells. The two most common inciting factors are ultraviolet radiation and human papillomavirus.4 It most commonly occurs in persons with white skin and is typically found in patients older than 55 years.
Nodular melanoma usually arises from normal skin, grows rapidly, and evolves over several months. This type of melanoma is most often a blue or blue-black nodule but may be pink (amelanotic). The depth of the lesion determines its prognosis, with deeper lesions more likely to metastasize. Wide local excision is the treatment recommended for primary melanoma. The depth of the melanoma determines the excision margins. Dacarbazine is the most common chemotherapeutic agent, and interferon-alfa 2b is used as alternate therapy.5 Combination chemotherapy and immunotherapy are being investigated.6
This patient underwent a biopsy of the lesion, which showed malignant melanoma to a depth of 3.55 mm (0.14 in), with metastasis to the lymph nodes in the right neck. The patient was referred to a melanoma specialty clinic.