
This is a corrected version of the article that appeared in print.
Am Fam Physician. 2005;71(6):1062-1064
to the editor: A 35-year-old man with relapsing infections of the upper respiratory tract and nasal bleeding for five months was admitted to our hospital. The patient had been discharged from another hospital after showing no clinical improvement from one month of antibacterial and antituberculous treatment, and refusing to undergo lung operation for the postulated diagnosis of pulmonary abscess.
Physical examination on admission to our hospital showed fever as high as 38.8° C (101.9° F), pulse of 80 beats per minute, and blood pressure of 120/70 mm Hg. The only abnormal findings on physical examination were small blood clots in the nose and ronchi in the upper right lung field. Laboratory tests revealed the following: white blood cell count of 13,230 per mm3 (13.2 × 109 per L [77.9 percent neutrophils, 12.9 percent lymphocytes]); hematocrit level, 36.3 percent; hemoglobulin level, 11.4 g per dL (114 g per L); platelet count, 588,000 per mm3 (5,880 × 109 per L); C-reactive protein 21.74 mg per dL (normal values less than 0.50 mg per dL); and erythrocyte sedimentation rate (ESR), 105 mm per first hour (normal values zero to 20 mm per hour). Laboratory tests for renal function, including urinalysis, were normal. Chest radiography and computed tomography (CT) of the thorax showed a large infiltrate with a central cavitation in the right upper pulmonary field (see accompanying figure). Craniofacial CT revealed ethmoid sinusitis.
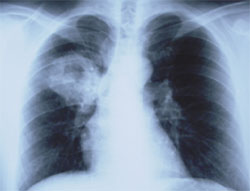
The diagnosis of Wegener’s granulomatosis was suggested by a significantly increased titer of the cytoplasmic-type antineutrophil cytoplasmic antibody (c-ANCA) of 65.3 u (normal: up to 30 u), and was confirmed by histopathologic examination of excised nasal mucosal specimens. The patient received treatment with cyclophosphamide, prednisolone, and cotrimoxazole, which improved symptoms and laboratory test abnormalities.
When fever persists in a patient with a significantly high ESR value, and radiographic and CT findings reveal sinusitis or a large pulmonary infiltrate with a central cavitation, Wegener’s granulomatosis must be considered.1 Differential diagnosis of a pulmonary abscess-like lesion in an imaging test should include bronchial neoplasms (either as necrotizing carcinoma or as the cause of poststenotic cavernous pneumonia that led to an abscess), infectious diseases (like tuberculosis, aspergillosis and other fungal infections, Pneumonocystis carinii pneumonia, and actinomycosis), pulmonary embolism, or vasculitis (primarily Wegener’s granulomatosis).2,3 Surgical lung biopsy may establish the final diagnosis; however, when Wegener’s granulomatosis is suspected, the upper respiratory tract may be involved, making diagnosis less invasively established from histopathologic examination of biopsied nasal specimens.4–6
The diagnostic clue from our patient’s clinical history was the upper respiratory tract symptoms for five months with progressive deterioration and nasal bleeding. Otorhinolaryngologists and other physicians should always have a high index of suspicion because Wegener’s granulomatosis often presents at early stages as a localized form with disease activity limited to the upper respiratory tract.6 In most cases, Wegener’s granulomatosis is diagnosed histologically on biopsy specimens taken from the ear, nose, and throat region. Initially, the disease acute-phase proteins and c-ANCA have a normal value.5 Early diagnosis can lead to early institution of the appropriate treatment and can prevent the irreversible destructive lesions of the disease.