Am Fam Physician. 2011;84(11):1195-1198
Author disclosure: No relevant financial affiliations to disclose.
to the editor: Popliteal artery entrapment syndrome (PAES) is an uncommon cause of leg pain. PAES usually affects young athletes with well-developed calf muscles, who lack risk factors for atherosclerosis. We present a case of an adolescent with bilateral PAES and illustrate why early diagnosis and surgical treatment are important for a good clinical outcome in patients with this condition.
A 17-year-old male soccer player with no relevant medical history presented with progressive pain in his lower legs during training. The pain started about one year prior. He recalled no injury or infection. He described progressive sharp pain and cramps in his calves during training. However, these symptoms disappeared quickly after a moment of rest. His right leg was more affected than his left leg. He had no symptoms while resting or when walking at a normal pace.
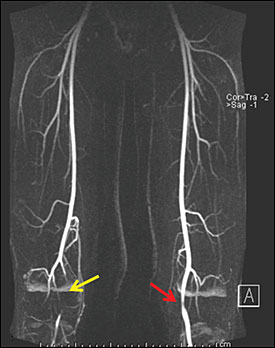
Pulsations of the right dorsalis pedis artery and the right posterior tibial artery were not palpable on physical examination. Pulsations of the right popliteal artery were very weak. The ankle brachial indices for his right leg and left leg were 0.6 and 1.2, respectively. Magnetic resonance angiography (see accompanying figure) demonstrated an occlusion of the left popliteal artery and a significant stenosis of the right popliteal artery. Medial deviation of the popliteal artery around the normally placed medial head of the gastrocnemius muscle led to entrapment of the popliteal artery.
The patient decided to undergo bypass surgery to his left leg because of the extremely disabling symptoms. He had an uncomplicated postoperative course, and his left leg pain disappeared completely. He underwent successful surgery for his right leg six months later and was able to return to playing soccer at his previous level.
PAES was first described in 1879 by T.P. Anderson Stuart.1 Entrapment of the popliteal artery is a syndrome related to an abnormal embryologic development. There is an abnormal relationship between the popliteal artery and the surrounding structures, which can cause unilateral or bilateral compression of the popliteal arteries.2 The incidence of PAES in the general population is unknown.2 It often affects young persons with well-developed leg muscles, like athletes or soldiers. Although rare, if not recognized early, PAES can lead to critical ischemia and serious morbidity. This diagnosis should be considered in young active persons with symptoms of calf and foot claudication.