Illegal drug use continues to be a significant problem in the United States. In 2010, 8.9 percent of Americans 12 years and older reported using an illicit drug in the previous month, including marijuana, cocaine, heroin, hallucinogens, inhalants, and prescription drugs used nonmedically.1 The negative effects of drug use are numerous, and many are well documented in the medical literature. Illicit drug use should be considered in the differential diagnosis of many clinical presentations, especially in patients with positive drug screens or a history of substance abuse, because the list of known deleterious effects is growing. There are an increasing number of case reports involving uncommon adverse effects of commonly abused illicit drugs (Table 1).2–7
Table 1. Uncommon Adverse Effects of Illicit Drug Use

| Drug | Uncommon effect | Treatment | |
|---|---|---|---|
| Cocaine2,3 |
|
| |
| Heroin4,5 |
|
| |
| Marijuana6,7 |
|
| |
Common acute manifestations of marijuana abuse include euphoria, conjunctival injection, and xerostomia. Cannabinoid hyperemesis syndrome is a lesser-known outcome of chronic marijuana use. Recently, clinical criteria have been proposed to aid in the diagnosis of cannabinoid hyperemesis syndrome.6 The condition occurs in susceptible individuals and leads to intermittent severe nausea, hyperemesis, and abdominal pain. A unique finding of this syndrome is temporary relief through compulsive bathing in hot water.7 Definitive treatment of cannabinoid hyperemesis syndrome requires cessation of marijuana use.
Well-known adverse effects of cocaine use include cardiovascular manifestations (e.g., myocardial infarction, arrhythmias), psychiatric conditions (e.g., psychosis, paranoia), and neurologic findings (e.g., headache, stroke, seizures). Recently, however, many cocaine users have presented to health care facilities with an unusual clinical triad of leukopenia, positive autoimmune markers, and dermatologic manifestations.2 This unusual presentation has been linked to the adulteration of cocaine with levamisole, an anthelmintic agent currently used in veterinary medicine. Although it is uncertain why levamisole is added to cocaine, it is undetectable by most street tests for the purity of cocaine, making it useful when a person is trying to “cut” or dilute the drug. Levamisole has also been theorized to increase the euphoria associated with cocaine use. This problem will likely become more recognized, because the Centers for Disease Control and Prevention reported that 69 percent of all cocaine seized in 2009 contained this adulterant.3 Patients who use cocaine containing levamisole often have impressive reticular, purpuric lesions on the ears and extremities due to underlying vasculitis (Figure 1). Assuming there are no superimposed infections, the effects often resolve with the cessation of use of the adulterated cocaine and supportive care.
Figure 1.
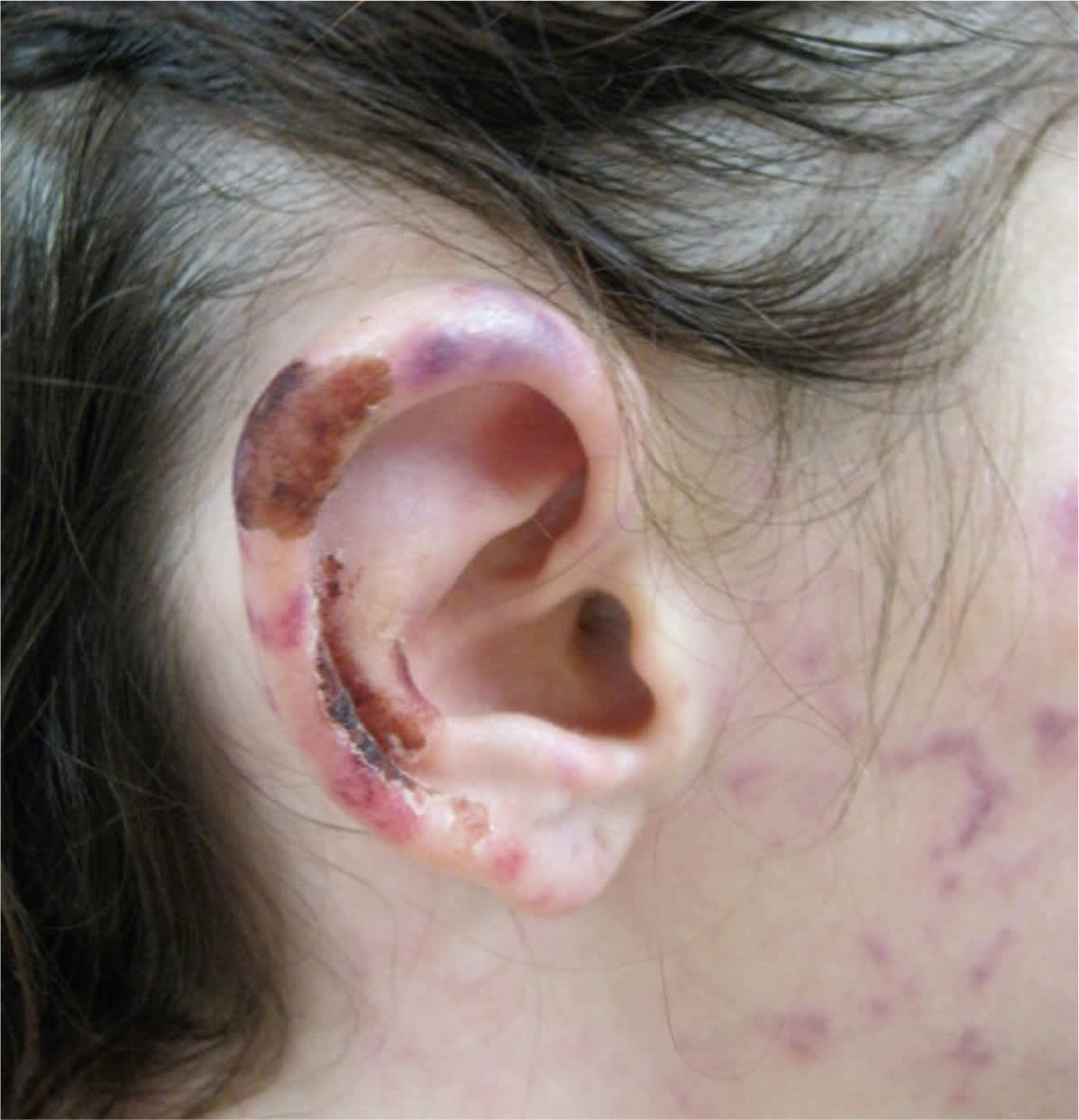
Reticular, purpuric lesions caused by the use of cocaine contaminated with levamisole.
Acute heroin intoxication is known to cause euphoria, miosis, xerostomia, bradycardia, hypotension, and respiratory depression. Less common effects include transverse myelitis and rhabdomyolysis with subsequent acute kidney injury.4,5 The underlying mechanism of these effects is not known, and the patient's description of symptoms may be vague, leading to a delay in clinical recognition. Denial of drug use may further hinder recognition. Prompt treatment of transverse myelitis and rhabdomyolysis is imperative to minimize any long-term sequelae. Transverse myelitis should be treated with corticosteroids. Rhabdomyolysis is treated with aggressive rehydration to prevent kidney injury.
Because of the social implications related to illicit drugs, patients may conceal their use of these substances, further complicating a difficult diagnosis. Promptly beginning the cessation discussion is an important aspect in the overall treatment of adverse effects from illicit drug use. Family physicians are often the first to recognize serious drug abuse. They can be especially helpful to these patients by remaining actively involved in their care as the patients receive comprehensive, multidisciplinary treatment for substance abuse and addiction.

