The notion that sodium restriction might be of value for patients with heart failure has been around since at least the 1940s.1 In recent years, sodium restriction has become a standard component of heart failure treatment. A variety of professional organizations now recommend that patients with heart failure, and indeed all adults, limit their sodium intake because of concerns that high sodium intake leads to adverse cardiovascular outcomes.
Many physicians are unaware, however, that there is controversy about the degree to which they should encourage patients with heart failure to restrict their sodium intake. Several recent studies suggest that there may be no benefit to aggressive sodium restriction in persons with heart failure, and in fact, there may be harm.
Of particular relevance to family physicians, who often see patients with heart failure, is a 2008 study of outpatients with stable heart failure. The study included 232 patients who had been discharged from the hospital after an exacerbation of heart failure and who were in stable condition at the time of their one-month follow-up visit.2 The patients were randomized at the one-month visit to consume a low-sodium diet (an average of 1,840 mg per day) or a normal-sodium diet (approximately 2,800 mg per day). Patients in both groups received high-dose diuretic therapy and were advised to limit fluid intake to 1 L per day. On follow-up six months later, the group consuming a low-sodium diet had experienced a higher rate of readmission to the hospital (26.3% vs. 7.6%) and more deaths. One explanation suggested for these differences is that sodium restriction combined with diuretic therapy leads to higher levels of aldosterone and renin secretion, and this may adversely affect cardiac function. Patients in the sodium-restricted group also had lower serum sodium levels and higher creatinine levels (2.1 mg per dL [186 μmol per L] vs. 1.5 mg per dL [133 μmol per L]), which could be further indication of the deleterious effects of sodium restriction; however, these differences may simply have been the result of fluid restriction and high-dose diuretic therapy rather than sodium restriction.
In another study, patients hospitalized with decompensated heart failure were randomized to a diet with sodium restriction (800 mg per day) plus fluid restriction or to a standard hospital diet. Follow-up results showed no advantage to sodium restriction. There was no difference in weight loss between patients on low-sodium vs. standard diets (the study was powered to detect a weight loss of 2 kg [4.44 lb] during the first two days of hospitalization). There was also no difference in clinical improvement scores or 30-day readmission rates.3
One of the aforementioned studies and five others were included in a systematic review and meta-analysis of clinical trials involving a total of more than 2,500 patients with heart failure. In all six trials, the patients were randomized to intervention groups that consumed a sodium-restricted diet (less than 1,800 mg per day) or to control groups that did not restrict sodium (2,800 mg per day).4 Compared with the control groups, the sodium-restriction groups had nearly double the rate of all-cause mortality and more than double the rate of readmission for heart failure. After the publication of the systematic review, it was discovered that patients in two of the trials were the same patients. For this reason, the results of the analysis have been called into question, and the article reporting the results has been retracted pending further analysis of the original data.5 Despite the uncertainty raised by the retraction, it was one of the largest analyses of the issue of sodium restriction in patients with heart failure, and its results had been considered in a 2013 report from the Institute of Medicine on the benefits and risks of sodium restriction.6 Furthermore, all six trials reported that among patients randomized to a sodium-restricted diet, there was an increased rate of heart failure–related readmissions to the hospital, and the four trials that evaluated mortality rates all showed higher rates among those randomized to a sodium-restricted diet. So, the findings of the meta-analysis should still be taken seriously.
Given this controversy, what should clinicians do about sodium restriction in persons with heart failure? Should sodium restriction be recommended? Current thinking is that the effects of sodium restriction in patients with established cardiovascular disorders, including heart failure, likely follow a J-shaped curve (Figure 1), in which reducing sodium intake below the high levels typically consumed by American adults is beneficial, but marked sodium restriction is not beneficial and carries risk. It is unclear what degree of sodium restriction is optimal; however, analyses by the Institute of Medicine and others suggest that a sodium intake less than 2,300 to 2,500 mg per day may be undesirable for patients with established cardiovascular disease because it has no clear benefit and may carry risk.6,7 Therefore, based on current evidence and until further studies are completed, patients with heart failure should probably be discouraged from reducing their sodium consumption to less than 2,300 mg per day.
Figure 1.
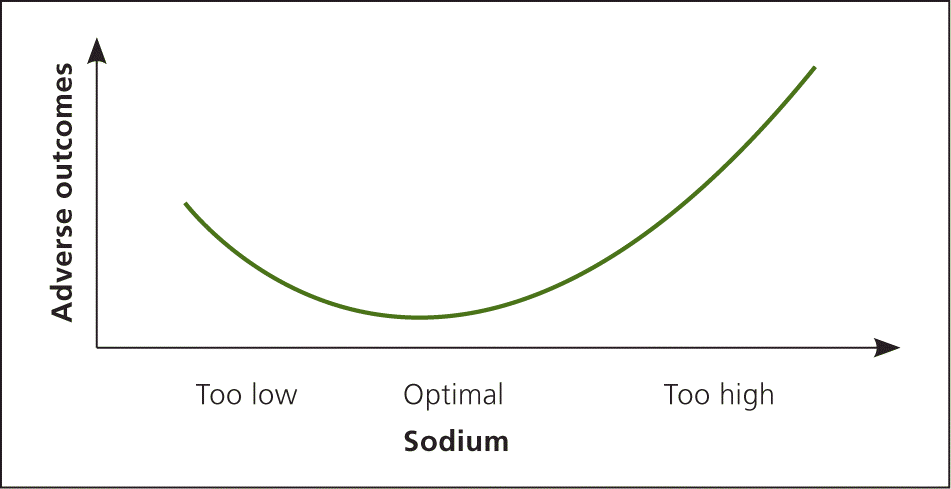
J-shaped curve for sodium consumption. On the J-shaped curve, reduction of sodium consumption below the optimal level appears to increase the risk of adverse outcomes for patients with heart failure, including higher rates of hospital readmission and higher rates of death. But, sodium consumption above the optimal level increases the risk of adverse outcomes to a far greater degree.
The possibility that aggressive sodium restriction may lead to unfavorable outcomes in patients with heart failure should not, however, be misconstrued as meaning that we should lose our focus on reducing sodium intake in the general population. The average American adult consumes 3,000 to 5,000 mg of sodium per day,8 which is on the far right-hand upslope of the J-shaped curve in Figure 1. Because such high sodium intake is strongly associated with development of cardiovascular disorders, there is still an urgent need for Americans to reduce their sodium consumption.9,10
editor's note: Dr. Weiss is an associate medical editor for American Family Physician.

