
Am Fam Physician. 2017;95(12):796-797
Author disclosure: No relevant financial affiliations.
Clinical Question
Which patients with nonalcoholic fatty liver disease (NAFLD) have a low likelihood of fibrosis or cirrhosis?
Evidence Summary
NAFLD is defined as hepatic steatosis on imaging or histology in the absence of other etiologies for secondary fat accumulation. It is usually identified during the evaluation of elevated transaminase levels in a patient without heavy alcohol intake, or found incidentally on imaging studies. The estimated median prevalence in the general population is 20% worldwide,1 and is an estimated 10% to 35% in the United States.2 Nonalcoholic steatohepatitis is a subset of NAFLD characterized by hepatic inflammation and evidence of hepatocyte injury with or without fibrosis, and is associated with an increased risk of cirrhosis and hepatocellular carcinoma.2 The prevalence of biopsy-proven nonalcoholic steatohepatitis in U.S. patients with NAFLD is about 3% to 5%.2
Although liver biopsy remains the standard test for diagnosing fibrosis, it is invasive with significant associated risks. Therefore, a noninvasive method for identifying those at low risk of fibrosis in whom liver biopsy can be avoided would be useful.
Several noninvasive scoring systems using readily available parameters have been proposed to identify advanced fibrosis in patients with NAFLD. These include the aspartate transferase to platelet ratio index3; the alanine transferase ratio4; and the BARD score,5 which comprises the weighted sum of three variables (body mass index [BMI] of 28 kg per m2 or more, aspartate transferase to alanine transferase ratio, and the presence of diabetes mellitus). The FIB-4 score has similar variables as the aspartate transferase to platelet ratio index, with the addition of age.6 Finally, the NAFLD fibrosis score includes age, BMI, blood glucose levels, transferase levels, platelet count, and albumin levels.7 It identifies low-, moderate-, and high-risk groups. However, there is no good prospective evidence that identifying and evaluating high-risk groups with liver biopsy leads to improved health outcomes.
Pooled data from a meta-analysis of 13 studies with 3,064 patients compared the diagnostic accuracy of noninvasive clinical scoring systems using liver biopsy as a reference standard.8 Three scoring systems were evaluated: NAFLD fibrosis score; BARD score; and transient elastography (Fibroscan), an ultrasound-based technique that uses measured liver stiffness to estimate fibrosis.9 The NAFLD fibrosis score was the best scoring system to predict fibrosis with regards to ease of use, cost, and independent validation across various populations. The low-risk group has a negative likelihood ratio (LR–) of 0.17 for advanced fibrosis (stage 3 or more on the annual fibrosis progression rate), whereas the high-risk group has a positive likelihood ratio (LR+) of 20.3 for advanced fibrosis.
A systematic review of nine studies with 3,425 patients found summary estimates for sensitivity and specificity of 90% and 97%, respectively, and an area under the receiver operating characteristic curve (AUROC) of 0.85 for the NAFLD fibrosis score.10 A 2016 meta-analysis of four studies with 1,038 patients compared the FIB-4 score, NAFLD fibrosis score, and BARD score.11 The FIB-4 score with a low cutoff of 1.3 had better diagnostic accuracy for advanced fibrosis than the other scoring systems, using pooled summary receiver operating curves. The AUROC was 0.85; however, this finding was of limited value because of a low specificity of 0.69 and a low LR+ of 2.95. In the same study, pooled data regarding the NAFLD fibrosis score had an AUROC of 0.84 for the lower cutoff, with an LR+ of 3.1 and LR– of 0.32. For the high cutoff of 0.68, the AUROC was lower at 0.65; however, the LR+ of 11.6 was very good.
The FIB-4 score and NAFLD fibrosis score are recommended for identifying patients at risk of fibrosis. The NAFLD fibrosis score has the benefit of a good negative predictive value for excluding fibrosis, an important consideration. The NAFLD fibrosis score has also been the most extensively validated tool for identifying those with advanced disease. The American Gastroenterological Association, American Association for the Study of Liver Diseases, and American College of Gastroenterology recommend its use for determining the need for liver biopsy.1 The score is also available as a free online calculator at https://www.mdcalc.com/nafld-non-alcoholic-fatty-liver-disease-fibrosis-score.
Patients with an NAFLD fibrosis score less than the low cutoff can reliably be considered at low risk of fibrosis and can be managed by their primary care physicians (Figure 18 ). Patients with an indeterminate or high risk using the high cutoff warrant further investigation, including fibrosis biomarker identification, imaging, and possible referral for liver biopsy.10
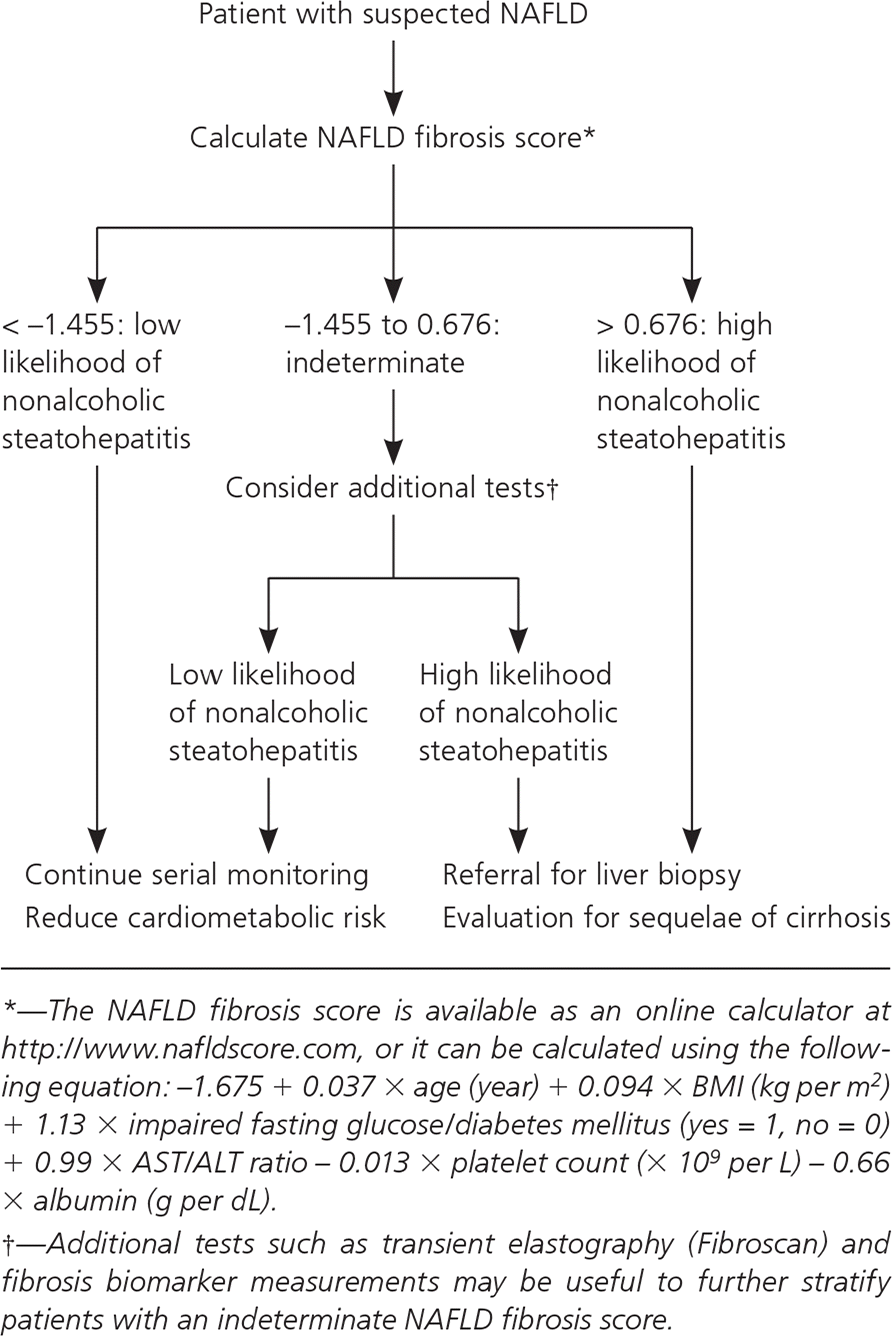
Applying the Evidence
A 56-year-old woman with a BMI of 32 kg per m2 has a mild elevation of transaminase levels on routine screening. Her aspartate transferase level is 83 U per L (1.39 μkat per L), normal = 10 to 40 U per L (0.17 to 0.67 μkat per L); and alanine transferase is 100 U per L (1.67 μkat per L), normal = 7 to 56 U per L (0.12 to 0.94 μkat per L). Other pertinent laboratory findings include a serum albumin level of 4.4 g per dL (44 g per L), normal = 3.5 to 5.5 g per dL (35 to 55 g per L); and a normal complete blood count, with a platelet count of 230 × 103 per mm3 (230 × 109 per L). Ultrasonography shows fatty infiltration of the liver. She does not have impaired glucose tolerance, and she does not drink alcohol. How should this patient be managed?
Answer: Using the online calculator (https://www.mdcalc.com/nafld-non-alcoholic-fatty-liver-disease-fibrosis-score), she has an NAFLD fibrosis score of −1.667, which is less than the low cutoff of −1.455. Thus, the probability that she has significant fibrosis is low, and she can be treated by her primary care physician.