
Am Fam Physician. 2017;96(9):online
Author disclosure: No relevant financial affiliations.

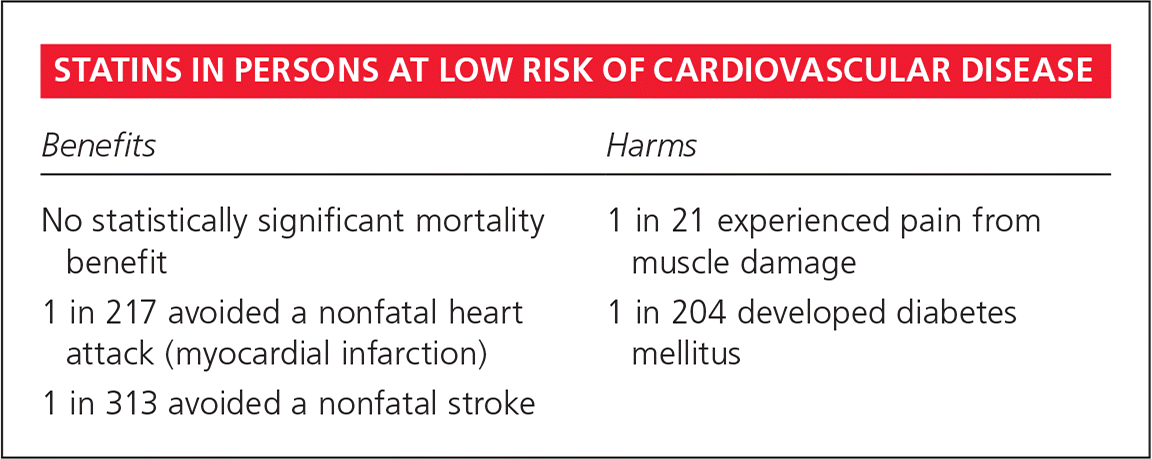
| Benefits | Harms |
|---|---|
| No statistically significant mortality benefit | 1 in 21 experienced pain from muscle damage |
| 1 in 217 avoided a nonfatal heart attack (myocardial infarction) | 1 in 204 developed diabetes mellitus |
| 1 in 313 avoided a nonfatal stroke |
Details for This Review
Study Population: Adult patients, typically 50 to 70 years of age, at varying cardiovascular risk levels but primarily without pre-existing cardiovascular disease; most studies enrolled patients with some elevation in blood cholesterol, and most performed run-out phases (i.e., removing those who did not tolerate the drug or take it consistently)
Efficacy End Points: Death, heart attack (myocardial infarction), stroke
Harm End Points: New-onset diabetes mellitus, muscle symptoms
Narrative: Statins may prevent clotting events by reducing cholesterol and arterial plaque in blood vessels. Vascular diseases are important causes of death and disability, and there is evidence that statins reduce mortality, heart attacks, and strokes in those at high risk (20% or higher 10-year risk of cardiovascular disease).1 Whether the drugs should be used for persons at lower risk, however, is controversial.2
The summary of the 2012 Cholesterol Treatment Trialists (CTT) meta-analysis is unique because it shows trial results according to baseline risk.3 For nonfatal stroke and nonfatal heart attack, the CTT meta-analysis does not show outcomes based on risk and does not report them separately from fatal events. Therefore, the U.S. Preventive Services Task Force (USPSTF) review of statins for primary prevention is used for these end points.4 The occurrence of adverse effects associated with statins is summarized from three sources: the USPSTF summary of serious adverse events (generally, all illnesses and those requiring hospitalization),4 one randomized trial of statin-induced muscle damage,5 and the largest meta-analysis of statin-induced diabetes.6
The CTT meta-analysis, which included 22 trials with more than 130,000 patients, showed no statistically significant mortality benefit from statins in the two low-risk groups (lower than 10% and lower than 20% 10-year risk), separately and combined.3,7 Conversely, the USPSTF, pooling data from 15 trials with more than 70,000 patients, found that 0.4% fewer patients taking a statin died than patients taking placebo (number needed to treat [NNT] = 250).4 Importantly, some of the trials in the USPSTF analysis included high-risk patients or patients with cardiovascular disease.
The USPSTF found that statins have a 0.46% absolute benefit (NNT = 217) for non-fatal heart attacks.4 This NNT is probably artificially improved (lowered) by the predominance of events that occurred in high-risk individuals. In trials, however, 30% to 40% fewer heart attacks occurred in statin groups compared with placebo groups, suggesting that the benefit is reliable and can therefore be accepted as the best available estimate. Nonfatal strokes occurred in 0.32% fewer patients taking statins (NNT = 313), with the same caveats.4
Importantly, despite the small reductions in nonfatal heart attacks and strokes, statins were not associated with a reduction in serious illness overall (relative risk = 0.99; 95% confidence interval, 0.94 to 1.04).4 Adverse events from statin use include myalgia and new-onset diabetes at a rate of 4.8% (number needed to harm [NNH] = 21) and 0.49% over five years (NNH = 204), respectively.5,6 Other adverse events, although often reported, have not been well studied.
Caveats: There is controversy about whether statins reduce all-cause mortality in low-risk persons—analyses finding a mortality benefit universally included some high-risk patients. Although statins provide a significant reduction in mortality in high-risk groups, this benefit has not been shown in lower-risk groups. This could be because of underpow-ered trials (i.e., insufficient numbers of low-risk patients included). If so, any mortality benefit would be small and would result in a very large NNT.
The importance of the adverse effects of statins, although historically minimized, is becoming increasingly apparent.8 The Effect of Statins on Skeletal Muscle Function and Performance (STOMP) trial found that statin-induced myalgias are relatively common at 4.8%.5 The trial also found that patients taking statins commonly have increased creatine kinase enzyme levels, indicating some degree of muscle damage. The 4.8% incidence of statin-induced myalgias is almost certainly an underestimation because the STOMP trial enrolled patients for six months, which is one-tenth of the median duration of trials testing benefits. Because it is unclear if the incidence of statin-related muscle symptoms increases with time, the results cannot be extrapolated forward. Clinicians and patients should be aware that the true incidence of statin-related muscle symptoms is likely higher than reported in the STOMP trial. It should also be noted that only one of the 42 trials included in a meta-analysis addressing statin-induced muscle problems prospectively inquired about muscle symptoms.9
The USPSTF review found no increase in the risk of new-onset diabetes associated with statin therapy for primary prevention.4 However, the best predictor of developing statin-induced diabetes is diabetes risk, not cardiovascular risk.10 Therefore, analyzing exclusively primary prevention data may have underpowered the analysis. A 2010 meta-analysis of 13 trials with more than 90,000 patients, which is broadly cited as the most complete assessment of statin-induced diabetes, shows a 9% relative increase (not far from the USPSTF's result of 5%) in diabetes risk.6 The absolute increase was 0.098% per year of statin exposure.6 This becomes 0.49% at five years, although the number will vary with diabetes risk, just as statin benefits vary with cardiovascular risk.
In summary, studies have found no significant overall mortality benefit with statin therapy in low-risk patients, as well as no reduction in the risk of serious illness overall and very small benefits for nonfatal heart attack and stroke. Statins also appear to cause diabetes. Although this is uncommon, diabetes may occur more often than the prevention of a heart attack or stroke in patients taking statins. It appears that the existing evidence is in disagreement that statins should be used for patients with a 10-year cardiovascular risk below 20%.4,11,12 With no mortality benefit, no reduction in serious illness, an approximately 1% chance of avoiding a nonfatal heart attack or stroke, a similar or greater chance of developing diabetes, and a one in 21 chance of muscle damage, it seems wiser to focus on lifestyle changes (such as adopting a Mediterranean diet, exercising, and not smoking) instead of cholesterol drugs in low-risk patients. These individuals should be informed of the known risks and benefits of statins, and the decision to start statin therapy should be shared by the patient and physician, rather than imposed by guidelines.
We have categorized statins for low-risk patients as red, or not recommended, based on certain value judgments. Statin studies, mostly industry sponsored, used methods such as run-out phases, and the raw trial data continue to be withheld by manufacturers despite many requests by independent groups.13 Thus, it is reasonable to assume that the reported benefits represent a best-case, whereas harms are most likely underestimated. In addition, although statin-induced muscle symptoms are at least five times more likely than any benefit, this is typically reversible. The decision not to categorize statins for low-risk patients as black, or harms greater than benefits, is based on value judgments about this compared with cardiovascular events. This decision becomes trickier when considering the additional burden of statin-induced diabetes. One large, high-quality trial did not find an increase in diabetes risk.14 However, originally unpublished results from the Stroke Prevention by Aggressive Reduction in Cholesterol Levels trial failed to disclose that the NNH for new-onset diabetes was just 38 in patients treated with atorvastatin (Lipitor), 80 mg, compared with placebo.15
Finally, revascularization was not used as an end point because therapeutic decisions are nonstandardized, patients in statin trials are functionally unblinded by lowered low-density lipoprotein cholesterol levels, and the procedure does not save lives or prevent heart attacks in stable patients.16
Copyright 2017 The NNT Group (theNNT.com). Used with permission.
This series is coordinated by Dean A. Seehusen, MD, MPH, AFP Contributing Editor, and Daniel Runde, MD, from the NNT Group.
A collection of Medicine by the Numbers published in AFP is available at https://www.aafp.org/afp/mbtn.
This review is available from the NNT Group at http://www.thennt.com/nnt/statins-persons-low-risk-cardiovascular-disease/.
