
Am Fam Physician. 2018;97(12):815-817
Author disclosure: No relevant financial affiliations.
An otherwise healthy 34-year-old man presented in late fall with a progressive rash that started four days earlier on his hands and then spread to his arms, back, chest, and feet. The rash was mildly pruritic but nontender. He had gingival soreness. He had a mild upper respiratory tract infection one week prior that resolved. He had no recent changes in detergents, soaps, or shampoos. He had no constitutional symptoms.
He went hiking in Pennsylvania five days before the rash appeared, but he did not report any insect bites and had not traveled outside the United States. The patient had one long-term sex partner and no other sexual contacts or history of sexually transmitted infections.
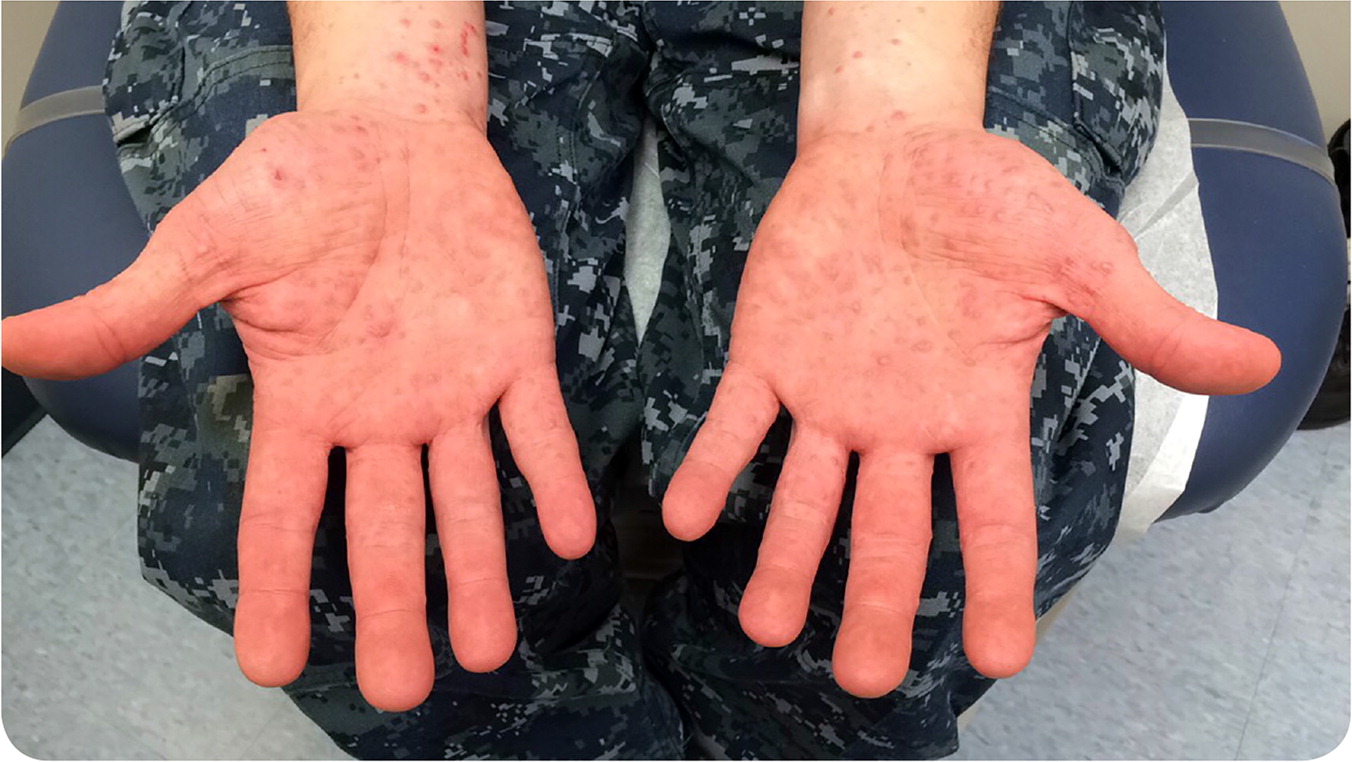
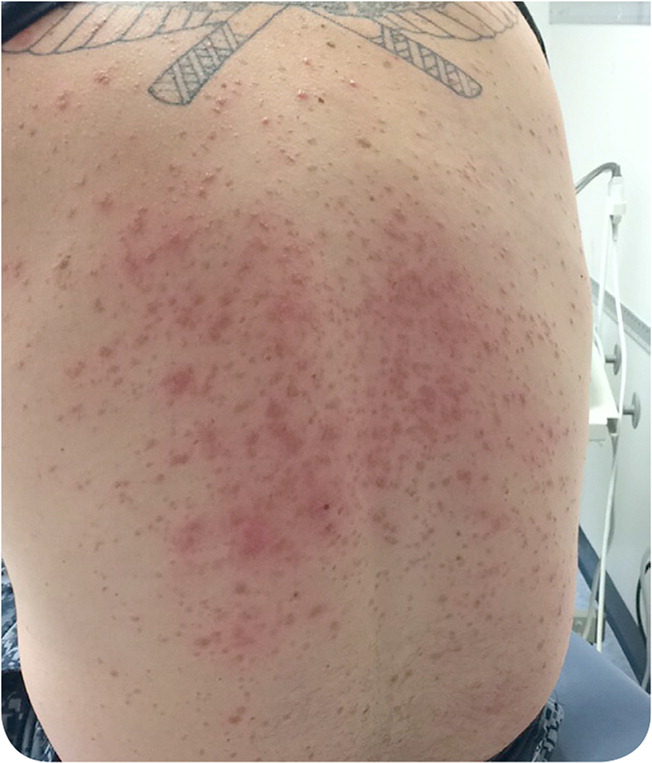
Question
Discussion
The answer is D: Rickettsia rickettsii infection. R. rickettsii is a gram-negative bacterium that causes Rocky Mountain spotted fever. It is transmitted from the bites of various tick species, but one-third of patients with the infection do not report tick bites. Five states (North Carolina, South Carolina, Tennessee, Oklahoma, and Arkansas) account for more than 60% of spotted rickettsial disease cases in the United States.1
Rickettsial disease presents as fever, headaches, myalgias, and gastrointestinal symptoms within two weeks after a tick bite followed by the classic rash, which is characterized by erythematous macules that start around the wrists and ankles and spread across the body. The rash includes papular lesions on the palms and soles but spares the face. However, the rash does not develop in up to 12% of patients.2 In severe cases, a petechial rash can result from the disseminated infection affecting endothelial cells, leading to increased vascular permeability.
Because of the delayed development of serologic markers, antirickettsial agents should be started empirically based on clinical suspicion.3 Rocky Mountain spotted fever can lead to thrombocytopenia, hyponatremia, and elevated liver transaminase levels.
Coxsackie virus is a human enterovirus that can cause hand-foot-and-mouth disease. Although it usually affects children two to 10 years of age, it may also occur in adults.4 Coxsackie virus infection presents as fever and sore mouth progressing to oral lesions, as well as vesicular eruptions and erythematous papules on the palms and soles, and possibly the buttocks and perineum. The diagnosis is typically clinical.
Herpes simplex virus infection is the most common trigger of erythema multiforme.3 Erythema multiforme is an immune-mediated condition characterized by the abrupt onset of erythematous macules that progress to papules and then target lesions. The rash typically favors the face and distal extremities, particularly the dorsal hands and forearms. The rash fully develops within 72 hours and resolves within two weeks.4 Painful vesiculobullous lesions of the mucosa may also be present.
Measles (rubeola), caused by a paramyxovirus, is highly contagious through respiratory spread. It leads to a prodrome of fever, cough, nasal congestion, and rhinoconjunctivitis. The exanthema is a morbilliform eruption, including erythematous macules and papules, that starts on the trunk and spreads to the extremities. Koplik spots (gray-white papules on the buccal mucosa) are pathognomonic. Serologic testing can confirm the diagnosis. Vaccination for measles is 99% effective.5
Treponema pallidum is a sexually transmitted spirochete bacterium that causes syphilis. If left untreated, the disease progresses through three stages. In secondary syphilis, constitutional symptoms, such as low-grade fever, malaise, sore throat, adenopathy, and myalgias, may occur with a generalized maculopapular eruption involving the face, trunk, extremities, palms, and soles.4
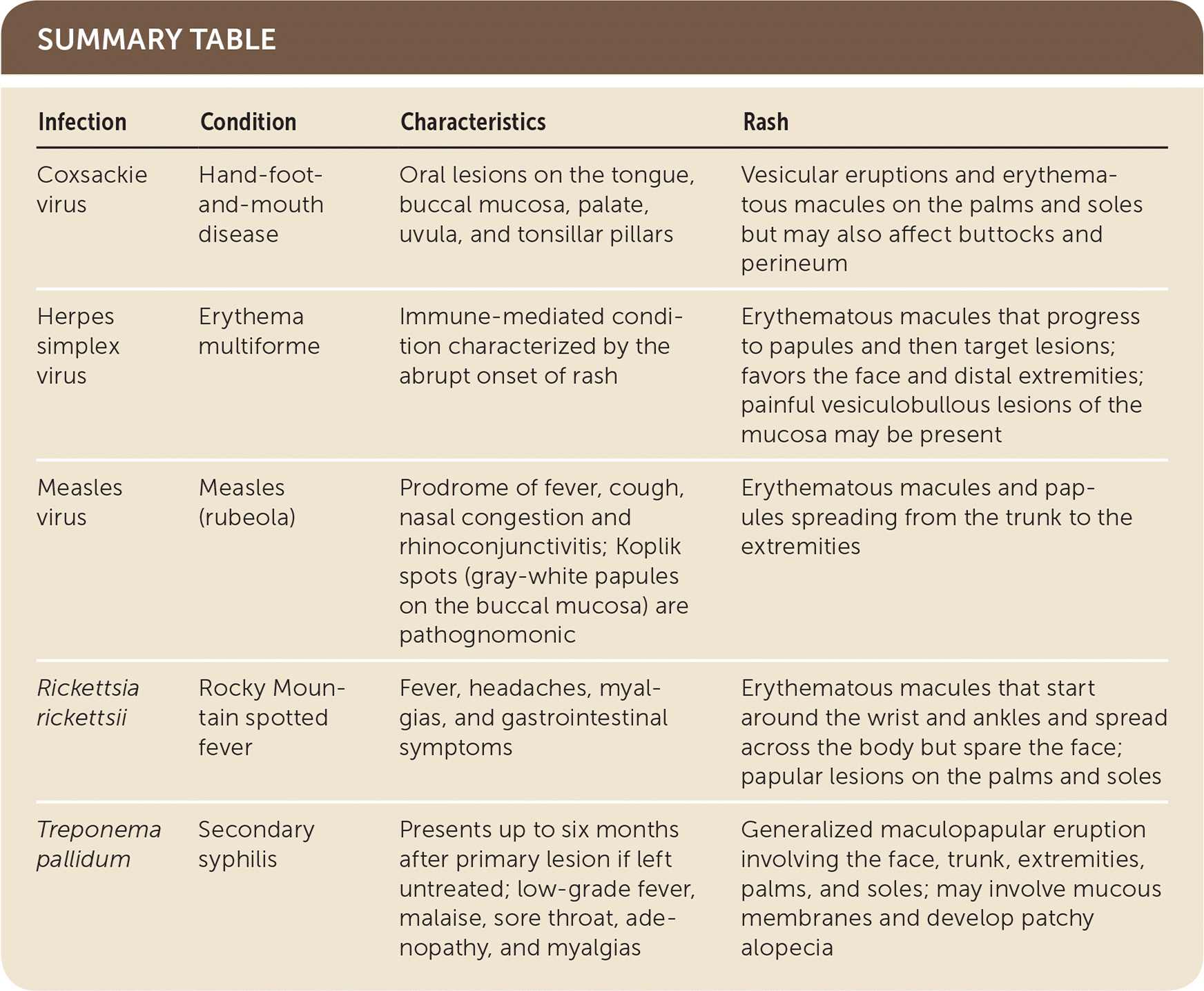
| Infection | Condition | Characteristics | Rash |
|---|---|---|---|
| Coxsackie virus | Hand-foot-and-mouth disease | Oral lesions on the tongue, buccal mucosa, palate, uvula, and tonsillar pillars | Vesicular eruptions and erythematous macules on the palms and soles but may also affect buttocks and perineum |
| Herpes simplex virus | Erythema multiforme | Immune-mediated condition characterized by the abrupt onset of rash | Erythematous macules that progress to papules and then target lesions; favors the face and distal extremities; painful vesiculobullous lesions of the mucosa may be present |
| Measles virus | Measles (rubeola) | Prodrome of fever, cough, nasal congestion and rhinoconjunctivitis; Koplik spots (gray-white papules on the buccal mucosa) are pathognomonic | Erythematous macules and papules spreading from the trunk to the extremities |
| Rickettsia rickettsii | Rocky Mountain spotted fever | Fever, headaches, myalgias, and gastrointestinal symptoms | Erythematous macules that start around the wrist and ankles and spread across the body but spare the face; papular lesions on the palms and soles |
| Treponema pallidum | Secondary syphilis | Presents up to six months after primary lesion if left untreated; low-grade fever, malaise, sore throat, adenopathy, and myalgias | Generalized maculopapular eruption involving the face, trunk, extremities, palms, and soles; may involve mucous membranes and develop patchy alopecia |
