Depression affects an estimated 8% of persons in the United States and accounts for more than $210 billion in health care costs annually. The U.S. Preventive Services Task Force (USPSTF) and American Academy of Family Physicians recommend screening for depression in the general adult population. Additionally, the USPSTF recommends screening children and adolescents 12 to 18 years of age for major depressive disorder. All screening should be implemented with adequate systems in place to ensure accurate diagnosis, effective treatment, and appropriate follow-up. The two-item and nine-item Patient Health Questionnaires (PHQs) are commonly used validated screening tools. The PHQ-2 has sensitivity comparable with the PHQ-9 in most populations; however, the specificity of the PHQ-9 ranges from 91% to 94%, compared with 78% to 92% for the PHQ-2. If the PHQ-2 is positive for depression, the PHQ-9 or a clinical interview should be administered. Screening all postpartum women for depression is recommended by the USPSTF, American Academy of Family Physicians, American Academy of Pediatrics, and American College of Obstetricians and Gynecologists. Women should be screened for depression at least once during the perinatal period using the PHQ-2, PHQ-9, or Edinburgh Postnatal Depression Scale. In older adults, the Geriatric Depression Scale is also an appropriate screening tool for depression. If screening is positive for possible depression, the diagnosis should be confirmed using Diagnostic and Statistical Manual of Mental Disorders, 5th ed., criteria.
Major depression is one of the most common mental health disorders in the United States. Prevalence is estimated at 8% in persons 12 years and older.1 In 2015, an estimated 16.1 million adults 18 years and older had at least one major depressive episode in the previous year, and the condition accounted for 3.7% of all U.S. disability-adjusted life years.2 Globally, more than 300 million persons of all ages have depression, which is the leading cause of disability worldwide.3
WHAT IS NEW ON THIS TOPIC
Depression is a major risk factor for suicide in older men, with suicide rates increasing with age in this population. A recent study showed that men older than 75 years had the highest annual incidence of suicide.
The U.S. Preventive Services Task Force, American Academy of Family Physicians, American Academy of Pediatrics, and American College of Obstetricians and Gynecologists recommend screening all postpartum women for depression. Evidence supports the use of the two- or nine-item Patient Health Questionnaire or the Edinburgh Postnatal Depression Scale.
A 2016 systematic review including three randomized trials with more than 6,500 women found a lower prevalence of postpartum depression at follow-up for those screened four to eight weeks after delivery.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
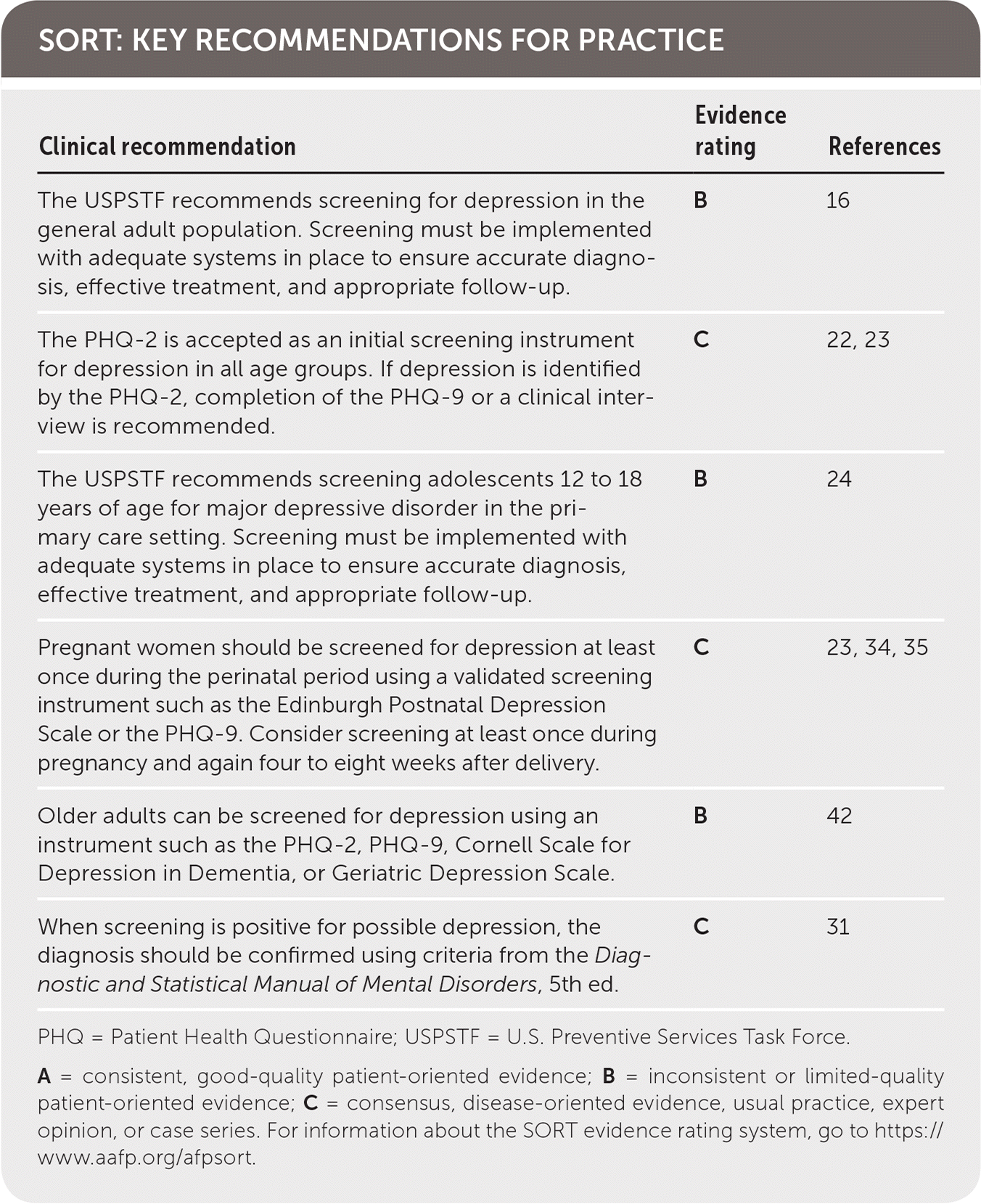
| The USPSTF recommends screening for depression in the general adult population. Screening must be implemented with adequate systems in place to ensure accurate diagnosis, effective treatment, and appropriate follow-up. | B | 16 |
| The PHQ-2 is accepted as an initial screening instrument for depression in all age groups. If depression is identified by the PHQ-2, completion of the PHQ-9 or a clinical interview is recommended. | C | 22, 23 |
| The USPSTF recommends screening adolescents 12 to 18 years of age for major depressive disorder in the primary care setting. Screening must be implemented with adequate systems in place to ensure accurate diagnosis, effective treatment, and appropriate follow-up. | B | 24 |
| Pregnant women should be screened for depression at least once during the perinatal period using a validated screening instrument such as the Edinburgh Postnatal Depression Scale or the PHQ-9. Consider screening at least once during pregnancy and again four to eight weeks after delivery. | C | 23, 34, 35 |
| Older adults can be screened for depression using an instrument such as the PHQ-2, PHQ-9, Cornell Scale for Depression in Dementia, or Geriatric Depression Scale. | B | 42 |
| When screening is positive for possible depression, the diagnosis should be confirmed using criteria from the Diagnostic and Statistical Manual of Mental Disorders, 5th ed. | C | 31 |
PHQ = Patient Health Questionnaire; USPSTF = U.S. Preventive Services Task Force.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
If left untreated, depression may lead to suicide. Persons with an affective disorder have a 0.5% to 4% increased lifetime risk of suicide compared with the general population.4
The economic burden of major depressive disorder is estimated at $210.5 billion per year, with a 21.5% increase from 2005 to 2010.5 Approximately one-half of the costs are attributed to the workplace and one-half to direct medical costs. The burden is significant in the ambulatory care setting, with depression accounting for 10% of physician office visits in 2014.1
Screening for depression is the cornerstone of early recognition, diagnosis, and management. Despite the high prevalence of depression and recommendations for screening, a recent survey of 33,653 physician-patient encounters showed that less than 5% of adults are screened for depression in the primary care setting.6
Risk Factors
The risk factors for depression are multifactorial but can be split into the three broad categories of internal factors, external factors, and adverse life events (Table 1).7–9 Risk factors have been evaluated independently in men and women with no significant differences.7–9
TABLE 1. Risk Factors for Depression

| Internal factors |
| Female sex |
| History of anxiety |
| Low self-esteem |
| Neuroticism* |
| External factors |
| Conduct disorder |
| Substance use |
| Adverse life events |
| Childhood sexual abuse |
| Chronic medical conditions |
| Disturbed family environment |
| History of divorce |
| Lifetime trauma |
| Low educational status |
| Low social support |
| Parental loss |
*—A dimension of temperament marked by elevated stress reactivity resulting in frequent negative emotions.9
Risk factors for late-life depression include female sex, social isolation, death of a spouse, being divorced or separated, lower socioeconomic status, comorbid general medical conditions, uncontrolled pain, insomnia, and cognitive and functional impairments.10 For noninstitutionalized older patients, rates of depression are thought to be similar to those of the general adult population; however, as many as 50% of nursing home residents may be depressed.11 Depression is a major risk factor for suicide in older men, with suicide rates in this population increasing with age. A study showed that men older than 75 years have the highest annual incidence of suicide at 39 deaths per 100,000 men, compared with four deaths per 100,000 women older than 75 years.12
There are numerous medical conditions associated with depression, as mimics of depression or coexisting conditions. Associated neurologic conditions include epilepsy, multiple sclerosis, Alzheimer disease, Parkinson disease, cerebrovascular disease, and traumatic brain injury. Other associated conditions include human immunodeficiency virus infection or AIDS, neurosyphilis, cardiomyopathy, ischemic heart disease, heart failure, hypothyroidism, diabetes mellitus, vitamin deficiencies, parathyroid disorders, irritable bowel syndrome, collagen vascular diseases, and chronic liver disorders.13
Symptoms
Symptoms of depression are commonly known by the SIGECAPS mnemonic: sleep disorders (either increased or decreased sleep); interest deficit (anhedonia); guilt (worthlessness, hopelessness, regret); energy deficit; concentration deficit; appetite disorder (either decreased or increased); psychomotor retardation or agitation; and suicidality. Depressed mood and anhedonia are the two cardinal symptoms of depression. The presence of four SIGECAPS symptoms plus depressed mood or anhedonia suggests depression, and further screening should be considered.
Depression may manifest differently between men and women. Women with depression are more likely to report physical ailments such as headaches, myalgias, or gastrointestinal problems. They are also more likely to exhibit emotional effects such as stress and crying easily.14 Men with depression are more likely to report acts of aggression, anger, substance use disorder, and risky behavior.15
Screening for Depression
ADULTS
The U.S. Preventive Services Task Force (USPSTF) and American Academy of Family Physicians recommend screening for depression in the general adult population, and screening should be implemented with adequate systems in place to ensure accurate diagnosis, effective treatment, and appropriate follow-up.16,17 Screening is recommended for all adults older than 18 years, regardless of risk factors.
There is a lack of evidence to suggest a specific screening interval. The USPSTF suggests a pragmatic approach of screening all adults who have not been previously screened, and using clinical judgment in consideration of risk factors, comorbid conditions, and life events to determine if additional screening of high-risk patients is warranted.16 The Department of Veterans Affairs recommends annual screening.18 The American College of Physicians does not make specific screening recommendations.19 For ease of implementation, one approach is to screen during routine health visits.
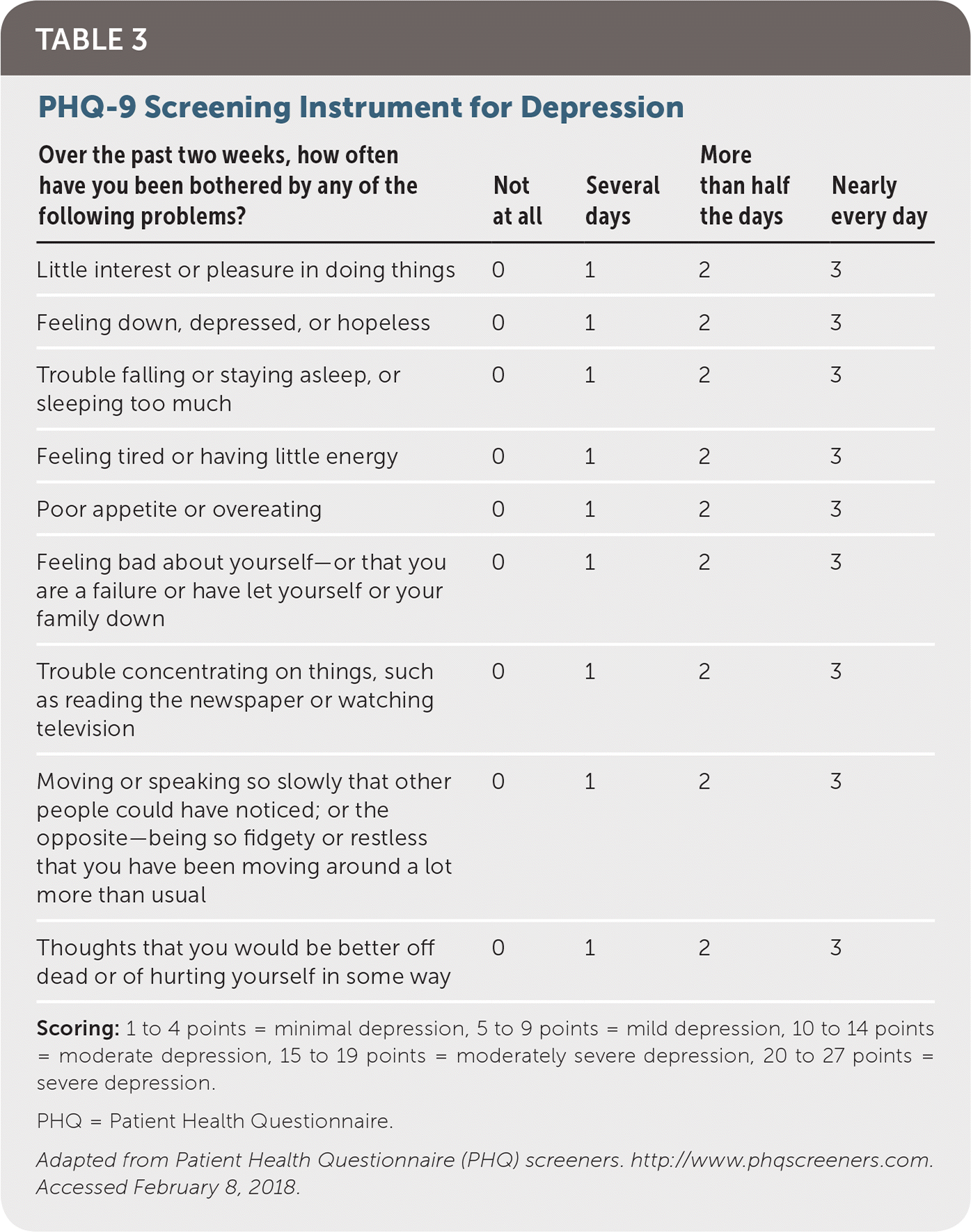
There is a lack of evidence to recommend one screening instrument over another. The two-item and nine-item Patient Health Questionnaires (PHQs) are the most widely used. The PHQ-2 (Table 220 ) has similar sensitivity to the more comprehensive PHQ-9 (Table 320 ), but specificity of the PHQ-9 is higher at 91% to 94%, compared with 78% to 92% for the PHQ-2.21 The PHQ-2 is accepted as an initial screening tool in all age groups. If depression is identified, the PHQ-9 or a clinical interview should be completed.22,23
TABLE 2. PHQ-2 Screening Instrument for Depression

| Over the past two weeks, how often have you been bothered by any of the following problems? | Not at all | Several days | More than half the days | Nearly every day |
|---|---|---|---|---|
| Little interest or pleasure in doing things | 0 | 1 | 2 | 3 |
| Feeling down, depressed, or hopeless | 0 | 1 | 2 | 3 |
Scoring: A score of 3 or more is considered a positive result. The PHQ-9 (Table 3) or a clinical interview should be completed for patients who screen positive.
PHQ = Patient Health Questionnaire.
Adapted from Patient Health Questionnaire (PHQ) screeners. http://www.phqscreeners.com. Accessed February 8, 2018.
TABLE 3. PHQ-9 Screening Instrument for Depression
| Over the past two weeks, how often have you been bothered by any of the following problems? | Not at all | Several days | More than half the days | Nearly every day |
|---|---|---|---|---|
| Little interest or pleasure in doing things | 0 | 1 | 2 | 3 |
| Feeling down, depressed, or hopeless | 0 | 1 | 2 | 3 |
| Trouble falling or staying asleep, or sleeping too much | 0 | 1 | 2 | 3 |
| Feeling tired or having little energy | 0 | 1 | 2 | 3 |
| Poor appetite or overeating | 0 | 1 | 2 | 3 |
| Feeling bad about yourself—or that you are a failure or have let yourself or your family down | 0 | 1 | 2 | 3 |
| Trouble concentrating on things, such as reading the newspaper or watching television | 0 | 1 | 2 | 3 |
| Moving or speaking so slowly that other people could have noticed; or the opposite—being so fidgety or restless that you have been moving around a lot more than usual | 0 | 1 | 2 | 3 |
| Thoughts that you would be better off dead or of hurting yourself in some way | 0 | 1 | 2 | 3 |
Scoring: 1 to 4 points = minimal depression, 5 to 9 points = mild depression, 10 to 14 points = moderate depression, 15 to 19 points = moderately severe depression, 20 to 27 points = severe depression.
PHQ = Patient Health Questionnaire.
Adapted from Patient Health Questionnaire (PHQ) screeners. http://www.phqscreeners.com. Accessed February 8, 2018.
CHILDREN AND ADOLESCENTS
The USPSTF recommends screening adolescents 12 to 18 years of age for major depressive disorder in the primary care setting when systems are in place to ensure accurate diagnosis, effective treatment, and appropriate follow-up.24 This is in accordance with the American Academy of Pediatrics Bright Futures guideline, which recommends annual screening for patients 12 to 21 years of age.22
The two most widely used screening instruments for depression in adolescents are the PHQ for Adolescents and the primary care version of the Beck Depression Inventory. The traditional PHQ-2 may also be used in adolescents; a positive screening (score of 3 or more) should prompt additional assessment for major depressive disorder. In a primary care sample of 499 adolescents, a PHQ-2 score of 1 or more had a sensitivity of 74% and specificity of 75% for detecting major depression.25
PREGNANT AND POSTPARTUM WOMEN
The prevalence of depression in the postpartum period (commonly defined as the first 12 months after birth) has been estimated at 10%.26,27 The onset of postpartum depression occurs during the prenatal and antepartum periods in approximately 50% of pregnancies.28 For cases that begin after delivery, roughly 90% occur in the first four months.29
Postpartum depression has significant effects on the entire family. It is associated with abnormal development, cognitive impairment, and psychopathology in children.30 It can interfere with breastfeeding, maternal-infant bonding, and the mother's relationship with her partner.26 It is often overlooked and may be mistaken for normal behavioral changes that occur during this period, known as the postpartum blues. Postpartum depression is not listed as its own diagnosis in the Diagnostic and Statistical Manual of Mental Disorders, 5th ed. (DSM-5), but rather as a qualifier to the diagnosis of major depressive disorder.31
The USPSTF, American Academy of Family Physicians, and American College of Obstetricians and Gynecologists recommend screening all postpartum women for depression.16,17,23,32,33 Patients should be screened for depression at least once during the perinatal period. Evidence supports the use of the PHQ-2, PHQ-9, or Edinburgh Postnatal Depression Scale (EPDS).33 The Postpartum Depression Screening Scale is a more in-depth tool; however, it requires additional time to administer with more than 20 questions, limiting its use during routine outpatient office visits.
The EPDS is the most commonly used tool, is simple to score, and is available in more than 50 languages.34 In a 2013 systematic review of 11 studies and more than 3,000 postpartum women, a cutoff score of 12 yielded sensitivities and specificities from 80% to 90%.35 The EPDS has been found to be more accurate at identifying women with and without postpartum depression than the PHQ-9 or the Postpartum Depression Screening Scale.36
Screening for postpartum depression appears to be effective. A 2016 systematic review including three randomized trials and more than 6,500 women found a lower prevalence of postpartum depression at follow-up for those screened four to eight weeks after delivery.23 If postpartum depression was diagnosed, improvement or remission of symptoms at follow-up (as measured by the EPDS) was 11% greater in patients who were screened than in those who were not screened.
The American College of Obstetricians and Gynecologists does not include guidance on the specific timing and frequency of screening. One approach is to screen at least once during pregnancy and again four to eight weeks after delivery. The American Academy of Pediatrics recommends that physicians screen mothers for postpartum depression at the infant's one-, two-, and four-month visits.22
Family physicians practicing full-spectrum care have other opportunities to screen for postpartum depression. Screening during infant hospitalizations can identify previously unscreened mothers. A 2016 prospective observational study of mothers screened during infant hospitalizations showed that only 14.6% of these women had previously received appropriate depression screening. Of those screened during the infant hospitalization, 28% had a positive screening result. However, few positive screening results were diagnostically confirmed, partly because of the high number of women lost to follow-up.37
OLDER PERSONS
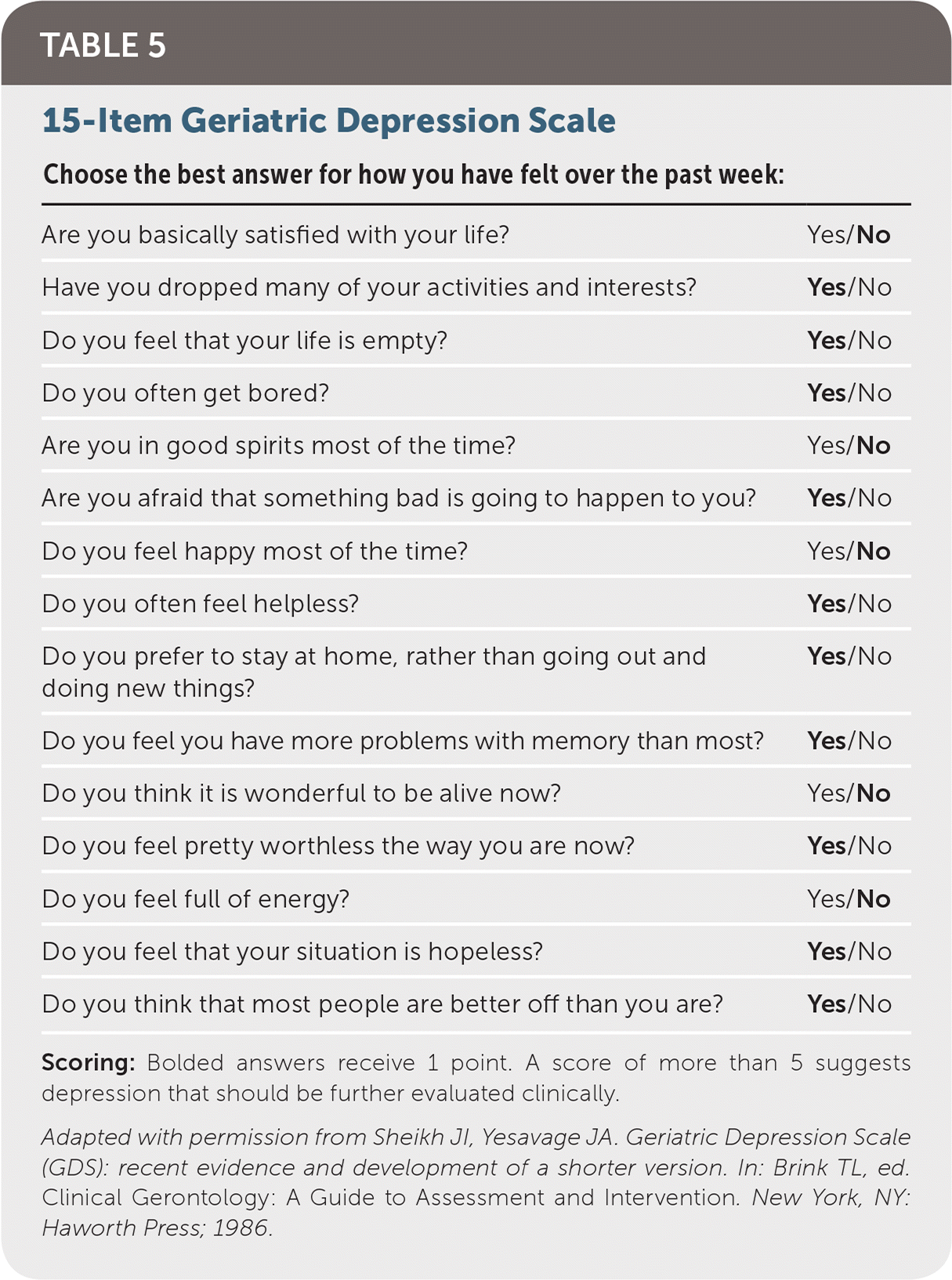
Multiple screening tests have been developed to address the confounding factors that make depression screening and diagnosis more challenging later in life. The Geriatric Depression Scale is a five-, 15-, or 30-item questionnaire that screens for depression in older patients without dementia. Notably, it does not assess for somatic issues because this is thought to interfere with the diagnosis.38 The five-item Geriatric Depression Scale (Table 439 ) was found to have a sensitivity of 94% and specificity of 81%, which are similar to those of the 15-item test (Table 540 ).
TABLE 4. Five-Item Geriatric Depression Scale

| Choose the best answer for how you have felt over the past week: | |
|---|---|
| Are you basically satisfied with your life? | Yes/No |
| Do you often get bored? | Yes/No |
| Do you often feel helpless? | Yes/No |
| Do you prefer to stay at home rather than going out and doing new things? | Yes/No |
| Do you feel pretty worthless the way you are now? | Yes/No |
Scoring: Bolded answers receive 1 point. A score of 2 or more is considered a positive result.
Adapted with permission from Maurer DM. Screening for depression [published correction appears in Am Fam Physician. 2013;87(7):464]. Am Fam Physician. 2012;85(2):142.
TABLE 5. 15-Item Geriatric Depression Scale
| Choose the best answer for how you have felt over the past week: | |
|---|---|
| Are you basically satisfied with your life? | Yes/No |
| Have you dropped many of your activities and interests? | Yes/No |
| Do you feel that your life is empty? | Yes/No |
| Do you often get bored? | Yes/No |
| Are you in good spirits most of the time? | Yes/No |
| Are you afraid that something bad is going to happen to you? | Yes/No |
| Do you feel happy most of the time? | Yes/No |
| Do you often feel helpless? | Yes/No |
| Do you prefer to stay at home, rather than going out and doing new things? | Yes/No |
| Do you feel you have more problems with memory than most? | Yes/No |
| Do you think it is wonderful to be alive now? | Yes/No |
| Do you feel pretty worthless the way you are now? | Yes/No |
| Do you feel full of energy? | Yes/No |
| Do you feel that your situation is hopeless? | Yes/No |
| Do you think that most people are better off than you are? | Yes/No |
Scoring: Bolded answers receive 1 point. A score of more than 5 suggests depression that should be further evaluated clinically.
Adapted with permission from Sheikh JI, Yesavage JA. Geriatric Depression Scale (GDS): recent evidence and development of a shorter version. In: Brink TL, ed. Clinical Gerontology: A Guide to Assessment and Intervention. New York, NY: Haworth Press; 1986.
The Cornell Scale for Depression in Dementia is a 19-item screening tool that can be used in older patients. It retains its validity when used in patients with dementia, unlike the Geriatric Depression Scale. The Cornell Scale for Depression in Dementia has a sensitivity of 93% and specificity of 97%.38
The PHQ-2 can be used in the older population and may have similar effectiveness with greater brevity and ease of use than other instruments. The PHQ-2 has been shown to have a sensitivity nearing 100% and specificity of 77% in non-institutionalized adults older than 65 years.41 In a more recent systematic review, combined data showed a sensitivity and specificity for the PHQ-2 of 91.8% and 67.7%, respectively. The performance of the PHQ-2 is comparable to that of other instruments, including clinician-rated scales, in noninstitutionalized older persons42 and nursing home residents.43
PATIENTS WITH CHRONIC MEDICAL CONDITIONS
The incidence of depression is higher in patients with chronic medical conditions. A Canadian study demonstrated a 1.45 times greater risk of depression in these patients.44 A study of the relationship between depression and diabetes and coronary artery disease specifically showed it to be bidirectional.45 Given these findings, physicians should consider screening patients with chronic medical conditions for depression. Physicians should also be mindful that many symptoms commonly attributed to chronic medical conditions are also symptoms of underlying depression.
Diagnosis of Depression
When screening is positive for possible depression, the diagnosis should be confirmed using DSM-5 criteria, which are presented in Table 6.31 When symptoms do not meet the criteria for depression, other mental health disorders should be considered, such as bereavement, persistent depressive disorder (dysthymia), premenstrual dysphoric disorder, and substance/medication-induced depressive disorder. A major depressive episode must not be better explained by schizoaffective disorder, schizophrenia, or schizophreniform disorder. Bipolar disorder must also be excluded, especially if the patient has ever had a manic or hypomanic episode. Physicians should familiarize themselves with basic screening tools for bipolar disorder.31,46
TABLE 6. DSM-5 Diagnostic Criteria for Major Depressive Disorder

| A. Five (or more) of the following symptoms have been present during the same 2-week period and represent a change from previous functioning; at least one of the symptoms is either (1) depressed mood or (2) loss of interest or pleasure. Note: Do not include symptoms that are clearly attributable to another medical condition. | |
| 1. Depressed mood most of the day, nearly every day, as indicated by either subjective report (e.g., feels sad, empty, hopeless) or observation made by others (e.g., appears tearful). (Note: In children and adolescents, can be irritable mood.) | |
| 2. Markedly diminished interest or pleasure in all, or almost all, activities most of the day, nearly every day (as indicated by either subjective account or observation). | |
| 3. Significant weight loss when not dieting or weight gain (e.g., a change of more than 5% of body weight in a month), or decrease or increase in appetite nearly every day. (Note: In children, consider failure to make expected weight gain.) | |
| 4. Insomnia or hypersomnia nearly every day. | |
| 5. Psychomotor agitation or retardation nearly every day (observable by others, not merely subjective feelings of restlessness or being slowed down). | |
| 6. Fatigue or loss of energy nearly every day. | |
| 7. Feelings of worthlessness or excessive or inappropriate guilt (which may be delusional) nearly every day (not merely self-reproach or guilt about being sick). | |
| 8. Diminished ability to think or concentrate, or indecisiveness, nearly every day (either by subjective account or as observed by others). | |
| 9. Recurrent thoughts of death (not just fear of dying), recurrent suicidal ideation without a specific plan, or a suicide attempt or a specific plan for committing suicide. | |
| B. The symptoms cause clinically significant distress or impairment in social, occupational, or other important areas of functioning. | |
| C. The episode is not attributable to the physiological effects of a substance or to another medical condition. | |
| Note: Criteria A–C represent a major depressive episode. | |
| Note: Responses to a significant loss (e.g., bereavement, financial ruin, losses from a natural disaster, a serious medical illness or disability) may include the feelings of intense sadness, rumination about the loss, insomnia, poor appetite, and weight loss noted in Criterion A, which may resemble a depressive episode. Although such symptoms may be understandable or considered appropriate to the loss, the presence of a major depressive episode in addition to the normal response to a significant loss should also be carefully considered. This decision inevitably requires the exercise of clinical judgment based on the individual's history and the cultural norms for the expression of distress in the context of loss. | |
| D. The occurrence of the major depressive episode is not better explained by schizoaffective disorder, schizophrenia, schizophreniform disorder, delusional disorder, or other specified and unspecified schizophrenia spectrum and other psychotic disorders. | |
| E. There has never been a manic episode or a hypomanic episode. Note: This exclusion does not apply if all of the manic-like or hypomanic-like episodes are substance-induced or are attributable to the physiological effects of another medical condition. | |
DSM = Diagnostic and Statistical Manual of Mental Disorders.
Reprinted with permission from the American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th ed. Washington, DC: American Psychiatric Association; 2013:160–161.
It is reasonable to obtain basic laboratory testing when confirming the diagnosis of depression, especially in older patients, to exclude medical conditions that may mimic depression. Thyroid-stimulating hormone testing may be considered because hypo- or hyperthyroidism may cause fatigue or psychomotor changes, or weight and appetite changes. A complete blood count may be considered to evaluate for chronic infections or malignancy. Patients with anemia may present with fatigue, depression, anorexia, and weight loss. Pernicious anemia may manifest as mood changes and insomnia, warranting vitamin B12 testing. Serum electrolytes and liver function are useful tests in adults because abnormalities such as a sodium imbalance may lead to confusion, weakness, and early delirium, which may mimic depression. Hepatic encepha lopathy may also mimic depression and go unrecognized. Finally, when considering pharmacologic therapy in older patients, it is useful to know about any underlying liver impairment, which could limit the use of some medications.
This article updates previous articles on this topic by Sharp and Lipsky,47 and Maurer.39
Data Sources: A PubMed search was completed in Clinical Queries using the key terms depression and screening. The search included meta-analyses, randomized controlled trials, and reviews. We also searched the Agency for Healthcare Research and Quality evidence reports, the Cochrane database, Family Physicians Inquiries Network, Essential Evidence Plus, DynaMed Plus, Journal Watch, the Prescriber's Letter, and UpToDate. Search dates: June 25, 2017, and July 15, 2018.
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the U.S. Army Medical Department or the U.S. Army at large.

