
Am Fam Physician. 2018;98(8):535-536
Author disclosure: No relevant financial affiliations.
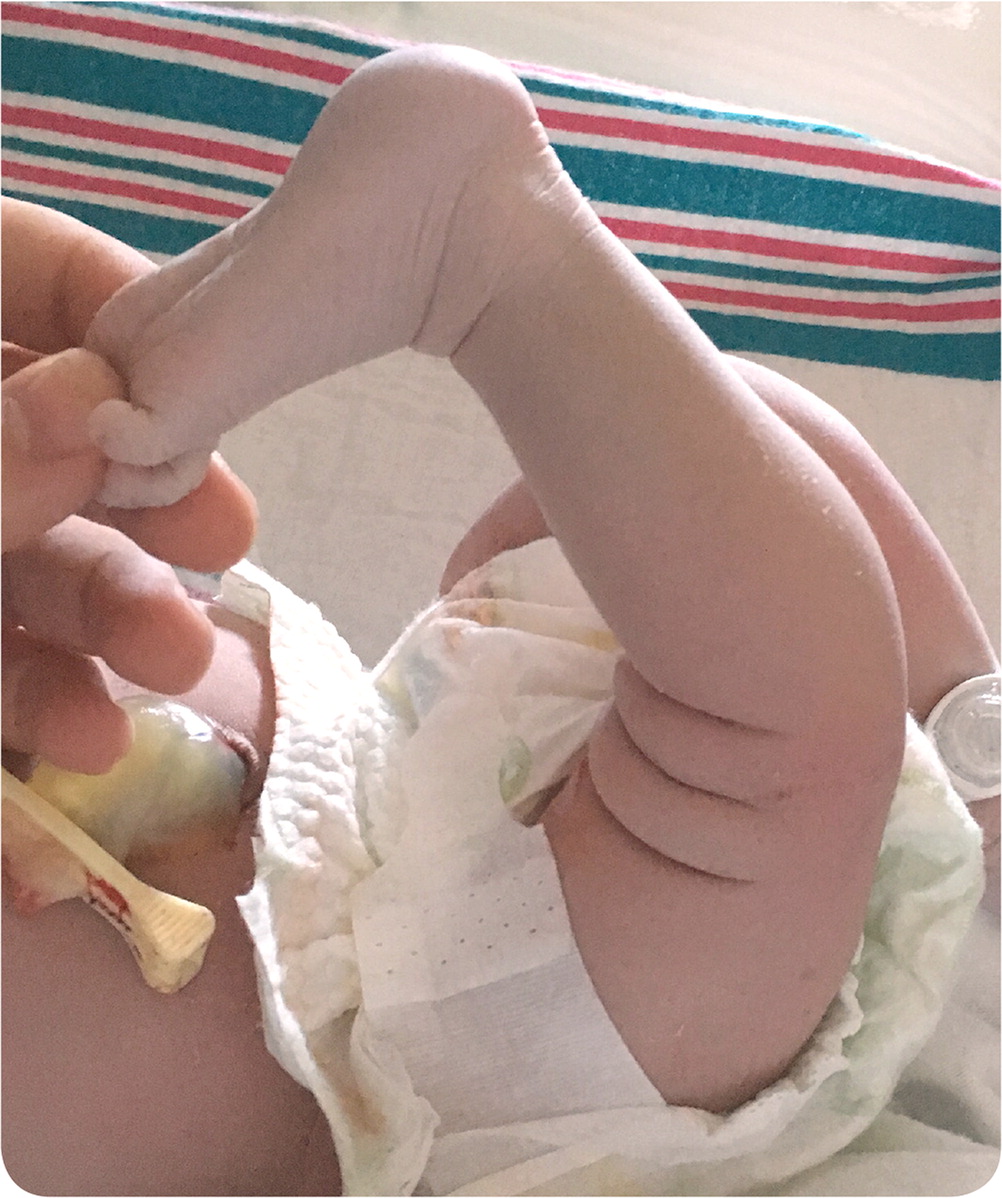
A 32-year-old woman (gravida 5, para 1) delivered a healthy newborn girl at 40 weeks' gestation. The prenatal course was unremarkable. Labor was uncomplicated with a spontaneous vaginal delivery. The initial examination of the infant was notable for passive hyperextension at the right knee (Figure 1) with otherwise full range of motion, including normal flexion. A “pop” was palpated when transitioning from a neutral position to flexion. Barlow and Ortolani hip testing was negative. The remainder of the musculoskeletal examination was normal. The patient's neurovascular status was intact in the lower extremities bilaterally. Radiography of the right knee was negative for fracture or other acute pathology.
Question
Discussion
The answer is C: serial casting. Serial casting is the initial treatment of choice for congenital dislocation of the knee, also known as congenital genu recurvatum. This condition is typically diagnosed at birth by clinical examination findings. The examination will be notable for various degrees of passive hyperextension and associated transverse anterior skin markings. The incidence of congenital dislocation of the knee is approximately one in 100,000.1,2
There are three grades of congenital dislocation of the knee based on the degree of extension, ability to reduce the joint, and stability of the joint.2,3 Grade I is easily reducible, grade II is unstable when reduced, and grade III is irreducible. Congenital knee dislocation is associated with dislocations of the hip, clubfoot, and metatarsus adductus.4,5 The etiology is not well defined, but it is likely related to fetal positioning (i.e., breech), abnormal contracture of the anterior knee capsule or quadriceps, and hypoplastic or absent collateral ligaments.
Surgical correction of congenital knee dislocation primarily involves two procedures: percutaneous quadriceps recession or V–Y quadricepsplasty. These methods are used when nonoperative or conservative treatment fails. Percutaneous quadriceps recession involves division of the fascial layer of the rectus femoris, allowing for further knee reduction. V–Y quadricepsplasty is a more extensive surgery that may include incising the quadriceps tendon, releasing the anterior knee capsule, and mobilizing or reconstructing the collateral ligament. The choice between the two types of surgical repair is dependent on the patient's native anatomy and abnormalities found on examination.3,5
