The prevalence of type 2 diabetes mellitus in children and adolescents has increased worldwide over the past three decades. This increase has coincided with the obesity epidemic, and minority groups are disproportionately affected. The American Diabetes Association recommends screening for type 2 diabetes beginning at 10 years of age or the onset of puberty in children who are overweight or obese and have two additional risk factors. Diagnostic criteria include a fasting blood glucose level of 126 mg per dL or greater, a two-hour plasma glucose level of 200 mg per dL or greater during an oral glucose tolerance test, an A1C level of 6.5% or more, or a random plasma glucose level of 200 mg per dL or greater plus symptoms of polyuria, polydipsia, or unintentional weight loss. Management should be focused on a multidisciplinary, family-centered approach. Nutrition and exercise counseling should be started at the time of diagnosis and as a part of ongoing management. Metformin is the first-line therapy in conjunction with lifestyle changes. Insulin therapy should be initiated if there are signs of ketosis or ketoacidosis, or if the patient has significant hyperglycemia (A1C greater than 9% or a random plasma glucose level of 250 mg per dL or greater).
Type 2 diabetes mellitus is characterized by hyperglycemia with insulin resistance and impaired insulin secretion. In contrast with type 1 diabetes, pancreatic beta cell dysfunction in type 2 diabetes is not mediated by an autoimmune process.
WHAT IS NEW ON THIS TOPIC
Type 2 diabetes accounts for one in three newly diagnosed cases of diabetes in U.S. children and adolescents.
Up to 32% of adolescents with type 2 diabetes have hypertension at the time of diagnosis.
The American Diabetes Association recommends that screening for type 2 diabetes begin at 10 years of age or the onset of puberty in children who are overweight and have two additional risk factors.
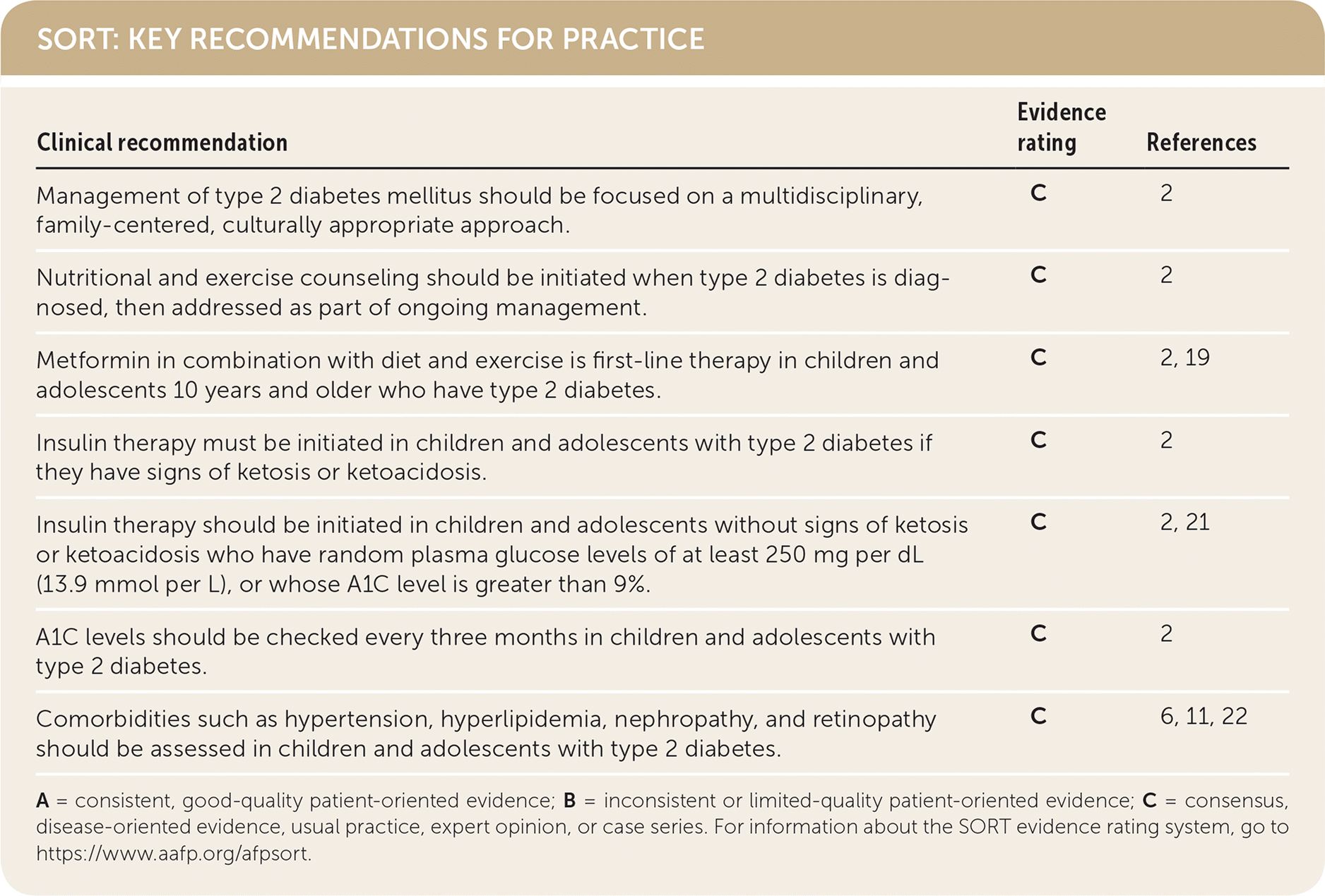
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Management of type 2 diabetes mellitus should be focused on a multidisciplinary, family-centered, culturally appropriate approach. | C | 2 |
| Nutritional and exercise counseling should be initiated when type 2 diabetes is diagnosed, then addressed as part of ongoing management. | C | 2 |
| Metformin in combination with diet and exercise is first-line therapy in children and adolescents 10 years and older who have type 2 diabetes. | C | 2, 19 |
| Insulin therapy must be initiated in children and adolescents with type 2 diabetes if they have signs of ketosis or ketoacidosis. | C | 2 |
| Insulin therapy should be initiated in children and adolescents without signs of ketosis or ketoacidosis who have random plasma glucose levels of at least 250 mg per dL (13.9 mmol per L), or whose A1C level is greater than 9%. | C | 2, 21 |
| A1C levels should be checked every three months in children and adolescents with type 2 diabetes. | C | 2 |
| Comorbidities such as hypertension, hyperlipidemia, nephropathy, and retinopathy should be assessed in children and adolescents with type 2 diabetes. | C | 6, 11, 22 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
The incidence of type 2 diabetes in children and adolescents has increased worldwide over the past three decades.1 Type 2 diabetes accounts for one in three new cases of diabetes diagnosed in children and adolescents in the United States.2 This increase has coincided with the obesity epidemic, and minority groups are disproportionately affected at all ages.3,4 Some studies have shown that children of women with gestational diabetes are at greater risk of type 2 diabetes.5
Physicians and health care systems are ill-equipped to handle the challenges associated with type 2 diabetes in children. Most education materials designed for children address type 1 diabetes.2 This article reviews recommendations from a clinical practice guideline by the American Academy of Pediatrics.2 It also highlights the American Diabetes Association's current clinical practice recommendations.6
Clinical Presentation, Diagnosis, and Screening
Children with type 2 diabetes may present as symptomatic or asymptomatic. As in type 1 diabetes, the symptoms of hyperglycemia include polyuria, polydipsia, and unintentional weight loss. The initial presentation can also include diabetic ketoacidosis. Asymptomatic children (up to 40% of cases) are typically early in the disease process and are often identified during screening for hyperglycemia because of the presence of diabetes risk factors.7
There is considerable overlap between type 1 and type 2 diabetes in children, and patients can have features of both. Although overweight and obesity are associated with type 2 diabetes, 24% of children with type 1 diabetes are overweight at diagnosis.6 Autoantibodies to insulin, islet cell cytoplasm, glutamic acid decarboxylase, tyrosine phosphatase (insulinoma associated), or zinc-activated channels are present in 85% to 98% of children with type 1 diabetes and can be useful in confirming this diagnosis.8 However, glutamic acid decarboxylase and islet antigen-2 antibodies may be present in up to 10% of children with clinically diagnosed type 2 diabetes.9 Reports suggest that up to 25% of children and adolescents who present with ketoacidosis have type 2 diabetes.10
Accurate diagnosis is based on a combination of clinical presentation and the patient history. There are currently no recommendations for diagnostic laboratory testing in children.
The American Diabetes Association recommends screening for type 2 diabetes beginning at 10 years of age or the onset of puberty in children who are overweight (body mass index or weight for height greater than the 85th percentile, or weight for ideal height greater than the 120th percentile) and have two additional risk factors (Table 1).2,6,11,12
TABLE 1 Indications to Screen for Type 2 Diabetes Mellitus in Children and Adolescents

| Patient is overweight (body mass index > 85th percentile for age and sex, weight for height > 85th percentile, or weight for ideal height > 120th percentile) |
Plus any two of the following risk factors:
|
Note: Screening should be performed at 10 years of age or onset of puberty, whichever is earlier. If results are negative, screening should be repeated at least every three years (more frequently if body mass index increases).
Adapted with permission from American Diabetes Association. Type 2 diabetes in children and adolescents. Diabetes Care. 2000;23(3):386, with additional information from references 2, 6, and 11.
Diagnostic criteria for type 2 diabetes in children are the same as for adults: a fasting blood glucose level of at least 126 mg per dL (7.0 mmol per L), a two-hour plasma glucose level of at least 200 mg per dL (11.1 mmol per L) during an oral glucose tolerance test, an A1C level of 6.5% or greater, or a random plasma glucose level of at least 200 mg per dL plus symptoms of polyuria, polydipsia, or unintentional weight loss11 (Table 22,6,11,12 ).
TABLE 2 Diagnostic Criteria for Type 2 Diabetes Mellitus

| A1C ≥ 6.5% |
| Fasting (more than eight hours) blood glucose ≥ 126 mg per dL (7.0 mmol per L) |
| Random plasma glucose ≥ 200 mg per dL (11.1 mmol per L) with signs or symptoms of type 2 diabetes (e.g., polyuria, polydipsia, unintentional weight loss) |
| Two-hour plasma glucose ≥ 200 mg per dL during oral glucose tolerance test using 1.75 g glucose per kg body weight (up to 75 g) |
Adapted with permission from American Diabetes Association. Type 2 diabetes in children and adolescents. Diabetes Care. 2000;23(3):382, with additional information from references 2, 6, and 11.
The validity of A1C in the diagnosis of type 2 diabetes in children has been questioned because of inaccuracies among certain ethnicities and comorbidities (e.g., sickle-cell trait).13 The American Diabetes Association continues to support the use of A1C levels for diagnosis, while acknowledging a lack of studies supporting its use in children with type 2 diabetes.6
Management
Management of type 2 diabetes should be focused on a multidisciplinary, family-centered, culturally appropriate approach.2 Primary care physicians should work closely with a team of subspecialists trained in the care of children and adolescents with type 2 diabetes if available, practical, and appropriate,2 especially if treatment goals are not met.2
NONPHARMACOLOGIC MANAGEMENT
Nutritional Counseling. Clinicians should focus on nutritional counseling for children with type 2 diabetes at the time of diagnosis and as a part of ongoing management.2 Clinicians should consider referral to a registered dietitian who has expertise in treating children with type 2 diabetes. Healthy eating patterns should be encouraged, with an emphasis on consuming nutrient-dense, high-quality foods and reducing calorie-dense, nutrient-poor foods.6,14 The target body mass index for children with type 2 diabetes is less than the 85th percentile for age and sex.6
Exercise Counseling. Exercise counseling should also be addressed at the time type 2 diabetes is diagnosed and as a part of ongoing management.2 Clinicians should encourage patients to engage in moderate to vigorous exercise for at least 60 minutes per day and to limit nonacademic screen time to less than two hours per day.2 Exercise can be completed in multiple shorter sessions. Clinicians should recognize the potential effects of exercise on the need for hypoglycemic medication and adjust the dosage accordingly, especially in patients receiving insulin.2,15
Family Involvement. Lifestyle changes are most successful when the patient's entire family is involved.2,16 Engaging family members also improves medication adherence.2 Because type 2 diabetes disproportionately affects minorities, clinicians should ensure that family-centered education is culturally appropriate.2 Children and adolescents should self-manage their diabetes to the extent appropriate for their age.17 The psychosocial effects of diabetes should be addressed to help children and adolescents cope with the disease.17
PHARMACOLOGIC MANAGEMENT
Metformin and insulin are the only medications for type 2 diabetes that are approved by the U.S. Food and Drug Administration for use in children and adolescents.18 Metformin in combination with diet and exercise is first-line therapy in children 10 years and older.2,19 Metformin should be initiated at a dosage of 500 mg per day, regardless of the patient's weight, then titrated in 500-mg intervals over four weeks to the maximum dosage of 2,000 mg per day.20
Although newly diagnosed type 2 diabetes may respond to metformin and lifestyle changes, insulin therapy must be initiated if the patient has signs of ketosis or ketoacidosis.2 Insulin is also recommended for patients without signs of ketosis or ketoacidosis who have random plasma glucose levels of 250 mg per dL (13.9 mmol per L) or greater, or whose A1C level is greater than 9%.2 Insulin may be beneficial for these patients on a short-term basis and can be discontinued after initiating metformin therapy and lifestyle changes.21
Monitoring Glycemic Control. The American Academy of Pediatrics recommends that clinicians monitor A1C levels every three months in children and adolescents with type 2 diabetes.2 The suggested target is less than 7%; however, this is supported only by expert opinion because no randomized controlled trials have established the relationship between glycemic control and the risk of microvascular complications in this population.2 Individualized goals are acceptable if an A1C target of less than 7% is unattainable.2 If glycemic control is not achieved, the treatment regimen should be intensified (e.g., more frequent clinic visits and blood glucose monitoring, modification or addition of medication, change in diet and exercise regimens).
Self-monitored blood glucose (finger-prick) testing should be performed at least three times per day in children who are on insulin therapy, whose dosage or treatment regimen is changing, who have comorbid illness, or who are not meeting goals for glycemic control.2
Comorbidities
Comorbidities such as hypertension, hyperlipidemia, nephropathy, and retinopathy may already be present at the time of diagnosis of type 2 diabetes in children and adolescents.6,22 Because the risk of diabetes-related complications is related to the duration of the disease, prompt diagnosis and appropriate therapy are important.11 At diagnosis and annually thereafter, a lipid panel and liver function tests should be ordered, and the patient should be evaluated for microalbuminuria, retinopathy, and sleep apnea.11,23 The American Diabetes Association also recommends routine blood pressure checks in children and adolescents with type 2 diabetes.6 The timeline for these and other screening recommendations is summarized in Table 3.2,6,11,17,24,25 Children and adolescents with high-normal blood pressure (systolic or diastolic blood pressure in 90th percentile or greater for age, sex, and height) or hypertension (95th percentile or greater) on three separate occasions should be treated.6 Patients with high-normal blood pressure should focus on dietary modification and increased exercise. Those with hypertension should be started on an angiotensin-converting enzyme inhibitor.6
TABLE 3 Schedule for Recommended Care of Children and Adolescents with Type 2 Diabetes Mellitus

| At diagnosis |
| Assess baseline A1C level, order lipid panel and liver function tests, and screen for retinopathy |
| Begin diabetes education for patient and family |
| Check blood pressure |
| Establish goals of care and treatment requirements |
| Evaluate for microalbuminuria and sleep apnea |
| Provide nutritional and exercise counseling |
| Once |
| Administer one dose of 23-valent pneumococcal polysaccharide vaccine (Pneumovax) at least eight weeks after previous dose of 13-valent pneumococcal conjugate vaccine (Prevnar 13) |
| Quarterly |
| Assess A1C level |
| Assess psychosocial adherence, self-management skills, dietary needs, and physical activity level |
| Check blood pressure |
| Review self-managed blood glucose records (when indicated) |
| Annually |
| Administer influenza vaccine |
| Evaluate for microalbuminuria and sleep apnea |
| Order lipid panel and liver function tests, and screen for retinopathy |
Further Study
There is only limited evidence for medical interventions in children and adolescents with type 2 diabetes. Future studies should explore whether lifestyle changes without pharmacotherapy are a reliable first step in treating selected children with type 2 diabetes. Although metformin and insulin are the only agents approved by the U.S. Food and Drug Administration for the management of type 2 diabetes in children, research studies are examining the use of thiazolidinediones and incretins in adolescents.24,25
This article updates a previous article on this topic by Peterson, et al.17
Data Sources: We searched Essential Evidence, the Cochrane database, the Agency for Healthcare Research and Quality evidence reports, Medline, PubMed, and the U.S. Preventive Services Task Force websites using the key words type 2 diabetes and children. Search dates: March 2017 and July 2018.

