
Am Fam Physician. 2018;98(9):607-608
Author disclosure: No relevant financial affiliations.
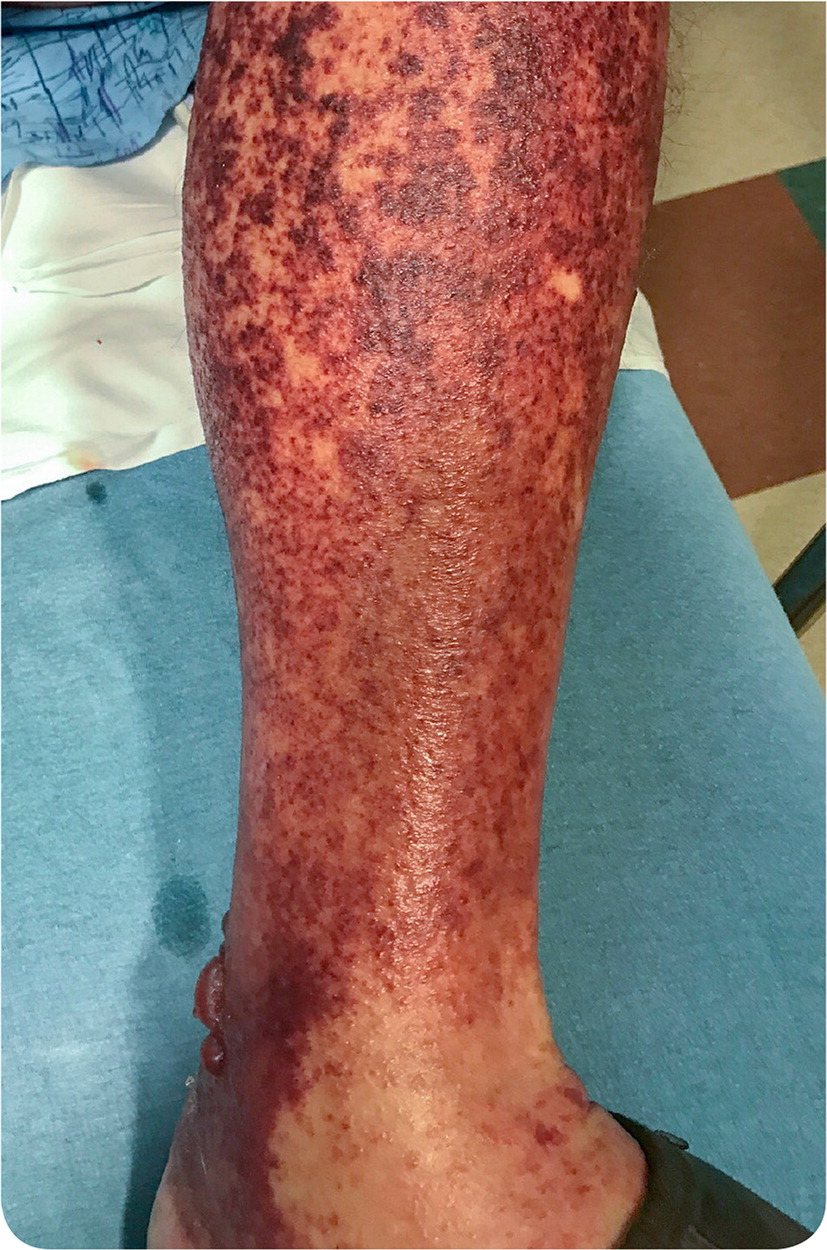
An 80-year-old man presented with a painful rash on both lower extremities. The rash developed six hours after the patient took naproxen for chronic knee pain, and it progressed in an ascending fashion. The patient had a history of atrial fibrillation, chronic obstructive pulmonary disease, hypertension, hyperlipidemia, and moderate osteoarthritis.
Physical examination revealed tender, nonblanching, nonpruritic purpura on the lower legs (Figure 1). Biopsy of the skin lesions showed neutrophilic infiltration of capillaries and venules, fibrin deposits, tissue necrosis, and extravasation of red blood cells.
Question
Discussion
The answer is A: cutaneous leukocytoclastic vasculitis. Leukocytoclastic vasculitis is a small vessel vasculitis that is also known as hypersensitivity angiitis, drug-induced vasculitis, and hypersensitivity vasculitis.1 It is characterized by leukocytoclasis, a process of neutrophil infiltration, degranulation, and subsequent cell death that leads to the release of inflammatory mediators and vascular damage.1 Leukocytoclastic vasculitis may cause only cutaneous symptoms or may involve other organ systems such as the joints, kidneys, and gastrointestinal tract. It occurs equally in men and women and at any age.1
The classic presentation of cutaneous leukocytoclastic vasculitis includes nonblanching, nonpruritic, palpable purpura and petechiae on the legs or areas with tight-fitting clothing.2 Less common clinical findings include urticarial plaques, vesicles, bullae, pustules, and livedo reticularis.2 Leukocytoclastic vasculitis can be caused by medications, foods, infections, collagen-vascular disorders, or malignancies, but it is often idiopathic.3 Medications most commonly associated with the condition include antibiotics, nonsteroidal anti-inflammatory drugs, diuretics, phenytoin (Dilantin), and allopurinol.4 Infections, such as β-hemolytic streptococci, hepatitis B and C, infectious endocarditis, and human immunodeficiency virus infection, are also associated with leukocytoclastic vasculitis.4
Evaluation should begin with an assessment for potential secondary causes. Suspicious cutaneous lesions should be biopsied within 48 hours of initial manifestation. Characteristic findings on biopsy are polymorphonuclear neutrophil infiltration, activation, degranulation, and leukocytoclasia within blood vessel walls, with resulting tissue damage, fibrinoid necrosis, and extravasation of red blood cells.5 Treatment varies based on the underlying cause. Cessation of an associated medication can lead to response within two weeks. Treatment of an underlying malignancy can also lead to resolution.
Immune thrombocytopenic purpura is a thrombocytopenia caused by autoantibodies against platelets. It usually occurs after an inciting event, such as an infection or disruption to the immune system.6 Some patients are asymptomatic, but most present with petechiae, purpura, or bleeding-related symptoms (e.g., epistaxis, severe hemorrhage).
The classic form of Kaposi sarcoma is a low-grade vascular neoplasm that occurs most often in older men. It may mimic the purpuric lesions of cutaneous leukocytoclastic vasculitis, but it can also appear as violaceous macules, papules, plaques, or nodules on the lower extremities, head, neck, and oral mucosa.7 The nodular lesions may ulcerate and bleed.
Schamberg disease, the most common type of pigmented purpuric dermatosis, presents as nonblanching, reddish-brown purpuric patches consisting of clusters of nonpalpable, pinpoint petechiae, usually on the lower extremities and buttocks. There are many potential risk factors for this disease, including venous hypertension, infection, systemic disease, alcohol use, medication use, and exposure to chemicals or allergens.8
Scurvy presents as hemorrhagic skin lesions that are initially flat and then coalesce into palpable purpura on the lower extremities. Patients with scurvy have a history of severe malnourishment and other symptoms such as follicular hyperkeratosis, perifollicular purpura, corkscrew-shaped body hair, impaired wound healing, and bleeding gums.9
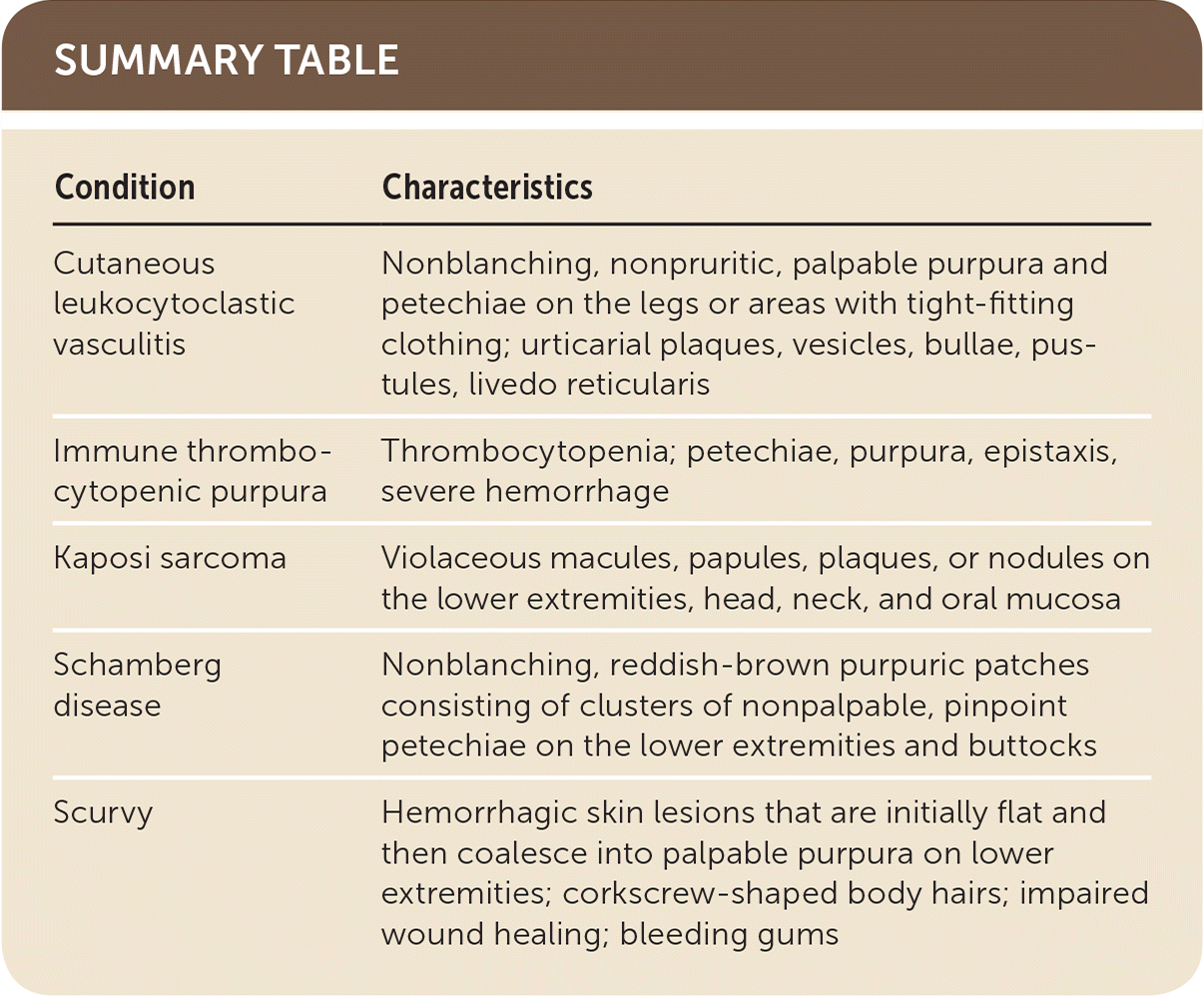
| Condition | Characteristics |
|---|---|
| Cutaneous leukocytoclastic vasculitis | Nonblanching, nonpruritic, palpable purpura and petechiae on the legs or areas with tight-fitting clothing; urticarial plaques, vesicles, bullae, pustules, livedo reticularis |
| Immune thrombocytopenic purpura | Thrombocytopenia; petechiae, purpura, epistaxis, severe hemorrhage |
| Kaposi sarcoma | Violaceous macules, papules, plaques, or nodules on the lower extremities, head, neck, and oral mucosa |
| Schamberg disease | Nonblanching, reddish-brown purpuric patches consisting of clusters of nonpalpable, pinpoint petechiae on the lower extremities and buttocks |
| Scurvy | Hemorrhagic skin lesions that are initially flat and then coalesce into palpable purpura on lower extremities; corkscrew-shaped body hairs; impaired wound healing; bleeding gums |
