Manipulative therapies include osteopathic manipulative treatment and many other forms of manual therapies used to manage a variety of conditions in adults and children. Spinal manipulative therapy may provide short-term improvement in patients with acute or chronic low back pain, comparable with other standard treatments. When compared with oral analgesics, cervical manipulation and/or mobilization appears to provide better short-term pain relief and improved function in patients with neck pain. Manipulative therapies may be as effective as amitriptyline for treating migraine headaches and can reduce the frequency and intensity of pain. Although manipulative therapy is sometimes recommended to treat conditions in children (e.g., musculoskeletal problems, otitis media, respiratory conditions, infantile colic, allergies), there is supporting evidence only for reducing the length of hospital stay for preterm infants. Mild adverse events, such as muscle stiffness and soreness, occur in up to 50% of adults who undergo manipulative therapy. Although serious adverse events such as lumbar disk herniation, cauda equina syndrome, and vertebrobasilar injury are rare, they can cause significant disability or death. Given the limited proven benefits of manipulative therapies and small risk of serious adverse events, additional high-quality, adequately powered studies are needed before definitive recommendations can be made for treating many conditions.
Nearly one-third of the U.S. population uses some form of complementary and alternative medicine (CAM) in a given year.1 Osteopathic health care is used by nearly 16% of the U.S. population at some point in their lifetime.2 This article reviews the evidence on manipulative therapies including osteopathic manipulative treatment (OMT) for certain common medical conditions and the risks of adverse events related to its use.
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Spinal manipulative therapy may be considered for patients with acute low back pain to provide modest improvement in pain and function at up to six weeks, comparable with other therapies. | B | 8–10 |
| Spinal manipulative therapy may be considered for patients with chronic low back pain. It results in modest improvement in pain and function for up to six months and is comparable with other therapies. | B | 11–13 |
| Cervical manipulation and mobilization may be considered to provide short-term improvement in pain relief and function in patients with neck pain. | B | 14–16 |
| Manipulative therapies are not recommended for treatment of childhood conditions such as acute otitis media, respiratory conditions, colic, or allergies. | B | 5, 6, 20, 21 |
| Mild adverse events of manipulative therapies are common. Serious adverse events are rare but can include vertebrobasilar injuries, lumbar disk herniations, cauda equina syndrome, and death. | B | 6, 22–24 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
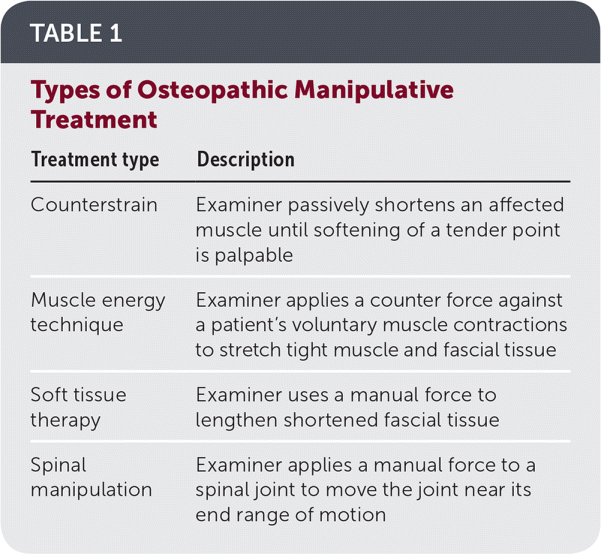
The American Osteopathic Association defines OMT as the therapeutic application of manually guided interventions by a clinician to improve physiologic function or to support homeostasis that has been altered by somatic dysfunction.3 Types of OMT are summarized in Table 1. The rationale for osteopathic manipulation is based on the theory that the structure and function of the body are closely related and that somatic dysfunction occurs when the neurologic, musculoskeletal, circulatory, and visceral structures are not working together properly.4 OMT encompasses a variety of manipulative techniques that include, but are not limited to, muscle energy technique, soft tissue therapy, counterstrain, and spinal manipulation, with the goal of restoring the body back to its natural balance.1,5 Osteopathic physicians, physical therapists, massage therapists, naturopathic physicians, and chiropractors all may perform types of manual therapies in their practice.6 Studies evaluating these therapies can be difficult to evaluate because of variability in technique, frequency of treatment, and overall treatment characteristics. Online resources specifically on manipulative therapies are listed in Table 2.
TABLE 1. Types of Osteopathic Manipulative Treatment
| Treatment type | Description |
|---|---|
| Counterstrain | Examiner passively shortens an affected muscle until softening of a tender point is palpable |
| Muscle energy technique | Examiner applies a counter force against a patient's voluntary muscle contractions to stretch tight muscle and fascial tissue |
| Soft tissue therapy | Examiner uses a manual force to lengthen shortened fascial tissue |
| Spinal manipulation | Examiner applies a manual force to a spinal joint to move the joint near its end range of motion |
TABLE 2. Resources for Information on Manipulative Therapies
| American Academy of Family Physicians |
| American College of Osteopathic Family Physicians |
| American Osteopathic Association |
Low Back Pain
Low back pain is one of the most common reasons patients seek treatment with CAM therapies, specifically manipulative therapy.1,7 Spinal manipulation is the manipulative technique used most often for back pain in the United States.7
ACUTE BACK PAIN
Treatment of acute low back pain includes multiple different modalities (e.g., oral analgesics, exercises, heat, ice, manipulative therapy), and there is little evidence that one modality is superior to another.8 Multiple systematic reviews on spinal manipulation have been performed with varying conclusions.8 A 2003 meta-analysis of 39 randomized controlled trials (RCTs) with 5,486 patients found that spinal manipulation had clinically and statistically significant benefits (10-mm difference on a 100-mm visual analog scale; 95% confidence interval [CI], 2 to 17 mm) when compared with sham manipulation, but no benefit when compared with other common treatments for acute low back pain, including analgesics, physical therapy, exercise, or back school.9
A 2012 systematic review examined 20 RCTs with 2,674 total patients and found that spinal manipulation was no more effective for the treatment of acute low back pain than sham manipulation, standard medical therapy, or as an adjunct to another intervention.10 A 2017 meta-analysis of 26 RCTs compared spinal manipulative therapy (SMT) with physical therapy, exercises, and sham therapy for the treatment of acute low back pain. It concluded that for patients with acute low back pain, SMT led to significant improvements in pain (improvement of 10 mm on a 100-mm visual analog scale; 95% CI, –15.6 to –4.3 mm) and short-term function (effect size = –0.39; 95% CI, –0.71 to –0.07) at up to six weeks.8 Overall, spinal manipulation does not confer a definitive benefit over standard medical treatment for acute low back pain, but it is better than sham therapy and is a reasonable treatment option. Costs, safety, and patient preferences should be weighed when considering manipulative therapies vs. alternative treatments.
CHRONIC BACK PAIN
Chronic low back pain is typically described as low back pain lasting at least 12 weeks and is often associated with physical disabilities and psychological symptoms.11 A 2004 Cochrane review analyzed 39 RCTs of 5,486 patients with low back pain who were treated with spinal manipulation. For patients with chronic low back pain, spinal manipulation was superior to sham therapy with a clinically and statistically significant improvement up to six months (19-mm improvement on a 100-mm visual analog scale [95% CI, 3 to 35 mm]), but it was not more beneficial than standard treatment with oral analgesics, exercises, or physical therapy.12 A more recent meta-analysis examined 26 RCTs that included 6,070 patients with chronic low back pain. It found that patients treated with spinal manipulation had no clinically significant short-term improvements in pain (4 mm on a 100-mm scale; 95% CI, –7.0 to –1.4 mm) or function (standardized mean difference [SMD] = –0.22; 95% CI, –0.36 to –0.07) when compared with other treatments such as physical therapy, exercises, massage, or ultrasound therapy.13 As in acute low back pain, spinal manipulation may be considered for the treatment of chronic low back pain after costs, safety, and patient preferences are discussed.
Neck Pain
Manual therapies are commonly chosen to manage neck pain.14 A 2004 systematic review of 33 RCTs examined the effect of manipulation and/or mobilization in conjunction with other standard treatments in adults with mechanical neck pain.15 It found that manipulation and/or mobilization plus exercise provided clinically and statistically significant improvements in pain (SMD = –0.85; 95% CI, –1.20 to –0.50) and function (SMD = –0.57; 95% CI, –0.94 to –0.21) in patients with subacute or chronic mechanical neck pain when compared with no treatment. However, manipulation and/or mobilization alone or in combination with treatments other than exercise was not effective.15
A 2010 systematic review of 27 RCTs compared cervical manipulation or cervical mobilization with sham therapy or no treatment in 1,522 patients with subacute or chronic neck pain.16 It concluded that cervical manipulation (SMD = –0.90; 95% CI, –1.78 to –0.02) and cervical mobilization produced similar, clinically significant improvements in short-term pain relief in patients with subacute or chronic neck pain.16
More recently, a Cochrane review of 51 RCTs with a total of 2,920 patients examined the effects of manipulation and mobilization on patients with neck pain. In patients with acute or subacute neck pain, cervical manipulation produced better pain relief immediately after treatment (SMD = –0.34; 95% CI, –0.64 to –0.05) and at long-term follow-up (SMD = –0.32; 95% CI, –0.61 to –0.02) compared with standard oral analgesics.14 Cervical mobilization had similar improvements in pain relief when compared with cervical manipulation at short- and intermediate-term follow-up in patients with acute or chronic neck pain.14 The risk of serious adverse events associated with cervical manipulation should be considered when deciding whether manual therapies should be used to treat neck pain.
Headache
Multiple different types of manipulative therapies are used in the prevention and treatment of headaches.17,18 A 2004 systematic review of 22 RCTs with 2,628 patients evaluated the effect of noninvasive physical therapies that are used in the treatment of common types of headache.19 It concluded that spinal manipulation had similar, modest short-term effects to amitriptyline for the prophylactic treatment of migraine headache. However, it is less effective than amitriptyline for the prophylaxis of chronic tension-type headaches. The same review concluded that SMT is effective for the prophylaxis of cervicogenic headache with a reduction in the pain intensity at one week (SMD = 0.7; 95% CI, 0.3 to 1.2) and modestly lower pain intensity in the long term (SMD = 0.4; 95% CI, 0.0 to 0.8).19
A 2017 systematic review of five RCTs with 265 patients concluded that OMT, when compared with other treatments such as usual care, sham therapy, or muscle relaxation techniques, may reduce the frequency and intensity of pain as well as disability associated with headaches.18 However, it is important to note that the conclusions from these systematic reviews are limited by the small number of quality reviews, low number of patients studied, and high risk of bias. More study is needed before manipulative therapies can be confidently recommended to prevent and treat headaches.
Manipulative Therapies in Infants and Children
In the United States, manipulative therapies have been recommended for many conditions in children and infants, including musculoskeletal problems, otitis media, respiratory conditions, infantile colic, and allergies. It is estimated that almost 2.3 million children in the United States used OMT or chiropractic manipulation in 2007.5 In addition, chiropractic care is the most common CAM therapy used by children in the United States.6 In 2012, a meta-analysis of six RCTs with a total of 325 infants treated with manipulative therapies for infantile colic could not reach any definitive conclusions about treatment effectiveness compared with no treatment.20 Another systematic review of 17 RCTs evaluated the effectiveness of OMT for multiple childhood conditions such as cerebral palsy, respiratory conditions (bronchiolitis and asthma), otitis media, musculoskeletal function, attention-deficit/hyperactivity disorder, infantile colic, congenital nasolacrimal duct obstruction, and dysfunctional voiding, as well as length of hospital stay in premature infants.5 Investigators concluded that OMT should not be recommended for infants and children based on the low quality of supporting evidence. Finally, a systematic review of five RCTs with 1,306 patients compared the length of hospital stay for preterm infants who received manipulative therapies with those who received sham or no treatment. It found that infants who were treated with manipulative therapies had a length of stay three days shorter than those who were not treated with manipulative therapies.21
Overall, it is difficult to make any recommendations about the use of manipulative therapies in infants and children because most studies had a high potential for bias with small numbers of patients and low methodologic quality.
Adverse Events
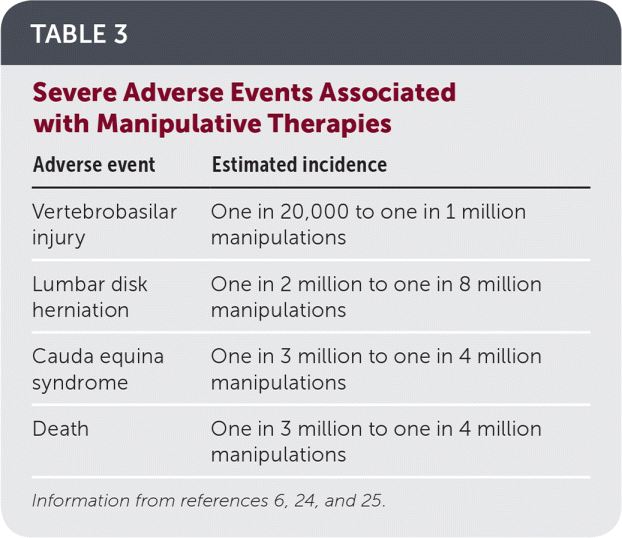
When considering manipulative therapies for the management of medical conditions, it is important to consider the possibility of adverse events and ensure that the patient is informed of any risks. Minor adverse events (e.g., muscle stiffness and soreness, increased pain, fatigue, weakness) are commonly reported and occur in up to 50% of adults undergoing manipulative therapies.6,22,23 Serious adverse events associated with manipulative therapies are typically defined as conditions that lead to hospital admission or death, but these are rare.24 Two recent systematic reviews have identified rare serious adverse events associated with SMT including cauda equina syndrome, lumbar disk herniation, fractures, hematoma, stroke, vertebrobasilar accident, cerebrovascular accident, and death.23,24 In children, serious adverse events resulting in hospitalization, permanent disability, or death due to spinal manipulation have rarely been reported in case series.6 Although the incidence of serious adverse events associated with manipulative therapies is thought to be extremely low, the true risk is difficult to estimate because such events are likely underreported.6,23,24 Recent estimates of the incidence of serious adverse events range from one in 20,000 manipulations to one in 250,000,000 manipulations24 (Table 36,24,25 ).
TABLE 3. Severe Adverse Events Associated with Manipulative Therapies
| Adverse event | Estimated incidence |
|---|---|
| Vertebrobasilar injury | One in 20,000 to one in 1 million manipulations |
| Lumbar disk herniation | One in 2 million to one in 8 million manipulations |
| Cauda equina syndrome | One in 3 million to one in 4 million manipulations |
| Death | One in 3 million to one in 4 million manipulations |
Editor's Note: Visual analog scale: A visual analog scale asks participants to rate pain or some other subjective outcome on a scale, typically ranging from 0 to 100 points, where 0 is no pain and 100 is the worst possible pain imaginable. A difference of at least 10 points is the smallest change that is clinically noticeable or significant. Smaller differences may be statistically significant but are unlikely to be noticeable by patients.1 Standardized mean difference (SMD): Also known as Cohen's d, the SMD is used to combine the results from studies using scales that have different lengths or sizes but are attempting to measure the same underlying parameter. For example, the 30-point Mini-Mental State Examination score and the 72-point Alzheimer's Disease Assessment Scale–cog score are both measures of the severity of cognitive impairment. The SMD is calculated as the difference in the mean outcome between groups divided by the standard deviation. In general, an SMD less than 0.2 is not clinically significant, an SMD of 0.2 represents a small clinical effect, an SMD of 0.5 is a moderate effect, and an SMD of 0.8 or greater is a large effect.2 For more evidence-based medicine definitions, see the AFP EBM Glossary at https://www.aafp.org/journals/afp/authors/ebm-toolkit/glossary.html.—Mark H. Ebell, MD, MS, Deputy Editor for Evidence-Based Medicine
1. Kelly AM. The minimum clinically significant difference in visual analogue scale pain score does not differ with severity of pain. Emerg Med J. 2001;18(3):205–207.
2. Cohen J. Statistical Power Analysis for the Behavioral Sciences. 2nd ed. Hillsdale, N.J.: Lawrence Erlbaum Associates; 1988.
Data Sources: A PubMed search was performed using the following terms: manipulative treatment, manipulation, osteopathic therapy, osteopathic manipulation, OMT, spinal manipulation, spinal manipulative therapy, adverse events of manipulation, risks of manipulation, manipulation for low back pain, manipulation for neck pain, complementary/alternative medicine. The search included meta-analyses, randomized controlled trials, and reviews. We reviewed Essential Evidence Plus, the Cochrane database, and National Institute for Health and Care Excellence guidelines. Search dates: December 16, 2016, to May 15, 2018.

