In 2018, through regular surveillance of more than 110 English-language research journals, 255 research studies met the criteria to become POEMs (patient-oriented evidence that matters). Using a validated tool, physician members of the Canadian Medical Association rated these POEMs for their relevance to patients in their practices. This article summarizes the clinical questions and bottom-line answers from the top 20 POEMs of 2018, as determined by these physicians. The top POEMs summarize potentially practice-changing research on the importance of accurate blood pressure measurement, the unclear benefits of lower blood pressure targets for hypertension, the lack of evidence regarding treatment of cough, advantages of shorter over longer courses of antibiotics for several common infections, the value of increased fluid intake for preventing recurrent urinary tract infections, and the benefit of nitrofurantoin over fosfomycin for the treatment of urinary tract infection. Other conclusions include the lack of benefit of anticonvulsants for low back pain, the value of nonopioid pain management compared with opioids, the risk of anxiety recurrence when an antidepressant is discontinued, the value of exercise for reducing the risk of depression, and the increased risk of fractures with the use of Z-drug hypnotics. Regarding clinical preventive services, adherence is better with fecal immunochemical tests than with older guaiac-based fecal occult blood tests for colon cancer screening; statins showed no benefit for patients 75 years or older; aspirin showed no benefit for cardiovascular disease prevention; and exercise, vision assessment, and environmental assessments may reduce the risk of falls. Finally, we identify the top POEMs summarizing clinical practice guidelines from the American College of Physicians, American College of Cardiology/American Heart Association, and the U.S. Preventive Services Task Force.
Annually, a group of experts in evidence-based medicine systematically review more than 110 English-language research journals to identify the evidence most likely to change primary care practice. The group includes physicians in the fields of family medicine, pharmacology, hospital medicine, and women’s health.1,2
The goal of this process is to identify POEMs (patient-oriented evidence that matters). A POEM must report patient-oriented outcomes, such as improvement in symptoms, morbidity, or mortality; be free of important methodologic bias; and recommend a change in practice for many physicians. Adopting valid POEMs in clinical practice could therefore result in improved patient outcomes. Of more than 20,000 research studies published in 2018 in the journals reviewed, 255 met the criteria for validity, relevance, and practice change.
The Canadian Medical Association (CMA) provides a subscription to POEMs for all of its members, who have the option to receive the daily POEM by e-mail. When members read the POEM, they can rate it with a validated tool called the Information Assessment Method. This tool addresses the domains of clinical relevance, cognitive impact, use in practice, and expected health benefits if that POEM was applied in patient care.3,4 Each POEM was rated by an average of 1,574 physicians.
In this article, we present the 20 POEMs that were rated highest for clinical relevance by CMA members in 2018. In this installment of our annual series (https://www.aafp.org/afp/toppoems), we summarize the clinical question and bottom-line answer for each research study identified as a top 20 POEM, organized by topic and followed by a brief discussion. We also present the five most relevant practice guidelines.
Hypertension
Our first group of POEMs focuses on hypertension (Table 1).5–9 Blood pressure measurement is a routine part of the physical examination in the office setting. Yet, POEM 1 shows that ambulatory blood pressure is considerably lower on average than office-based blood pressure, and that blood pressure readings from an ambulatory blood pressure device are more predictive of all-cause mortality than office-based blood pressure readings.5 Mortality is likely the outcome that matters most for patients.
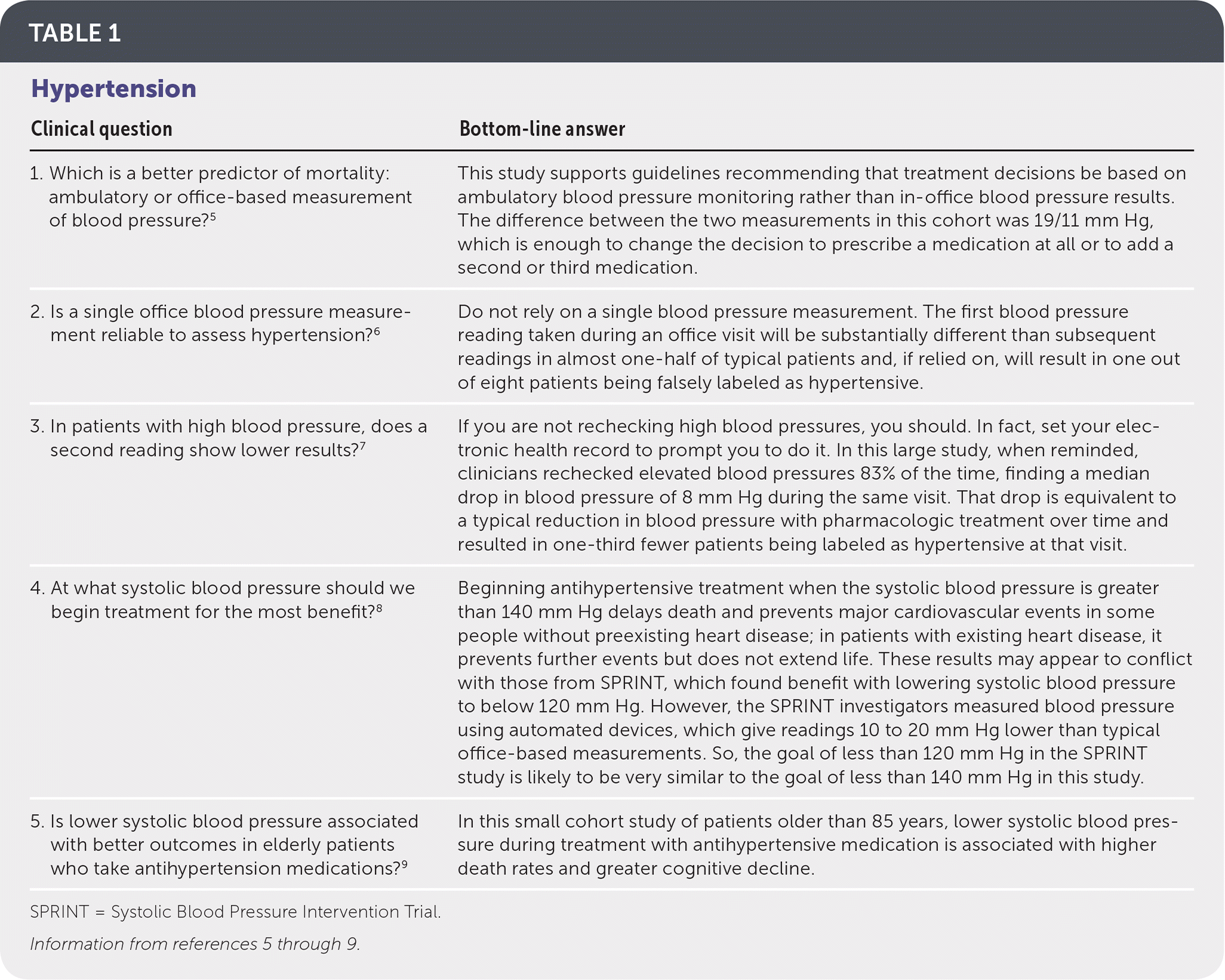
TABLE 1. Hypertension
| Clinical question | Bottom-line answer |
|---|---|
| 1. Which is a better predictor of mortality: ambulatory or office-based measurement of blood pressure?5 | This study supports guidelines recommending that treatment decisions be based on ambulatory blood pressure monitoring rather than in-office blood pressure results. The difference between the two measurements in this cohort was 19/11 mm Hg, which is enough to change the decision to prescribe a medication at all or to add a second or third medication. |
| 2. Is a single office blood pressure measurement reliable to assess hypertension?6 | Do not rely on a single blood pressure measurement. The first blood pressure reading taken during an office visit will be substantially different than subsequent readings in almost one-half of typical patients and, if relied on, will result in one out of eight patients being falsely labeled as hypertensive. |
| 3. In patients with high blood pressure, does a second reading show lower results?7 | If you are not rechecking high blood pressures, you should. In fact, set your electronic health record to prompt you to do it. In this large study, when reminded, clinicians rechecked elevated blood pressures 83% of the time, finding a median drop in blood pressure of 8 mm Hg during the same visit. That drop is equivalent to a typical reduction in blood pressure with pharmacologic treatment over time and resulted in one-third fewer patients being labeled as hypertensive at that visit. |
| 4. At what systolic blood pressure should we begin treatment for the most benefit?8 | Beginning antihypertensive treatment when the systolic blood pressure is greater than 140 mm Hg delays death and prevents major cardiovascular events in some people without preexisting heart disease; in patients with existing heart disease, it prevents further events but does not extend life. These results may appear to conflict with those from SPRINT, which found benefit with lowering systolic blood pressure to below 120 mm Hg. However, the SPRINT investigators measured blood pressure using automated devices, which give readings 10 to 20 mm Hg lower than typical office-based measurements. So, the goal of less than 120 mm Hg in the SPRINT study is likely to be very similar to the goal of less than 140 mm Hg in this study. |
| 5. Is lower systolic blood pressure associated with better outcomes in elderly patients who take antihypertension medications?9 | In this small cohort study of patients older than 85 years, lower systolic blood pressure during treatment with antihypertensive medication is associated with higher death rates and greater cognitive decline. |
SPRINT = Systolic Blood Pressure Intervention Trial.
POEMs 2 and 3 remind us of the pitfalls of measuring office blood pressure. A cross-sectional study found that a single manual blood pressure measurement often yields falsely elevated results.6 POEM 3 summarizes an American study of a large cohort with a mean age of 61 years. In this study, electronic reminders were used to prompt clinicians to recheck blood pressure in patients with a high initial reading.7 On recheck, the median drop in blood pressure was 8 mm Hg, and 36% of patients no longer had a blood pressure of 140/90 mm Hg or higher. The findings of these POEMs should give us pause. Changing from office to ambulatory blood pressure monitoring in older people would seem to be the right thing to do, but practical ways of implementing the use of these ambulatory monitors in the outpatient setting are needed.
Family medicine strives to be patient-centered, not target-centered. Yet, even a patient-centered discipline must consider numerical thresholds and “treat to target” recommendations in managing hypertension. In one of our previous articles in this series, a top POEM of 2012 summarized a Cochrane review of four primary studies. This Cochrane review found no benefit to the pharmacologic treatment of mild hypertension (defined as blood pressure of 140/90 mm Hg to 159/99 mm Hg) in people without cardiovascular disease (CVD).10
POEM 4 asks at what systolic blood pressure should we recommend initiating treatment? The pooling of data from 74 studies of 306,000 patients (average age 64 years) showed that lowering systolic blood pressure that was initially greater than 140 mm Hg delays death and prevents major cardiovascular events in some people without preexisting heart disease. But, treating systolic blood pressure that was initially less than 140 mm Hg did not affect morbidity or mortality.8 Thus, from a much larger body of research, a small benefit of treating stage 1 hypertension emerged, effectively overturning the finding from the 2012 Cochrane review but contradicting the recent American College of Cardiology/American Heart Association guidelines that recommend a lower blood pressure target of 130/80 mm Hg for most patients.11
When is blood pressure too low in older patients? POEM 5, a Dutch cohort study of 570 people 85 years or older, addressed this question.9 During a five-year follow-up period, 46% of this cohort died. Lower systolic blood pressure during treatment with antihypertensive medication was associated with higher death rates and greater cognitive decline. Although a more aggressive systolic blood pressure target of 120 mm Hg in SPRINT (Systolic Blood Pressure Intervention Trial) led to a small benefit, SPRINT enrolled much younger patients with a mean age of 68 years and measured blood pressure using an automated method.12
Infection
Our next group of POEMs focuses on infections (Table 2).13–17 How long do we have to treat common infections? A body of literature has been building for two decades that convincingly argues for shorter courses of antibiotic therapy in most cases. Advantages include lower cost, fewer adverse effects, and a lower risk of resistance developing in the community.
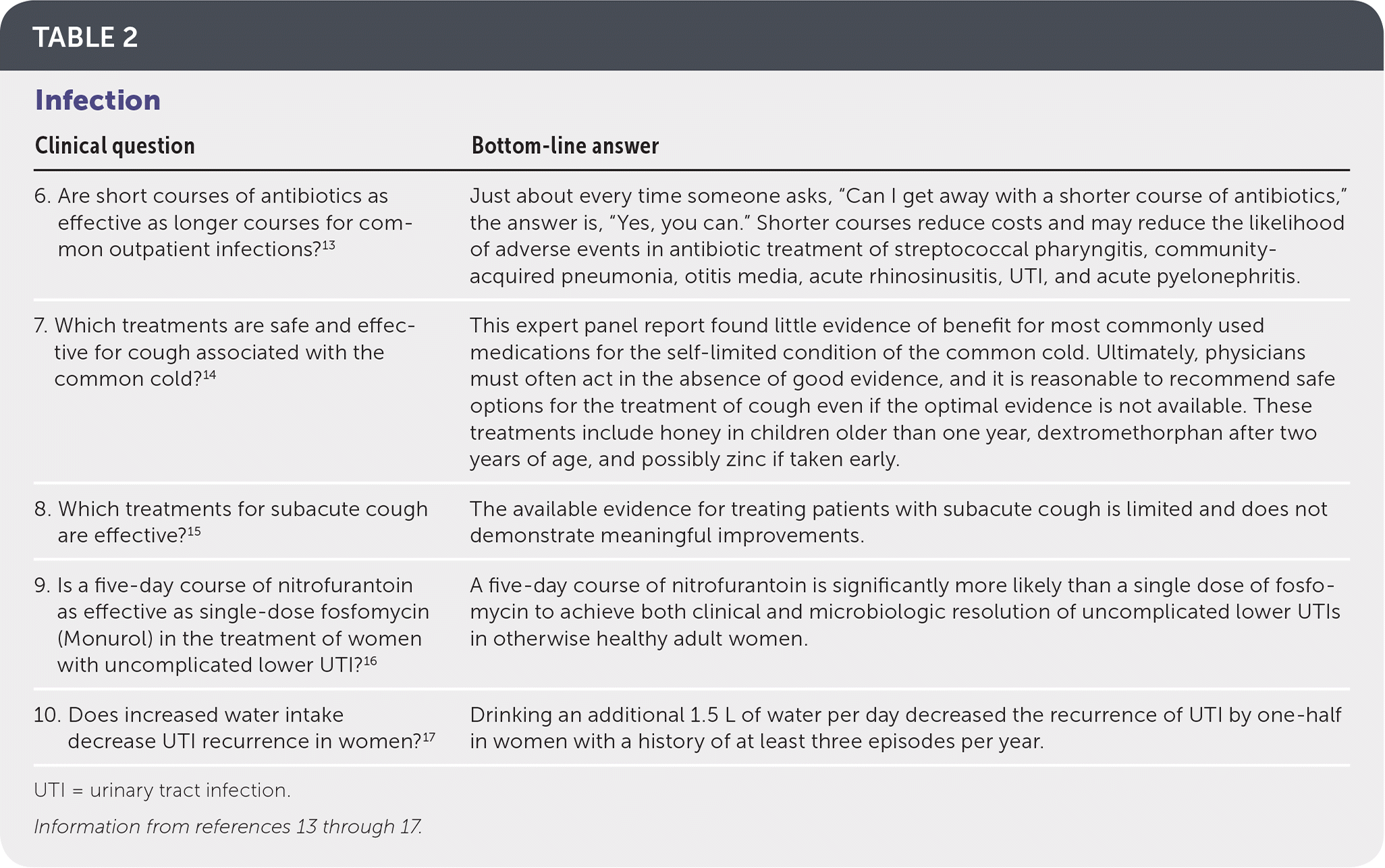
TABLE 2. Infection
| Clinical question | Bottom-line answer |
|---|---|
| 6. Are short courses of antibiotics as effective as longer courses for common outpatient infections?13 | Just about every time someone asks, “Can I get away with a shorter course of antibiotics,” the answer is, “Yes, you can.” Shorter courses reduce costs and may reduce the likelihood of adverse events in antibiotic treatment of streptococcal pharyngitis, community-acquired pneumonia, otitis media, acute rhinosinusitis, UTI, and acute pyelonephritis. |
| 7. Which treatments are safe and effective for cough associated with the common cold?14 | This expert panel report found little evidence of benefit for most commonly used medications for the self-limited condition of the common cold. Ultimately, physicians must often act in the absence of good evidence, and it is reasonable to recommend safe options for the treatment of cough even if the optimal evidence is not available. These treatments include honey in children older than one year, dextromethorphan after two years of age, and possibly zinc if taken early. |
| 8. Which treatments for subacute cough are effective?15 | The available evidence for treating patients with subacute cough is limited and does not demonstrate meaningful improvements. |
| 9. Is a five-day course of nitrofurantoin as effective as single-dose fosfomycin (Monurol) in the treatment of women with uncomplicated lower UTI?16 | A five-day course of nitrofurantoin is significantly more likely than a single dose of fosfomycin to achieve both clinical and microbiologic resolution of uncomplicated lower UTIs in otherwise healthy adult women. |
| 10. Does increased water intake decrease UTI recurrence in women?17 | Drinking an additional 1.5 L of water per day decreased the recurrence of UTI by one-half in women with a history of at least three episodes per year. |
UTI = urinary tract infection.
POEM 6, a systematic review, found that a shorter course of therapy is as effective as longer courses for children with streptococcal pharyngitis (five to seven days is as good as 10 days), community-acquired pneumonia (three days is as good as five days), otitis media (two or more days is as good as seven or more days), or urinary tract infection (UTI; two to four days is as good as seven to 14 days); for adults with acute rhinosinusitis (three to seven days is as good as six to 10 days), uncomplicated UTI (three days is as good as five or more days), acute pyelonephritis (seven to 14 days is as good as 14 to 42 days), or community-acquired pneumonia (seven or fewer days is as good as more than seven days); and for older women with UTI (three to six days is as good as seven to 14 days).13
According to POEMs 7 and 8, there is not much evidence regarding treatment of acute or subacute cough.14,15 Although absence of evidence is not evidence of absence, it is a call for research into how to help patients with cough. Effective therapies for acute cough include honey in children older than one year, dextromethorphan after two years of age, and possibly zinc if taken early.
POEMs 9 and 10 address prevention and treatment of UTI. The first, which compared five days of nitrofurantoin, 100 mg three times daily, with a single 3-g dose of fosfomycin (Monurol), found that nitrofurantoin was more effective in terms of clinical resolution (70% vs. 58%; number needed to treat = 8; 95% CI, 5 to 26).16 Nitrofurantoin is also less expensive than fosfomycin ($10 vs. $95).18
Although physicians have long recommended increased fluid intake to prevent recurrent UTIs, this recommendation is solidified with POEM 10.17 In this study, 140 premenopausal women who had experienced at least three UTIs in the previous year were randomized to an additional 1.5 L of bottled water per day or usual care. Those with increased fluid intake had only 1.7 UTIs in the next year, compared with 3.2 UTIs in the usual care group (P < .001).17
Pain Management
Three POEMs address the management of pain (Table 3).19–22 POEM 11 identified 240 patients with chronic back, hip, or knee pain that was rated at least moderately severe and had been present for at least six months.19 These patients were randomized to an opioid-based, stepped therapy beginning with oral opioids and advancing as needed to sustained-release oral opioids and, if needed, transdermal fentanyl, with a maximum daily dosage of 100 morphine equivalents. The nonopioid group started with acetaminophen and nonsteroidal anti-inflammatory drugs, advancing as needed to amitriptyline or gabapentin (Neurontin) as an adjuvant and finally to tramadol (only 11% required the latter). After 12 months, there was no difference between groups in function, and pain intensity was lower in the nonopioid group. There were more dropouts because of medication adverse effects in the opioid group (19% vs. 8%).
TABLE 3. Pain Management

| Clinical question | Bottom-line answer |
|---|---|
| 11. Are opioid medications preferable for improving pain-related function in adults with severe chronic back, hip, or knee pain?19 | Nonopioid medications were at least as effective as opioid medications for improving pain-related function over 12 months in adults with severe chronic back pain or hip or knee osteoarthritis pain. The evidence that opioids are not superior to nonopioid medications for both chronic and acute pain continues to mount. The tough job will be getting patients and clinicians to believe the evidence. |
| 12. What oral analgesic combinations are effective for reducing the pain of an acute extremity injury in adults in the emergency department?20 | In adults with pain severe enough to warrant radiologic investigation, ibuprofen plus acetaminophen was equally effective in reducing pain intensity at two hours compared with three different opioid and acetaminophen combination analgesics. In a similar study, naproxen alone was as effective as naproxen plus oxycodone/acetaminophen or naproxen plus cyclobenzaprine for reducing pain from acute musculoskeletal low back pain.21 It is time to stop believing that opioids are superior to nonsteroidal anti-inflammatory drugs for acute pain control. |
| 13. Are anticonvulsants an effective treatment for low back pain?22 | The use of anticonvulsants, such as gabapentin (Neurontin), for painful conditions has increased greatly in recent years. However, this systematic review found good evidence that these drugs are not effective for the treatment of low back pain, with or without radiculopathy, and are associated with an increased risk of adverse events. |
POEM 12 compared ibuprofen, 400 mg, plus acetaminophen, 1,000 mg, with three opioid regimens (oxycodone, 5 mg; hydrocodone, 5 mg; or codeine, 30 mg, each combined with acetaminophen, 300 mg) for reducing the pain of an acute extremity injury. There were no significant differences among the groups, with all four regimens reducing pain by about the same amount (3.5 to 4.4 points on a 10-point scale).20 Finally, although anticonvulsants are widely used for painful conditions, POEM 13 (a systematic review) found little evidence to support the effectiveness of anticonvulsants for low back or lumbar radicular pain. Of 14 comparisons in nine randomized trials, only two small studies found a clinically important and statistically significant benefit.22
Behavioral Medicine
Our fourth set of POEMs focuses on behavioral medicine (Table 4).23–25 A meta-analysis has given us yet another reason to recommend exercise to patients of all ages. POEM 14 included 49 prospective cohort studies with more than 1.8 million person-years of follow-up among patients who did not have depression at baseline. These patients were followed for a mean of 7.4 years to determine the incidence of depression. The meta-analysis found a consistent association between more physical activity and a lower risk of depression (adjusted odds ratio = 0.83; 95% CI, 0.79 to 0.88).23
TABLE 4. Behavioral Medicine

| Clinical question | Bottom-line answer |
|---|---|
| 14. Is physical activity at baseline associated with a reduced risk of subsequent incident depression?23 | People with a high level of physical activity (more than 150 minutes of at least moderate-intensity activity per week) were less likely to have subsequent incident depression than those who had a low level of physical activity. Given the large size of the population, the prospective nature of the studies, and the consistency across age groups, the suggestion that exercise is a preventive factor for new-onset depression is relatively strong. This is further evidence that exercise is medicine. |
| 15. How common is relapse in patients with anxiety disorder following the discontinuation of treatment with an antidepressant?24 | About one-third of patients will have a relapse after discontinuation of antidepressant therapy. One in six patients treated successfully will also relapse despite continued treatment. |
| 16. Are nonbenzodiazepine hypnotics associated with harms in older adults?25 | Among 14 observational studies, the use of so-called Z-drugs was associated with higher risk of fracture (hazard ratio = 1.6; 95% CI, 1.4 to 1.9). |
In patients treated with an antidepressant for an anxiety disorder (e.g., panic disorder, generalized anxiety disorder, posttraumatic stress disorder, a phobia), what is the likelihood of relapse when the medication is discontinued? POEM 15 is a systematic review that identified 28 studies with 5,233 patients. These patients were randomized to continued therapy or placebo and were followed for two to 12 months. The relapse rate was 36% in the placebo group, compared with 16% in the continued therapy group (number needed to harm = 5). However, thinking of it a different way, 64% who were taken off of an antidepressant did not relapse.24
Family physicians know to avoid using benzodiazepines to treat insomnia because of the well-documented increase in the risk of falls. POEM 16 asked whether the so-called Z-drugs (zolpidem [Ambien], zopiclone [not available in the United States], eszopiclone [Lunesta], and zaleplon) also increase the risk of falls and fractures. They did, but only for the outcome of fracture, with an estimated number needed to harm of about 250. It should be noted that these are observational studies and do not provide the strongest evidence possible.25 For patients who have been taking these drugs regularly for years, the Canadian Deprescribing Guidelines in the Elderly Project has published evidence-based recommendations on how to taper these drugs safely.26 These guidelines were summarized in a recent issue of American Family Physician (https://www.aafp.org/afp/2019/0101/p57.html).
Screening and Prevention
Our fifth set of POEMs focuses on screening and prevention (Table 5).27–30 Countries such as England have organized screening programs for colorectal cancer. Some programs are now based on the fecal immunochemical test (FIT), because randomized trials show that screening with this test reduces mortality from colorectal cancer. In POEM 17 (a nonrandomized study), the practical advantages of FIT over the older guaiac-based fecal occult blood tests became apparent with a higher return of completed tests (66.4% vs. 59.3%).27 In addition, the rates of cancer and advanced adenoma detection were 0.24% and 1.29% with FIT, and only 0.12% and 0.35% with guaiac-based fecal occult blood tests.
TABLE 5. Screening and Prevention

| Clinical question | Bottom-line answer |
|---|---|
| 17. Are the uptake and detection rates better for the FIT test than for older guaiac-based screening tests for colorectal cancer?27 | The FIT is more sensitive and specific than guaiac-based fecal occult blood tests. We now know that the FIT is also more acceptable to patients and increases uptake in a centrally administered screening program. Physicians should offer patients the option of the FIT or colonoscopy, and should replace their stocks of guaiac-based fecal occult blood tests with FITs in their office practice. |
| 18. In older people without a history of CVD, is statin treatment associated with better outcomes?28 | In this retrospective study, statin treatment in patients 75 years or older without preexisting CVD did not change the likelihood of developing CVD or reduce all-cause mortality. However, patients 75 to 84 years of age with diabetes mellitus benefited from treatment. These results are consistent with ALLHAT findings. |
| 19. Is low-dose aspirin effective for the primary prevention of CVD in moderate-risk patients?29 | In this study, after five years of treatment, patients at moderate risk of heart disease who took low-dose aspirin did not show a decrease in coronary events and all-cause mortality and had slightly more, albeit mostly minor, gastrointestinal bleeding. Using aspirin for primary prevention of CVD is not a one-size-fits-all proposition and may be less beneficial than previously thought. |
| 20. Are there specific interventions that are effective in reducing the risk of injurious falls in older adults?30 | Exercise alone, exercise combined with vision assessment/treatment, exercise combined with vision assessment/treatment and environmental assessment/modification, and clinic-level quality-improvement strategies combined with multifactorial assessment/treatment are all effective interventions for reducing the risk of injurious falls in older adults. |
ALLHAT = Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial; CVD = cardiovascular disease; FIT = fecal immunochemical test.
A top POEM of 2017 described the lipid-lowering trial component of ALLHAT (Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial).31 This POEM reported no benefit from statins for primary prevention of CVD in people 65 to 74 years of age. This finding, with the absence of direct trial evidence of a benefit from statins for primary prevention of CVD in people older than 65 years, may have an impact on future guideline recommendations.
Consistent with the ALLHAT findings, POEM 18 found that in patients 75 years or older without preexisting CVD, statin treatment did not change the likelihood of developing CVD or reduce mortality. However, patients 75 to 84 years of age with diabetes mellitus benefited from treatment.28
Decades of research has attempted to clarify the value of aspirin in the primary prevention of CVD in adults at moderate risk (defined as a 10% to 20% 10-year risk based on age, sex, smoking status, blood pressure, lipids, and family history). POEM 19 describes the ARRIVE (Aspirin to Reduce Risk of Initial Vascular Events) study, a randomized placebo-controlled trial of daily aspirin therapy.29 After five years, patients who took aspirin, 100 mg daily, did not have a decrease in coronary events and all-cause mortality and had slightly more, albeit mostly minor, gastrointestinal bleeding.
A top POEM of 2015 showed that exercise can prevent falls that cause injury in older women.32 POEM 20 summarizes a new systematic review and meta-analysis confirming this earlier finding in older adults.30
Practice Guidelines
Finally, we present the five guidelines that were rated the highest, summarized as POEMs (Table 6).8,11,33–38 The American College of Physicians guidelines recommend an A1C goal of 7% to 8% for most adults with type 2 diabetes.33 The American College of Cardiology/American Heart Association guidelines recommend a blood pressure target of 130/80 mm Hg for most patients based on SPRINT, but this has not been endorsed by the American College of Physicians or American Academy of Family Physicians, who continue to recommend targets of 140/90 mm Hg for most adults and 150/90 mm Hg for adults 60 years or older.11,34,35,39
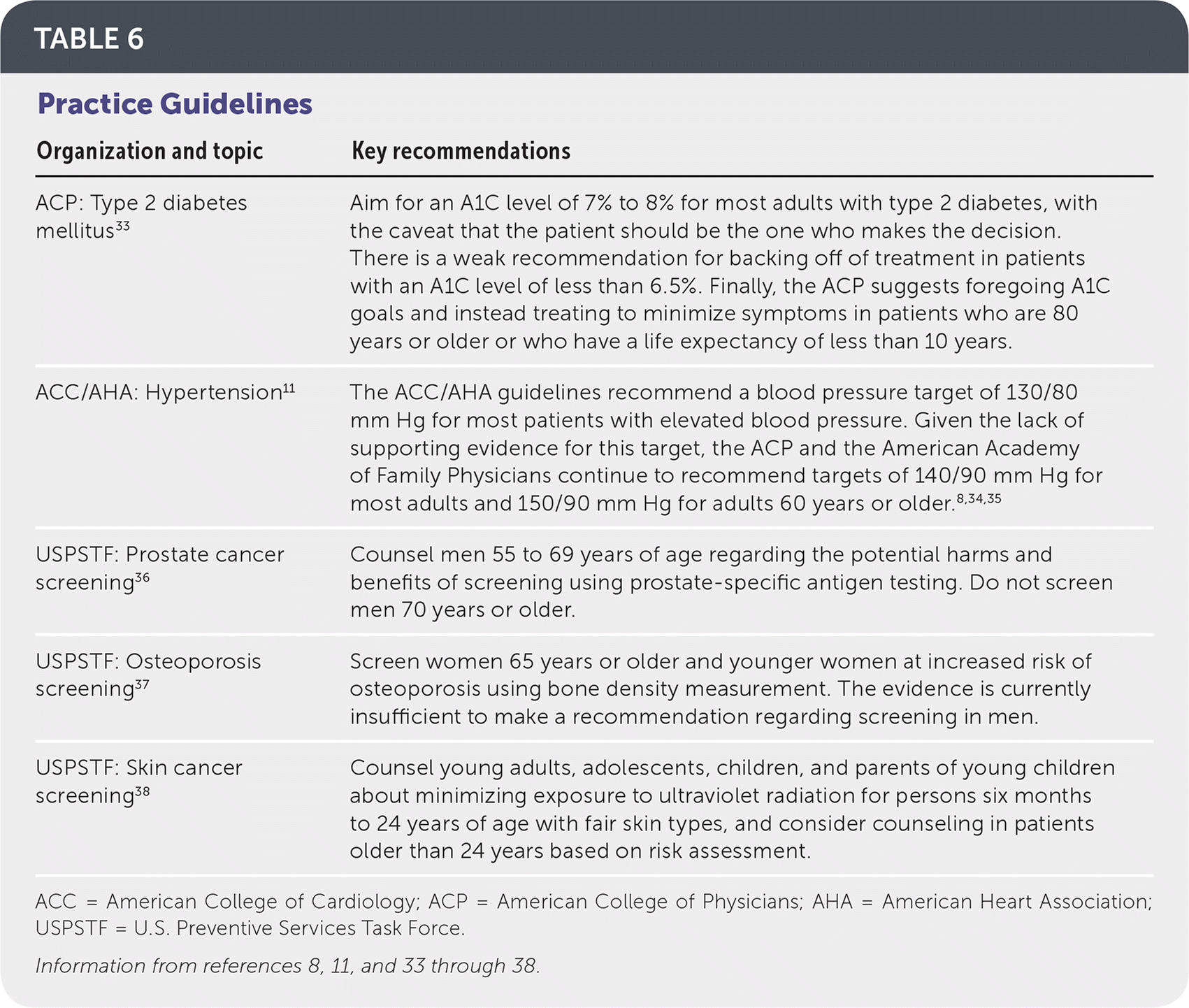
TABLE 6. Practice Guidelines
| Organization and topic | Key recommendations |
|---|---|
| ACP: Type 2 diabetes mellitus33 | Aim for an A1C level of 7% to 8% for most adults with type 2 diabetes, with the caveat that the patient should be the one who makes the decision. There is a weak recommendation for backing off of treatment in patients with an A1C level of less than 6.5%. Finally, the ACP suggests foregoing A1C goals and instead treating to minimize symptoms in patients who are 80 years or older or who have a life expectancy of less than 10 years. |
| ACC/AHA: Hypertension11 | The ACC/AHA guidelines recommend a blood pressure target of 130/80 mm Hg for most patients with elevated blood pressure. Given the lack of supporting evidence for this target, the ACP and the American Academy of Family Physicians continue to recommend targets of 140/90 mm Hg for most adults and 150/90 mm Hg for adults 60 years or older.8,34,35 |
| USPSTF: Prostate cancer screening36 | Counsel men 55 to 69 years of age regarding the potential harms and benefits of screening using prostate-specific antigen testing. Do not screen men 70 years or older. |
| USPSTF: Osteoporosis screening37 | Screen women 65 years or older and younger women at increased risk of osteoporosis using bone density measurement. The evidence is currently insufficient to make a recommendation regarding screening in men. |
| USPSTF: Skin cancer screening38 | Counsel young adults, adolescents, children, and parents of young children about minimizing exposure to ultraviolet radiation for persons six months to 24 years of age with fair skin types, and consider counseling in patients older than 24 years based on risk assessment. |
ACC = American College of Cardiology; ACP = American College of Physicians; AHA = American Heart Association; USPSTF = U.S. Preventive Services Task Force.
The USPSTF recommends counseling men 55 to 69 years of age regarding the potential harms and benefits of prostate cancer screening; screening women 65 or older and younger women at increased risk of osteoporosis to prevent fragility fracture; and counseling young adults, adolescents, children, and parents of young children about minimizing exposure to ultraviolet radiation.36–38 Of note, the American Academy of Family Physicians supports these USPSTF recommendations with the exception of prostate cancer screening, for which it recommends shared decision-making in men who express a desire for screening.40–42
The full text of the POEMs discussed in this article is available at https://www.aafp.org/journals/afp/content/top-poems/2018.html.
A list of top POEMs from previous years is available at https://www.aafp.org/afp/toppoems.
Editor’s Note: This article was cowritten by Dr. Mark Ebell, who is deputy editor for evidence-based medicine for AFP and cofounder and editor-in-chief of Essential Evidence Plus, published by Wiley-Blackwell, Inc. Because of Dr. Ebell’s dual roles and ties to Essential Evidence Plus, the concept for this article was independently reviewed and approved by a group of AFP’s medical editors. In addition, the article underwent peer review and editing by three of AFP’s medical editors. Dr. Ebell was not involved in the editorial decision-making process.—Sumi Sexton, MD, Editor-in-Chief.
The authors thank Wiley-Blackwell, Inc., for giving permission to excerpt the POEMs; Drs. Allen Shaughnessy, Henry Barry, David Slawson, Nita Kulkarni, and Linda Speer for their work in selecting and writing the original POEMs; the academic family medicine fellows and faculty of the University of Missouri– Columbia for their work as peer reviewers; Pierre Pluye, PhD, for his work in codeveloping the Information Assessment Method; and Maria Vlasak for her assistance with copyediting the POEMs for the past 25 years.

