Key Points for Practice
• The ACS recommends yearly screening for breast cancer in women 45 to 54 years of age and those 40 to 44 years of age who choose earlier screening.
• Women with atypical squamous cells of undetermined significance on cervical cancer screening that were found to be negative for HPV should have repeat screening in three years.
• Physicians should initiate discussions on prostate cancer with those at average risk starting at 50 years of age, at 45 years with higher risk, and at 40 years in those at even higher risk.
From the AFP Editors
The American Cancer Society (ACS) provides a summary of recommendations for cancer screening (Table 1) each year, including any updates and recent data, and advice for when recommendations cannot be made. In addition to this summary, the 2018 report outlines issues that affect screening for breast, cervical, colorectal, and prostate cancer; further explains the 2013 recommendations for lung cancer screening via low-dose computed tomography; compares the ACS recommendations with those of other professional health care organizations; and provides information from the National Health Interview Survey.
TABLE 1 American Cancer Society Recommendations for the Early Detection of Cancer in Average-Risk Asymptomatic Adults*
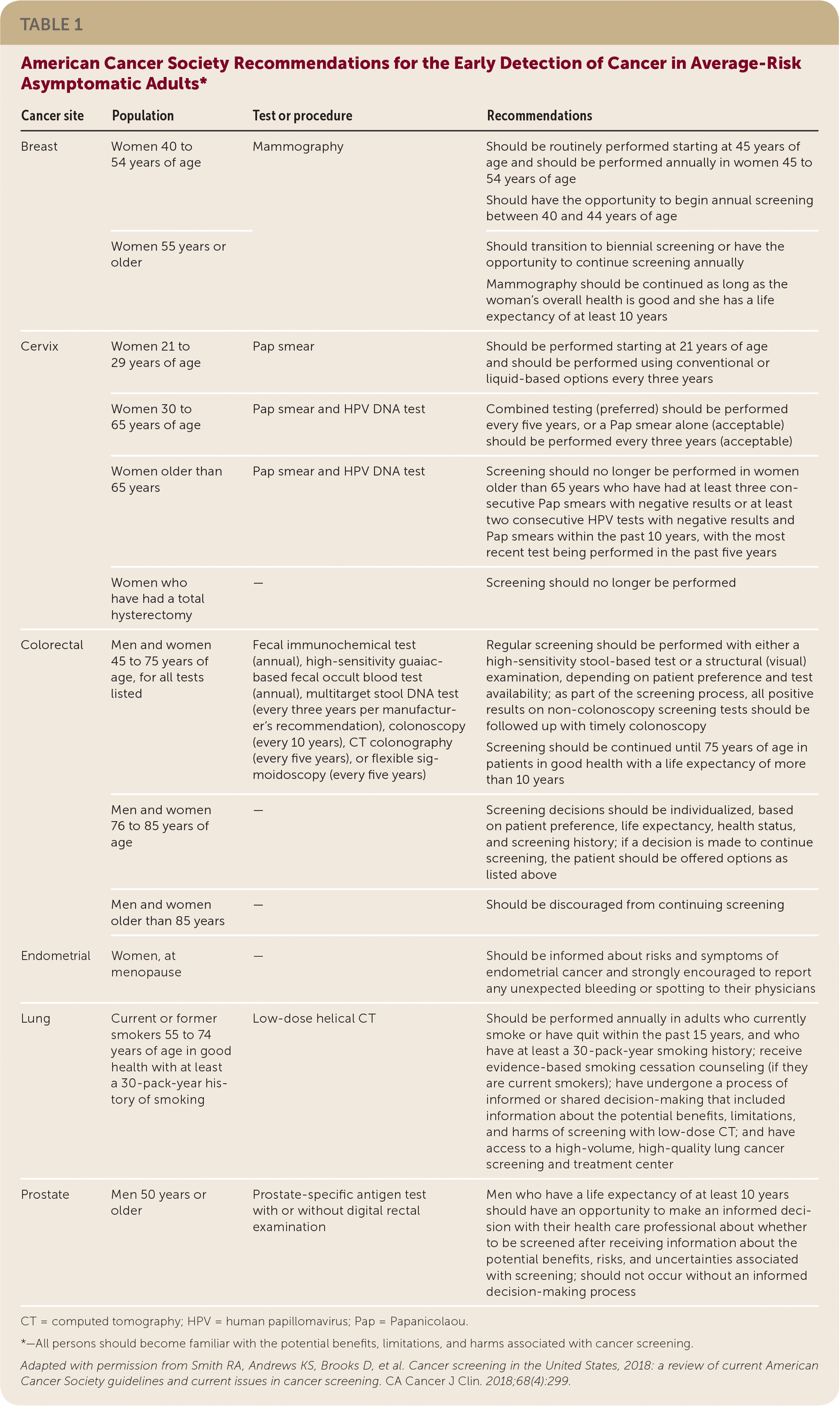
| Cancer site | Population | Test or procedure | Recommendations |
|---|---|---|---|
| Breast | Women 40 to 54 years of age | Mammography | Should be routinely performed starting at 45 years of age and should be performed annually in women 45 to 54 years of age Should have the opportunity to begin annual screening between 40 and 44 years of age |
| Women 55 years or older | Should transition to biennial screening or have the opportunity to continue screening annually Mammography should be continued as long as the woman's overall health is good and she has a life expectancy of at least 10 years | ||
| Cervix | Women 21 to 29 years of age | Pap smear | Should be performed starting at 21 years of age and should be performed using conventional or liquid-based options every three years |
| Women 30 to 65 years of age | Pap smear and HPV DNA test | Combined testing (preferred) should be performed every five years, or a Pap smear alone (acceptable) should be performed every three years (acceptable) | |
| Women older than 65 years | Pap smear and HPV DNA test | Screening should no longer be performed in women older than 65 years who have had at least three consecutive Pap smears with negative results or at least two consecutive HPV tests with negative results and Pap smears within the past 10 years, with the most recent test being performed in the past five years | |
| Women who have had a total hysterectomy | — | Screening should no longer be performed | |
| Colorectal | Men and women 45 to 75 years of age, for all tests listed | Fecal immunochemical test (annual), high-sensitivity guaiac-based fecal occult blood test (annual), multitarget stool DNA test (every three years per manufacturer's recommendation), colonoscopy (every 10 years), CT colonography (every five years), or flexible sigmoidoscopy (every five years) | Regular screening should be performed with either a high-sensitivity stool-based test or a structural (visual) examination, depending on patient preference and test availability; as part of the screening process, all positive results on noncolonoscopy screening tests should be followed up with timely colonoscopy Screening should be continued until 75 years of age in patients in good health with a life expectancy of more than 10 years |
| Men and women 76 to 85 years of age | — | Screening decisions should be individualized, based on patient preference, life expectancy, health status, and screening history; if a decision is made to continue screening, the patient should be offered options as listed above | |
| Men and women older than 85 years | — | Should be discouraged from continuing screening | |
| Endometrial | Women, at menopause | — | Should be informed about risks and symptoms of endometrial cancer and strongly encouraged to report any unexpected bleeding or spotting to their physicians |
| Lung | Current or former smokers 55 to 74 years of age in good health with at least a 30-pack-year history of smoking | Low-dose helical CT | Should be performed annually in adults who currently smoke or have quit within the past 15 years, and who have at least a 30-pack-year smoking history; receive evidence-based smoking cessation counseling (if they are current smokers); have undergone a process of informed or shared decision-making that included information about the potential benefits, limitations, and harms of screening with low-dose CT; and have access to a high-volume, high-quality lung cancer screening and treatment center |
| Prostate | Men 50 years or older | Prostate-specific antigen test with or without digital rectal examination | Men who have a life expectancy of at least 10 years should have an opportunity to make an informed decision with their health care professional about whether to be screened after receiving information about the potential benefits, risks, and uncertainties associated with screening; should not occur without an informed decision-making process |
CT = computed tomography; HPV = human papillomavirus; Pap = Papanicolaou.
*—All persons should become familiar with the potential benefits, limitations, and harms associated with cancer screening.
Adapted with permission from Smith RA, Andrews KS, Brooks D, et al. Cancer screening in the United States, 2018: a review of current American Cancer Society guidelines and current issues in cancer screening. CA Cancer J Clin. 2018;68(4):299.
Breast Cancer
Breast cancer is the most common cancer in women living in the United States, with an estimated 266,120 patients diagnosed with invasive breast cancer in 2018 and an associated 40,920 deaths. The ACS screening recommendations in women at average risk were updated in 2015 and have not changed. This guideline underscores the importance of yearly screening in women 45 to 54 years of age and those 40 to 44 years who choose earlier screening, because evidence has shown that such screening in premenopausal women is associated with a significantly decreased risk of identifying advanced breast cancer compared with screening performed every other year. Postmenopausal women do not have similar benefits associated with yearly screening, unless they are currently receiving hormone treatment for menopause; therefore, women 55 years or older can receive screening every other year or yearly, depending on patient preference. An age to stop screening is not identified, but continued screening may be beneficial in certain women 75 years or older, taking into account mortality, age, comorbidities, and function. These recommendations were made after a review of the burden of disease and of the benefits and harms of screening. An update to the 2007 screening recommendations in women at greater than average risk is currently being completed.
Cervical Cancer
An estimated 13,240 persons will be diagnosed with invasive cervical cancer in 2018, with an associated 4,170 deaths. The ACS, American Society for Colposcopy and Cervical Pathology, and American Society for Clinical Pathology recommendations for screening are based on age, history of screening, and available screening options. Currently, the guidelines address screening women 21 to 65 years of age and 65 years or older who are at average risk of cervical cancer, recommending that women younger than 21 years not be screened regardless of any risk factors or sexual history. They also address the human papillomavirus (HPV) vaccine and other special considerations. The current guidelines recommend that women with atypical squamous cells of undetermined significance that were found to be negative for HPV should have repeat screening in three years. The recommendations on atypical squamous cells of undetermined significance and HPV vaccines have been added since the 2012 guideline, and a full update of the cervical cancer screening guidelines is currently being completed.
Colorectal Cancer
An estimated 140,250 persons will be diagnosed with colorectal cancer in 2018, with an associated 50,630 deaths. Despite this, the incidence and mortality rates have been decreasing in persons 50 years or older, based mainly on the use of screening for prevention and early identification. In 2018, the ACS updated its recommendations for screening in persons at average risk, with the most notable change being to start screening at 45 years of age; emphasizing screening in general via a variety of options, with appropriate guidance about their benefits and harms, rather than a preference for certain screening options; and describing follow-up protocols in patients with concerning results on stool testing. The guidance specific to persons at increased and high risk was last updated in 2001.
Prostate Cancer
Prostate cancer is the second most common cancer in U.S. men, with an estimated 164,690 diagnoses in 2018 and an associated 29,430 deaths. Recommendations for early identification of prostate cancer were last published in 2010, with a full update anticipated for 2019. Decisions about screening should be made using an informed decision-making process, with physicians initiating discussions with those at average risk starting at 50 years of age, with those at high risk (e.g., black, family history of a diagnosis at younger than 65 years) at age 45, and those at even higher risk (e.g., family history of multiple diagnoses at younger than 65 years) at age 40.
Lung Cancer
In its 2013 guidance, the ACS recommended that physicians discuss current smoking, as well as smoking history, with persons 55 to 74 years of age. Subsequently, physicians who have contacts with high-quality treatment facilities also should discuss screening methods and their associated benefits and harms with those patients in good health who have at least a 30-pack-year history of smoking, who smoke currently, or who only quit smoking in the past 15 years. This recommendation, however, has been misconstrued by some physicians to mean that decisions to screen should involve shared decision-making, instead of a firm recommendation to screen combined with appropriate discussions with the patient.
To clarify this recommendation and appropriately place the emphasis, as ACS intended, on a firm recommendation for screening, in 2017, the ACS modified the wording to say that yearly screening should be performed with low-dose computed tomography in this patient population, combined with counseling on smoking cessation in current smokers and provision of information about benefits and harms of such screening. In addition, smoking cessation counseling was emphasized as an important component of identifying adults who should receive screening, which is not a replacement for smoking cessation.
Editor's Note: The AAFP's screening recommendations differ in some important respects from those of the ACS. The AAFP recommends starting routine mammography and colorectal cancer screening at age 50 in average-risk adults, and supports providing prostate specific antigen–based screening only to men 55 to 69 years of age who express a clear preference for the test after shared decision-making. In contrast to the ACS's “firm recommendation to screen” for lung cancer in persons 55 to 74 years of age with at least a 30-pack-year history of smoking, the AAFP concluded that the evidence was insufficient to recommend for or against annual low-dose computed tomography in this population. In its recommendation, the AAFP cited concerns about high false-positive rates, unknown long-term harms of radiation exposure from follow-up full-dose computed tomography, and the lack of replication of the National Lung Screening Trial results in community settings (https://www.aafp.org/patient-care/clinical-recommendations/all/lung-cancer.html).—Kenny Lin, MD, MPH, Deputy Editor
Guideline source: American Cancer Society
Evidence rating system used? Yes
Systematic literature search described? No
Guideline developed by participants without relevant financial ties to industry? No
Recommendations based on patient-oriented outcomes? Yes
Published source: CA Cancer J Clin. July/August, 2018;68(4):297–316

