Clinical Question
When is it safe to treat a patient with community-acquired pneumonia (CAP) as an outpatient?
Evidence Summary
Some patients with CAP can be treated safely as outpatients. Several clinical prediction rules have been developed to determine the likelihood of mortality in patients with CAP, and the use of these rules is recommended by practice guidelines to support clinician decision-making. For example, the 2007 guidelines from the Infectious Diseases Society of America and American Thoracic Society note that the Pneumonia Severity Index and the CURB-65 (confusion, uremia, respiratory rate, blood pressure, 65 years of age) rule can help identify patients with CAP who are candidates for outpatient therapy.1 The 2009 guidelines from the British Thoracic Society recommend use of the CURB-65 rule for patients evaluated in the emergency department and the CRB-65 rule for patients evaluated in the primary care or community setting.2
The Pneumonia Severity Index (https://www.mdcalc.com/psi-port-score-pneumonia-severity-index-cap) has been developed and validated in hospital-based settings.3,4 However, the rule has 20 data elements, and a chest radiograph and several blood tests, such as arterial blood gas, are required. Even in the emergency department setting where these tests are readily available, the number of data elements makes the Pneumonia Severity Index difficult to use in real-world practice.
The CURB-65 (https://www.mdcalc.com/curb-65-score-pneumonia-severity) has only five data elements, is accurate, and has been well validated.5 However, it requires blood urea nitrogen testing, which is not readily available in the outpatient primary care setting. The CRB-65 is identical to the CURB-65, except that it does not require a blood urea nitrogen measurement, and has also been well validated in the primary care setting. A recent meta-analysis of the CRB-65 found an overall area under the receiver operating characteristic curve of 0.74 (good discrimination); a ratio of observed to expected mortality of 1.04 (good calibration); and likelihood ratios for mortality of 0.13, 1.3, and 5.6 for low-, moderate-, and high-risk groups, respectively. The meta-analysis was limited to the eight studies judged to be at low risk of bias in which patients could be treated as outpatients or inpatients.6
Because it has only four data elements and does not require blood tests or a radiograph, the CRB-65 is the best choice for risk stratification in the outpatient primary care setting. In two European studies, the overall mortality was 4% in patients with CAP presenting in the outpatient primary care setting who could be treated as inpatients or outpatients.5,7 Applying the likelihood ratios to this baseline risk of mortality, the mortality rate for patients at low, moderate, and high risk based on the CRB-65 rule is shown in Table 1.5–7
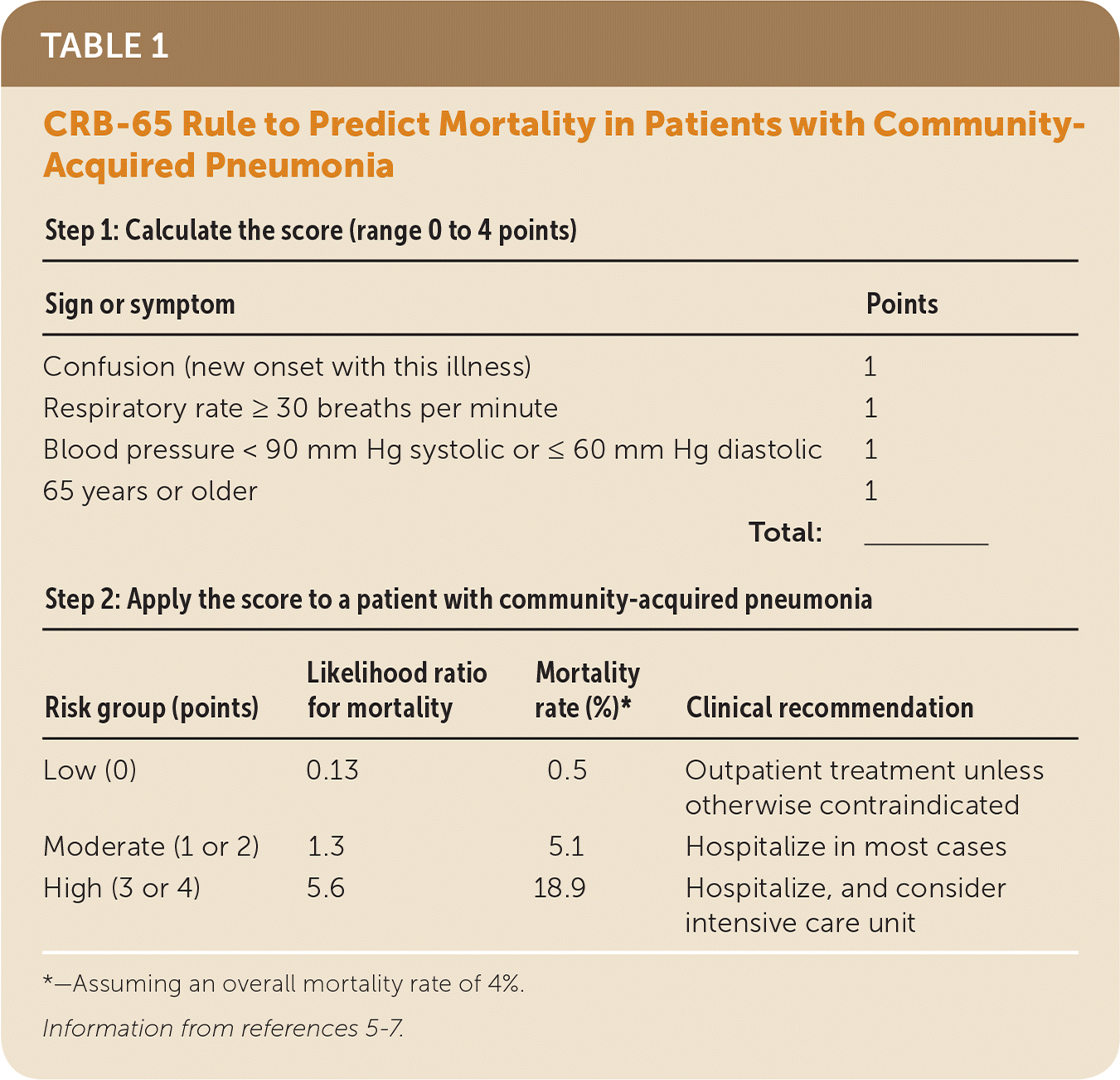
TABLE 1. CRB-65 Rule to Predict Mortality in Patients with Community-Acquired Pneumonia
| Step 1: Calculate the score (range 0 to 4 points) | |||
| Sign or symptom | Points | ||
| Confusion (new onset with this illness) | 1 | ||
| Respiratory rate ≥ 30 breaths per minute | 1 | ||
| Blood pressure < 90 mm Hg systolic or ≤ 60 mm Hg diastolic | 1 | ||
| 65 years or older | 1 | ||
| Total: | ______ | ||
| Step 2: Apply the score to a patient with community-acquired pneumonia | |||
| Risk group (points) | Likelihood ratio for mortality | Mortality rate (%)* | Clinical recommendation |
| Low (0) | 0.13 | 0.5 | Outpatient treatment unless otherwise contraindicated |
| Moderate (1 or 2) | 1.3 | 5.1 | Hospitalize in most cases |
| High (3 or 4) | 5.6 | 18.9 | Hospitalize, and consider intensive care unit |
*—Assuming an overall mortality rate of 4%.
It is important to note that because patients 65 years or older receive one point using the CRB-65 rule, they should be considered for inpatient therapy. In addition, external factors such as important comorbidities not included in the clinical rules (e.g., HIV, chronic obstructive pulmonary disease), failure of outpatient oral therapy, and social factors (e.g., a patient's inability to obtain or reliably take medication) are appropriate considerations when deciding on inpatient or outpatient treatment.
Applying the Evidence
A previously healthy 56-year-old man presents with two days of worsening cough, purulent sputum production, measured fever of 102°F (39°C), myalgias, and chills. He has no signs of confusion. His respiratory rate is 20 breaths per minute, and his blood pressure is 124/82 mm Hg. Examination findings are consistent with CAP; a chest radiograph shows an infiltrate, confirming the diagnosis.
The patient's CRB-65 score is 0, so you decide to treat him as an outpatient. You schedule a nurse visit at 24 hours and return visits to see you at three and seven days, and the patient does well.

