A 72-year-old man presented with a worsening pruritic rash and painful blisters on his trunk, bilateral upper and lower extremities, face, and groin. The rash appeared two months prior. He had a history of hypertension and diabetes mellitus.
Physical examination revealed extensive, nearly confluent, pink-red plaques associated with tense and flaccid bullae, as well as erosions resulting from ruptured bullae (Figure 1). He had larger hyperpigmented patches with erosions, ulcerations, and inflammatory, red borders on his trunk. Tense bullae were largely localized to the inflammatory borders. There were no mucosal lesions.
FIGURE 1
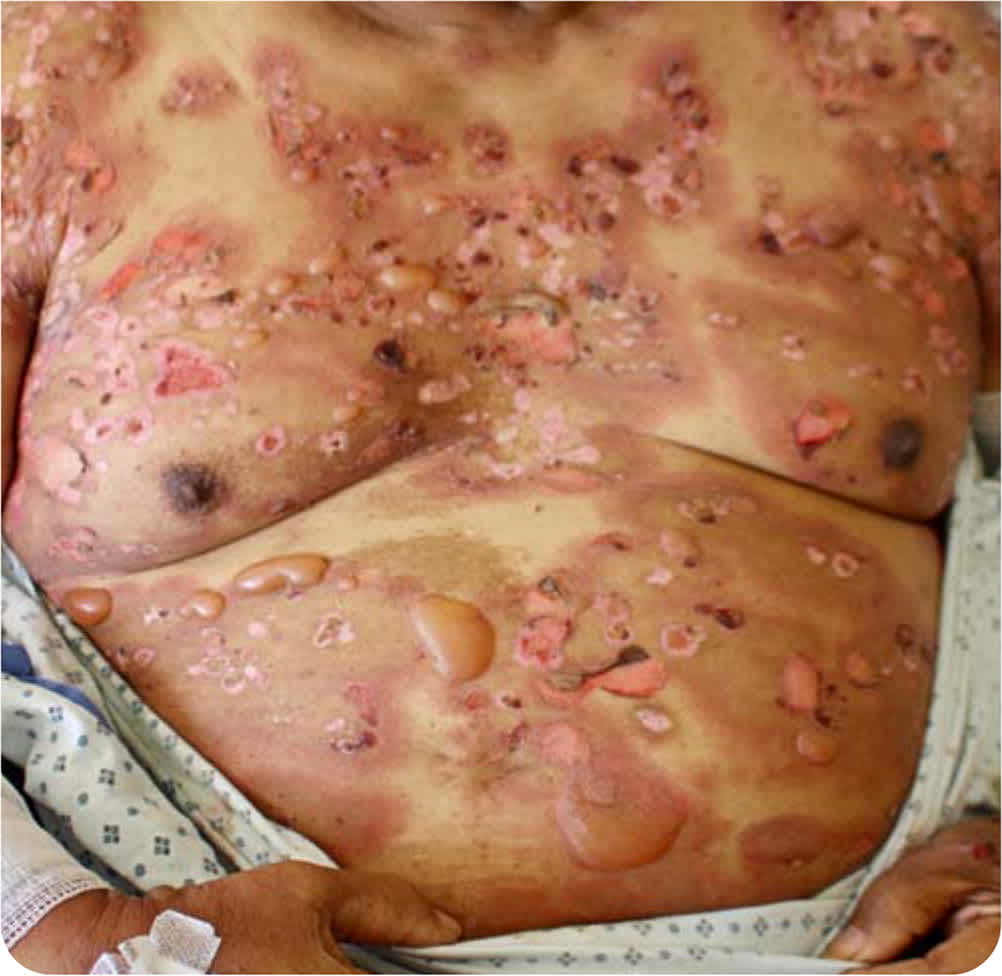
The patient's complete blood count results were remarkable for an eosinophil count of 1,800 per uL (1.80 × 109 per L; 14%; twice the upper limit of normal). Serum immunoglobulin E (IgE) levels were elevated at 700 kU per L (reference range: 0 to 115 kU per L). Histologic examination of a punch biopsy from the edge of a tense bulla revealed a subepidermal blister with a mixed inflammatory infiltrate including eosinophils. Direct immunofluorescence of a punch biopsy from adjacent skin showed linear IgG deposition at the dermal-epidermal junction.
Question
Based on the patient's history, physical examination, and laboratory findings, which one of the following is the most likely diagnosis?
A. Bullosis diabeticorum.
B. Bullous pemphigoid.
C. Pemphigus vulgaris.
D. Stevens-Johnson syndrome.
Discussion
The answer is B: bullous pemphigoid. Bullous pemphigoid is an autoimmune disorder characterized by autoantibodies targeting hemidesmosomal proteins of the skin and potentially mucous membranes. The primary autoantigens implicated are collagen XVII and dystonin-e. Classic bullous pemphigoid presents with tense, serous, or hemorrhagic bullae of 1 to 3 cm in diameter on the trunk and extremities that are often associated with urticarial plaques.1 In patients of color, these urticarial plaques may become hyperpigmented over time as in this patient. Typically, the skin shows a mixture of tense bullae, as well as erosions and ulcerations from ruptured bullae. Patients describe intense pruritus and often have eosinophilia.
Bullous pemphigoid is most common in women and older adults. The typical age of onset is 60 to 80 years. The Asboe-Hansen sign, also known as the indirect Nikolsky sign, is a common finding in patients with bullous pemphigoid. This sign is the extension of a blister to adjacent unblistered skin when pressure is applied on the top of a bulla.
Histologically, bullous pemphigoid presents with subepidermal blister formation, often with eosinophil accumulation at the dermal-epidermal junction. Linear deposition of IgG and C3 at the dermal-epidermal junction can be shown on direct immunofluorescence, which is the best method for diagnosis of bullous pemphigoid with a sensitivity of 90.8%.2 Detection of circulating autoantibodies against collagen XVII and dystonin-e by enzyme-linked immunosorbent assay may aid in the diagnosis.
Bullosis diabeticorum is a rare blistering condition in patients with diabetes. It is characterized by spontaneous formation of tense bullae on normal-appearing, noninflamed skin on the feet, lower legs, and hands. The lesions are usually asymptomatic and are believed to be associated with peripheral neuropathy.3
Pemphigus vulgaris is also an autoimmune blistering disease of the skin. It typically presents with painful, flaccid bullae with erosions and hemorrhagic crust formation on the face, scalp, trunk, and intertriginous areas. Pemphigus vulgaris usually occurs in younger patients (mean age of onset is 40 to 60 years) and often has mucosal involvement. The Nikolsky sign (dislodgement of superficial epidermis with a shearing force) is typically present, indicating a plane of cleavage in the skin at the dermal-epidermal junction. The autoantibodies in pemphigus vulgaris are directed against desmogleins within the epidermis.3
Stevens-Johnson syndrome is a rare and potentially fatal drug reaction that presents with painful skin and mucosal erosions. Typically, the rash begins as a pink-red morbilli-form rash on the face, trunk, and extremities (including palms and soles) that progresses to purpuric macules and papules with painful epidermal detachment within one to three days. There is always mucosal involvement, typically painful erosions in buccal, ocular, and genital mucosae. The Nikolsky sign is usually present.3
SUMMARY TABLE

| Condition | Clinical characteristics | Mucosal involvement | Nikolsky sign |
|---|---|---|---|
| Bullosis diabeticorum | Tense bullae on normal-appearing, noninflamed acral sites in patients with diabetes mellitus; asymptomatic lesions | Not present | Not present |
| Bullous pemphigoid | Tense, serous, or hemorrhagic bullae on the trunk and extremities; often associated with pruritic urticarial plaques | Not commonly present | Not present (positive Asboe-Hansen sign) |
| Pemphigus vulgaris | Painful, flaccid bullae with erosions and hemorrhagic crust formation; usually on the face, scalp, trunk, and intertriginous areas | Present | Present |
| Stevens-Johnson syndrome | Pink-red morbilliform rash on the face, trunk, and extremities that progresses to purpuric macules and patches with painful epidermal detachment | Present | Present |

