Clinical Question
Does pelvic floor muscle training improve the symptoms of urinary incontinence in women?
Evidence-Based Answer
Use of pelvic floor muscle training to treat women with all subtypes of urinary incontinence results in improvement or cure vs. no treatment (number needed to treat [NNT] = 2.5; 95% CI, 1.4 to 5.4). Treatment with pelvic floor muscle training also results in one fewer episode of leakage per day and a reduction in leakage volume of 9.7 g per hour. Treatment is cost-effective, and risks are minimal.1 (Strength of Recommendation: A, based on consistent, good-quality patient-oriented evidence.)
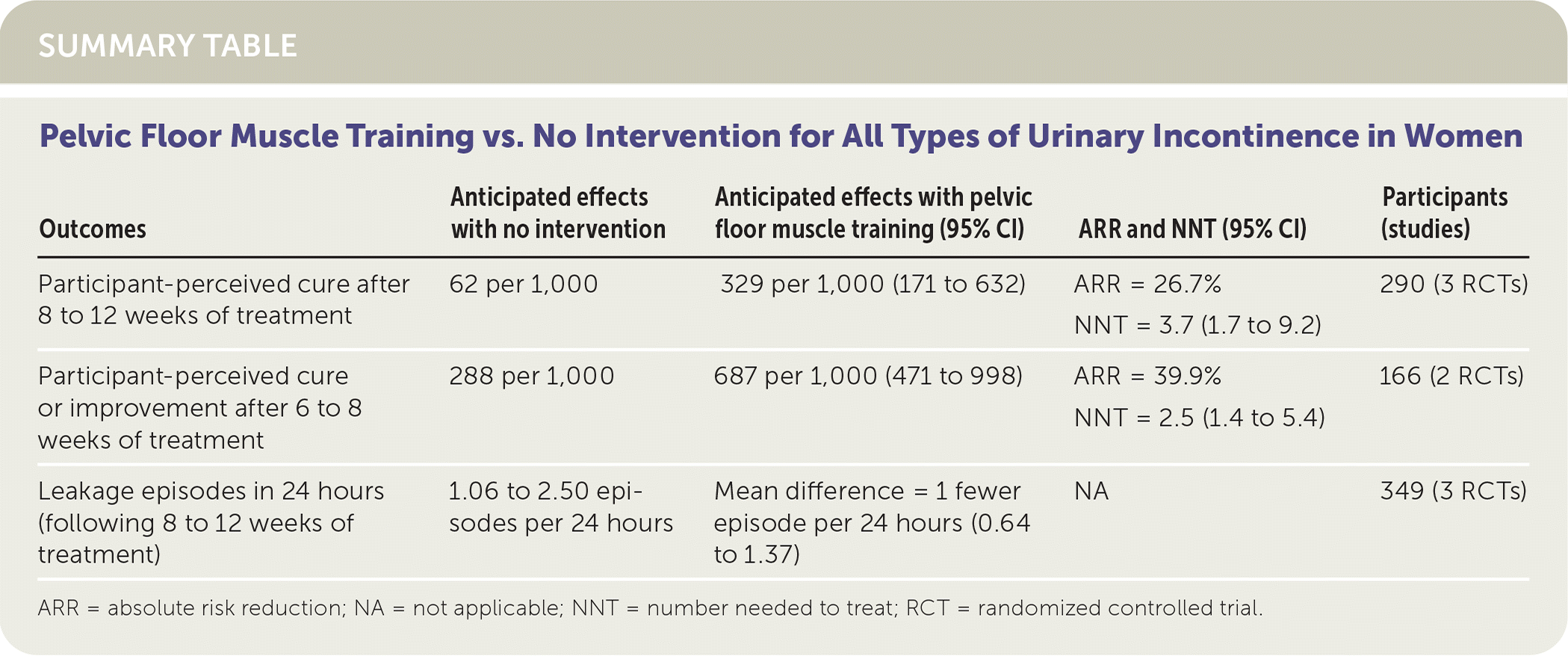
SUMMARY TABLE
| Outcomes | Anticipated effects with no intervention | Anticipated effects with pelvic floor muscle training (95% CI) | ARR and NNT (95% CI) | Participants (studies) |
|---|---|---|---|---|
| Participant-perceived cure after 8 to 12 weeks of treatment | 62 per 1,000 | 329 per 1,000 (171 to 632) | ARR = 26.7% NNT = 3.7 (1.7 to 9.2) | 290 (3 RCTs) |
| Participant-perceived cure or improvement after 6 to 8 weeks of treatment | 288 per 1,000 | 687 per 1,000 (471 to 998) | ARR = 39.9% NNT = 2.5 (1.4 to 5.4) | 166 (2 RCTs) |
| Leakage episodes in 24 hours (following 8 to 12 weeks of treatment) | 1.06 to 2.50 episodes per 24 hours | Mean difference = 1 fewer episode per 24 hours (0.64 to 1.37) | NA | 349 (3 RCTs) |
ARR = absolute risk reduction; NA = not applicable; NNT = number needed to treat; RCT = randomized controlled trial.
Practice Pointers
Urinary incontinence affects an estimated 15% to 46% of community-dwelling older adults2 and has profound health impacts, limiting social engagement and sexual function. Urinary incontinence is a primary driver for initiation of nursing home care and contributes to skin breakdown and increased falls, with a projected cost of $82.6 billion in 2020.3 Historically, pelvic floor muscle training has been reserved primarily for stress incontinence, rather than mixed or urge incontinence.4 The authors of this Cochrane review sought to demonstrate whether pelvic floor muscle training can be applied to all types of urinary incontinence in women, as well as to confirm its effectiveness.
This Cochrane review included 31 trials and 1,817 patients, with a follow-up time of less than 12 months.1 Trials varied widely in study populations, outcome measures, and treatment characteristics. Only randomized controlled trials or quasi-randomized controlled trials were included in the review, with women who had urinary incontinence randomized to treatment with pelvic floor muscle training or to a control arm that consisted of no treatment, sham/placebo treatment, or inactive control treatment. Treatment duration varied from six weeks to six months, and trials were subgrouped by diagnosis of urinary incontinence and outcome measures.
Studies with different end points could not be merged, but for women with urinary incontinence of any subtype, pelvic floor muscle training improved the likelihood of reporting improvement or cure using various validated scales and questionnaires compared with patients in the control groups (67% vs. 29%; relative risk = 2.39; 95% CI, 1.64 to 3.47; two trials; 166 women; moderate-quality evidence). Pelvic floor muscle training also decreased average daily leakage episodes in women with any type of urinary incontinence. Volume of urine leakage varied among patients studied, but it was reduced in all women with incontinence, no matter the subtype.
The highest-quality randomized controlled trials indicated that women with stress urinary incontinence who received pelvic floor muscle training were more likely to report a symptomatic cure than patients not using pelvic floor muscle training (56% vs. 6%; four trials; 165 women; NNT = 2.2; 95% CI, 1 to 6). Women with stress urinary incontinence were also more likely to report improvement or cure (NNT to achieve this parameter = 1.5; 95% CI, 1 to 3). Volume of urine leakage was reduced in those with stress urinary incontinence by a mean difference (MD) of 9.7 g per hour (95% CI, 0.5 to 18.92). The authors of the review did not comment on what should be considered a clinically meaningful difference. Women with stress urinary incontinence treated with pelvic floor muscle training also had fewer episodes of leakage per day (MD = 1.23 fewer episodes per day; 95% CI, 0.68 to 1.78; seven trials; 432 women), although as a whole, women with urinary incontinence of all types also had fewer episodes per day (MD = 1.00 fewer episodes; 95% CI, 0.64 to 1.37; four trials; 349 women).
Women who received pelvic floor muscle training also reported improved quality of life and higher satisfaction with treatment. Trials were small and mostly of moderate quality using GRADE rating for many reasons, including the inability to blind patients to treatment intervention. However, trials consistently demonstrated that pelvic floor muscle training conferred significant benefit on all types of urinary incontinence, including mixed and urge urinary incontinence. Adverse effects were rare and minor, with the most common being psychological discomfort from focusing on incontinence.
Practice guidelines from the American College of Obstetricians and Gynecologists state that pelvic floor muscle training can be effective when used as first-line therapy for stress, urge, or mixed urinary incontinence.5 Information for patients about how to do pelvic exercises on their own can be found online at https://www.youtube.com/watch?v=kQKR5uLkeUM. Family physicians should engage patients using a shared decision-making approach and consider educating patients on the usefulness of pelvic floor muscle training as first-line treatment for women with any type of urinary incontinence.
The practice recommendations in this activity are available at http://www.cochrane.org/CD005654.
Editor's Note: The absolute risk reductions and numbers needed to treat reported in this Cochrane for Clinicians were calculated by the authors based on raw data provided in the original Cochrane review. Dr. Fogleman is an assistant medical editor for AFP.

