Asymptomatic bacteriuria, defined as the presence of bacteria in the urine in the absence of urinary symptoms, is a common clinical finding that often warrants a decision about whether to initiate antimicrobial therapy. There are few indications to treat asymptomatic bacteriuria, and inappropriate treatment contributes to the development of antimicrobial resistance. In 2019, the Infectious Diseases Society of America revised its 2005 guidelines on asymptomatic bacteriuria, incorporating new evidence. The updated guidelines recommend screening and appropriate treatment for asymptomatic bacteriuria in pregnant women and in individuals undergoing endourological procedures associated with mucosal trauma. The guidelines recommend against screening and treatment in infants and children; healthy adults, including nonpregnant pre- and postmenopausal women; and patients with diabetes mellitus, long-term indwelling catheters, or spinal cord injuries. The guidelines also recommend against screening and treatment in patients undergoing nonurological surgery, patients who have had a kidney transplant more than one month prior, recipients of other solid organ transplants, or those with impaired voiding following spinal cord injury. Although delirium in older adults can be caused by a urinary tract infection, the guidelines recommend that patients with delirium and no urinary or systemic symptoms be assessed for other causes of delirium, rather than initiating treatment for asymptomatic bacteriuria, because treatment has not been shown to have any beneficial effect on clinical outcomes.
Urinary tract infections (UTIs) are among the most common reasons antimicrobials are prescribed. Often, however, clinicians prescribe antimicrobials for asymptomatic bacteriuria, which is defined as the presence of bacteria in the urine in the absence of urinary symptoms. Treating asymptomatic bacteriuria is not beneficial for most patients and may be detrimental. For example, a retrospective study of more than 2,700 patients with asymptomatic bacteriuria at 46 hospitals showed that antimicrobial treatment did not improve outcomes and was associated with longer hospitalization.1
WHAT'S NEW ON THIS TOPIC
A 2019 retrospective study of more than 2,700 patients with asymptomatic bacteriuria at 46 hospitals showed that antimicrobial treatment does not improve outcomes and is associated with longer hospitalization.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
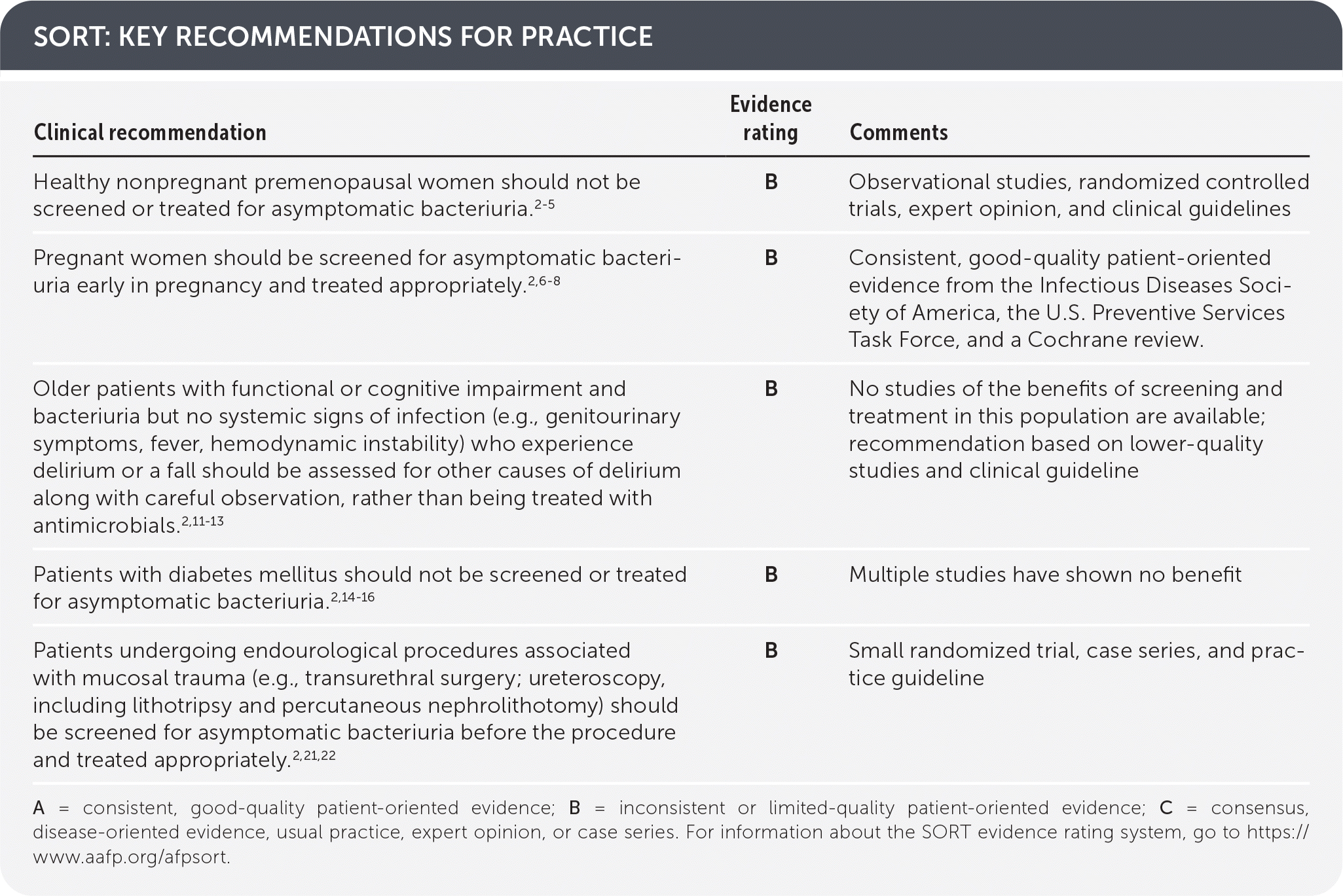
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN INFECTIOUS DISEASE
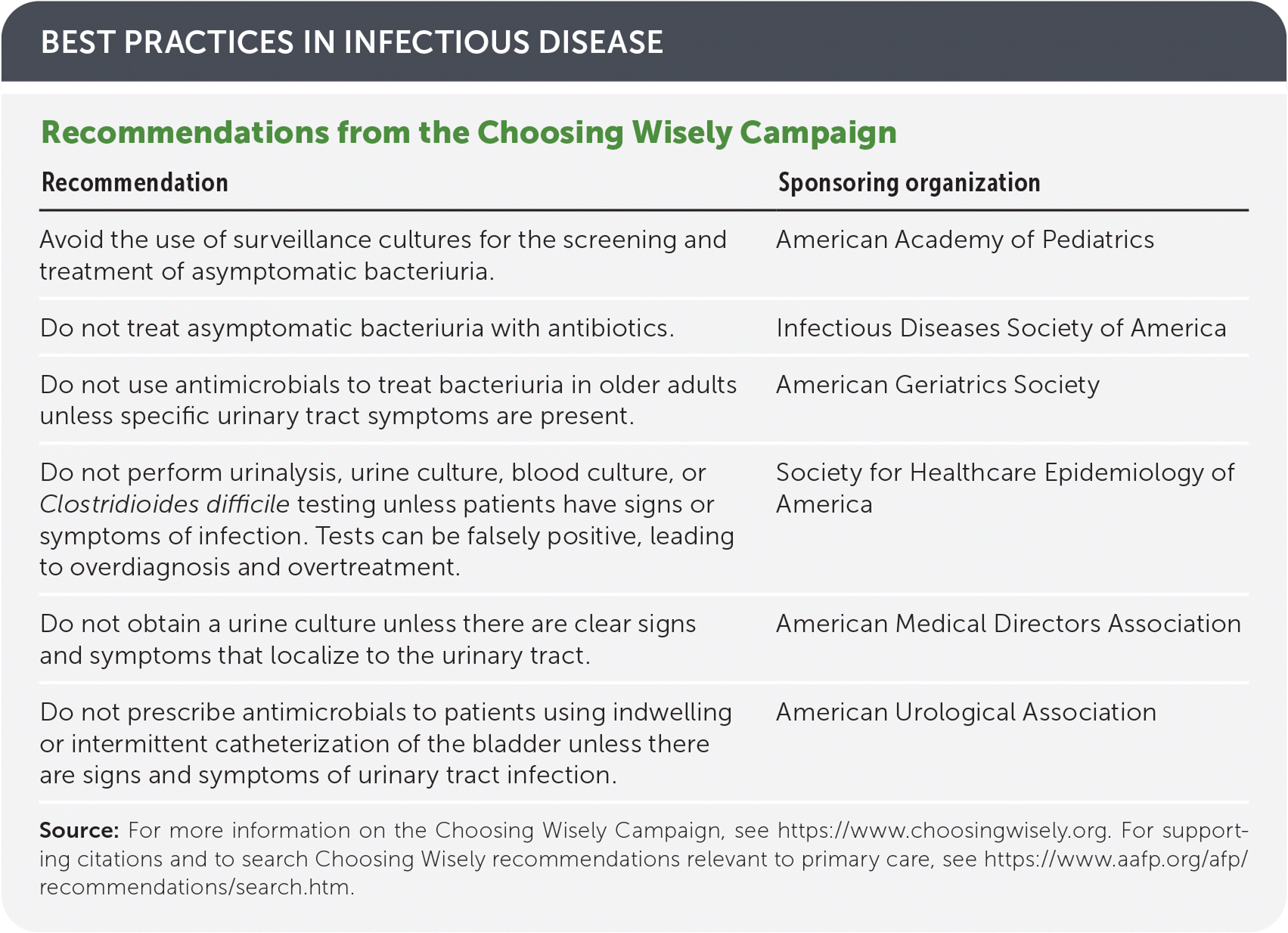
| Recommendation | Sponsoring organization |
|---|---|
| Avoid the use of surveillance cultures for the screening and treatment of asymptomatic bacteriuria. | American Academy of Pediatrics |
| Do not treat asymptomatic bacteriuria with antibiotics. | Infectious Diseases Society of America |
| Do not use antimicrobials to treat bacteriuria in older adults unless specific urinary tract symptoms are present. | American Geriatrics Society |
| Do not perform urinalysis, urine culture, blood culture, or Clostridioides difficile testing unless patients have signs or symptoms of infection. Tests can be falsely positive, leading to overdiagnosis and overtreatment. | Society for Healthcare Epidemiology of America |
| Do not obtain a urine culture unless there are clear signs and symptoms that localize to the urinary tract. | American Medical Directors Association |
| Do not prescribe antimicrobials to patients using indwelling or intermittent catheterization of the bladder unless there are signs and symptoms of urinary tract infection. | American Urological Association |
Source: For more information on the Choosing Wisely Campaign, see https://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
Antimicrobial resistance is increasing around the world, and antimicrobial stewardship programs have identified inappropriate treatment of asymptomatic bacteriuria as an important reason for unnecessary antimicrobial use.2 In 2019, the Infectious Diseases Society of America (IDSA) updated its guidelines on screening and treatment for asymptomatic bacteriuria.2 The guidelines include recommendations for populations not addressed in previous guidelines, such as children, and patients with solid organ transplants. This article reviews the key recommendations from the new guidelines.
Epidemiology
Although asymptomatic bacteriuria is uncommon in children (less than 1% in boys and 1% to 2% in girls), it occurs in up to 5% of healthy premenopausal women, 2.8% to 8.6% of postmenopausal women, and 1.9% to 9.5% of pregnant women.2 Asymptomatic bacteriuria occurs in 100% of patients with long-term indwelling catheters.2 Table 1 shows the prevalence of asymptomatic bacteriuria in different patient populations.2
TABLE 1. Prevalence of Asymptomatic Bacteriuria in Different Populations

| Population | Prevalence (%) |
|---|---|
| Children | |
| Boys | Less than 1 |
| Girls | 1 to 2 |
| Healthy women | |
| Premenopausal | 1 to 5 |
| Pregnant | 1.9 to 9.5 |
| Postmenopausal (50 to 70 years of age) | 2.8 to 8.6 |
| People with diabetes mellitus | |
| Women | 10.8 to 16 |
| Men | 0.7 to 11 |
| Older adults in long-term care facilities | |
| Women | 25 to 50 |
| Men | 15 to 50 |
| People with spinal cord injury | |
| Intermittent catheter use | 23 to 69 |
| Sphincterotomy/condom catheter | 57 |
| People with kidney transplant | |
| First month posttransplant | 23 to 24 |
| One month to one year posttransplant | 10 to 17 |
| More than one year posttransplant | 2 to 9 |
| People with an indwelling catheter | |
| Long term (30 days or more) | 100 |
| Short term (less than 30 days) | 3 to 5 per day the catheter is present |
Adapted with permission from Nicolle LE, Gupta K, Bradley SF, et al. Clinical practice guideline for the management of asymptomatic bacteriuria: 2019 update by the Infectious Diseases Society of America. Clin Infect Dis. 2019;68(10):e87.
Diagnosis
Asymptomatic bacteriuria is diagnosed when one bacterial species grows in the urine with at least 100,000 colony-forming units (CFUs) per mL, with or without pyuria, in a patient with no signs or symptoms of UTI.2 In asymptomatic patients with a newly inserted catheter or for specimens collected through in-and-out catheterization, a colony count of at least 100 CFUs per mL indicates asymptomatic bacteriuria. The diagnostic criteria for asymptomatic bacteriuria is summarized in Table 2.2
TABLE 2. Diagnostic Criteria for Asymptomatic Bacteriuria

| Midstream clean-catch urine in patients without indwelling catheters or signs and symptoms of UTI Women: two consecutive specimens, preferably within two weeks of each other, with one bacterial species isolated in quantitative counts of at least 100,000 CFUs per mL of urine Men: a single specimen with one bacterial species isolated in a quantitative count of at least 100,000 CFUs per mL of urine |
| Patients with indwelling catheters and no signs or symptoms of UTI Newly inserted catheter or in-and-out catheterization: in women or men, a single specimen with one bacterial species isolated in a quantitative count of at least 100 CFUs per mL of urine Long-term catheterization: in women or men, a single specimen with one bacterial species isolated in a quantitative count of at least 100,000 CFUs per mL of urine |
CFUs = colony-forming units; UTI = urinary tract infection.
Information from reference 2.
Screening and Treatment Recommendations
CHILDREN
Asymptomatic bacteriuria is uncommon in children with a normal urinary tract and has not been shown to cause harm. In addition, young children cannot reliably give a clean-catch urine specimen,2 and there is no evidence that treatment of asymptomatic bacteriuria in children prevents symptomatic UTI, pyelonephritis, renal scarring, or renal insufficiency.2 Based on these factors, the IDSA recommends against screening and treating infants and children for asymptomatic bacteriuria.2
NONPREGNANT WOMEN
Asymptomatic bacteriuria in nonpregnant premenopausal women usually resolves spontaneously. Although symptomatic UTI is more likely in these women compared with those who do not have asymptomatic bacteriuria, observational studies do not report increased rates of adverse outcomes such as hypertension, chronic kidney disease, increased serum creatinine levels, and abnormal intravenous pyelogram findings.3 In addition, treatment of asymptomatic bacteriuria does not appear to reduce the incidence of symptomatic UTI or adverse outcomes.4,5 Therefore, the IDSA recommends against screening and treating healthy nonpregnant premenopausal women for asymptomatic bacteriuria.2 For similar reasons, the guidelines also recommend against screening and treating healthy postmenopausal women.
PREGNANT WOMEN
Prospective randomized studies have shown that antimicrobial treatment of asymptomatic bacteriuria decreases the incidence of pyelonephritis in pregnant women with asymptomatic bacteriuria (20% to 35% vs. 1% to 4%).6 Treatment may also reduce the risk of preterm birth and very low birth weight.
The IDSA thus recommends screening for asymptomatic bacteriuria early in pregnancy. When asymptomatic bacteriuria is diagnosed, it should be treated with four to seven days of antimicrobial therapy.2 This recommendation is in agreement with U.S. Preventive Services Task Force recommendations, which are supported by the American Academy of Family Physicians.7–9 Nitrofurantoin and beta-lactam antibiotics (usually ampicillin or cephalexin [Keflex]) are preferred because of their demonstrated safety in pregnant women2 (Table 32,3,10 ). There is not enough evidence to inform a recommendation for or against repeat screening during pregnancy in women with an initial negative screening result or following initial treatment.2
TABLE 3. Oral Antimicrobials for Treatment of Pregnant Women with Asymptomatic Bacteriuria

| Agent* | Comments |
|---|---|
| Amoxicillin | — |
| Amoxicillin/clavulanate (Augmentin) | — |
| Ampicillin | — |
| Cefuroxime axetil | Possible risk of induced abortions based on conflicting human data |
| Cephalexin (Keflex) | — |
| Ciprofloxacin | Risk and benefits should be weighed during pregnancy; no known risk of teratogenicity based on human and animal data; possible risk of spontaneous abortion based on conflicting human data |
| Levofloxacin (Levaquin) | Risk and benefits should be weighed during pregnancy; possible risk of spontaneous abortion, although human data are inadequate to fully assess risk |
| Nitrofurantoin | Contraindicated at 38 to 42 weeks' gestation, and alternative should be considered in first trimester (otherwise may use during pregnancy); possible risk of teratogenicity and hemolytic anemia based on conflicting human data; dose-dependent risk of teratogenicity |
| Sulfamethoxazole/trimethoprim | Alternative therapy should be considered in the first trimester. Caution is advised for use in the third trimester because there is a risk of kernicterus near term based on human data |
*—May use during pregnancy; possible risk of teratogenicity based on conflicting human data; and no known risk of fetal harm based on animal data, unless otherwise noted.
PATIENTS WITH FUNCTIONAL IMPAIRMENT LIVING IN THE COMMUNITY OR LONG-TERM CARE FACILITIES
A causal relationship between asymptomatic bacteriuria and delirium (acute mental status change with fluctuating level of confusion and orientation) has not been established, and treatment of asymptomatic bacteriuria in patients with delirium has not been shown to have any beneficial effect on clinical outcomes compared with no treatment.2 Thus, for older patients with functional or cognitive impairment and bacteriuria but no systemic signs of infection (e.g., genitourinary symptoms, fever, hemodynamic instability) who experience delirium or a fall, the IDSA recommends assessment for other causes of delirium with careful observation, rather than antimicrobial treatment.2,11–13 In those with systemic signs of infection or hemodynamic instability consistent with sepsis syndrome for whom another source of infection is not identified, antimicrobials may be indicated for potential infection, such as a UTI, pending culture results.
PATIENTS WITH DIABETES MELLITUS
The IDSA recommends against screening and treating patients with diabetes for asymptomatic bacteriuria.2 There is no evidence that antimicrobial treatment of asymptomatic bacteriuria reduces the risk of symptomatic UTI, including pyelonephritis, in people with diabetes.2,14–16
PATIENTS WITH SPINAL CORD INJURIES
Clinical signs and symptoms of UTI in patients with spinal cord injuries may differ from the classic genitourinary symptoms in patients with normal sensation. Symptoms that may indicate a UTI in patients with spinal cord injuries include fever, malaise, lethargy or sense of unease, new or worsening urinary incontinence or leaking around a catheter, spasticity, cloudy urine, malodorous urine, back pain, bladder pain, dysuria, and autonomic dysreflexia (sudden onset of elevated blood pressure).17 In a prospective study of individuals with spinal cord injuries, patients were better at predicting when they did not have a UTI than predicting when they did have a UTI (defined as bacteriuria with a colony count of at least 100,000 CFUs per mL and at least one sign or symptom of UTI).18 In the absence of symptoms, the IDSA recommends against screening and treating patients with spinal cord injuries for asymptomatic bacteriuria.2
PATIENTS WITH INDWELLING CATHETERS
Because of the universal formation of biofilm along an indwelling catheter, all patients with a long-term indwelling catheter will eventually develop bacteriuria.19 Individuals with short-term indwelling catheters (in place for less than 30 days) may not develop bacteriuria before removal of the catheter.2
A UTI is uncommon in patients with long-term or short-term indwelling catheters and bacteriuria.20 Thus, the IDSA recommends against screening and treating these patients for asymptomatic bacteriuria. Whether to screen and treat at the time of catheter removal is a separate area of research, but the evidence is mixed and lacks generalizability, and the IDSA guidelines do not include a recommendation.2
PATIENTS UNDERGOING ENDOUROLOGICAL PROCEDURES
Patients undergoing endourological procedures associated with mucosal trauma (e.g., transurethral surgery; ureteroscopy, including lithotripsy and percutaneous nephrolithotomy) should be screened for asymptomatic bacteriuria before the procedure and treated if positive to avoid serious postoperative UTI-related sepsis.2,21,22 Results of the urine culture and sensitivity testing should be obtained before the procedure, and targeted antimicrobial therapy should be prescribed, rather than using empiric therapy. A short course of antimicrobial therapy (one or two doses) is recommended rather than a longer course and should be initiated 30 to 60 minutes before the procedure.2,21,22 Procedures that do not disrupt the mucosal lining, such as diagnostic cystoscopy, are considered low risk and do not warrant screening or treatment for asymptomatic bacteriuria.
ADDITIONAL CONSIDERATIONS
Several other patient scenarios may arise for which clinicians might consider screening for asymptomatic bacteriuria. The IDSA recommends against screening and treatment for asymptomatic bacteriuria in patients undergoing elective nonurological surgery, patients who have had a kidney transplant more than one month prior, recipients of other solid organ transplants, or those with impaired voiding following spinal cord injury. The IDSA makes no recommendation for or against screening and treating patients with high-risk neutropenia (absolute neutrophil count less than 100 per μL [0.10 × 109 per L] occurring for more than seven days) following cytotoxic chemotherapy.2
This article updates a previous article by Colgan, et al.10
Data Sources: This article reviews the 2019 IDSA guidelines on asymptomatic bacteriuria. The original literature search criteria and data sources are delineated in the guideline.2 We updated the search using the parameters established by the IDSA. We searched PubMed from June 2017 to September 2019 and February 2020; the IDSA's search was from January 2005 to June 2017. Our key search terms were asymptomatic bacteriuria, bacteriuria, urinary tract infection, screening, and treatment. Additional searches for multiple subtitles included the same key terms in addition to pregnancy, renal transplant, diabetes, endourologic surgery, urologic devices, urinary catheter, older adults, nursing home, long-term care, spinal cord injury, neurogenic bladder, falls, and delirium. Systematic reviews of relevant topics were identified using PubMed and the Cochrane Library. Search dates: June 2017 to September 2019, and February 2020.

