Am Fam Physician. 2020;102(6):327-328
Author disclosure: No relevant financial affiliations.
To the Editor: During the coronavirus disease 2019 (COVID-19) pandemic, everyone has been advised to wash their hands more often. The Centers for Disease Control and Prevention recommends handwashing for 20 seconds or using a hand sanitizer with 60% or more alcohol if soap and water are inaccessible.1 Several reports have described cutaneous complications that health care workers have experienced as a result of these enhanced prevention measures.2,3
A 64-year-old patient developed irritant contact dermatitis on the hands following repeated hand-washing with standard dish soap to help reduce the transmission of COVID-19. By day 5, erythematous, eczematous patches were visualized on the dorsal aspects of the hands (Figure 1). The patient reported significant discomfort, prompting the patient to alter handwashing by avoiding the affected areas of the hands. Over-the-counter skin care products were used, including a cream with little benefit and emollients that provided significant relief. Following five days of using emollients and abstaining from washing the dorsal hands, the patient reported complete resolution of symptoms.
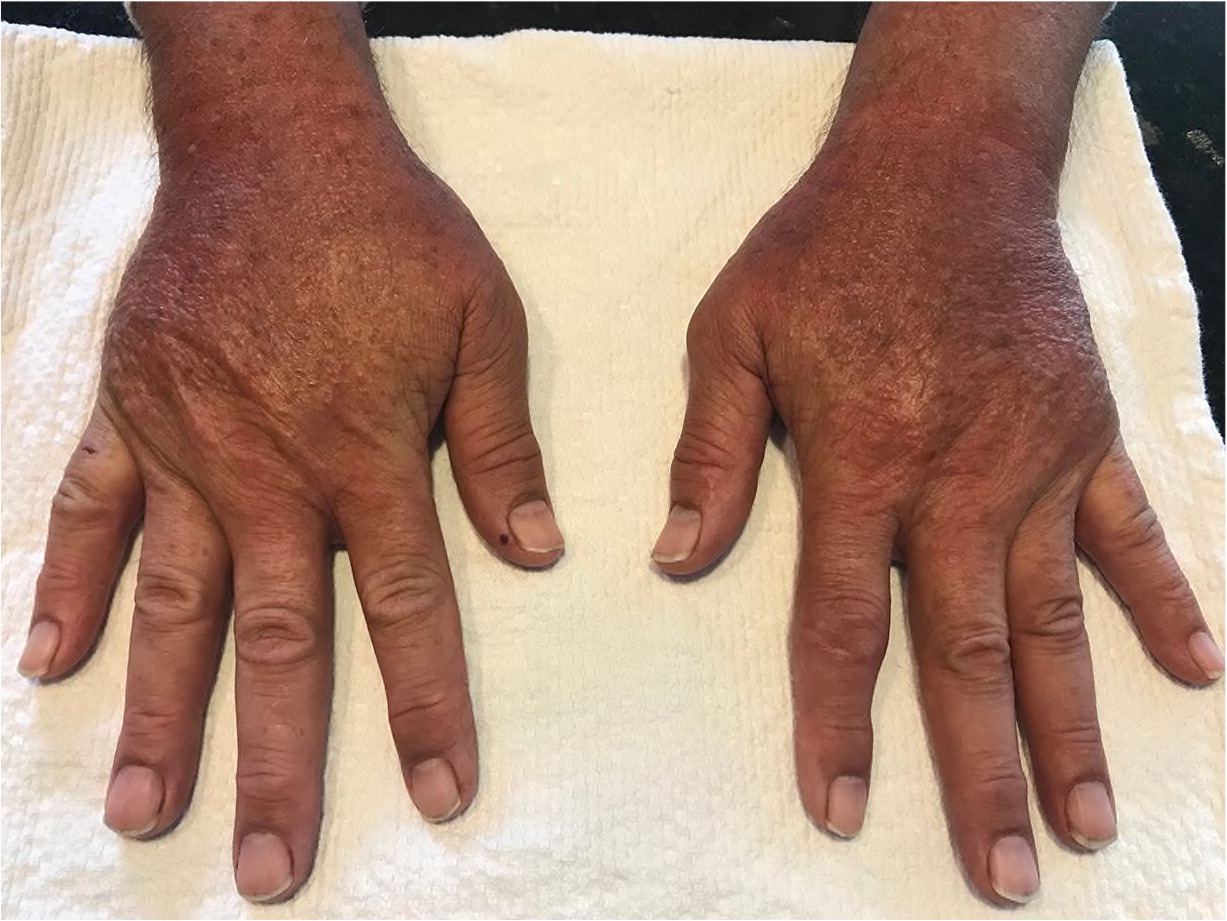
Clinicians need to educate patients and the general public on the prevention of hand dermatitis and effective strategies for symptom management. This education is especially relevant for patients with risk factors, including a history of atopic dermatitis, asthma, tobacco smoking, dry skin, and wet work (e.g., washing dishes, watering plants).4
COVID-19 shows low resistance to disinfectants, such as hand sanitizer.5 Therefore, we recommend the use of hand sanitizers with moisturizing ingredients such as glycerin as an alternative to handwashing with soap.6 If the patient does not have access to hand sanitizer with moisturizer, we recommend the regular use of emollients after each wash with soap and water. At bedtime, patients can apply a thick coat of lipid-rich ointment (such as CeraVe healing ointment, Aquaphor, or even Vaseline petroleum jelly) followed by wearing cotton gloves overnight. Encourage the use of gloves with a cotton liner on dry hands whenever the patient is performing wet work. During a flare-up, an over-the-counter topical corticosteroid is an effective first-line treatment.4 Patients should be advised to avoid hot water (hotter than 122°F [50°C]) because this may exacerbate symptoms. If patients continue to experience significant pain and blistering, referral to a dermatologist is warranted.