
Am Fam Physician. 2020;102(7):403-404
Author disclosure: No relevant financial affiliations.
Clinical Question
What are the sensitivity and specificity of computed tomography (CT) for the diagnosis of acute appendicitis in nonpregnant adults?
Evidence-Based Answer
In a nonpregnant adult with clinical signs and symptoms of appendicitis, CT has a sensitivity of 95% and specificity of 94%. Therefore, the probability of having appendicitis following a positive CT result is 92%, and the probability of having appendicitis following a negative CT result is 4%. These conclusions are based on studies of low methodologic quality.1 (Strength of Recommendation: B, based on inconsistent or limited-quality patient-oriented evidence.)
Practice Pointers
The lifetime risk of appendicitis is approximately 10%. The “classic” clinical presentation of periumbilical abdominal pain migrating to the right lower quadrant, loss of appetite, nausea and/or vomiting, fever, and leukocytosis occurs in approximately 50% of patients. Before widespread use of diagnostic imaging, the acceptable negative appendectomy rate (i.e., no appendicitis found intraoperatively) was 10% in young, otherwise healthy male patients and approximately 20% in female patients. With the use of imaging (mostly CT), the negative appendectomy rate has decreased to around 8% regardless of a patient's sex or age.2
The findings of this Cochrane review were based on 64 studies that included 71 separate study populations in 22 countries (30 studies were performed in the United States) with a total of 10,280 participants (55% women; median age of 33 years). Included studies were prospective and had at least 10 nonpregnant patients older than 14 years who presented to the emergency department with suspected appendicitis based on history, physical examination, and/or laboratory testing. No studies compared antibiotic therapy with surgery. The reference standard for diagnosing appendicitis was histologic examination of the resected appendix or intraoperative findings consistent with appendicitis if histology was not available.
Among the patients in this analysis (i.e., those seen in the emergency department whose initial history and workup led to CT), 43% had appendicitis. This analysis demonstrates that CT is a good screening test (sensitivity = 95%; 95% CI, 72% to 100%) and a good confirmatory test (specificity = 94%; 95% CI, 50% to 100%). Using normalized frequencies, if 1,000 patients presented to the emergency department with possible appendicitis based on history, physical examination, and laboratory findings, the CT results of 443 of these patients would further suggest this diagnosis. However, if each of those 443 patients went to surgery, 35 would not have appendicitis. Of the 557 patients whose CT results did not suggest appendicitis, 22 would ultimately have the condition.
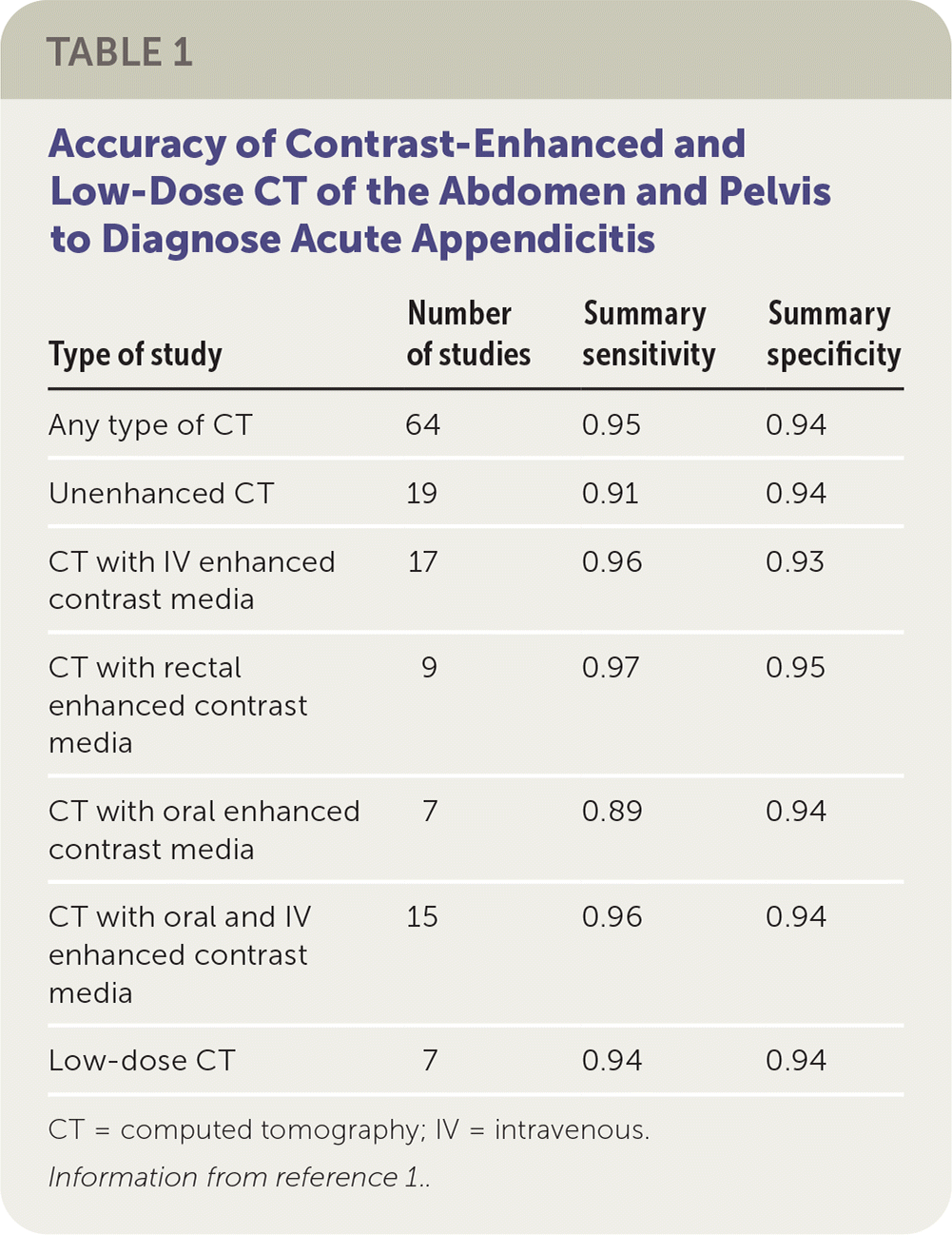
The secondary aim of this review was to determine how the use of contrast in both conventional and low-dose protocols affected accuracy (Table 1).1 Unenhanced, standard-dose CT and CT with use of oral contrast alone appeared to be slightly less sensitive than standard-dose CT with rectal, intravenous, or oral plus intravenous contrast enhancement; however, they would each have similar specificity. Low-dose vs. standard-dose CT had equivalent sensitivity and specificity (Table 1).1
| Type of study | Number of studies | Summary sensitivity | Summary specificity |
|---|---|---|---|
| Any type of CT | 64 | 0.95 | 0.94 |
| Unenhanced CT | 19 | 0.91 | 0.94 |
| CT with IV enhanced contrast media | 17 | 0.96 | 0.93 |
| CT with rectal enhanced contrast media | 9 | 0.97 | 0.95 |
| CT with oral enhanced contrast media | 7 | 0.89 | 0.94 |
| CT with oral and IV enhanced contrast media | 15 | 0.96 | 0.94 |
| Low-dose CT | 7 | 0.94 | 0.94 |
The results were based on studies of low methodologic quality. Major methodologic problems were poor reference standards and inadequate follow-up for those who did not have surgery. The comparisons between types of contrast enhancement and radiation dose may have been unreliable because they were based on indirect comparisons that may have been confounded by multiple other factors. This testing is not without risk; the estimated increased lifetime risk of cancer from one abdominopelvic CT is as high as 0.14%.3
According to the American College of Radiology (ACR) Appropriateness Criteria for right lower quadrant pain–suspected appendicitis, abdominal and pelvic CT with intravenous contrast is “usually appropriate” (highest rating) whereas an abdominal and pelvic CT without intravenous contrast “may be appropriate” (middle rating).2 The results of this Cochrane review are consistent with the ACR decision-support recommendations.
The practice recommendations in this activity are available at http://www.cochrane.org/CD009977.
The views expressed in this article are those of the author and do not necessarily reflect the official policy or position of the Uniformed Services University of the Health Sciences, the Department of Defense, or the U.S. government
