
Am Fam Physician. 2021;103(12):755-756
Author disclosure: No relevant financial affiliations.
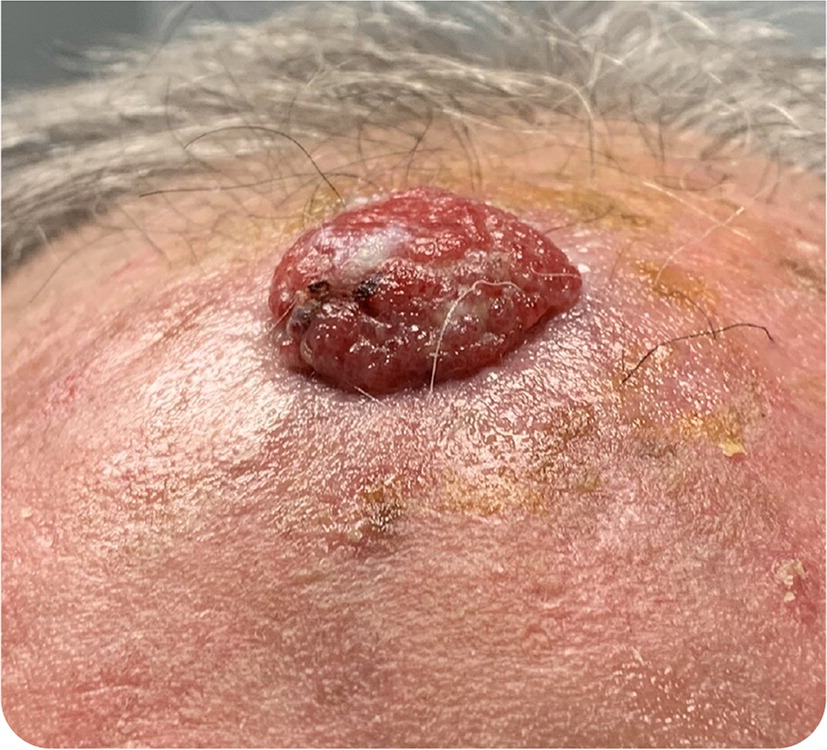
A 79-year-old patient presented with a lesion on the scalp, which they noticed one month earlier because of a short episode of bleeding. The lesion was asymptomatic but enlarged rapidly. There was no improvement with topical antibiotics. The patient had a history of coronary artery disease and hypertension but no history of malignancy.
Physical examination revealed a 2-cm, fleshy, erythematous, round, exophytic nodule over the frontal scalp (Figure 1).
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Amelanotic melanoma.
B. Angiosarcoma.
C. Cutaneous metastasis.
D. Keratoacanthoma.
E. Porocarcinoma.
Discussion
Answer is E: porocarcinoma. Eccrine porocarcinoma is a rare eccrine gland tumor that accounts for 0.005% to 0.01% of all cutaneous tumors.1 The disease is most prevalent in adults 50 to 80 years of age.1 The pathogenesis of porocarcinoma is not fully understood. The lesion may develop from eccrine poromas (porocarcinoma's benign counterpart) through various triggers, including chronic actinic damage.2
Clinically, a porocarcinoma typically presents as an asymptomatic erythematous nodule. 3 The lesion most commonly appears on the lower extremities but may occur anywhere on the body, including the scalp.1 Porocarcinomas may be aggressive with distant metastasis. A history of bleeding, rapid growth, pain, or pruritus may indicate a more aggressive clinical course.3 Histologically, eccrine porocarcinomas typically appear as broadly anastomosing bands of epithelial downgrowths composed of small pleomorphic atypical epithelioid cells, conspicuous mitotic activity, ductal differentiation, and increased dilated blood vessels in the dermis.1,2
Although no standard of care has been established, a recent systematic review recommends imaging to rule out metastasis in patients with porocarcinomas on the extremities, buttocks, or genitalia and in those with worrying clinical features.1 A wide local excision with 2- to 3-cm margins is first-line therapy for eccrine porocarcinomas.1 Mohs micrographic surgery has also been shown to be an appropriate treatment and may have a lower local recurrence rate and reduced rates of metastasis than wide local excision.1
Amelanotic, or hypomelanotic, melanoma may be difficult to diagnose because the lack of pigment inhibits use of color criteria in its detection.4 This uncommon form of melanoma has been described in all histologic melanoma subtypes and typically presents as a rapidly growing, skin-colored to red papule or nodule on chronically sun-exposed skin in older patients. It may bleed or ulcerate. Amelanotic melanoma has a poorer prognosis than pigmented forms, possibly because of diagnostic delay.
Angiosarcomas are rare aggressive soft tissue vascular neoplasms that commonly present as rapidly growing bruises, blue-black nodules, or unhealing ulcerations on the heads of older men.5 Bleeding or pain may be present.
As a late manifestation of visceral carcinoma, cutaneous metastasis is uncommon and may occur because of direct extension of the tumor or as local or distant metastasis.6 In most cases, cutaneous metastasis occurs after the initial diagnosis and is associated with advanced disease and poor prognosis. The scalp is a common metastatic site, possibly because of the abundant blood supply, immobility, and warmth of the region. It may present as a rapidly growing, skin-colored or red nodule or nodules, with or without ulceration, and may mimic primary benign and malignant skin tumors.
Keratoacanthoma is a common epithelial neoplasm that closely resembles cutaneous squamous cell carcinoma.7 Some support classifying keratoacanthomas as squamous cell carcinoma. A keratoacanthoma typically presents as a rapidly growing keratotic nodule with a central crater that enlarges over a few weeks to months. In most cases, this is followed by spontaneous resolution over four to six months, but some are more aggressive and do not spontaneously resolve.
| Condition | Characteristics |
|---|---|
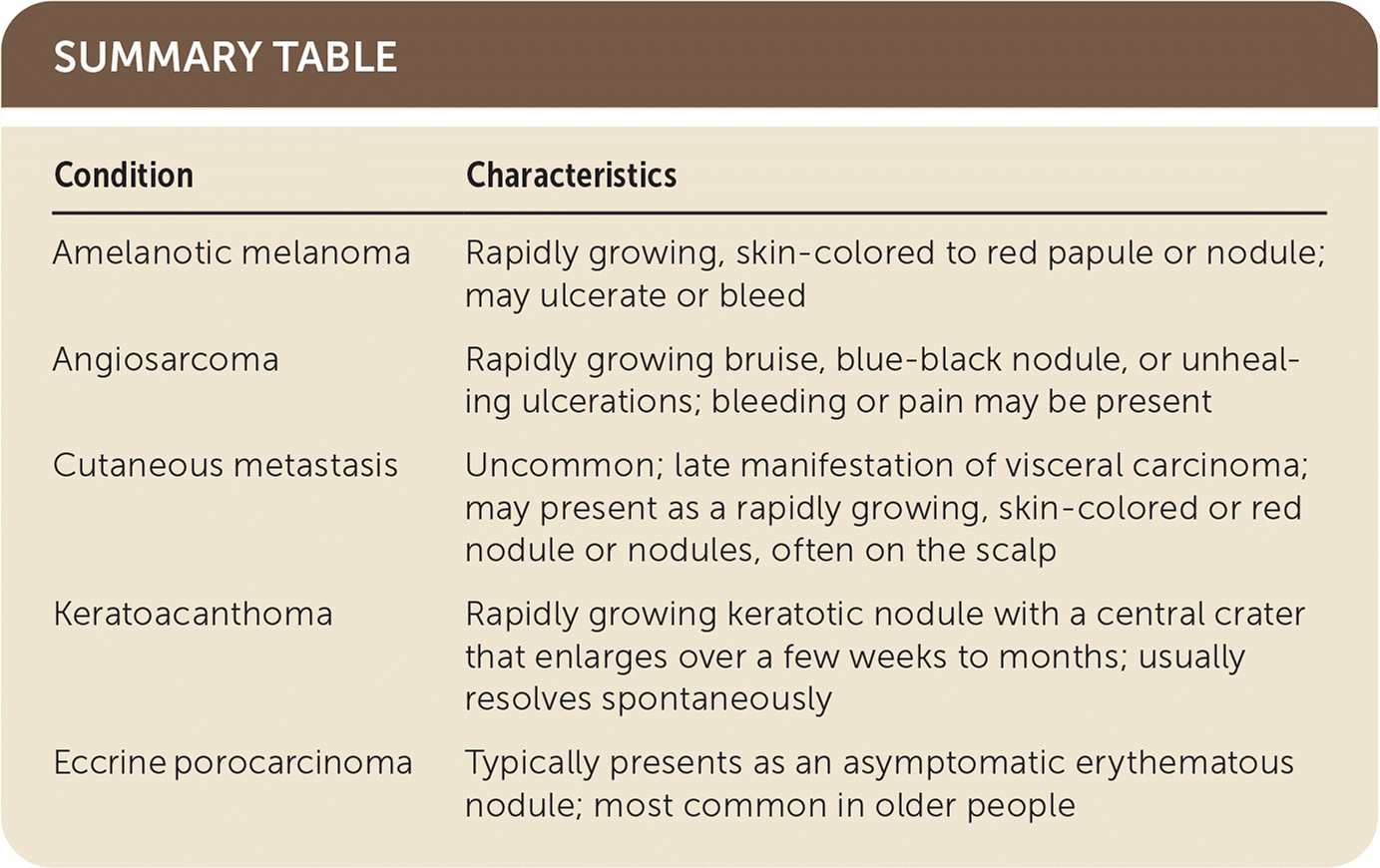
| Amelanotic melanoma | Rapidly growing, skin-colored to red papule or nodule; may ulcerate or bleed |
| Angiosarcoma | Rapidly growing bruise, blue-black nodule, or unhealing ulcerations; bleeding or pain may be present |
| Cutaneous metastasis | Uncommon; late manifestation of visceral carcinoma; may present as a rapidly growing, skin-colored or red nodule or nodules, often on the scalp |
| Keratoacanthoma | Rapidly growing keratotic nodule with a central crater that enlarges over a few weeks to months; usually resolves spontaneously |
| Eccrine porocarcinoma | Typically presents as an asymptomatic erythematous nodule; most common in older people |
