
Am Fam Physician. 2021;104(2):201-202
Author disclosure: No relevant financial affiliations.
A 54-year-old patient presented with stiffness and pain in the lower back and both thighs. The pain was worse when sitting and lying down, but there was no pain when standing. The patient described the pain as compression in the flanks that radiated to the right groin and both lateral thighs.
The patient had urinary hesitancy but no trauma, fever, weight loss, or blood in the urine. Symptoms were not relieved with ibuprofen and cyclobenzaprine. The medical history was significant for renal stones and gastroesophageal reflux. The patient had no history of back problems or repetitive lifting.
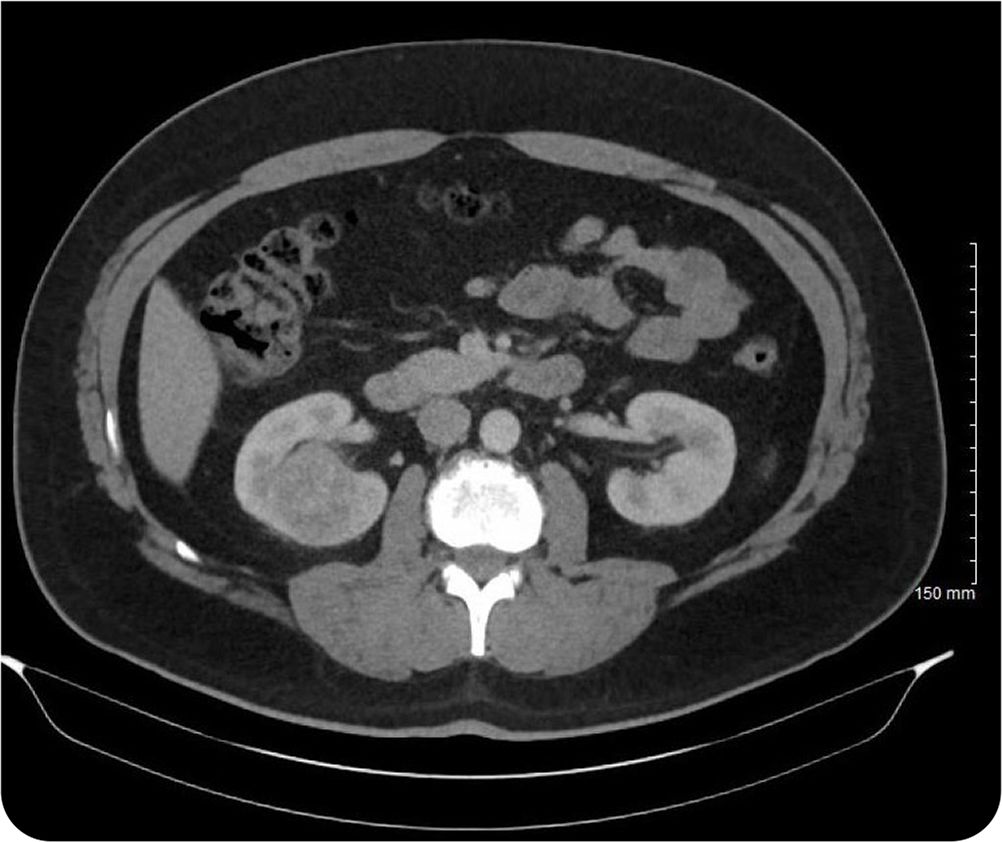
Physical examination revealed normal motor strength in the lower extremities and negative findings on the straight leg raise test. There was tenderness on palpation of the right flank. Results of a point-of-care urinalysis were normal. Prostate-specific antigen was mildly elevated at 5.84 ng per mL (5.84 mcg per L). Computed tomography (CT) of the abdomen was performed (Figure 1).
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Angiomyolipoma.
B. Metanephric adenoma.
C. Oncocytoma.
D. Renal abscess.
E. Renal cell carcinoma.
Discussion
The answer is E: renal cell carcinoma. Renal cell carcinoma is often an incidental finding until the tumor enlarges to an advanced size. Presenting symptoms vary and include hematuria, abdominal pain, or a palpable mass. The likelihood of renal cell carcinoma is higher when all three of these symptoms are present (the classic triad). Approximately 80% to 85% of tumors in the renal cortex are renal cell carcinomas. In these cases, paraneoplastic symptoms may develop because of the production of ectopic hormones such as erythropoietin, parathyroid hormone–like protein, gonadotropins, chorionic somatomammotropin, adrenocorticotropic hormone–like substance, renin, glucagon, and insulin.1
The diagnostic workup for renal cell carcinoma includes CT or ultrasonography, although ultrasonography is less sensitive. Magnetic resonance imaging can be used in some patients. In this patient, CT identified a mass in the right kidney measuring 3.8 cm × 4.0 cm × 3.5 cm. Resection is necessary if imaging studies cannot differentiate benign renal lesions from carcinoma. Tissue biopsy of the mass can establish the diagnosis of malignancy and identify the histopathologic type. Clear cell subtypes, as in this patient, account for up to 75% of cases.2
Angiomyolipoma is a benign renal tumor that can grow to impair renal function. It is strongly associated with tuberous sclerosis, a multisystem autosomal dominant genetic disease, and lymphangioleiomyomatosis. On histology, angiomyolipomas are composed of blood vessels, smooth muscle cells, and fat cells. Patients may be asymptomatic, but rupture of involved blood vessels can result in retroperitoneal hemorrhage accompanied by nausea and vomiting.3
Metanephric adenomas are rare, benign renal lesions. They are more common in women than men (2:1).4 Signs and symptoms may include hematuria, flank pain, and a palpable mass. They can be misidentified on CT as renal cell carcinoma or an epithelial Wilms tumor. Metanephric adenomas are more calcified than other renal tumors. Histopathology reveals small epithelial cells that form small acini in an acellular stroma.
Oncocytoma is a benign tumor composed of large epithelial cells rich in granular eosinophilic cytoplasm and excessive numbers of mitochondria. Renal oncocytoma primarily arises from intercalated cells of the collecting ducts in the kidney. Renal oncocytoma is usually asymptomatic, although hematuria, flank pain, and an abdominal mass may be present. Less than 5% of surgically resected renal neoplasms are oncocytomas.5
Renal abscesses arise from an infectious source and are usually associated with pyelonephritis. They may also be associated with diabetes mellitus, pregnancy, and urinary tract abnormalities. Renal abscesses are pus-filled pockets that appear as hypodense regions on contrast-enhanced CT.6 Symptoms may include fever, vague lumboabdominal pain, pallor, fatigue, sweating, and weight loss.
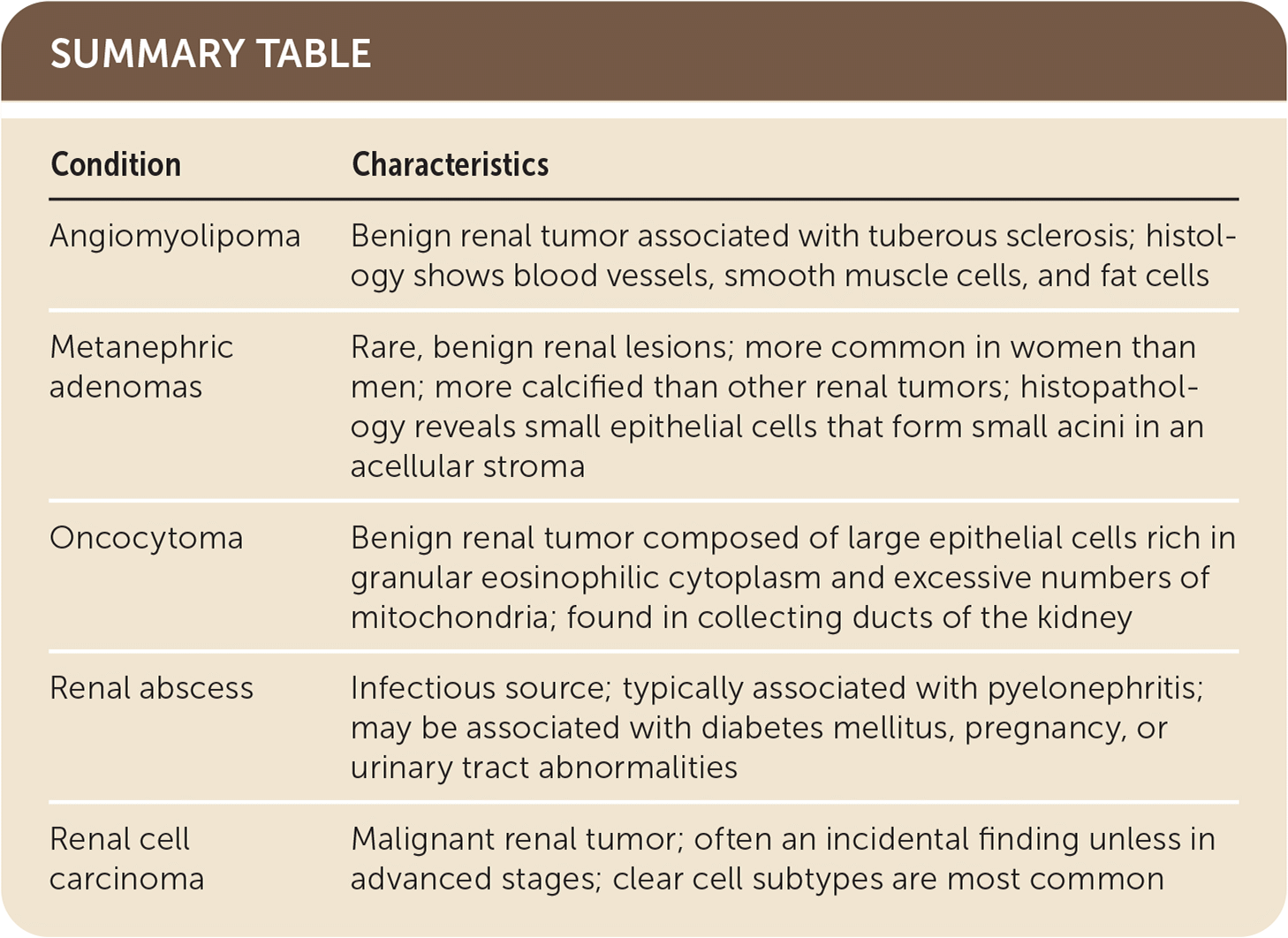
| Condition | Characteristics |
|---|---|
| Angiomyolipoma | Benign renal tumor associated with tuberous sclerosis; histology shows blood vessels, smooth muscle cells, and fat cells |
| Metanephric adenomas | Rare, benign renal lesions; more common in women than men; more calcified than other renal tumors; histopathology reveals small epithelial cells that form small acini in an acellular stroma |
| Oncocytoma | Benign renal tumor composed of large epithelial cells rich in granular eosinophilic cytoplasm and excessive numbers of mitochondria; found in collecting ducts of the kidney |
| Renal abscess | Infectious source; typically associated with pyelonephritis; may be associated with diabetes mellitus, pregnancy, or urinary tract abnormalities |
| Renal cell carcinoma | Malignant renal tumor; often an incidental finding unless in advanced stages; clear cell subtypes are most common |
