Am Fam Physician. 2021;104(4):332-333
Author disclosure: No relevant financial affiliations.
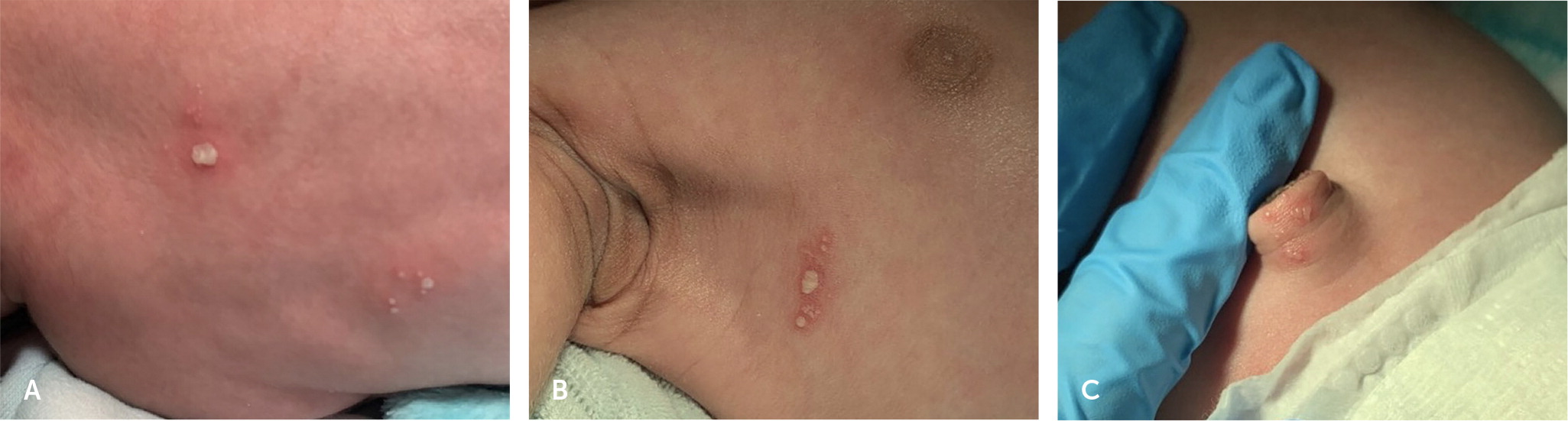
To the Editor: A 12-day-old infant with no significant birth history presented with several 1-mm grouped pustular lesions on erythematous bases on the back and right axilla, and vesicular lesions on the umbilicus (Figure 1). The patient looked well, and vital signs were within normal limits. There were no other symptoms or parental concerns. A physical examination was otherwise unremarkable. Complete blood count, metabolic panel, and urine analysis results were within normal ranges. The erythrocyte sedimentation rate was mildly elevated at 26 mm per hr (reference range = 0 to 10 mm per hr). Swabs were collected for a bacterial culture and herpes simplex virus (HSV) polymerase chain reaction (PCR). A Tzanck test was performed, which found multi-nucleated giant cells and viral cytopathic effect. A lumbar puncture was performed, and cerebrospinal fluid studies showed a mildly elevated protein of 65 mg per dL (reference range = 15 to 45 mg per dL) with no pleocytosis. The patient was admitted to the hospital and administered empiric ampicillin, ceftazidime (Fortaz), and acyclovir.
Urine, blood, and lesion cultures had no bacterial growth after 48 hours. The HSV PCR of skin and plasma was positive for HSV-1. HSV-1 and HSV-2 were not detected in the PCR of cerebrospinal fluid. The patient completed a 14-day course of intravenous acyclovir and was discharged with oral suppression therapy.
Neonatal HSV infections are classified into three subtypes: localized with skin, eye, or mouth disease; localized central nervous system disease; and disseminated multi-organ involvement. 1 Skin, eye, or mouth disease presents at 10 to 11 days after birth with groups of discrete vesicles on erythematous bases. These lesions coalesce into clusters, differentiating this infection from erythema toxicum neonatorum.2
A skin examination revealed grouped vesicles on the umbilicus, which are morphologically different from the more typical HSV lesions of grouped pustules on an erythematous base found in other areas. Early diagnosis of neonatal HSV and adequate antiviral treatment have lowered the percentage of patients with a developmental delay because of skin, eye, or mouth disease from 25% to less than 2%.3
Tzanck smear with Giemsa stain is an inexpensive test for rapid detection of HSV infection. Although the Tzanck test has lower sensitivity than PCR, a positive Tzanck smear with multinucleated giant cells and viral cytopathic changes is 100% specific for HSV infection.4 For this patient, a Tzanck smear expedited the initiation of anti-viral therapy before PCR results were available.
The authors thank Dr. Jeremy D. Jackson for oversight and comment on the Letter to the Editor.