Am Fam Physician. 2021;104(4):351-352
Author disclosure: No relevant financial affiliations.
In 2016, for the first time, less than one-half of practicing physicians had an ownership stake in their own practices.1 The most recent American Medical Association Physician Practice Benchmark Survey reveals that this trend continues.2 More physicians are identifying as employees instead of owners, with family physicians being the second most likely specialty to be employed. This trend has significant implications for reimbursement and practice patterns, and potential impacts on physician burnout if scope is limited by employers.2,3
The Robert Graham Center, in conjunction with researchers at the American Board of Family Medicine and IBM Watson Health, examined employment trends in the report “Primary Care in the United States, A Chartbook of Facts and Statistics.” 4 Employment status of primary care physicians was analyzed using 2016 National Ambulatory Medical Care Survey data (Figure 1). Slightly less than one-half (49%) of primary care physicians owned their own practices. Most working physicians were employees of a non–physician-owned practice.
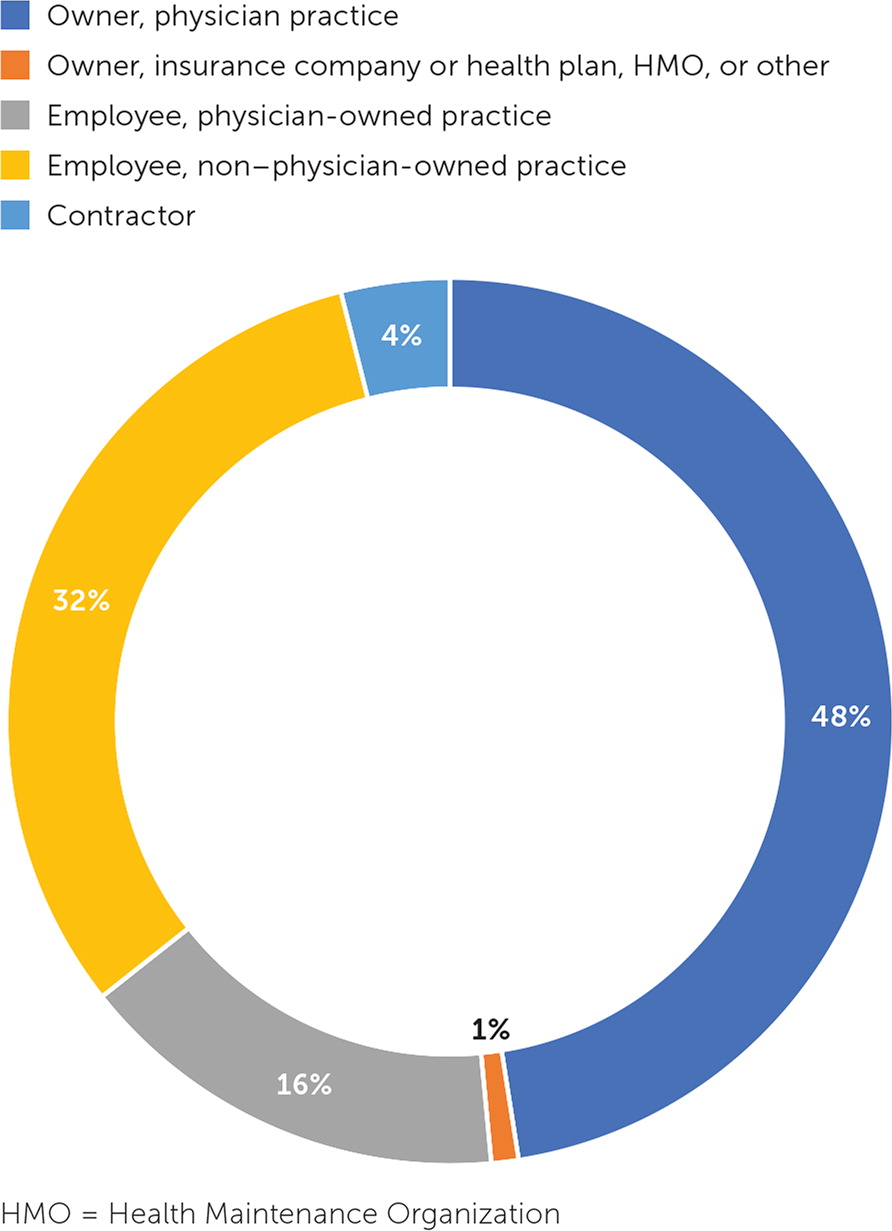
The increasing percentage of employed physicians may be due to a variety of factors, including greater financial stability.5 Younger physicians are also reported to be less attracted to the entrepreneurial aspect of private practice ownership.6 Although these trends may reflect financial and lifestyle decisions, the implications of a largely employed primary care workforce are not necessarily positive. For example, employers in multispecialty practices could be defining or limiting the scope of practice of their physicians, which has implications for training, physician satisfaction, and health care costs.3,7
The impact of employment status on health care quality is still unclear. Some studies suggest that it has no relationship to health care quality.2 Other studies show that primary care ownership is associated with less use of quality improvement process measures in comparison with federally qualified health centers and hospital-owned practices.8,9 In addition, hospital-owned practices demonstrated greater use of evidence-based chronic care management processes, which may improve care coordination.9
Although there are benefits to choosing employment instead of ownership, the disadvantages for primary care physicians and their patients may be significant and are worth further exploration.