
Fam Pract Manag. 1998;5(3):30-33
AMA seeks more input about documentation guidelines
The Health Care Financing Administration (HCFA) has agreed to a process proposed by the AMA that could result in additional changes in the revised documentation guidelines for evaluation and management (E/M) services. The revised guidelines, which were developed by HCFA and the AMA and released in 1997, are scheduled to take effect July 1. During the current grace period, physicians may follow either the revised guidelines or the original guidelines, which were released in 1994.
AMA and HCFA officials met in January, a month after the AMA House of Delegates fell one vote shy of moving to rescind the guidelines. In a February letter to AMA members, AMA President Percy Wootton, MD, wrote that HCFA agreed to a “proposed process for fixing documentation problems” during the current grace period.
The AMA has subsequently invited national, state and local medical associations and specialty societies to submit comments and suggestions for improving the guidelines. The AMA CPT Editorial Panel will consider the suggestions at its March and August meetings, and the AMA plans to convene an April meeting for specialty society and state medical association leaders to review the suggestions and proposed solutions.
Look for more information on these developments over the next several months in Family Practice Management.
Company takes new tiered approach to drug co-payments
United HealthCare Corp., based in Minneapolis, recently introduced a tiered co-payment system for its 1998 preferred drug list (PDL). Under the “incented co-payment” option, a health plan member might pay $5 for generic drugs, $10 for brand-name products on the PDL and $25 for brand-name products not on the PDL. A similar option is available for members of United HealthCare's Medicare plans. The 1998 PDL comprises 800 prescription medicines, 70 percent of which are brand-name pharmaceuticals.
Pharmacy benefit costs for many managed care companies are rising at a rate of 15 percent to 18 percent, according to Eric Bergen, vice president of pharmacy management for United HealthCare. “With the new PDL and the incented co-payment option, we help make sure members have access to all of a plan's covered medicines while reducing the strain on their pocketbooks,” Bergen says.
Quote. End quote.
“First, do nothing.”
The “Hippocratic oath” of HMO Black, a bogus HMO organized by professors at the Massachusetts Institute of Technology and Harvard Medical School who hope to use humor to point out the “ludicrous and dangerous” aspects of managed care.
Business groups trying to stop patients' rights bills
As proposals to protect the rights of patients in managed care plans circulate around Capitol Hill, a business coalition has launched a $1 million advertising campaign to turn public opinion against such legislation.
President Clinton has called on Congress to pass a health care bill of rights, including guarantees of broader access to specialists, emergency services and meaningful appeals processes. From the other side of the aisle, Rep. Charlie Norwood, R-Ga., has proposed even tougher regulation of managed care organizations (MCOs) in the Patient Access to Responsible Care Act.
The coalition of business groups argues that this type of legislation would make health care and health insurance more expensive, thereby forcing employers to cut back on employees' coverage. Coalition members include the National Federation of Independent Business, the Health Insurance Association of America, the American Association of Health Plans, the U.S. Chamber of Commerce, the National Association of Manufacturers and the Business Roundtable.
A number of states are also considering legislation this year to protect patients' rights under managed care.
While these debates continue, Chicago has become the first city in the nation to regulate MCOs locally. The city's new managed care monitoring office will collect information from health plans about their programs, publish a consumer guide to local MCOs, provide a consumer help line, investigate consumers' complaints and refer complaints to the Illinois Department of Insurance. The services are expected to be available by the end of the year.
Minorities lead drop in applications to U.S. medical schools
The number of applicants to U.S. medical schools declined last year for the first time in four years. According to Facts: Applicants, Matriculants and Graduates, 1991–1997, published by the Association of American Medical Colleges (AAMC), the overall applicant rate dropped 8.4 percent in 1997. AAMC President Jordan J. Cohen, MD, attributes this decline, in part, to the elimination of affirmative action in California, Texas, Mississippi and Louisiana.
Medical schools in these states experienced a 17 percent decline in applications from minorities residing in-state, and the acceptance rate for these applicants plunged 27 percent. In contrast, the number of minorities residing and applying to medical schools in all other states decreased by 7 percent.
“This is an ominous sign for the medical community and our nation, which badly needs a physician workforce that is both diverse and reflective of our society as a whole,” says Cohen. “We find it particularly alarming that a large percentage of under-represented minorities are ... choosing not to pursue careers in medicine at all.”
Health benefit costs expected to rise, despite managed care
Last year, as managed care enrollment hit an all-time high of 85 percent of all U.S. employees, health care benefit costs were kept in check, growing just 0.2 percent. But this year, with managed care enrollment still growing, health care benefit costs are expected to rise noticeably, perhaps by 7 percent, according to the 12th annual Mercer/Foster Higgins National Survey of Employer-Sponsored Health Plans.
The survey points out that while more employees are choosing managed care plans over costly indemnity plans, they are opting for managed care's more expensive options: PPOs and point-of-service (POS) plans. Together, these plans enroll 55 percent of employees. Another 15 percent are in indemnity plans; the remaining 30 percent are enrolled in closed-panel HMOs, the least costly option of all. Even the strictest HMOs, though, seem to be taking on attributes of their more expensive counterparts. According to the survey, 12 percent of HMOs offered some sort of open-access option, in which patients are allowed to see subspecialists without referrals.
Also of note, the survey found that greater patient choice translated into higher costs for POS plans. When at least 20 percent of member services were delivered by providers outside the POS plan's network, health benefit costs rose an average of $289 per employee.
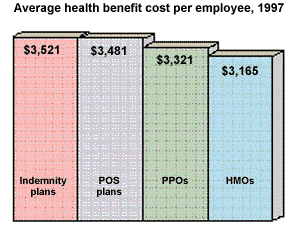
Source: Mercer/Foster Higgins National Survey of Employer-Sponsored Health Plans, 1997.