
Fam Pract Manag. 1999;6(1):17-18
Y2K update: Millennium bug isn't just HCFA's problem
Although much attention has focused on whether HCFA's computers will be ready for the year 2000, practices should remember that it takes two to complete a Medicare transaction, says one HCFA official.
“Doctors need to be testing their own billing systems to make sure they can generate bills to their Medicare carriers and other third-party payers in January 2000,” says Joe Tilghman, administrator of HCFA's region VII, which includes Nebraska, Kansas, Missouri and Iowa. “Our goal is to ensure that providers continue to get paid in a timely and accurate fashion. We're on track to do just that with our own computer systems and those of our contractors. But the providers need to examine their own systems and take whatever steps are necessary to make sure they will function in January 2000.”
For Medicare fee-for-service carriers and intermediaries, as well as managed care plans contracting with Medicare, the deadline for Y2K compliance was Dec. 31. Tilghman says testing of the entire claim submission, processing and payment system will be ongoing through 1999.
Device database offers compliance updates
Among the potential effects of the year-2000 problem are malfunctions of medical devices and lab equipment. If you'd like to know the Y2K-compliance status of a device or piece of equipment you use, you can search a database of manufacturers on the Food and Drug Administration's web site.
The database is updated as the FDA receives new information. But keep in mind that the manufacturers report their products' compliance information, and the FDA doesn't guarantee the accuracy of their reports.
HMO lets doctors choose referral physicians
The largest HMO in New Mexico is giving primary care physicians the chance to choose their own referral physicians — and assume greater economic risk — rather than selecting from the health plan's referral list.
Under the new system, “physician- directed teams” (e.g., groups and IPAs) contracting with Presbyterian Health Plan will have the option of subcapitating their referrals: Each team will receive a budget from the plan based on the number of members it serves; then the team will contract with the referral physicians of its choice, paying them from that budget. The plan no longer will require that these physicians' referrals be authorized.
The arrangement gives primary care physicians greater control over their referrals, but it doesn't completely remove the administrative hassles related to them. “For years, we've had to live with lists of specialists,” says Weston Sumner, MD, of Sandia (N.M.) Independent Physician Association. “We still have to check lists. We just get to choose who's on the list.”
A matter of trust
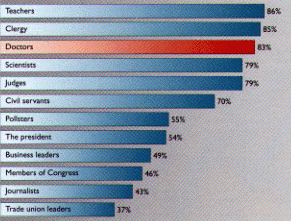
In an industry filled with turmoil and uncertainty, finally there's some good news for physicians. You are among the most trusted professionals in America, nearly tied for top honors with teachers and clergy, according to a recent Harris Poll.
Business leaders, members of Congress and journalists are among those least trusted by the American public. Trade union leaders came in last at just 37 percent.
Percentage of Americans who said they would trust certain professionals to tell the truth
Groups call for patient privacy improvements
Patients' concerns about the privacy of their medical records, which may lead them to withhold vital information from their physicians, could “seriously threaten the quality of health care,” warns a new report from the Joint Commission on Accreditation of Healthcare Organizations and the National Committee for Quality Assurance.
The report, “Protecting Personal Health Information: A Framework for Meeting the Challenges in a Managed Care Environment,” urges the health care community to develop consistent policies and practices for protecting patient confidentiality. The groups' recommendations include obtaining patient consents that are “truly informed, specific and voluntary”; educating patients about their rights and how their health information may be used; improving information systems to offer increased security; and increasing managed care accountability through periodic audits of plans' policies and procedures related to patient confidentiality.
Glossary
Pareto analysis: The act of identifying and focusing on the “important few” — for example, the few problems that are most responsible for poor patient satisfaction in a practice — in order to maximize the returns on quality improvement efforts.
Unbundling: The generally prohibited practice of billing separately for individual components of a service or procedure that are normally billed under a single charge.
National health care spending slows ...
Overall health care spending has seen its slowest annual increase in roughly 40 years, says a report released in November by HCFA. National health care spending increased 4.8 percent in 1997, reaching $1.1 trillion overall or just under $4,000 per person.
Despite the report's good news, HCFA projects that, by the year 2007, public health spending will nearly double, to $2.1 trillion.
... with help from Medicare, Medicaid
Spending growth for public health care programs, primarily Medicare and Medicaid, slowed again in 1997, for the third year in a row. But public health care spending is still growing faster than spending for privately funded health care.
According to HCFA, public health care spending grew at a rate of 5.3 percent in 1997, one percentage point higher than the rate of growth in private health care spending.
Medicare spending, which totaled $214.6 billion, grew at a rate of 7.2 percent in 1997, down from 8.1 percent in 1996. In contrast, Medicaid spending increased only 3.8 percent in 1997, the slowest growth rate in Medicaid's nearly 30-year history. HCFA attributes this low growth rate to decreases in Medicaid enrollment from 1995 to 1997 as well as reductions in per-enrollee spending.
Public programs continue to pay for an increasing percentage of all U.S. health care. Since 1990, the proportion of health care spending from public sources has risen from 40.5 percent to 46.4 percent in 1997.
Annual percentage growth in public and private health care spending

HCFA. Highlights, national health expenditures, 1997. Available at: http://www.hcfa.gov/stats/nhe-oact/hilites.htm. Accessed Nov. 25, 1998.
HCFA. National health expenditures, table 1. Available at: http://www.hcfa.gov/stats/nhe-oact/tables/t09.htm. Accessed Nov. 25, 1998.
Physicians fare well, despite managed care
Despite the squeeze of managed care in recent years, physicians' incomes have grown faster than those of the average American worker.
A Kaiser Family Foundation analysis of data from the American Medical Association and the U.S. Bureau of the Census shows that, from 1985 to 1996, physicians' median net income grew 77 percent, from $94,000 to $166,000 (the analysis did not provide information by specialty). Meanwhile, median net income for all full-time American workers grew 43 percent, from $17,836 to $25,480.
Four family physicians go to Washington
When the 106th Congress convenes this month in Washington, four family physicians will be among its members, all serving in the U.S. House of Representatives.
Ernest Fletcher, MD (R-Ky.), is the newest family physician on board, elected in November. Delegate Donna M. Christian-Green, MD (D-Virgin Islands), and Vic Snyder, MD (D-Ark.), were elected to the House in 1996 and will be serving their second terms. Tom Coburn, MD (R-Okla.), returns to the House for his third term; he was first elected in 1994.