
The quality of your care is linked to the quality of your care process. A practice ‘blueprint’ can show you ways to improve.
Fam Pract Manag. 1999;6(6):45-47
Today's emphasis on quality and continuous improvement is different from what we've seen in the past. In an increasingly competitive and complex health care environment, physicians must meet the demands of federal agencies, professional associations, accrediting bodies and insurance companies, particularly managed care organizations — all with their own quality standards and outcome measures.
As you try to satisfy the various requirements of these third parties, which often involves tremendous amounts of paperwork documenting that you adhered to their standards, it is easy to lose sight of the patient's perspective on care. Although most patients are not in a position to evaluate the quality of their care from a medical perspective, they can provide useful information about how their care was delivered. In fact, the way physicians deliver care, or the care process, is significant because there is an important link between how care is provided and what health outcomes are achieved. An effective way to assess this process is to develop a practice blueprint, or flow diagram.
What is a practice blueprint?
A practice blueprint uses patient, staff and physician input to construct a picture of the process patients go through as they receive care, from making an appointment to exiting the physician's office (perhaps also including off-site testing and referrals). The diagram also traces steps that patients do not see, such as the billing cycle and telephone calls made by nurses to arrange referrals.
The blueprint show below represents a typical visit to a family physician. The blueprint is the result of 17 patients' descriptions of their visits and an observer's description of activities that happen behind the scenes (or below the “line of visibility”). The blueprint begins with a patient entering the clinic and being greeted by the receptionist and ends with the patient receiving test results, or appropriate follow-up.
A practice blueprint
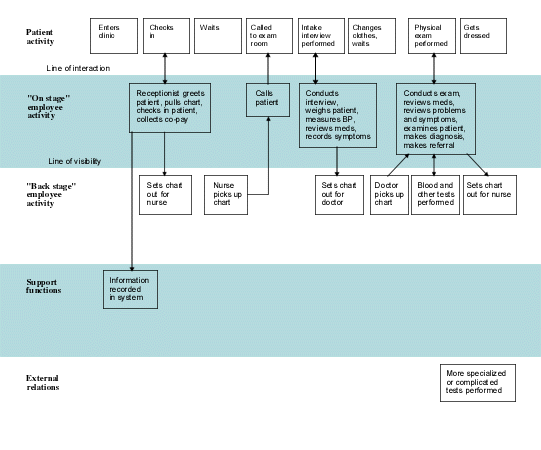
(image continued)
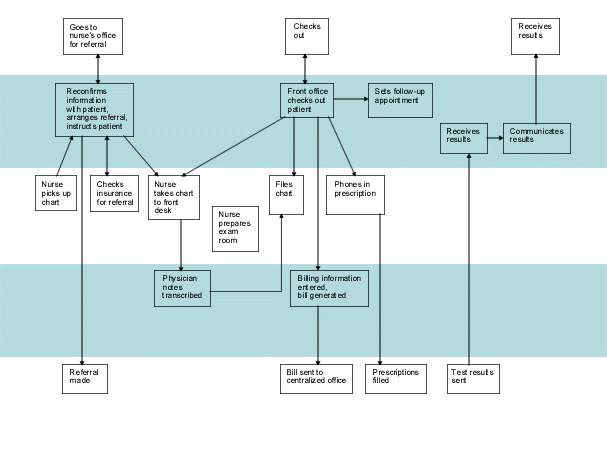
The value of a blueprint
A practice blueprint can be useful in several ways. First, it clarifies each team member's roles and responsibilities, including direct patient interaction and behind-the-scenes activities. This answers questions such as “Who is responsible for patient education?” or “Who should call patients with their test results?”
Second, it helps reveal problem areas and targets for improvements. Perhaps the care process is inconsistent from patient to patient, or perhaps it works well for some patients but not for others. You may find that one segment of your patient population needs more time with the physicians or would benefit from additional steps in the process. Improvements may be relatively easy to make (for example, systematically offering maps to referral locations) and can dramatically improve patients' perceptions of quality of care.
Third, a practice blueprint is especially valuable for helping you compare observed processes with the practice's mission and goals. For example, if prevention and wellness have been established as priorities for the practice, the care process should reflect these goals. Is the process consistent across physicians and other staff members so that the practice's goals and objectives can be met? It can also be useful to evaluate your actual process against what you define as the ideal process and then identify opportunities for improvement.
Finally, you can use a practice blueprint to illustrate that providing patient care is a team effort. Members of the practice team must understand their own responsibilities as well as how their roles fit into the overall process. A practice blueprint can facilitate this understanding for staff members.
How to do it
It's relatively easy to construct a practice blueprint. Data for the steps above the line of visibility come from a sample of patients. In most situations, a representative sample of 15 to 30 patients is sufficient, although separate analyses for multiple groups of patients (e.g., geriatrics and pediatrics) will require a larger sample. When selecting participants, try to include patients with different demographics and service needs (for example, health-maintenance visits vs. acute-care visits). At check-in, the receptionist can ask patients to participate and can tell them how to record their observations. Patients list the activities and interactions that make up their appointments in as much detail as possible and simply return their lists of observations to the receptionist when they check out. Alternatively, patients can complete and mail their lists from home, although those data generally are not as reliable.
Data for steps below the line of visibility can be gathered fairly easily from members of your office team. They can provide this information individually or through group discussions, or a third party can observe and record the activities and interactions that take place.
Using patient and staff information, you can then begin to map out your care process. You can use graphics software (such as CorelDRAW, which we used) to create the actual blueprint document. Directional arrows help illustrate the flow of information and connect related steps in the process. When your blueprint is complete, ask other members of the practice team to examine it and verify that it accurately reflects your care process. We have found that a group effort yields more accurate and detailed diagrams than individual efforts.
Once you have a blueprint that reflects the actual care process of your practice, you can use it to find ways to improve the process. Are certain steps inefficient, confusing or unnecessary? Are there bottlenecks? Is everyone following the same procedures? Do you need additional steps to help you accomplish specific practice goals (e.g., patient education or prevention)? By answering questions such as these, you will be on your way to creating a solid care process that will yield better outcomes and improved quality.