
Fam Pract Manag. 1999;6(7):15-16
Physician groups call for universal coverage
The AAFP joined six other national physician organizations in a call to make universal health care coverage a top priority for the 106th Congress and the 2000 presidential candidates.
The medical groups plan to use their organizational resources and collective grassroots membership of more than 600,000 doctors to press political candidates on the subject of the uninsured. The six other medical societies devoted to this effort are the AMA, the American Academy of Pediatrics, the American College of Emergency Physicians, the American College of Obstetricians and Gynecologists, the American College of Physicians-American Society of Internal Medicine, and the American College of Surgeons.
Last year, the AAFP created a Task Force on Universal Coverage to examine the issues surrounding the availability of health insurance for U.S. citizens and options for moving toward coverage for all. Currently, more than 43 million Americans lack health insurance, and the number is expected to grow to more than 47 million within the next five years.
Family physicians see small income gain
Median net income for office-based family physicians rose to $128,000 last year, a 2.4 percent increase over 1997, according to new data from the AAFP. In recent years, most increases for family physicians have been small. An exception was 1995, when net income rose 10 percent.
Median net income for all non-federal physicians (excluding residents) fell 1.2 percent in 1997 to $164,000, according to the June 7 American Medical News, citing the AMA's latest Socioeconomic Monitoring System Survey of Physicians.
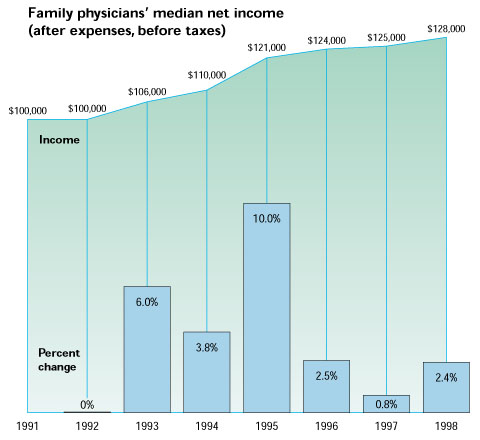
Source: AAFP. Practice Profile Survey I, May 1999, and Facts About Family Practice, 1993-1998.
AMA delegates vote to create union
The AMA House of Delegates voted in June to reverse the AMA's traditional opposition to unionization and form a national labor union to represent employed physicians and, where allowed, residents.
“Our objective here is to give America's physicians the leverage they now lack to guarantee that patient care is not compromised or neglected for the sake of profits,” says Randolph D. Smoak Jr., MD, AMA chair. Officials say the union will not strike and will not focus on matters such as pay and benefits, reports the June 24 New York Times.
But some observers doubt that altruism underlies the AMA's move. “This is happening because doctors' incomes [and] doctors' sense of autonomy are getting killed,” says Howard Berliner, a professor of health policy at the New School for Social Research in New York, quoted in the Times.
The AMA says it will work to unionize self-employed physicians too, but it must first lobby Congress for a federal antitrust exemption that would allow independent physicians to bargain collectively. The day before the AMA vote, officials with the Justice Department and the Federal Trade Commission (FTC) testified against that idea before the House Judiciary Committee.
“The commission continues to believe that such an exemption would be bad medicine for consumers” because it would increase health care costs, says FTC Chairman Robert Pitofsky, quoted in the Times. “Competition among health care providers and among health plans is an important tool for controlling costs, providing consumer choice and promoting innovation and high quality.”
Physician report cards receive low grade
Results of a study sponsored by the Agency for Health Care Policy and Research (AHCPR) question whether physician report cards really measure how well physicians manage their patients' care. Report cards are used by growing numbers of health care plans and hospitals as a way to help doctors improve their performance and to help patients select their physicians.
Researchers, who studied physicians' care of patients with type 2 diabetes mellitus, found that the report cards could not detect true practice differences among the participating doctors. In fact, they found that differences in the physicians' practice styles contributed no more than 4 percent to the overall variance in patient outcomes. The main difficulty in judging performance by outcomes was the relatively small number of patients with a given condition managed by each physician.
“Apart from hypertension, it is difficult to imagine that there would be enough cases per primary care physician to construct disease-specific profiles for almost any other chronic condition,” said Sheldon Greenfield, MD, a co-author of the study, noting that physicians are sometimes evaluated based on as few as four patients. “The science does not support such reckless use of numbers for judging physicians.”
Greenfield noted that the findings do not excuse physicians from being accountable for patients' outcomes but that health care plans and hospitals should reconsider their methods for judging physician performance.
HHS expands ‘senior patrols,’ billing education
In June, Health and Human Services (HHS) Secretary Donna Shalala announced the awarding of $7 million in grants to expand the Senior Medicare Patrol Project, which recruits and trains retired professionals nationwide to identify problems such as over-billing, overcharging and providing unnecessary or inappropriate services.
The project began in 1997 and has trained more than 6,000 retirees, who in turn have trained more than 70,000 Medicare beneficiaries. The latest grants will support training for 15,000 more volunteers, who will help educate an additional 250,000 beneficiaries.
Also in June, HCFA announced that it is expanding a program designed to educate physicians and other providers about Medicare's billing procedures. The initiative includes seminars, Internet-based training and hands-on training for residents.
The program is designed to teach physicians more about Medicare coverage and claims procedures, as well as the government's efforts to prevent waste, fraud and abuse. For more information, visit www.hcfa.gov/learning/default.htm.
Quote. Endquote.
“[Insurers] make the IRS look fast and fair.”
Delaware Valley Healthcare Council President Andrew Wigglesworth, commenting in the June 13 Philadelphia Inquirer on the problem of denied and delayed payments from insurance companies.
Y2K Update: More medical devices found to be noncompliant
Almost 4,500 medical devices are not yet Y2K compliant, almost five times the number manufacturers previously reported to the FDA, according to Joel Willemssen of the General Accounting Office. The June 11 Dallas Morning News reported that, during testimony before the Senate Special Committee on the Year 2000 Problem, Willemssen described the majority of the problems with equipment as incorrect date readings that would not directly affect patients' health but “could pose a risk” if used for purposes such as calculating blood glucose levels. The FDA has developed a list of potentially high-risk medical devices, such as ventilators and infusion pumps, that could cause immediate harm to patients should the devices fail to operate as expected due to Y2K problems.
Rural hospitals struggling
Health care entities at greatest risk for Y2K noncompliance are rural hospitals. Mark Stoddard, president of Utah-based Rural Health Management Corp., testified before the Senate Special Committee on the Year 2000 Problem that rural hospitals are having an especially hard time preparing for Y2K because they lack resources, partly as a result of federal reductions in Medicare reimbursements. In the June 10 Salt Lake Tribune, Stoddard said that preparing a CT scanner for the year 2000 can cost up to $1 million, “so to say we're nervous about the future would be a bit of an understatement.” The committee's chair, Sen. Robert Bennett (R- Utah), is expected to introduce a bill that would provide $50 million in funding to assist rural hospitals.
Studies: Social status determines health
An influx of recent research suggests that “the higher the rung on the socioeconomic ladder, the lower the [health] risk,” reports the June 1 New York Times. “And this relationship holds even at the upper reaches of society, where it might seem that an abundance of resources would even things out.”
The first major research linking social status and health came in the late 1960s through the Whitehall study. Researchers studying men in the British civil service found a consistent decrease in mortality rates as job classification increased. In the last five years, 193 papers addressing this subject have appeared in scientific journals, double the number of the previous five years, says the Times. Researchers have found that socioeconomic status may have a greater impact on one's health than smoking, exposure to carcinogens or genetics.