
For some physicians, the family focus goes deeper than simply taking a health history.
Fam Pract Manag. 2001;8(3):49-50
In family practice, the concept of “family” matters. Indeed, as a specialty, “Our roots are in family.”1 But how is this family orientation translated into daily practice? How prevalent is a family focus in family practice? And does this focus make a difference in patient outcomes?
Study results
To answer these questions, we examined data from 4,454 directly observed visits to 138 family physicians in Northeast Ohio as part of the Direct Observation of Primary Care Study. The study found that there is a strong focus on the family in family practice.2 In fact, based on multiple measures, 92 percent of family physicians demonstrate some evidence of a family focus. For example, family histories are taken during more than half of new-patient visits and almost one-quarter of established-patient visits. More than one-third of medical records have information about the patient’s family history of breast cancer, colon cancer and alcohol abuse. And, on average, 10 percent of visit time is spent discussing family issues.
A family health focus appears to be important to patients as well. Among established patients, 72 percent report that multiple family members see the same doctor. In almost one-third of observed visits, a patient’s family member was present, and in 18 percent of visits, family physicians discussed the health problems of a patient’s family member.3
Using a statistical technique for clustering data (factor analysis), we found that physicians had two different styles of incorporating the family in patient care. Physicians with a “family history style” gathered and used family information to provide a context for treating the individual patient, but they did not delve deeply into family problems. Physicians with a “family orientation style” were more likely to view the family as a unit of care, seeing multiple members of the same family, using family charts and addressing family issues during patient visits. Patients reported that physicians with a family orientation style “know a lot about my family.” Physicians with a family history style were less likely to be rated as such.
ILLUMINATING THE ‘BLACK BOX’ OF PRIMARY CARE
This article continues our series offering practical lessons from the Direct Observation of Primary Care (DOPC) Study, which was funded by the National Institutes of Health and conducted by the Center for Research in Family Practice and Primary Care, with support from the AAFP. The study demonstrates the complexities of the patient visit, the demands of real-world practice and the value of primary care, issues that policymakers, the public and even clinicians have not fully understood. Researchers used a multi-method approach, including direct observation, to study 4,454 patient visits to 138 family physicians in 84 practice sites.
Take-away lessons
Methods of focusing on the family are becoming increasingly important as genetic assessment, which may require extensive and detailed documentation of family history, becomes more prevalent. Since family physicians have a unique opportunity to identify individuals and families at risk for inherited conditions,4 it is important that we explore additional time-efficient methods of gathering and recording family histories. A visual aid, such as a genogram can simplify the family history record and make it more accurate and easier to maintain.5
A focus on the family is one of the keys to providing comprehensive care. But does a particular family focus style affect patient care outcomes? We will examine that question in the next article in this series.
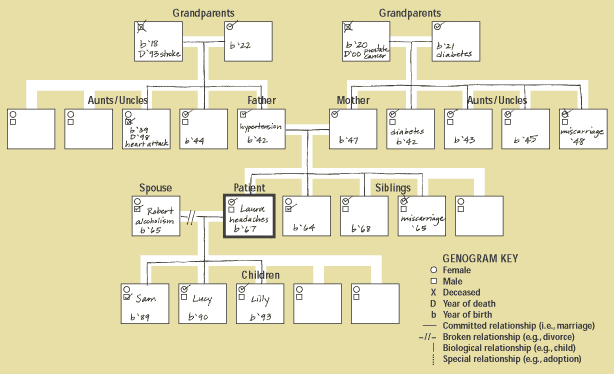
A SAMPLE GENOGRAM
A genogram is simply a pictorial display of a patient’s family relationships and medical history. It can provide a quick and useful context in which to evaluate an individual’s health risks.
Genograms are constructed much like a family tree but include individuals’ cause of death and significant health problems, such as diabetes, heart disease, cancer, alcohol or drug abuse, eating disorders and depression. A completed genogram template is shown below. Although this template will not apply to all family situations, it offers a useful starting point for introducing genograms in your practice. Click below to print a blank copy of the template ready for use in your practice.
Editor’s note: Part two of this series will appear in the April 2001 issue of FPM.