
Fam Pract Manag. 2002;9(1):21-22
Medicare physician payments face significant cuts
The 5.4 percent drop in the conversion factor under Medicare’s 2002 physician fee schedule represents the largest one-year decrease since the fee schedule was implemented in 1992 and the fourth time in 10 years that physician payments have been reduced.
Medicare payments are determined by multiplying each code’s relative value units (RVUs) by a conversion factor to calculate a national payment, which is then modified by geographic cost adjustments. Because of changes in work and practice-expense RVUs, reimbursement for some codes will increase slightly despite this year’s lower conversion factor. Four evaluation and management (E/M) codes used often by family physicians will receive small increases: 99211 (1.9 percent), 99212 (0.67 percent), 99214 (0.13 percent) and 99203 (0.56 percent). Reimbursement for code 99213 is scheduled to drop by 0.36 percent.
At press time, efforts are underway in Congress to stop the reimbursement cuts and require that a new method be developed for determining the annual payment updates. However, according to the Nov. 12 Part B News, Ken Johnson, spokesperson for the House Commerce Committee, doesn’t think action on the proposals is likely: “I think during normal times, [the fee schedule issue] would be a priority …, but these aren’t normal times.”
PRACTICE PEARLS from here and there
Helping patients surf the Web
There are currently over 17,000 health-related Web sites on the Internet, many of which do not contain accurate, up-to-date information. To save yourself the time of having to debunk health-related misinformation, offer patients the following tips for locating accurate health information online:
Look for Web addresses that end in .gov, .org and .edu. These sites tend to be more reliable than commercial (or .com) sites.
Compare and contrast. Tell patients to get their information from several sites. If they find the same information on several sites, there is a greater chance that the information is accurate.
Trust your first impression. Look for sites that are professionally designed and have well-written articles supported by reasonably current references.
– How to find reliable health information on the Internet. National Women’s Health Report newsletter. New Brunswick, NJ: National Women’s Health Resource Center. October 2001:3.
PRACTICE PEARLS from here and there
Negative encounter log
Tracking all patient complaints – and then following up on them – can help you improve patient service and manage your liability risk. To do this, simply create a form that includes spaces for the following: the person named in the complaint, the date of the incident and report, the patient’s name and the physician’s name, the type of complaint, any steps taken in response, further follow-up needed, and the name of the complaint handler. Keep files of all complaints, separating the active from the resolved, and review them periodically looking for patterns that may direct you to underlying problems.
– Track and solve patient complaints with a negative encounter log. The Physician’s Advisory newsletter. Conshohocken, Pa: Advisory Publications. September 2001:8–9.
Studies document impact of direct-to-consumer ads, rising drug spending

Nearly one-third of adults have talked with their doctor about a drug they saw advertised, and 44 percent of those who talked to their doctor received a prescription for the medication they inquired about, according to a new survey by the Kaiser Family Foundation. Based on these results, the study concludes that 13 percent of Americans have received a specific prescription in response to seeing a drug ad.
In 2000, the pharmaceutical industry spent $2.5 billion on direct-to-consumer advertising, a ninefold increase since 1994 due largely to an increase in television advertising, according to another recently released Kaiser Family Foundation report. National spending for prescription drugs was an estimated $116.9 billion in 2000, nearly three times the amount spent in 1990, making prescription drugs the fastest growing segment of health care spending. Increased numbers of prescriptions and shifts in use from older to newer, more expensive drugs account for most of the growth, according to the report.
To read more about the Kaiser Family Foundation reports “Understanding the Effects of Direct-to-Consumer Prescription Drug Advertising” and “Prescription Drug Trends – A Chartbook Update,” visit the organization’s Web site at www.kff.org/content/2001/20011129a/.
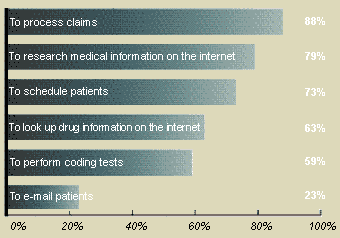
PHYSICIANS AND COMPUTERS
Ninety-six percent of medical practices use computers to some degree, according to the AMA’s 2001 Technology Usage in Physician Practice Management study. Although the study did not attempt to gauge the prevalence of electronic medical records (EMRs), it did find that only 13 percent of practices think EMRs would make their work easier.
No impact from gatekeeping

The “gatekeeper” model, in which patients are required to visit a primary care physician before accessing specialty care, may do little to reduce specialty visits and associated costs, according to research published in the Nov. 1 New England Journal of Medicine. Researchers studying the effects of one HMO's decision to abandon its use of gatekeepers found no change in the number of visits to specialists and only a slight drop in the number of visits to primary care physicians.
The costs of doing business
Overhead costs for multispecialty medical groups rose 6.2 percent in 2000 to nearly $300,000 per full-time physician, according to the Cost Survey: 2001 Report Based on 2000 Data, published by the Medical Group Management Association. Major contributors to the increase included rising supply costs (averaging $22,686 per full-time physician) and rising support-staff costs (averaging $156,492 per full-time physician).
New and improved Medicare enrollment
The Centers for Medicare & Medicaid Services (CMS) recently simplified its Medicare physician enrollment form, “the most recent result of our agency-wide efforts to reduce Medicare hassles and let physicians and physician groups focus on patient care, not paperwork,” said CMS Administrator Thomas A. Scully. The revised form is 31 pages long, with half of those pages devoted to instructions. CMS says its goal is to process 90 percent of completed forms within 60 days, and 99 percent within 120 days.
$50 million to fight errors
The Agency for Healthcare Research and Quality has awarded $50 million to fund 94 new patient safety research projects. The research topics include using error-reporting systems to identify the causes of errors, preventing errors through the use of technology and understanding how working conditions (e.g., staffing levels, fatigue and stress) can affect patient safety.
Pain management 101
Doctors in California are now required under state law to take courses in pain management and end-oflife care as part of their continuing education to renew their medical licenses, according to the Oct. 30 San Francisco Chronicle. The law – the first of its kind in the nation – was inspired by the case of an elderly California man who suffered from bone fractures and probable lung cancer at the end of his life yet was denied adequate pain medication. Under the new law, the state medical board will be required to track complaints of physicians mishandling pain care and ensure that such cases are reviewed.
Myths about the uninsured
A new report from the Institute of Medicine puts to rest some common misconceptions about the country's uninsured. Titled Coverage Matters, the report notes that, of the approximately 40 million uninsured people in the United States, more than 80 percent live in working families and roughly one quarter are children. As the economy cools and health care premiums rise, the uninsured problem is expected to worsen.
Rx vending machines?
Just insert your prescription and swipe your credit card and out pops your medication from a giant vending machine. While it may sound like fiction, it's actually a fact – at least in Minnesota, where InstyMeds is approved for a statewide pilot project, reports the Nov. 13 Dallas Morning News. The automated prescription-filling machine was developed by a former ER physician, who came up with the idea as a way to reduce prescription errors and long lines at the pharmacy.
Gourmet hospital cuisine

As evidence of an industrywide trend to improve patient service, the University of Texas MD Anderson Cancer Center in Houston is now serving its patients butterflied shrimp with crab stuffing covered in a lobster bisque sauce, among other menu options, according to the Nov. 23 Houston Business Journal. The hospital says its cuisine helps patients regain their appetites and strength during their stays. For those patients who prefer the simpler things, standard hospital fare such as Jell-O and cottage cheese are also available.