
This unorthodox practice, built on four “ideal” principles, is steadily proving itself a success.
Fam Pract Manag. 2002;9(3):25-29
On Feb. 26, 2001, after nearly a decade of salaried practice within a large organization, I opened a solo office with no support staff and just 150 square feet. I took this radical step because I believe our current health care system is so deeply flawed that incremental improvements to current practice cannot possibly save it. I wanted to create an office that would simultaneously deliver on what the Institute for Healthcare Improvement (IHI) has identified as the four themes for ideal practice: unbeatable access to care for patients, deep and personal patient interactions, the utmost reliability in clinical care, and practice vitality in terms of finances, physician and staff satisfaction, and innovation.
In a previous article (“Going Solo: Making the Leap,” FPM, February 2002, page 29), I described the reasoning behind this unlikely leap. This article explores the results to date.
Four pillars of success
I was very nervous for much of 2001. While I felt comfortable with the theories behind my new practice – and had, in fact, implemented many of them (such as open-access scheduling) in my previous practice – I had never put all the components together in one office. Did the pieces fit? Were breakthroughs achievable across the board? Would my phone ring off the hook or not at all? Making the process even more complicated was the fact that I was pursuing my new practice only part-time. (I hold a part-time administrative position with Strong Health, my previous practice’s employer, based in Rochester, N.Y., where I assist other practices in developing lean and ideal systems of care.)
Let me describe the strategies I embraced and the results my practice achieved in terms of the IHI’s four themes for ideal practice:
1. Access: Patients have unlimited access to the care and information they need, when they need it. To achieve unlimited access, I have taken several steps. First, I have maintained “open-access” scheduling from day one. What that means is that, when I am in town, I offer an appointment “today” to every patient who calls my office, regardless of the perceived urgency of their complaints. The benefits of this are plenty: My patients are delighted that they can see me on the day their needs arise, I spend very little time on the phone negotiating appointments or assessing the “urgency” of the problem, and tomorrow’s schedule is free for whatever might come up. Also, if, say, my children are sick, I can stay home with them without great upheavals as I have at most one or two pre-scheduled patient visits to cancel.
KEY POINTS
The author’s solo, idealized practice operates with no support staff and just 150 square feet, making monthly operating expenses low.
Patients of the practice can see their personal physician on the day they call the office with a health care complaint, and the practice reports high rates of patient satisfaction and clinical success.
When the practice reaches its full volume of patients (just 12 per day), the author expects to take home more than $155,000 per year, thanks to lean systems and low overhead.
Another step I have taken is simply to do without an answering service and pager. Instead, I give out my home and cell phone numbers, asking patients to use their best judgment regarding after-hours calls. I take all call myself (meaning I have been on call continuously since Feb. 26, 2001). I have been called after 10 p.m. an average of once per month, and I receive just one or two calls per weekend.
In my former practice, when I was part of a “call group,” I received many more calls than this – and often spent call nights in the attic so as not to ruin sleep for the rest of my family. The paradoxical effect of barriers to access is that we increase unnecessary demand (e.g., “I just assumed there was a doctor in some call center awaiting my 2 a.m. call about hemorrhoids”) and we create a more difficult process (e.g., “I don’t know these patients calling me; therefore, I have to work harder to make sure I’m doing the right thing”).
True and unfettered access results in less unnecessary (and uncompensated) work for me as well as better care for my patients. Now, every call I receive is about a patient I know personally. The calls are much shorter. I always agree with what the on-call doctor said. And I don’t need to sort and fax a bunch of call slips in the morning. Patients have not abused their direct access to me. If anything, they have honored my trust with respect and consideration. When we remove the barriers and give patients direct access to their personal physician, their health care experience is enriched, our connection to them and understanding of them is enriched, and our work is easier.
2. Interaction: Interaction between the patient and care team is deep and personal. The care team has “memory” of the patient. Interaction is not the price we pay to submit a claim. It is the very essence of what we do. It is the vehicle for all that occurs in health care. Productivity-based compensation models and thin operating margins put severe pressure on time, thereby robbing patients and physicians of the meaningful interaction that is the core ingredient in good care. But an ideal practice has the time for patients to speak uninterrupted, for shared decision making, for sensitivity to cultural and community context, and for listening to patients’ stories.
Interaction with the people who come to my practice is often my deepest reward as I participate in the big and small things that compose their lives. Because my practice is relatively small (my goal is just 1,350 patients), deep and personal interaction is the norm. I know each and every one of my patients. I do not have to remember masses of patients who pass through my office in 10-minute slots.
On average, patients spend about 50 minutes in their doctor’s office but only 10 minutes with their personal physician. Yet the public is so used to suboptimal care that they are willing to say we have met their expectations with these rushed, impersonal interactions. Meeting expectations is not enough; we must exceed expectations.
I offer 30-minute appointments to my patients and regularly survey them about their experience in my office. More than 90 percent of them rate the amount of time they had to wait as “excellent” and their time spent with the physician as “excellent” as well. More than 80 percent of my patients report that they received more help than they expected from the day’s visit. And 100 percent report that they are “definitely” satisfied with the explanations I give regarding their care.
3. Reliability: The system exhibits high reliability in that it provides all and only the care known to be effective. If we are honest with ourselves, we physicians know there are serious and frightening gaps between what we do and what we could accomplish in the clinical arena if we had better systems to support our work. [See the reports “To Err Is Human” and “Crossing the Quality Chasm” by the Institute of Medicine.]
In safety, the strategy of exhortation, “Try harder! Read one more article! Check one more time! Go to another CME event!” is bankrupt. Humans make mistakes. One of the biggest mistakes in primary care isn’t what we do to patients but what we omit. We then label this as “noncompliance” on the patient’s part. For instance, the sixth report of the Joint National Committee on Prevention, Detection, Evaluation and Treatment of High Blood Pressure (JNC VI) states that across the United States, the average internist has 19 percent of his or her hypertensive patients treated to goal. The national best is 69 percent.
To provide more reliable care, simply trying harder and reading more articles isn’t going to cut it. Instead, we must begin to embrace information systems that can support our clinical efforts, whether they be electronic medical records, computerized care reminders, online clinical resources, etc. One fairly simple step I took was to follow the advice of Lawrence Staker, MD, who has shown how using disease registries – that is, keeping and reviewing simple lists of our patients who have chronic diseases – can achieve unprecedented results. Using a registry has allowed me to do better than the JNC VI’s “national best” in the treatment of hypertension. More than 75 percent of my patients are treated to goal, and I am aiming for 90 percent. To accomplish this, each month I review those patients who have exceeded limits (e.g., their blood pressure is too high or they have no blood pressure readings within acceptable time limits). I then call those patients and ask them to give me their current readings or come in to my office. I can no longer rest on “noncompliance” as an excuse for poor outcomes.
FINANCIAL GOALS AND RESULTS
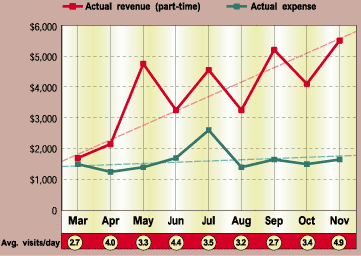
When his practice reaches full volume, the author will be able to average just 12 patient visits per day yet generate 130 percent of the salary he earned as an employed physician seeing 25 to 30 patients per day. The figures in the table (right) represent his goal (not actual) revenue, expenses and patient volume. The author’s actual monthly revenue, expenses and patient volume for his first nine months in private practice are shown in the graph. He is currently at approximately 50-percent capacity, as he has pursued his new practice only part-time while also holding a part-time administrative position at Strong Health, his former practice’s employer, where he assists offices and teams in their pursuit of lean and ideal systems of care.
| Goal revenue | Expenses (monthly) | ||
|---|---|---|---|
| Average $/visit | $65 | Non MD salary | $ —- |
| Visits/hour | 2 | Rent | $400 |
| Hours/day | 6 | Phone | $300 |
| Visits/day | 12 | Electronic chart | $250 |
| Days/week | 5 | Insurance | $100 |
| Weeks/year | 45 | Accounting | $50 |
| Visits/year | 2,700 | Loan | $350 |
| Average of visits/patient/year | 2 | Supplies | $150 |
| Patient panel | 1,350 | ||
| Gross revenue/month | $14,625 | Expenses/month | $1,600 |
| Gross revenue/year | $175,500 | Expenses/year | $19,200 |
| Net/month | $13,025 | ||
| Net/year | $156,300 |
4. Vitality: The practice has vitality: happy employees, a spirit of innovation and financial viability. Without intending to do so, we have created extremely expensive offices based on complex policies and procedures. In a typical office with three doctors and paper charts, it can often take a day and a half for a medication refill request to wind its way through the system and finally end up back in the medical record on the shelf. To support our complexity, we hire lots of staff, which in turn adds more expense, which then requires us to crank more patients through the system to pay for it all.
To break this cycle, practices have to question long-held assumptions and focus solely on value. With a pure focus on value from the patient perspective, an office can eliminate a great deal of non-value-added work that makes up the bulk of overhead. The value question is simply this: “What do my patients want and need?” When we apply this litmus test to all things in our office, we find out that a great deal of what we do does not add value from the perspective of patients.
FREQUENTLY ASKED QUESTIONS
How do you answer your own phone, manage “non-MD” tasks and see patients all at the same time?
Moore: When I am with a patient, my answering machine picks up all calls with the message: “This is Dr. Moore. I am with a patient right now. Please leave a message after the beep. If you have an urgent need to speak with me, call me directly on my cell phone at 555-5555.” With very low overhead, I don’t need to see hordes of patients each day to make ends meet. Seeing fewer patients, I don’t get that many phone calls. Because I use an electronic medical record and practice management system, making referrals, refilling prescriptions and all those little tasks have become much easier as well.
How are you building your patient panel? Were you able to continue seeing patients from your old practice?
Moore: I maintain a healthy and positive relationship with the health system that is my previous practice’s employer. I continue to work with the same specialists and admit to the same hospital. Some patients from my previous practice did come along.
Who takes care of your patients when you are out of town?
Moore: I simply leave a message on my answering machine that says: “I’m out of town. Please leave a message after the beep. I’ll be checking my messages regularly and will call you back. If you have an urgent need, please call me on my cell phone at 555-5555.” If a patient calls me and I determine that he or she needs an appointment that cannot wait until my return, I put them in touch with colleagues in town who have agreed to see my patients in these situations.
How do you handle gynecological or other sensitive exams without any staff members to serve as chaperones?
Moore: For any sensitive exam, I ask the patient to bring someone along or (as I rent a room in a specialist’s practice), I ask one of the specialist’s office staff to chaperone.
How does a physician survive financially while waiting for a new practice to reach its full volume of patients – and how long does this process take?
Moore: A typical office will take about 24 months to grow to full volume, but I do not recommend the typical office. Because patients have such an urgent and pressing need for access to and interaction with a personal, caring physician, an office that offers this will be more attractive to patients. If you commit to the creation of an ideal office practice and you get the message out locally, you will grow to full volume within six to 12 months. (My practice is at 50-percent capacity after 12 months because I have pursued it only part-time, given my part-time administrative position with a local health system.) Those first six months will be rich with new patient visits, generating healthy revenue. If you are beginning with some patients from a previous practice, it will be even easier.
What is the scope of your practice? Do you do any hospital work? Ob/gyn? Peds? Do you give your own shots?
Moore: I do hospital work. I do pediatrics. I do not do obstetrics. I love doing skin procedures, but no longer do them due to the overhead expense. I give my own shots.
Do you take Medicaid patients, given that the maximum reimbursement rate is just $30 per visit?
Moore: Yes, I do take Medicaid patients through HMOs. Although my business model assumes an average visit reimbursement of $65, I don’t mind the lower margin on Medicaid visits because my costs are so low. Also, I don’t want a VIP practice. I want to deliver VIP care to all comers.
Do you take HMO patients? If so, do you do your own referrals?
Moore: Yes, I do take HMO patients, but in Rochester, N.Y., HMOs use discounted fee-for-service. I do my own referrals electronically with the patient present (or on the phone), since it requires simply that I point, click, type a phrase and hit the “send” key.
For instance, does a patient want and need a support person to make their appointment, a person to pull their chart, a person to quiz them on the urgency of their request for an appointment? No. Ask your patients, and they will tell you that all they want is to know what is wrong with them and how to get better. In other words, my patients perceive me as the person who can deliver the value. Once I realized this, I decided to pursue it radically. By using technology and creating lean systems, I can manage the non-physician tasks with minimal hassle and remove the bulk of office expense while increasing the time I get to spend with patients.
This has become a virtuous cycle: With no office staff, seeing one patient at a time, I need only one exam room. Since I spend all of my time in that room, it is my office as well. Since I need so little room, I rent an exam room from a specialty colleague. The specialty front-office staff let me know when one of my patients arrives (I bought an inexpensive intercom for this purpose), I usher them in, the entire interaction is with me, and then the patient leaves.
The net result is monthly expenses of approximately $1,600, which means I can afford to spend the time I need to create robust interactions. (See “Financial goals and results.”) I do not ask patients to limit their concerns (doing so would increase unnecessary visits later) but address all concerns at hand, adding in appropriate preventive care. My typical office visit is a 99214, and my electronic chart allows easy documentation of the true care delivered.
A fundamental principle of an efficient office is being “in the loop” on crucial office functions, such as billing. Since I now do my own billing, I have learned the importance (as well as the dysfunction) of the ICD-9 and CPT nomenclatures. As of November 2001, more than 90 percent of my claims are paid within 30 days of the date of service. I do not have to pay for a billing service. I spend about one hour per week on billing (both getting the bills out as well as receiving the “explanation of benefits” and posting payments).
This is a prime example of the illusion of “economies of scale.” In a typical office, we believe that the doctor should be doing only doctoring. While this is true to a point, there are essential non-physician duties that we delegate at great risk. Billing is one. There is some perfect balance of teamwork and direct involvement, but we have gone so far in the direction of outsourcing and delegation that many physicians have a very poor understanding of the intricacies of billing, scheduling and office flow.
When we separate ourselves from these processes, our understanding degrades. At some point this degradation affects the quality of our work. The essential information for a clean bill comes only from the provider of that service, yet we often delegate the coding to another person in the office. When we find the errors and reimbursement unacceptable, we go one step further and outsource to a billing service and compensate the service with a percentage of our return.
So while it may seem absurd for a physician to answer every phone call, “arrive” the patient, take the vitals, collect the co-pay and submit the bill, it is little work in a continuous-flow office setting. With such a dramatic reduction in expenses, I must see an average of 60 patients per week, 45 weeks per year, to more than match my previous income as a salaried physician. While I am not there yet, my patient panel is growing steadily and my practice finances are on track.
Two roads diverged
An ideal office practice is attainable today. It is not attainable by tweaking the current system, but rather through a willingness to change any and all assumptions regarding the way office practices work. The choice is yours: Continue in your current model and achieve the same results you are getting now, or change.
My ultra-low-volume, continuous-flow office practice is one model of the ideal. One could easily add a secretary or nurse, but that would necessitate increasing one’s patient panel size and office space and creating policies for office communication. I have chosen the easy path for now. I encourage others to follow and help create innovative offices that achieve across-the-board results in access, interaction, reliability and vitality.