
Fam Pract Manag. 2002;9(6):24-28
Malpractice insurance rates on the rise

Medical malpractice premiums are reportedly soaring to unaffordable levels in certain parts of the country, with Texas, Pennsylvania, Nevada, Ohio and Mississippi among the states hit hardest in 2001, according to a recent analysis by AM News. Neurosurgeons, obstetricians and other high-risk specialists are seeing the highest increases, but some family physicians, particularly those who perform obstetric services, are being affected as well.
Malpractice insurance rates for family physicians vary widely by region and scope of practice. For example, in Alabama, family physicians with and without OB paid an average of $29,527 and $8,269, respectively, for malpractice premiums in 2001, roughly a 35 percent increase over the previous year. In West Virginia, family physicians with and without OB paid an average of $63,660 and $18,460, respectively, in 2001, an 18 percent increase over the previous year, according to Medical Assurance Inc.
In response to the situation, which some are calling a medical liability crisis, government and health care leaders are proposing a variety of solutions. Representatives James Greenwood, R-Pa., and Christopher Cox, R-Calif., have introduced legislation in Washington that would help reduce frivolous lawsuits and set caps for damages. Other groups are suggesting that improved patient safety initiatives are the answer. According to Jury Verdict Research, the median medical malpractice award jumped 43 percent in 2000 to $1 million.
Physicians challenge insurers over payment issues
In what has been called a landmark case, Blue Cross and Blue Shield of Georgia has been ordered to publish its fee schedule and method for calculating payments to doctors participating in its plans. The Medical Association of Georgia and four of its physicians filed the lawsuit against the Georgia Blues in 1997 when the health plan refused to provide participating physicians with information on how their payments are determined.
In Texas, the state's attorney general recently ruled that the Department of Insurance could force insurers to disclose their payment policies to physicians and other providers. Previously, the department had said it did not have that authority.
And in Connecticut, New Jersey, New York, South Carolina and Tennessee, medical associations have filed lawsuits against major insurers, alleging they use illegal methods to delay or deny reimbursements to physicians.
The methods in question include bundling separate services into a single reimbursable service, downcoding claims and using computer software programs that automatically reduce or deny certain kinds of claims, regardless of a patient's condition.
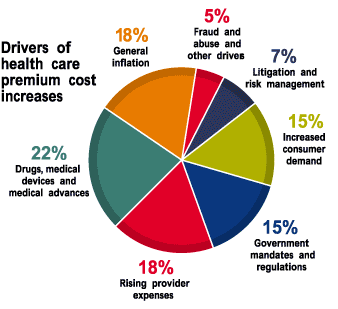
Why health care costs are rising
Spending on health care insurance premiums rose $67 billion in 2001, according to a new report from Pricewaterhouse-Coopers prepared for the American Association of Health Plans. Nearly a quarter of the increase is attributed to government mandates and litigation.
PRACTICE PEARLS from here and there
Stop penalizing your best staff members
Keep your high-performing staff members motivated by rewarding their work and making sure that those who perform poorly aren't being enabled, advises Sara Larch, COO of the University of Maryland School of Medicine's faculty practice and chair of the Medical Group Management Association's board of directors. Ask yourself whether any of the following are true for your practice:
Are poor performers repeatedly given overtime to complete tasks they should have finished during regular work hours?
Does everyone have the same opportunities to leave early or extend their lunch break when necessary, or do key employees not receive this flexibility because the practice depends so heavily on them?
Do excellent performers continually receive more projects, meaning they do more work than others?
Good employees are hard to find and harder to keep if the system doesn't reward their additional efforts.
– Maguire P. Rightsizing, not downsizing, is key to staffing success.
ACP–ASIM Observer. May 2002:5.
PRACTICE PEARLS from here and there
Gracefully close a chatty visit or call
Try the following suggestions the next time you need to end a patient visit or phone call that goes on and on and on …
Let the patient know the time limit for the visit is fast approaching. “Mr. Doe, we're coming to the close of our visit today. Do you have a question I can answer before we end?”
Try speaking in the past tense. “It's been nice talking with you.”
Let them know this isn't their last opportunity to communicate with you. “I'm looking forward to hearing more about your car when you come in for your next visit.”
– Baker SK. “Tips to end visits and telephone calls.” Available online at: www.susanbaker.com/tips/endingCalls.html. Accessed May 17, 2002.
Fixing the Medicare fee schedule
Some legislators aren't giving up. The May 14 CongressDaily reports that House Ways and Means Committee Chair Bill Thomas, R-Calif., has asked that language be attached to two upcoming bills “clarifying” that the Department of Health and Human Services has the legal authority to correct an apparent statistical error that resulted in this year's 5.4 percent reduction in physicians' Medicare payments. The Bush administration contends that only Congress can fix the error, which, if left uncorrected, would reduce physician payments 17 percent by 2005.
Money isn't everything
Over the past five years, the AMA has spent $83.5 million on lobbying efforts, more than any corporation, interest group or trade association, reports the April 27 National Journal. With all the money being spent to protect doctors' and patients' interests, some are wondering why the nation still lacks a patients' bill of rights and why physicians' Medicare reimbursements fell 5.4 percent this year. According to the National Journal, the AMA's poor relations with both political parties and internal strife are to blame.
$10 for your online time
Two-thirds of all adults use the Internet, and 90 percent of Internet users say they want to communicate online with their physicians, according to a recent report from Harris Interactive. Among Internet users, 37 percent would be willing to pay $10 per month on average for the ability to send and receive e-mails to and from their physicians. Over 50 percent said the ability to communicate online would influence their choice of physicians or health plans.
How not to negotiate a contract
Two Colorado physician groups charged with price fixing by the Federal Trade Commission have agreed to settle their case out of court without admitting liability, reports the May 14 Denver Rocky Mountain News. The groups' 86 physicians were allegedly advised to terminate or threaten to terminate individual contracts with health insurers in order to obtain higher reimbursement rates and better terms.
Prudent prescribing
Nearly 3 percent of prescription drugs approved by the Food and Drug Administration (FDA) between 1975 and 1999 were withdrawn from the market as unsafe, and more than 8 percent required warnings be added to alert physicians and patients of potentially dangerous side effects, reports a study in the May 1 Journal of the American Medical Association. The study's authors concluded that “clinicians should avoid using new drugs when older, similarly efficacious agents are available.” Both the FDA and the drug industry have questioned the findings.
Match game
A group of residents has filed a class-action lawsuit against the National Resident Matching Program, alleging that the program and its participating medical organizations and hospitals violate antitrust laws and force residents to accept below-market wages. If successful, the lawsuit could require hospitals and health care organizations to bid for residents' services, resulting in higher wages and shorter work-weeks.
Are you ready for HIPAA?
Eighty-one percent of California health care organizations have developed a plan for complying with the Health Insurance Portability and Accountability Act (HIPAA), according to a report from the California HealthCare Foundation. However, only 12 percent of the 100 organizations surveyed have carried out their compliance plans and 78 percent believe clarifications or modifications are needed to the HIPAA privacy rules before they can be implemented successfully. Physician groups reported the least progress towards compliance.
What's good for the goose …
Health and Human Services (HHS) Secretary Tommy Thompson, who has been known to take cigarettes away from HHS employees, is continuing his campaign for preventive services and healthier lifestyles, reports the May 7 Philadelphia Inquirer. Obesity, type-II diabetes and tobacco-related illnesses cost the nation $270 billion annually, lamented Thompson, who has done his part to reduce these costs by losing nine pounds this year and lowering his cholesterol by 155 points.