Fam Pract Manag. 2002;9(7):15-16
Primum non nocere, “first do no harm,” is one of our profession’s guiding principles. First and foremost, we want to avoid mistakes. In 1999, the Institute of Medicine’s (IOM) report, To Err Is Human: Building a Safer Health System, focused the spotlight on medical mistakes in hospitals. Yet, did the IOM’s report miss the mark? Hospitals represent a very small percentage of patient visits. Outpatient care is significantly more common, arguably more complex and varied, and much less structured and regulated. More patients visit family doctors than any other specialty. So, it seems prudent to ask, are medical errors equally serious and perhaps more prevalent in family practice? If so, can we do something to avoid them?
To begin with, let us consider what are common errors in family practice. Most of us may think of the patient whose breast lump was not diagnosed or the patient prescribed the wrong medication. What about the abnormal laboratory result that was misfiled or the cardiologist consultation recommending a medication change that was not communicated to the family physician? What about the patient with CHF who was not prescribed an ACE inhibitor or the patient who was not on a beta-blocker following his MI? What about the patient with hypertension who is overdue for a blood pressure evaluation, the one with diabetes overdue for an HbA1c or the child overdue for an immunization?
Understanding errors in family practice
We must all be able to define and understand the nature of errors in family practice before we can do something to avoid them. About the same time the IOM report was released, 42 family physicians in the AAFP’s National Network for Family Practice and Primary Care Research were busy identifying mistakes in their own practices. An elegantly simple, functional definition of medical errors guided this study. Participating family physicians were asked to report “anything that happened in their own practice that should not have happened, that was not anticipated and that makes them say,‘ That should not happen in my practice, and I don’t want it to happen again.’”
The mistakes reported by the 42 family doctors to Susan Dovey, MPH, and research colleagues at the AAFP’s Robert Graham Center were quite different in character than hospital-based medical errors. The errors (not surprisingly) highlighted the complex processes involved in primary care and the inadequate administrative systems physicians have to deal with.
Gaps in “knowledge and skills” (e.g., wrong diagnosis or treatment) accounted for a minority of errors. More than 80 percent of errors arose from administrative or “systems” errors. These included lapses in patient follow-up, misfiling or never documenting receipt of laboratory work or consultations, and miscommunication among facilities, physicians and patients. Physician offices accounted for more than 70 percent of the medical errors, but lack of coordination among physician offices and hospitals, emergency departments, skilled nursing facilities and home health were also cited. Almost half of these reports of errors were associated with adverse consequences, including hospital admission and even death.
Today, much work is underway to classify errors in primary care. A Primary Care International Study on Medical Errors is being conducted by family doctors in the United States, Australia, Canada, England, Germany, the Netherlands and New Zealand through the Linnaeus collaboration chaired by Dovey. This study will help develop and validate a classification system that we can use to collect, categorize and analyze errors in family practice and primary care. In addition, the AAFP has received a grant from the Agency for Healthcare Research and Quality to establish a Patient Safety Center. The center has developed a computerized, Web-based error-reporting system that meets federal confidentiality standards. This is a very impressive tool, one of the first of its kind. We are poised to put it into use, although its final configuration may await legislation enacted to protect any data collected from discovery.
The ability to report and learn from errors without being sued is a major concern. There may be reason to be hopeful, as legislation was recently introduced to protect physicians who report errors. The fate of such legislation will ultimately determine whether this and other error-reporting systems can be developed.
Eliminating errors
The ultimate purpose of analyzing errors is to learn how to avoid them by developing administrative systems in our office that prompt us to follow up and document that our patients are receiving state-of-the-art care. Today, others may assist family doctors in these efforts. For example, where I work, in AvMed Health Plan, a large Florida-based, nonprofit health system, we have elaborate chronic care databases and programs to help ensure that our family physicians can provide and document the best available care to their patients. Our results demonstrate that such systems of care can improve the health of our members.
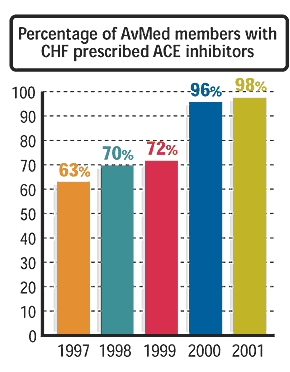
For example, today we can show that 98 percent of AvMed members with CHF are on life-saving ACE inhibitors (see “Percentage of AvMed members with CHF prescribed ACE inhibitors”). Caring for those with severe CHF is aided with electronic “telescales” AvMed purchases and installs in the patient’s home. These are scales that transmit changes in weight and symptoms to the family physician’s office. This early warning system has helped institute treatment that reduced hospitalizations by over 80 percent.
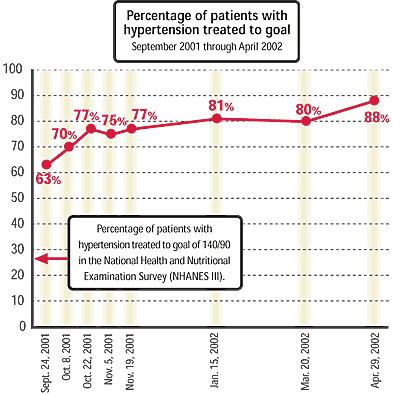
Today, aided by relatively inexpensive electronic medical records (EMRs), family physicians are designing their own administrative systems to avoid errors and document the quality care they provide. With an EMR, Gordon Moore, MD, a solo family physician, can demonstrate that 88 percent of his patients with hypertension are treated to goal (see “Percentage of patients with hypertension treated to goal”), far exceeding the percentages reported in the published literature. I would submit that documenting such quality outcomes is the result of our quest to avoid errors and to demonstrate objectively our value as family doctors. And the fact that encouraging results can be found both in large health plans and in solo practices is reason to believe that we can all make a difference, whatever our professional circumstances.
We hope that this special focus on medical errors and patient safety will help you begin to address these issues in your practice. We would like to share in the future how readers are tracking down and eliminating sources of error and, in the process, both improving and documenting their value as family doctors. In the meantime, ask yourself, did anything happen in your own practice that should not have happened and that you don’t want to have happen again? Let us know what you discover and how you go about preventing errors in the future.